Abstract
Purpose
To evaluate the anatomic versus functional changes in diabetic retinopathy (DR) by studying the correlation of retinal vascular perfusion density and dark adaptation (DA).
Methods
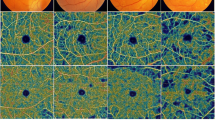
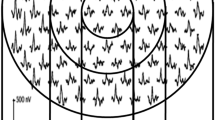
Optical coherence tomography angiography (OCTA) and DA tests were performed in diabetic patients and nondiabetic controls. DA was measured using AdaptDx dark adaptometer and the rod intercept was recorded. Macular OCTA images were acquired using the RTVue XR Avanti with AngioVue.
Results
Eighty-six eyes from 57 patients with diabetes (19 with no DR, 19 with non-proliferative DR [NPDR], and 19 with proliferative DR [PDR] who had undergone photocoagulation) and 10 eyes from 10 patients without diabetes were recruited. A significant decrease in vascular density and a prolonged rod intercept were found as DR progressed (P < .01). A negative trend was found between vascular density and the rod intercept. The negative trend in the deep layer (R2 = 0.28) was more substantial than that in the superficial layer (R2 = 0.14). A prolonged rod intercept was associated with elevated HbA1c (R2 = 0.08).
Conclusions
The vascular density of the macula could be assessed by OCTA and the functional change in the outer retina could be measured non-invasively by DA. The severity of decreasing vascular density and prolongation of DA are proportional to progression of DR. Decreased deep retinal vascular perfusion density and impaired DA response are correlated and show a negative trend according to the severity of DR.





Similar content being viewed by others
References
Yau JW, Rogers SL, Kawasaki R, Lamoureux EL, Kowalski JW, Bek T, Chen SJ, Dekker JM, Fletcher A, Grauslund J, Haffner S, Hamman RF, Ikram MK, Kayama T, Klein BE, Klein R, Krishnaiah S, Mayurasakorn K, O’Hare JP, Orchard TJ, Porta M, Rema M, Roy MS, Sharma T, Shaw J, Taylor H, Tielsch JM, Varma R, Wang JJ, Wang N, West S, Xu L, Yasuda M, Zhang X, Mitchell P, Wong TY, Meta-Analysis for Eye Disease Study G (2012) Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care 35:556–564. https://doi.org/10.2337/dc11-1909
Gardner TW, Abcouwer SF, Barber AJ, Jackson GR (2011) An integrated approach to diabetic retinopathy research. Arch Ophthalmol 129:230–235. https://doi.org/10.1001/archophthalmol.2010.362
Kurtenbach A, Mayser HM, Jagle H, Fritsche A, Zrenner E (2006) Hyperoxia, hyperglycemia, and photoreceptor sensitivity in normal and diabetic subjects. Vis Neurosci 23:651–661. https://doi.org/10.1017/S095252380623339X
Jia Y, Bailey ST, Hwang TS, McClintic SM, Gao SS, Pennesi ME, Flaxel CJ, Lauer AK, Wilson DJ, Hornegger J, Fujimoto JG, Huang D (2015) Quantitative optical coherence tomography angiography of vascular abnormalities in the living human eye. Proc Natl Acad Sci U S A 112:E2395–E2402. https://doi.org/10.1073/pnas.1500185112
Ishibazawa A, Nagaoka T, Takahashi A, Omae T, Tani T, Sogawa K, Yokota H, Yoshida A (2015) Optical coherence tomography angiography in diabetic retinopathy: a prospective pilot study. Am J Ophthalmol 160:35–44 e31. https://doi.org/10.1016/j.ajo.2015.04.021
Agemy SA, Scripsema NK, Shah CM, Chui T, Garcia PM, Lee JG, Gentile RC, Hsiao YS, Zhou Q, Ko T, Rosen RB (2015) Retinal vascular perfusion density mapping using optical coherence tomography angiography in normals and diabetic retinopathy patients. Retina 35:2353–2363. https://doi.org/10.1097/IAE.0000000000000862
Hwang TS, Gao SS, Liu L, Lauer AK, Bailey ST, Flaxel CJ, Wilson DJ, Huang D, Jia Y (2016) Automated quantification of capillary nonperfusion using optical coherence tomography angiography in diabetic retinopathy. JAMA Ophthalmol 134:367–373. https://doi.org/10.1001/jamaophthalmol.2015.5658
Takase N, Nozaki M, Kato A, Ozeki H, Yoshida M, Ogura Y (2015) Enlargement of foveal avascular zone in diabetic eyes evaluated by en face optical coherence tomography angiography. Retina 35:2377–2383. https://doi.org/10.1097/IAE.0000000000000849
Freiberg FJ, Pfau M, Wons J, Wirth MA, Becker MD, Michels S (2016) Optical coherence tomography angiography of the foveal avascular zone in diabetic retinopathy. Graefes Arch Clin Exp Ophthalmol 254:1051–1058. https://doi.org/10.1007/s00417-015-3148-2
Al-Sheikh M, Akil H, Pfau M, Sadda SR (2016) Swept-source OCT angiography imaging of the foveal avascular zone and macular capillary network density in diabetic retinopathy. Invest Ophthalmol Vis Sci 57:3907–3913. https://doi.org/10.1167/iovs.16-19570
Hasegawa N, Nozaki M, Takase N, Yoshida M, Ogura Y (2016) New insights into microaneurysms in the deep capillary plexus detected by optical coherence tomography angiography in diabetic macular edema. Invest Ophthalmol Vis Sci 57: OCT 348–355 DOI https://doi.org/10.1167/iovs.15-18782
Abraham FA, Haimovitz J, Berezin M (1988) The photopic and scotopic visual thresholds in diabetics without diabetic retinopathy. Metab Pediatr Syst Ophthalmol (1985) 11:76–77
Fortune B, Schneck ME, Adams AJ (1999) Multifocal electroretinogram delays reveal local retinal dysfunction in early diabetic retinopathy. Invest Ophthalmol Vis Sci 40:2638–2651
Tzekov R, Arden GB (1999) The electroretinogram in diabetic retinopathy. Surv Ophthalmol 44:53–60
Tyrberg M, Ponjavic V, Lovestam-Adrian M (2005) Multifocal electroretinography (mfERG) in insulin dependent diabetics with and without clinically apparent retinopathy. Doc Ophthalmol 110:137–143. https://doi.org/10.1007/s10633-005-4187-5
Bavinger JC, Dunbar GE, Stem MS, Blachley TS, Kwark L, Farsiu S, Jackson GR, Gardner TW (2016) The effects of diabetic retinopathy and pan-retinal photocoagulation on photoreceptor cell function as assessed by dark adaptometry. Invest Ophthalmol Vis Sci 57:208–217. https://doi.org/10.1167/iovs.15-17281
Arden GB, Jyothi S, Hogg CH, Lee YF, Sivaprasad S (2011) Regression of early diabetic macular oedema is associated with prevention of dark adaptation. Eye (Lond) 25:1546–1554. https://doi.org/10.1038/eye.2011.264
Arden GB, Gunduz MK, Kurtenbach A, Volker M, Zrenner E, Gunduz SB, Kamis U, Ozturk BT, Okudan S (2010) A preliminary trial to determine whether prevention of dark adaptation affects the course of early diabetic retinopathy. Eye (Lond) 24:1149–1155. https://doi.org/10.1038/eye.2009.328
Arden GB, Sidman RL, Arap W, Schlingemann RO (2005) Spare the rod and spoil the eye. Br J Ophthalmol 89:764–769. https://doi.org/10.1136/bjo.2004.062547
Ramsey DJ, Arden GB (2015) Hypoxia and dark adaptation in diabetic retinopathy: interactions, consequences, and therapy. Curr Diab Rep 15:118. https://doi.org/10.1007/s11892-015-0686-2
Wu L, Fernandez-Loaiza P, Sauma J, Hernandez-Bogantes E, Masis M (2013) Classification of diabetic retinopathy and diabetic macular edema. World J Diabetes 4:290–294. https://doi.org/10.4239/wjd.v4.i6.290
Holfort SK, Norgaard K, Jackson GR, Hommel E, Madsbad S, Munch IC, Klemp K, Sander B, Larsen M (2011) Retinal function in relation to improved glycaemic control in type 1 diabetes. Diabetologia 54:1853–1861. https://doi.org/10.1007/s00125-011-2149-x
Jackson GR, Scott IU, Kim IK, Quillen DA, Iannaccone A, Edwards JG (2014) Diagnostic sensitivity and specificity of dark adaptometry for detection of age-related macular degeneration. Invest Ophthalmol Vis Sci 55:1427–1431. https://doi.org/10.1167/iovs.13-13745
Flamendorf J, Agron E, Wong WT, Thompson D, Wiley HE, Doss EL, Al-Holou S, Ferris FL 3rd, Chew EY, Cukras C (2015) Impairments in dark adaptation are associated with age-related macular degeneration severity and reticular pseudodrusen. Ophthalmology 122:2053–2062. https://doi.org/10.1016/j.ophtha.2015.06.023
Owsley C, Huisingh C, Jackson GR, Curcio CA, Szalai AJ, Dashti N, Clark M, Rookard K, McCrory MA, Wright TT, Callahan MA, Kline LB, Witherspoon CD, McGwin G, Jr. (2014) Associations between abnormal rod-mediated dark adaptation and health and functioning in older adults with normal macular health. Invest Ophthalmol Vis Sci 55: 4776–4789 DOI https://doi.org/10.1167/iovs.14-14502
Jackson GR, Clark ME, Scott IU, Walter LE, Quillen DA, Brigell MG (2014) Twelve-month natural history of dark adaptation in patients with AMD. Optom Vis Sci 91:925–931. https://doi.org/10.1097/OPX.0000000000000247
Gołębiewska J, Olechowski A, Wysocka-Mincewicz M, Odrobina D, Baszyńska-Wilk M, Groszek A, Szalecki M, Hautz W (2017) Optical coherence tomography angiography vessel density in children with type 1 diabetes. PLoS One 20;12(10):e0186479. https://doi.org/10.1371/journal.pone.0186479.
Bursell SE, Clermont AC, Kinsley BT, Simonson DC, Aiello LM, Wolpert HA (1996) Retinal blood flow changes in patients with insulin-dependent diabetes mellitus and no diabetic retinopathy. Invest Ophthalmol Vis Sci 37:886–897
Feke GT, Buzney SM, Ogasawara H, Fujio N, Goger DG, Spack NP, Gabbay KH (1994) Retinal circulatory abnormalities in type 1 diabetes. Invest Ophthalmol Vis Sci 35:2968–2975
Nair G, Tanaka Y, Kim M, Olson DE, Thule PM, Pardue MT, Duong TQ (2011) MRI reveals differential regulation of retinal and choroidal blood volumes in rat retina. Neuroimage 54:1063–1069. https://doi.org/10.1016/j.neuroimage.2010.09.020
Klemp K, Sander B, Brockhoff PB, Vaag A, Lund-Andersen H, Larsen M (2005) The multifocal ERG in diabetic patients without retinopathy during euglycemic clamping. Invest Ophthalmol Vis Sci 46:2620–2626. https://doi.org/10.1167/iovs.04-1254
Bearse MA Jr, Adams AJ, Han Y, Schneck ME, Ng J, Bronson-Castain K, Barez S (2006) A multifocal electroretinogram model predicting the development of diabetic retinopathy. Prog Retin Eye Res 25:425–448. https://doi.org/10.1016/j.preteyeres.2006.07.001
Yonemura D, Aoki T, Tsuzuki K (1962) Electroretinogram in diabetic retinopathy. Arch Ophthalmol 68:19–24
Lains I, Miller JB, Park DH, Tsikata E, Davoudi S, Rahmani S, Pierce J, Silva R, Chen TC, Kim IK, Vavvas D, Miller JW, Husain D (2017) Structural changes associated with delayed dark adaptation in age-related macular degeneration. Ophthalmology 124:1340–1352. https://doi.org/10.1016/j.ophtha.2017.03.061
Arden GB (2001) The absence of diabetic retinopathy in patients with retinitis pigmentosa: implications for pathophysiology and possible treatment. Br J Ophthalmol 85:366–370
Birol G, Wang S, Budzynski E, Wangsa-Wirawan ND, Linsenmeier RA (2007) Oxygen distribution and consumption in the macaque retina. Am J Physiol Heart Circ Physiol 293:H1696–H1704. https://doi.org/10.1152/ajpheart.00221.2007
Stone J, van Driel D, Valter K, Rees S, Provis J (2008) The locations of mitochondria in mammalian photoreceptors: relation to retinal vasculature. Brain Res 1189:58–69. https://doi.org/10.1016/j.brainres.2007.10.083
Wikler KC, Williams RW, Rakic P (1990) Photoreceptor mosaic: number and distribution of rods and cones in the rhesus monkey retina. J Comp Neurol 22;297(4):499–508. https://doi.org/10.1002/cne.902970404
Curcio CA, Sloan KR, Kalina RE, Hendrickson AE (1990) Human photoreceptor topography. J Comp Neurol 22;292(4):497–523. https://doi.org/10.1002/cne.902920402
Funding
This study is supported by the joint funding of the National Taiwan University Hospital and SynCoreBio.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was waived due to the retrospective nature of this study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hsiao, CC., Hsu, HM., Yang, CM. et al. Correlation of retinal vascular perfusion density with dark adaptation in diabetic retinopathy. Graefes Arch Clin Exp Ophthalmol 257, 1401–1410 (2019). https://doi.org/10.1007/s00417-019-04321-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-019-04321-2