Abstract
Background
The European Society of Human Reproduction and Embryology–European Society for Gynaecological Endoscopy (ESHRE–ESGE) system is designed mainly for clinical orientation; its overdiagnosis of septate uteri was confirmed in a general population in comparison to the American Society of Reproductive Medicine (ASRM) supplemental classification proposed by Ludwin. However, the agreement among septate uterus recognition using the ESHRE–ESGE and the supplemental ASRM classifications and the rate of overdiagnosis of septate uterus by ESHRE-ESGE in infertile women remain unclear.
Methods
We conducted a retrospective study of 53,540 infertile patients in our reproductive centre from June 2013 to December 2016, to compare septate uterus recognition using three systems. The data were analysed by the ESHRE–ESGE system, the ASRM by Salim and the ASRM by Ludwin separately. The concordance of diagnoses of septate uteri using these three systems was compared.
Results
ESHRE–ESGE classification significantly increased the frequency of septate uteri (11.31%, 6056 vs. 7.20%, 3854 vs. 3.80%, 2034). Good agreement was observed between the ESHRE-ESGE and the ASRM by Salim (k = 0.686, p < 0.001) and between the ASRM by Salim and that by Ludwin (k = 0.671, p < 0.001), while moderate agreement was found between the ESHRE–ESGE and ASRM by Ludwin systems (k = 0.444, p < 0.001). These results suggest that Ludwin’s criteria are the strictest, while the ESHRE–ESGE system is much more relaxed for septate uterus diagnosis.
Conclusion
A risk of overtreatment may also exist in infertile patients when using the ESHRE–ESGE system. Therefore, the ESHRE–ESGE system should be used with caution when guiding hysteroscopic metroplasty in infertile patients.
Similar content being viewed by others
Background
Congenital uterine anomalies result from abnormal formation, canalisation, fusion or resorption of the unilateral or bilateral Müllerian ducts during embryogenesis [1, 2]. These anomalies, especially septate uteri, have been reported to be associated with infertility and adverse pregnancy outcomes, such as miscarriage and preterm delivery [3,4,5].
Four main systems have been proposed for classifying congenital uterine anomalies: the American Fertility Society (AFS), presently called the American Society of Reproductive Medicine (ASRM) system [6], the embryological–clinical classification system of genito-urinary malformations [7, 8], the vagina, cervix, uterus, adnex-associated malformations (VCUAM) system [9] and the European Society of Human Reproduction and Embryology–European Society for Gynaecological Endoscopy (ESHRE–ESGE) system [10].
Of these systems, the ASRM system has been the most popular for over 20 years. Septate uteri diagnosed by the ASRM are commonly considered as an indication for surgery in infertile women [11, 12]. However, the original ASRM system did not provide strict parameters to define septate uteri [6]. Some modified ASRM classifications have subsequently been proposed to better characterise and differentiate a septate from an arcuate uterus. These modified classifications differentiate a septate uterus from an arcuate uterus based on either the angle of the septum central point (Salim et al. < 90° vs. > 90) [13] or the length of the septum (Ludwin et al. > 15 mm vs. 10–15 mm) [14,15,16].
The ESHRE–ESGE system proposed in 2013 [10] was designed mainly for clinical orientation. However, some authors [17, 18] noted the risks of overdiagnosis and overtreatment of septate uteri using this system immediately after its introduction. Moreover, the use of the uterine wall as a benchmark was criticised as a logical paradox [17] and the use of ESHRE–ESGE criteria for post-operative assessment of the uterine cavity showed a high rate of residual septum after hysteroscopic metroplasty compared to the criterion of 1 cm used by surgeons to decide about reintervention [18, 19]. Additionally, an overdiagnosis of septate uteri by the ESHRE–ESGE system was confirmed in the general population compared to the diagnosis by the ASRM classification supplemented with morphometric criteria, as proposed by Ludwin [20].
Does the ESHRE–ESGE classification also significantly increase the diagnoses of septate uteri in infertile patients, and what is the agreement in septate uteri recognition among the three systems (ESHRE–ESGE vs. ASRM by Salim vs. ASRM by Ludwin)? The main objective of this study was to compare the recognition of septate uteri in infertile women via these three classifications.
Methods
Patients
This retrospective study was approved by the Institutional Review Board of the Reproductive and Genetic Hospital of CITIC-Xiangya. Infertile women who visited our hospital for assessment and treatment from June 2013 to December 2016 were recruited.
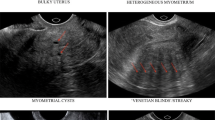
Only non-pregnant women younger than 45 years of age were recruited. Three-dimensional (3D) transvaginal sonography (TVS) scans were administered during the routine examinations of all patients to evaluate their uterine shape in our hospital. Patients who were found to have lesions in the myometrium of the uterine fundus, had a uterine fibroid/polyp distorting the endometrial cavity, had undergone surgeries that may have affected the original shape of the uterine cavity or had an ultrasound view that was insufficient to establish a definitive diagnosis, were excluded. The data from 53,540 patients were analysed. Written informed consent was obtained from all participants.
Diagnostic methods
A 3D-TVS scan combined with a gynaecological examination was routinely performed to assess the anatomy of the uterus. TVS scans were performed with GE VOLUSON E8/730 (General Electric Tech Co., Ltd., New York, USA) equipped with a 5–9 MHz transvaginal colour Doppler probe during the late follicular phase (days 10–14) of the menstrual cycle by experienced sonographers and were repeated during the luteal phase (days 15–28) if the initial examination was insufficiently clear. Women with irregular cycles and amenorrhoea were diagnosed regardless on any day of the cycle outside of the menstruation period.
The ultrasound technique included an initial 2D ultrasound assessment of the pelvis to exclude obvious pathology. The region of interest, which included the entire uterus and the upper cervix, was then selected for volume acquisition. Once an adequate data set had been acquired, the 3D data were saved in numbered format to the hard drive of the ultrasound machine.
If a patient was suspected of having a congenital uterine malformation during examination, a more senior doctor was asked to consult. Therefore, the diagnosis of a congenital uterine anomaly was the judgement of at least two sonographers. The data were analysed by the ESHRE–ESGE system [17, 21], the ASRM by Salim [13] and the ASRM by Ludwin [14,15,16] separately. The concordance of diagnoses of septate uteri using these three systems were then compared.
Statistical analysis
SPSS version 17.0 software (SPSS, Inc., Chicago, IL, USA) was used to perform statistical analyses. Measurement data are expressed as the mean ± standard deviation (SD), and differences in the means between two groups were analysed using Student’s t test. Enumerated data are expressed as rates (percentage), and two sets of rates were compared using the Chi-square test or Fisher’s exact test. The kappa (k)-value was interpreted to evaluate the agreement as follows: poor, < 0.20; fair, 0.21–0.40; moderate, 0.41–0.60; substantial/good, 0.61–0.80; and almost perfect/very good, 0.81–1.00 [22]. A value of p < 0.05 was considered significant.
Results
The age of the studied women was 29.82 ± 4.45 years, the body mass index (BMI) was 21.46 ± 2.74 and the infertility duration was 5.63 ± 3.82 years. Female factor was the most common infertility factor, and the second was the combined female and male factors. Most women came for secondary infertility (31,947, 59.67%). Among the secondary infertile patients, 23.14% (7394) had previous live deliveries, 25.45% (8131) had previous miscarriages and 7.78% (2485) had a history of recurrent miscarriage. The details of the clinical characteristics are shown in Table 1.
Among the 53,540 infertile women, 11.31% (6056) were found to have septate uteri using the ESHRE–ESGE classification system, while 7.20% (3854) and 3.80% (2034) were diagnosed according to the ASRM by Salim and by Ludwin, respectively. The incidence of septate uteri was significantly higher in the primary infertile patients than that in the secondary infertile patients (12.06%, 2604/21,593 vs. 10.80%, 3450/31,947, p < 0.001) according to the ESHRE–ESGE system, while the incidence was similar between primary and secondary infertile patients using either the ASRM by Salim (7.13%, 1539/21,593 vs. 7.32%, 2338/31,947, p = 0.403) or the ASRM by Ludwin system (3.75%, 809/21,593 vs. 3.92%, 1252/31,947, p = 0.684). Good agreement was noted for the differentiation of septate uteri between the ESHRE–ESGE system and the ASRM by Salim (k = 0.686, p < 0.001) and between the ASRM by Salim and by Ludwin (k = 0.671, p < 0.001). The ESHRE–ESGE system and the ASRM by Ludwin exhibited moderate agreement in diagnosing septate uteri (k = 0.444, p < 0.001) (Table 2).
The length of the internal indentation and the rate of the internal indentation/uterine wall thickness in partial septate uteri identified by the ESHRE–ESGE system were significantly lower than those found using the ASRM by Salim (8.82 ± 4.61 vs. 12.12 ± 3.46 mm, p < 0.001; 0.86 ± 0.37 vs. 1.39 ± 0.30, p < 0.001) and by Ludwin (8.82 ± 4.61 vs. 18.58 ± 3.79 mm, p < 0.001; 0.86 ± 0.37 vs. 1.99 ± 0.98, p < 0.001). Additionally, the length of the internal indentation and the rate of the internal indentation/uterine wall thickness in partial septate uteri identified using the ASRM by Salim were significantly lower than those diagnosed using the ASRM by Ludwin. While the length of the internal indentation (ESHRE–ESGE: 8.90 ± 3.91 vs. 8.81 ± 3.86 mm, p = 0.376; ASRM by Salim: 11.95 ± 1.84 vs. 12.74 ± 2.78 mm, p = 0.474; ASRM by Ludwin: 18.63 ± 2.56 vs. 19.30 ± 3.88 mm, p = 0.392) and the rate of the internal indentation/uterine wall thickness in partial septate uteri (ESHRE–ESGE: 0.88 ± 0.43 vs. 0.87 ± 0.69, p = 0.593; ASRM by Salim: 1.37 ± 0.26 vs. 1.40 ± 0.23, p = 0.843; ASRM by Ludwin: 1.97 ± 0.73 vs. 2.03 ± 1.35, p = 0.874) were similar between the primary and secondary infertile patients using all three systems.
The distributions of the internal indentation length of partial septate uteri were markedly different among the three systems (p < 0.001); most cases exhibited a length < 10 mm according to the ESHRE–ESGE system (48.01%), whereas most cases exhibited a length > 15 mm according to the ASRM by Salim (54.34%) and by Ludwin (100%) (Table 3).
Discussion
In this study, we compared septate uterus recognition in infertile patients using three systems and found good agreement between the ESHRE–ESGE and ASRM by Salim and between the ASRM by Salim and by Ludwin, while moderate agreement was found between the ESHRE–ESGE and ASRM by Ludwin systems. Ludwin’s criteria are the strictest, while the ESHRE–ESGE system is much more relaxed in the recognition of a septate uterus, which significantly increases the frequency of septate uteri identification. To our knowledge, this is the first study to compare these 3 classification systems for diagnosing septate uteri.
Among the same studied population, the ESHRE–ESGE system significantly increased the frequency of septate uterus diagnoses relative to the other two ASRM supplemental classifications (11.31% vs. 7.20% vs. 3.80%), consistent with findings in the general population [20]. The ESHRE–ESGE system diagnoses septate uteri based on the rate of the internal indentation/uterine wall thickness without providing detailed values of the internal indentation, and this system removed the classification of an “arcuate uterus” [10]. The result is an extraordinary increase in diagnoses of septate uteri, which may lead to a risk of overtreatment [17, 21]. Additionally, only infertile patients were included in this study which might also have a relevance of the over-diagnosis of mild subseptate uterus compared to previous studies including women from the general population [20]. Therefore, the current ESHRE–ESGE classification system may still require improvements. For example, this system could further divide septate uteri into subgroups according to the length of the septum or the co-factors that are associated with poor reproductive outcomes, which would be meaningful for clinical use. Furthermore, it is very important to define the clinical meaning of an arcuate uterus and to determine whether it should still be used because a large proportion of partial septate uteri diagnosed by the ESHRE–ESGE system were arcuate uteri according to both the supplemental ASRM systems in this study; however, the recent ASRM guidelines include arcuate and normal uteri in one group [23].
The original ASRM system did not provide measuring parameters to define a septate uterus [6]. Supplemental classifications have been proposed to better classify uterine anomalies. In supplemental classifications, the angle or absolute length of the septum was used to diagnose a septate uterus. The absolute length of the internal indentation was used in the ASRM by Ludwin [15, 16]: a septate uterus had a depth ≥ 15 mm, an arcuate uterus had a depth between 10 and 15 mm and a normal uterus had a depth < 10 mm. In the ASRM by Salim [13], when the central point of the internal indentation is < 90°, a septate uterus is diagnosed; an arcuate uterus is diagnosed with an angle > 90°. In this study, these two supplemental classifications showed relatively good consistency (k = 0.671) in the recognition of a septate uterus, which suggests that both the angle and the absolute length are powerful tools in the recognition of a septate uterus. However, Ludwin’s standard seems stricter than Salim’s, with fewer septate uteri recognised (2034 vs. 3854), and thus, Ludwin’s standard exhibited worse concordance with the ESHRE-ESGE system than Salim’s (0.444 vs. 0.686). The relatively poor agreement between the ESHRE-ESGE and the ASRM by Ludwin was consistent with previous results for the general population [20].
The internal indentation length and the rate of the internal indentation/uterine wall thickness in a partial septate uterus identified by the ESHRE–ESGE system were significantly less than those in the two supplemental ASRM systems, and Ludwin’s criteria had the highest numerical value, consistent with the results of Ludwin et al. [20]. Most of the internal indentations were < 10 mm (48.01%) based on the ESHRE–ESGE system, while only 3.01% had an indentation length < 10 mm according to Salim’s criteria and all had an internal indentation length ≥ 15 mm according to Ludwin’s criteria. These results suggest that among these three systems, Ludwin’s criteria are the strictest, while the ESHRE–ESGE system is much more relaxed in the diagnosis of a septate uterus.
According to recent guidelines for a septate uterus [23], criteria proposed by both Salim and Ludwin were officially endorsed by the ASRM, which further demonstrates the diagnostic value of both the angle and the absolute length. In the new guidelines, normal and arcuate uteri are combined into one group, with an indentation < 10 mm and an angle > 90°, while a septate uterus is defined as an indentation > 15 mm and an angle < 90°. However, this guideline has not mentioned how to classify an indentation between 10 mm–15 mm. To our knowledge, there has been no universally accepted classification system until now. Although new classifications are constantly being proposed, even the newest classification still has some limitations and requires improvements.
Our study has several strengths. The large sample size allowed us to conduct comparisons among the three classifications. One limitation is that our analysis was based on 3D-TVS examinations and was not further compared with hysteroscopic and/or laparoscopic results. In addition, the participants were confined to infertile patients and, therefore, whether the results relevant to Salim’s criteria could be the same as the general population requires further evaluation.
Conclusions
In summary, good agreement was found between the ESHRE–ESGE classification and the ASRM system by Salim and between the ASRM systems by Salim and by Ludwin in the recognition of a septate uterus, while moderate agreement was found between the ESHRE–ESGE classification and the ASRM system by Ludwin. The ESHRE–ESGE classification significantly increased the frequency of septate uteri in infertile women, which may cause the risk of overtreatment. Therefore, the ESHRE–ESGE system should be used with caution when guiding hysteroscopic metroplasty in infertile patients.
Abbreviations
- AFS:
-
American Fertility Society
- ASRM:
-
American Society of Reproductive Medicine
- VCUAM:
-
Vagina, cervix, uterus, adnex-associated malformations
- ESHRE–ESGE:
-
European Society of Human Reproduction and Embryology–European Society for Gynaecological Endoscopy
- 3D:
-
Three-dimensional
- TVS:
-
Transvaginal sonography
- SD:
-
Standard deviation
- BMI:
-
Body mass index
References
Devi Wold AS, Pham N, Arici A (2006) Anatomic factors in recurrent pregnancy loss. Semin Reprod Med 24:25–32
Acien P, Acien M (2016) The presentation and management of complex female genital malformations. Hum Reprod Update 22:48–69
Raga F, Bauset C, Remohi J, Bonilla-Musoles F, Simon C, Pellicer A (1997) Reproductive impact of congenital Mullerian anomalies. Hum Reprod 12:2277–2281
Golan A, Schneider D, Avrech O, Raziel A, Bukovsky I, Caspi E (1992) Hysteroscopic findings after missed abortion. Fertil Steril 58:508–510
Grimbizis GF, Camus M, Tarlatzis BC, Bontis JN, Devroey P (2001) Clinical implications of uterine malformations and hysteroscopic treatment results. Hum Reprod Update 7:161–174
The American Fertility Society (1988) The American Fertility Society classifications of adnexal adhesions, distal tubal occlusion, tubal occlusion secondary to tubal ligation, tubal pregnancies, mullerian anomalies and intrauterine adhesions. Fertil Steril 49:944–955
Acien P, Acien M, Sanchez-Ferrer M (2004) Complex malformations of the female genital tract. New types and revision of classification. Hum Reprod 19:2377–2384
Acien P, Acien MI (2011) The history of female genital tract malformation classifications and proposal of an updated system. Hum Reprod Update 17:693–705
Oppelt P, Renner SP, Brucker S, Strissel PL, Strick R, Oppelt PG, Doerr HG, Schott GE, Hucke J, Wallwiener D, Beckmann MW (2005) The VCUAM (Vagina Cervix Uterus Adnex-associated Malformation) classification: a new classification for genital malformations. Fertil Steril 84:1493–1497
Grimbizis GF, Gordts S, Di Spiezio Sardo A, Brucker S, De Angelis C, Gergolet M, Li TC, Tanos V, Brolmann H, Gianaroli L, Campo R (2013) The ESHRE/ESGE consensus on the classification of female genital tract congenital anomalies. Hum Reprod 28:2032–2044
Smit JG, Overdijkink S, Mol BW, Kasius JC, Torrance HL, Eijkemans MJ, Bongers M, Emanuel MH, Vleugels M, Broekmans FJ (2015) The impact of diagnostic criteria on the reproducibility of the hysteroscopic diagnosis of the septate uterus: a randomized controlled trial. Hum Reprod 30:1323–1330
Henmi H, Soyama H, Nagasawa K, Ikeda U (2015) Safe and effective surgery for septate uterus: 21 cases treated by hysteroscopic metroplasty with hysterography and custom-made intra-uterine silicone plate. J Minim Invasive Gynecol 22:S180
Salim R, Woelfer B, Backos M, Regan L, Jurkovic D (2003) Reproducibility of three-dimensional ultrasound diagnosis of congenital uterine anomalies. Ultrasound Obstet Gynecol 21:578–582
Bermejo C, Ten Martinez P, Cantarero R, Diaz D, Perez Pedregosa J, Barron E, Labrador E, Ruiz Lopez L (2010) Three-dimensional ultrasound in the diagnosis of Mullerian duct anomalies and concordance with magnetic resonance imaging. Ultrasound Obstet Gynecol 35:593–601
Ludwin A, Pitynski K, Ludwin I, Banas T, Knafel A (2013) Two- and three-dimensional ultrasonography and sonohysterography versus hysteroscopy with laparoscopy in the differential diagnosis of septate, bicornuate, and arcuate uteri. J Minim Invasive Gynecol 20:90–99
Ludwin A, Ludwin I, Pitynski K, Banas T, Jach R (2013) Differentiating between a double cervix or cervical duplication and a complete septate uterus with longitudinal vaginal septum. Taiwan J Obstet Gynecol 52:308–310
Ludwin A, Ludwin I, Pitynski K, Jach R, Banas T (2014) Are the ESHRE/ESGE criteria of female genital anomalies for diagnosis of septate uterus appropriate? Hum Reprod 29:867–868
Ludwin A, Ludwin I, Pitynski K, Banas T, Jach R (2014) Role of morphologic characteristics of the uterine septum in the prediction and prevention of abnormal healing outcomes after hysteroscopic metroplasty. Hum Reprod 29:1420–1431
Ludwin A, Ludwin I (2015) Diagnostic rate and accuracy of the ESHRE-ESGE classification for septate uterus and other common uterine malformations: why do we not see that the Emperor is naked? Ultrasound Obstet Gynecol 46:634–636
Ludwin A, Ludwin I (2015) Comparison of the ESHRE-ESGE and ASRM classifications of Mullerian duct anomalies in everyday practice. Hum Reprod 30:569–580
Grimbizis GF, Gordts S, Di Spiezio Sardo A, Brucker SY, De Angelis C, Gergolet M, Li TC, Tanos V, Brolmann HH, Gianaroli L, Campo R (2014) Reply: are the ESHRE/ESGE criteria of female genital anomalies for diagnosis of septate uterus appropriate? Hum Reprod 29:868–869
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Practice Committee of the American Society for Reproductive Medicine: (2016) Uterine septum: a guideline. Fertil Steril 106:530–540
Acknowledgements
The authors thank Qingqing Wu and Kailan Xiong for their assistance in collecting and sorting clinical data.
Availability of data and materials
The data sets used and/or analysed during the current study are available from the corresponding author on reasonable request. All data generated or analysed during this study are included in this published article.
Funding
This work was funded by the Science and technology project of Health and Family Planning Commission of Hunan Province (No. C20180898) and the CITIC-Xiangya Research Fund (No. KYXM-201703).
Author information
Authors and Affiliations
Contributions
YO and YY collected relevant clinical data. YO conducted statistical analyses and drafted the manuscript. FG and G L helped to collect relevant clinical data and have been involved in revising the manuscript. XL conceived of the study, and participated in drafting this manuscript. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Consent for publication
Not applicable.
Declaration
The authors report no financial or commercial conflicts of interest.
Ethics approval and consent to participate
This retrospective study was approved by the Institutional Review Board of the Reproductive and Genetic Hospital of Citic-Xiangya.
Rights and permissions
About this article
Cite this article
Ouyang, Y., Yi, Y., Gong, F. et al. ESHRE–ESGE versus ASRM classification in the diagnosis of septate uterus: a retrospective study. Arch Gynecol Obstet 298, 845–850 (2018). https://doi.org/10.1007/s00404-018-4878-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-018-4878-2