Abstract
Purpose
The aim of the study was to conduct a meta-analysis investigating the association of maternal iron deficiency anemia (IDA) and risk of gestational diabetes mellitus (GDM).
Methods
Literature search was conducted in various database websites such as PubMed, Cochrane Library, and Web of Science up to 17 June 2018 for related publications written in English. Selected data were extracted from the included studies and were subjected to statistical analysis. Odds ratios (ORs) and 95% confidence intervals (CIs) were computed, pooled, and interpreted. Subgroup analysis by ethnicity (Asians vs. Caucasians) was also performed.
Results
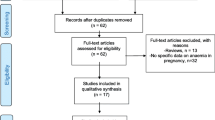
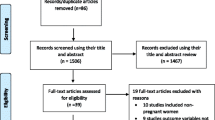
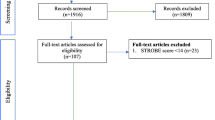
Six studies with a total sample size of 15,157 from various countries were included in this meta-analysis. Pooled ORs of all publications included show that pregnant women with IDA have a reduced risk of developing GDM (OR 0.61; 95% CI 0.47–0.80; PA = 0.0003). Subgroup analysis, on the other hand, showed significant associations among Asians (OR 0.60; 95% CI 0.45–0.79; PA = 0.0003) than Caucasians (OR 0.76; 95% CI 0.32–1.76; PA = 0.52).
Conclusion
Results of this meta-analysis suggests that pregnant women with IDA are 39% less likely to develop GDM. However, more studies are needed to confirm the claims of our results.



Similar content being viewed by others
References
Grewal A (2010) Anaemia and pregnancy: anaesthetic implications. Indian J Anaesth 54:380–386
Stevens GA, Finucane MM, De-Regil LM et al (2013) Global, regional, and national trends in haemoglobin concentration and prevalence of total and severe anaemia in children and pregnant and non-pregnant women for 1995–2011: a systematic analysis of population-representative data. Lancet Glob Health. https://doi.org/10.1016/s2214-109x(13)70001-9
McLean E, Cogswell M, Egli I et al (2009) Worldwide prevalence of anaemia, WHO Vitamin and Mineral Nutrition Information System, 1993–2005. Public Health Nutr 12:444–454. https://doi.org/10.1017/S1368980008002401
Milman N (2006) Iron and pregnancy—a delicate balance. Ann Hematol 85:559–565
Scholl TO (2010) Maternal nutrition and preterm delivery. Preventive nutrition. Springer, Cham, pp 673–703
Milman N (2008) Prepartum anaemia: prevention and treatment. Ann Hematol 87:949–959
Zhou LM, Yang WW, Hua JZ et al (1998) Relation of hemoglobin measured at different times in pregnancy to preterm birth and low birth weight in Shanghai, China. Am J Epidemiol 148:998–1006. https://doi.org/10.1093/oxfordjournals.aje.a009577
Turner S, Seybold D, Celestine C, Williams D (2012) Incidence of anemia among obstetric patients in an appalachian teaching clinic. Mil Med 177:1212–1216. https://doi.org/10.7205/MILMED-D-11-00445
Bánhidy F, Ács N, Puhó EH, Czeizel AE (2011) Iron deficiency anemia: pregnancy outcomes with or without iron supplementation. Nutrition 27:65–72. https://doi.org/10.1016/j.nut.2009.12.005
Lin L, Wei Y, Zhu W et al (2018) Prevalence, risk factors and associated adverse pregnancy outcomes of anaemia in Chinese pregnant women: a multicentre retrospective study. BMC Pregnancy Childbirth 18:111. https://doi.org/10.1186/s12884-018-1739-8
Lao TT, Pun T-C (1996) Anaemia in pregnancy—is the current definition meaningful? Eur J Obstet Gynecol Reprod Biol 68:53–58. https://doi.org/10.1016/0301-2115(96)02479-7
Lao TT, Chan LY, Tam KF, Ho LF (2002) Maternal hemoglobin and risk of gestational diabetes mellitus in Chinese women. Obstet Gynecol 99:807–812. https://doi.org/10.1016/S0029-7844(02)01941-5
Lao TT, Ho L-F (2004) Impact of iron deficiency anemia on prevalence of gestational diabetes mellitus. Diabetes Care 27:650–656
Wani AI, Bashir MI, Masoodi SR et al (2005) Relationship of prevalence of gestational diabetes mellitus with maternal hemoglobin. J Assoc Phys India 53:1077–1078
Tarim E, Kilicdag E, Bagis T, Ergin T (2004) High maternal hemoglobin and ferritin values as risk factors for gestational diabetes. Int J Gynecol Obstet 84:259–261. https://doi.org/10.1016/S0020-7292(03)00341-2
Wells GA, Shea B, O’Connell D et al (2013) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomized studies in meta-analyses. Ottawa Hosp Res Inst. https://doi.org/10.2307/632432
Pabalan N, Singh N, Pineda MR, Jarjanazi H (2014) Meta-analysis of the association between PTPN11 G/A polymorphism at intron 3 with risk of gastric atrophy among east Asians. J Gastrointest Cancer 45:319–324. https://doi.org/10.1007/s12029-014-9608-9
Pabalan N, Singian E, Tabangay L et al (2015) Associations of the A66G methionine synthase reductase polymorphism in colorectal cancer : a systematic review and meta-analysis. Biomark Cancer 7:21–28. https://doi.org/10.4137/bic.s25251.type
Pabalan N, Pineda MR, Jarjanazi H et al (2015) Association of the +331G/A progesterone receptor gene (PgR) polymorphism with risk of endometrial cancer in Caucasian women: a meta-analysis. Arch Gynecol Obstet 291:115–122. https://doi.org/10.1007/s00404-014-3344-z
Mantel N, Haenszel W (1959) Statistical aspects of the analysis of data from retrospective studies. J Natl Cancer Inst 22:719–748. https://doi.org/10.1093/jnci/22.4.719
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188
Lau J, Ioannidis JP, Schmid CH (1997) Quantitative synthesis in systematic reviews. Ann Intern Med 127:820–826. https://doi.org/10.7326/0003-4819-127-9-199711010-00008
Higgins JPT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ Br Med J 327:557–560. https://doi.org/10.1136/bmj.327.7414.557
Higgins JPT, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558. https://doi.org/10.1002/sim.1186
Ioannidis JPA, Trikalinos TA (2007) The appropriateness of asymmetry tests for publication bias in meta-analyses: a large survey. CMAJ 176:1091–1096. https://doi.org/10.1503/cmaj.060410
Lh A (2000) Anemia and iron deficiency: effects on pregnancy outcome. Am J Clin Nutr 7:1280–1284
Graham JJ, Ryall RG, Wise PH (1980) Glycosylated haemoglobin and relative polycythaemia in diabetes mellitus. Diabetologia 18:205–207. https://doi.org/10.1007/BF00251917
Roberts AP, Story CJ, Ryall RG (1984) Erythrocyte 2,3-bisphosphoglycerate concentrations and haemoglobin glycosylation in normoxic Type 1 (insulin-dependent) diabetes mellitus. Diabetologia 26:389–391. https://doi.org/10.1007/BF00266043
Samaja M, Melotti D, Carenini A, Pozza G (1982) Glycosylated haemoglobins and the oxygen affinity of whole blood. Diabetologia 23:399–402. https://doi.org/10.1007/BF00260950
Khambalia AZ, Aimone A, Nagubandi P et al (2016) High maternal iron status, dietary iron intake and iron supplement use in pregnancy and risk of gestational diabetes mellitus: a prospective study and systematic review. Diabet Med 33:1211–1221
Bencaiova G, Krafft A, Burkhardt T, Zimmermann R (2005) Hemoglobinopathies, body iron stores and gestational diabetes mellitus. Haematologica 90:1138–1139
Zhang C, Rawal S (2017) Dietary iron intake, iron status, and gestational diabetes. Am J Clin Nutr 106:1672S–1680S
Black RER, Victora CCG, Walker SSP et al (2013) Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet 382:427–451. https://doi.org/10.1016/S0140-6736(13)60937-X
Thomsen JK, Prien-Larsen JC, Devantier A, Fogh-Andersen N (1993) Low dose iron supplementation does not cover the need for iron during pregnancy. Acta Obstet Gynecol Scand 72:93–98. https://doi.org/10.3109/00016349309023419
Milman N, Agger AO, Nielsen OJ (1994) Iron status markers and serum erythropoietin in 120 mothers and newborn infants: effect of iron supplementation in normal pregnancy. Acta Obstet Gynecol Scand 73:200–204. https://doi.org/10.3109/00016349409023439
Bothwell TH (2000) Iron requirements in pregnancy and strategies to meet them. Am J Clin Nutr 72:257S–264S
Afkhami-Ardekani M, Rashidi M (2009) Iron status in women with and without gestational diabetes mellitus. J Diabetes Complicat 23:194–198. https://doi.org/10.1016/j.jdiacomp.2007.11.006
Behboudi-Gandevani S, Safary K, Moghaddam-Banaem L et al (2013) The relationship between maternal serum iron and zinc levels and their nutritional intakes in early pregnancy with gestational diabetes. Biol Trace Elem Res 154:7–13. https://doi.org/10.1007/s12011-013-9703-y
Omidvar S, Sharbatdaran M, Tilaki K et al (2013) Comparison of the serum iron, ferritin levels and total iron-binding capacity between pregnant women with and without gestational diabetes. J Nat Sci Biol Med 4:302. https://doi.org/10.4103/0976-9668.116977
Chen X, Scholl TO, Stein TP (2006) Association of elevated serum ferritin levels and the risk of gestational diabetes mellitus in pregnant women: the Camden study. Diabetes Care 29:1077–1082. https://doi.org/10.2337/dc06-0164
Soubasi V, Petridou S, Sarafidis K et al (2010) Association of increased maternal ferritin levels with gestational diabetes and intra-uterine growth retardation. Diabetes Metab 36:58–63. https://doi.org/10.1016/j.diabet.2009.06.010
Bo S, Menato G, Villois P et al (2009) Iron supplementation and gestational diabetes in midpregnancy. Am J Obstet Gynecol. https://doi.org/10.1016/j.ajog.2009.04.049
Rajpathak SN, Crandall JP, Wylie-Rosett J et al (2009) The role of iron in type 2 diabetes in humans. Biochim Biophys Acta Gen Subj 1790:671–681. https://doi.org/10.1016/j.bbagen.2008.04.005
Reif DW (1992) Ferritin as a source of iron for oxidative damage. Free Radic Biol Med 12:417–427. https://doi.org/10.1016/0891-5849(92)90091-T
Liu Q, Sun L, Tan Y et al (2009) Role of iron deficiency and overload in the pathogenesis of diabetes and diabetic complications. Curr Med Chem 16:113–129. https://doi.org/10.2174/092986709787002862
Wilson JG, Lindquist JH, Grambow SC et al (2003) Potential role of increased iron stores in diabetes. Am J Med Sci 325:332–339
Green A, Basile R, Rumberger JM (2006) Transferrin and iron induce insulin resistance of glucose transport in adipocytes. Metabolism 55:1042–1045. https://doi.org/10.1016/j.metabol.2006.03.015
Fan FS (2016) Iron deficiency anemia due to excessive green tea drinking. Clin Case Reports 4:1053–1056. https://doi.org/10.1002/ccr3.707
Sharma JB, Soni D, Murthy NS, Malhotra M (2003) Effect of dietary habits on prevalence of anemia in pregnant women of Delhi. J Obstet Gynaecol Res 29:73–78
Beck KL, Conlon CA, Kruger R et al (2014) Blood donation, being asian, and a history of iron deficiency are stronger predictors of iron deficiency than dietary patterns in premenopausal women. Biomed Res Int 2014:1–7. https://doi.org/10.1155/2014/652860
McGregor J, McKie AT, Simpson RJ (2004) Of mice and men: genetic determinants of iron status. Proc Nutr Soc 63:11–20. https://doi.org/10.1079/PNS2003312
Author information
Authors and Affiliations
Contributions
RET: Project development, data collection, data analysis, manuscript writing. EA: Data collection, data analysis, manuscript writing. BC: Data analysis, manuscript writing. MRP-C: Project development, data analysis, manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Tiongco, R.E., Arceo, E., Clemente, B. et al. Association of maternal iron deficiency anemia with the risk of gestational diabetes mellitus: a meta-analysis. Arch Gynecol Obstet 299, 89–95 (2019). https://doi.org/10.1007/s00404-018-4932-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-018-4932-0