Abstract
Background and purpose
The group of genetic degenerative ataxias shares the same feature of gradual deterioration in balance and coordination. However, no cure is yet available for this group of disorders, while rehabilitation remains a cornerstone in the current therapy. This review aims to present a summary of the current knowledge of balance and coordination training in patients with inherited degenerative ataxia and to discuss the training effectiveness accordingly.
Methods
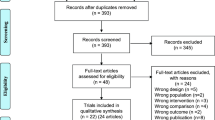
A comprehensive search was performed in 5 electronic databases (i.e., Cochrane Library, PEDro, EMbase, PubMed and MEDLINE) to identify the related publications from January, 1999 to January, 2020. Methodological quality was assessed using the Scottish Intercollegiate Guidelines Network (SIGN) grading system and the PEDro scale.
Results
A total of 33 out of 515 studies met the eligibility criteria, and were categorized and discussed by their training methods including: (1) conventional physical/occupational therapy, (2) virtual reality/videogame-based training, and (3) adapted physical activity. Despite the substantial variation among included studies, most patients achieved significant improvement in the aspect of balance and coordination following individually-tailored rehabilitation programs. The effects of training showed a relative consistency regardless of the functional dependency level on admission.
Conclusions
Balance and coordination training, especially the conventional physical/occupational therapy, is able to improve the balance and coordinative function of patients with genetic degenerative ataxia, but more high-quality studies are needed to formulate recommendations for clinical practice.

Similar content being viewed by others
References
Sun YM, Lu C, Wu ZY (2016) Spinocerebellar ataxia: relationship between phenotype and genotype—a review. Clin Genet 90(4):305–314
Burk K (2017) Friedreich Ataxia: current status and future prospects. Cerebellum Ataxias 4:4
Rothblum-Oviatt C, Wright J, Lefton-Greif MA, McGrath-Morrow SA, Crawford TO, Lederman HM (2016) Ataxia telangiectasia: a review. Orphanet J Rare Dis 11(1):159
Bird TD (1998, updated 2019) Hereditary ataxia overview. In: Adam MP, Ardinger HH, Pagon RA, Wallace SE, Bean LJH, Stephens K, Amemiya A (eds) GeneReviews((R)). Seattle (WA): University of Washington, Seattle; 1993–2020. Available from: https://www.ncbi.nlm.nih.gov/books/NBK1138/
Levy A, Lang AE (2018) Ataxia-telangiectasia: a review of movement disorders, clinical features, and genotype correlations. Movement Disord 33(8):1238–1247
Fonteyn EM, Keus SH, Verstappen CC, Schols L, de Groot IJ, van de Warrenburg BP (2014) The effectiveness of allied health care in patients with ataxia: a systematic review. J Neurol 261(2):251–258
Synofzik M, Ilg W (2014) Motor training in degenerative spinocerebellar disease: ataxia-specific improvements by intensive physiotherapy and exergames. Biomed Res Int 2014:583507
Marquer A, Barbieri G, Perennou D (2014) The assessment and treatment of postural disorders in cerebellar ataxia: a systematic review. Ann Phys Rehabil Med 57(2):67–78
Nardone A, Turcato AM, Schieppati M (2014) Effects of balance and gait rehabilitation in cerebellar disease of vascular or degenerative origin. Restor Neurol Neurosci 32(2):233–245
Martakis K, Stark C, Alberg E, Bossier C, Semler O, Schonau E, Duran I (2019) Motor function improvement in children with ataxia receiving interval rehabilitation, including vibration-assisted hometraining: a retrospective study. Klin Padiatr 231(6):304–312
Milne SC, Corben LA, Georgiou-Karistianis N, Delatycki MB, Yiu EM (2017) Rehabilitation for individuals with genetic degenerative ataxia: a systematic review. Neurorehabil Neural Repair 31(7):609–622
Harbour R, Miller J (2001) A new system for grading recommendations in evidence based guidelines. BMJ 323(7308):334–336
Maher CG, Sherrington C, Herbert RD, Moseley AM, Elkins M (2003) Reliability of the PEDro scale for rating quality of randomized controlled trials. Phys Ther 83(8):713–721
Marsden J, Harris C (2011) Cerebellar ataxia: pathophysiology and rehabilitation. Clin Rehabil 25(3):195–216
Miyai I, Ito M, Hattori N, Mihara M, Hatakenaka M, Yagura H, Sobue G, Nishizawa M, Cerebellar Ataxia Rehabilitation Trialists C (2012) Cerebellar ataxia rehabilitation trial in degenerative cerebellar diseases. Neurorehabil Neural Repair 26(5):515–522
Rodriguez-Diaz JC, Velazquez-Perez L, Rodriguez Labrada R, Aguilera Rodriguez R, Laffita Perez D, Canales Ochoa N, Medrano Montero J, Estupinan Rodriguez A, Osorio Borjas M, Gongora Marrero M, Reynaldo Cejas L, Gonzalez Zaldivar Y, Almaguer Gotay D (2018) Neurorehabilitation therapy in spinocerebellar ataxia type 2: a 24-week, rater-blinded, randomized, controlled trial. Movement Disord 33(9):1481–1487
Bunn LM, Marsden JF, Giunti P, Day BL (2015) Training balance with opto-kinetic stimuli in the home: a randomized controlled feasibility study in people with pure cerebellar disease. Clin Rehabil 29(2):143–153
Chang YJ, Chou CC, Huang WT, Lu CS, Wong AM, Hsu MJ (2015) Cycling regimen induces spinal circuitry plasticity and improves leg muscle coordination in individuals with spinocerebellar ataxia. Arch Phys Med Rehabil 96(6):1006–1013
Seco CJ, Fernandez IG, Verdejol IC, Perez VR, Atutxa AF, Torres-Unda J (2014) Improvements in quality of life in individuals with Friedreich’s ataxia after participation in a 5-year program of physical activity: an observational study pre-post test design, and two years follow-up. Int J Neurorehabil 1(3):129
Milne SC, Corben LA, Roberts M, Murphy A, Tai G, Georgiou-Karistianis N, Yiu EM, Delatycki MB (2018) Can rehabilitation improve the health and well-being in Friedreich's ataxia: a randomized controlled trial? Clin Rehabil 32(5):630–643
Barbuto S, Martelli D, Omofuma IB, Lee N, Kuo SH, Agrawal S, Lee S, O'Dell M, Stein J (2020) Phase I randomized single-blinded controlled study investigating the potential benefit of aerobic exercise in degenerative cerebellar disease. Clin Rehabil 34(5):584–594
Ilg W, Synofzik M, Brotz D, Burkard S, Giese MA, Schols L (2009) Intensive coordinative training improves motor performance in degenerative cerebellar disease. Neurology 73(22):1823–1830
Ilg W, Brotz D, Burkard S, Giese MA, Schols L, Synofzik M (2010) Long-term effects of coordinative training in degenerative cerebellar disease. Movement Disord 25(13):2239–2246
Keller JL, Bastian AJ (2014) A home balance exercise program improves walking in people with cerebellar ataxia. Neurorehabil Neural Repair 28(8):770–778
Tabbassum K, Zia N, Singh S, Suman K (2013) Core stability training with conventional balance training improves dynamic balance in progressive degenerative cerebellar ataxia. Indian J Physiother Occup Ther 7:136–140
Fonteyn EM, Heeren A, Engels JJ, Boer JJ, van de Warrenburg BP, Weerdesteyn V (2014) Gait adaptability training improves obstacle avoidance and dynamic stability in patients with cerebellar degeneration. Gait Post 40(1):247–251
Im SJ, Kim YH, Kim KH, Han JW, Yoon SJ, Park JH (2017) The effect of a task-specific locomotor training strategy on gait stability in patients with cerebellar disease: a feasibility study. Disabil Rehabil 39(10):1002–1008
Burciu RG, Fritsche N, Granert O, Schmitz L, Sponemann N, Konczak J, Theysohn N, Gerwig M, van Eimeren T, Timmann D (2013) Brain changes associated with postural training in patients with cerebellar degeneration: a voxel-based morphometry study. J Neurosci 33(10):4594–4604
Cakrt O, Vyhnalek M, Slaby K, Funda T, Vuillerme N, Kolar P, Jerabek J (2012) Balance rehabilitation therapy by tongue electrotactile biofeedback in patients with degenerative cerebellar disease. Neuro Rehabil 31(4):429–434
Jorge-Rodríguez JL, Fernández-Martínez E, Pérez DR, Peralta-Flores A, Bergado JA (2013) Motor improvement in cerebellar ataxia after integral rehabilitation. J Neurorestoratol 1:31–36
Milne SC, Campagna EJ, Corben LA, Delatycki MB, Teo K, Churchyard AJ, Haines TP (2012) Retrospective study of the effects of inpatient rehabilitation on improving and maintaining functional independence in people with Friedreich ataxia. Arch Phys Med Rehabil 93(10):1860–1863
Sawant P, Gokhale P (2015) Functional approach in spinocerebellar ataxia- occupational therapy perspective. Indian J Physiother Occup Ther 9:222–227
Sahay P, Roy D, Das S, Mondal M, Sarkar B (2017) Effects of intensive coordination training while walking in parallel bars with visual feedback in a case of spinocerebellar ataxia type I: a case report. Int J Health Sci Res 7(8):507–515
Schroeder T (2013) Rehabilitation of a US Army soldier diagnosed with cerebellar atrophy with an ataxic gait. Mil Med 178(7):e879–e883
Leonardi L, Aceto MG, Marcotulli C, Arcuria G, Serrao M, Pierelli F, Paone P, Filla A, Roca A, Casali C (2017) A wearable proprioceptive stabilizer for rehabilitation of limb and gait ataxia in hereditary cerebellar ataxias: a pilot open-labeled study. Neurol Sci 38(3):459–463
Bastani A, Cofre Lizama LE, Zoghi M, Blashki G, Davis S, Kaye AH, Khan F, Galea MP (2018) The combined effect of cranial-nerve non-invasive neuromodulation with high-intensity physiotherapy on gait and balance in a patient with cerebellar degeneration: a case report. Cerebellum Ataxias 5:6
Vanbellingen T, Filius SJ, Nyffeler T, van Wegen EEH (2017) Usability of videogame-based dexterity training in the early rehabilitation phase of stroke patients: a pilot study. Front Neurol 8:654
Rose FD, Brooks BM, Rizzo AA (2005) Virtual reality in brain damage rehabilitation: review. Cyberpsychol Behav 8(3):241–262 (discussion 263–271)
Levac D, Glegg S, Colquhoun H, Miller P, Noubary F (2017) Virtual reality and active videogame-based practice, learning needs, and preferences: a cross-Canada survey of physical therapists and occupational therapists. Games Health J 6(4):217–228
Bove RM, Rush G, Zhao C, Rowles W, Garcha P, Morrissey J, Schembri A, Alailima T, Langdon D, Possin K, Gazzaley A, Feinstein A, Anguera J (2019) A videogame-based digital therapeutic to improve processing speed in people with multiple sclerosis: a feasibility study. Neurol Ther 8(1):135–145
Dowling GA, Hone R, Brown C, Mastick J, Melnick M (2013) Feasibility of adapting a classroom balance training program to a video game platform for people with Parkinson's disease. Telemed J E Health 19(4):298–304
Wang RY, Huang FY, Soong BW, Huang SF, Yang YR (2018) A randomized controlled pilot trial of game-based training in individuals with spinocerebellar ataxia type 3. Sci Rep 8(1):7816
Ilg W, Schatton C, Schicks J, Giese MA, Schols L, Synofzik M (2012) Video game-based coordinative training improves ataxia in children with degenerative ataxia. Neurology 79(20):2056–2060
Santos G, Zeigelboim DBS, Severiano M, Teive H, Liberalesso P, Marques J, Cordeiro M (2017) Feasibility of virtual reality-based balance rehabilitation in adults with spinocerebellar ataxia: a prospective observational study. Hear Balance Commun. https://doi.org/10.1080/21695717.21692017.21381490
Schatton C, Synofzik M, Fleszar Z, Giese MA, Schols L, Ilg W (2017) Individualized exergame training improves postural control in advanced degenerative spinocerebellar ataxia: a rater-blinded, intra-individually controlled trial. Parkinsonism Related Disord 39:80–84
Synofzik M, Schatton C, Giese M, Wolf J, Schols L, Ilg W (2013) Videogame-based coordinative training can improve advanced, multisystemic early-onset ataxia. J Neurol 260(10):2656–2658
Zeigelboim BS, Souza SD, Mengelberg H, Teive HFG, Liberalesso PBN (2013) Vestibular rehabilitation with virtual reality in spinocerebellar ataxia. Audiol Commun Res 18(2):143–147
Toktaş H, Yaman F, Ulaşlı AM, Dündar Ü (2015) Virtual reality rehabilitation in a case with spinocerebellar ataxia. Turk J Phys Med Rehab 61:383–386
Kalyani HHN, Sullivan K, Moyle G, Brauer S, Jeffrey ER, Roeder L, Berndt S, Kerr G (2019) Effects of dance on gait, cognition, and dual-tasking in Parkinson's disease: a systematic review and meta-analysis. J Parkinsons Dis 9(2):335–349
Dos Santos DM, Komeroski IG, Monteiro EP, Costa RR, Haas AN (2018) Effects of dance practice on functional mobility, motor symptoms and quality of life in people with Parkinson's disease: a systematic review with meta-analysis. Aging Clin Exp Res 30(7):727–735
Hackney ME, Earhart GM (2010) Effects of dance on gait and balance in Parkinson's disease: a comparison of partnered and nonpartnered dance movement. Neurorehabil Neural Repair 24(4):384–392
Mandelbaum R, Triche EW, Fasoli SE, Lo AC (2016) A Pilot Study: examining the effects and tolerability of structured dance intervention for individuals with multiple sclerosis. Disabil Rehabil 38(3):218–222
Song YG, Ryu YU, Im SJ, Lee YS, Park JH (2019) Effects of dance-based movement therapy on balance, gait, and psychological functions in severe cerebellar ataxia: a case study. Physiother Theory Pract 35(8):756–763
Ni X, Liu S, Lu F, Shi X, Guo X (2014) Efficacy and safety of Tai Chi for Parkinson's disease: a systematic review and meta-analysis of randomized controlled trials. PLoS ONE 9(6):e99377
Winser SJ, Kannan P, Pang M, Smith C, Tsang WW (2018) Potential benefits and safety of T'ai Chi for balance and functional independence in people with cerebellar ataxia. J Altern Complement Med. https://doi.org/10.1089/acm.2017.0396
Bonnechere B, Jansen B, Omelina L, Van Sint JS (2016) The use of commercial video games in rehabilitation: a systematic review. Int J Rehabil Res 39(4):277–290
Rose T, Nam CS, Chen KB (2018) Immersion of virtual reality for rehabilitation—review. Appl Ergon 69:153–161
Lanza G, Casabona JA, Bellomo M, Cantone M, Fisicaro F, Bella R, Pennisi G, Bramanti P, Pennisi M, Bramanti A (2019) Update on intensive motor training in spinocerebellar ataxia: time to move a step forward? J Int Med Res:300060519854626
Funding
This work was supported by grants from Youth Program of National Natural Science Foundation of China (81901306, MH), Huxiang High-Level Talent Gathering Project of Hunan Province (2019RS1011, MH), the National Natural Science Foundation of China (No. 81672225, SSG).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical standard statement
The manuscript does not contain clinical studies or patient data.
Rights and permissions
About this article
Cite this article
He, M., Zhang, Hn., Tang, Zc. et al. Balance and coordination training for patients with genetic degenerative ataxia: a systematic review. J Neurol 268, 3690–3705 (2021). https://doi.org/10.1007/s00415-020-09938-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-020-09938-6