Abstract
Purpose
In this case–control study, the impact on quality of life and sexual function in women with cervical dysplasia and conization will be evaluated, in order to address coping with such a premalignant lesion and to improve strategies for salutogenesis.
Methods
This multicenter case–control study evaluates women at special dysplasia outpatient clinic (T1) as well as 3 (T2) and 6 (T3) months after the diagnosis of a dysplasia. The women were subgrouped upon dysplasia only (S2) or dysplasia with conization (S1). Sexual function as well as cervix-related and general quality of life was assessed using validated instruments (FSFI-d, EORTC-QLQ-CX24, SF-36).
Results
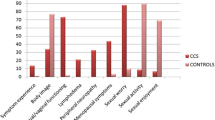
Women with dysplasia had a lower sexual functioning than controls (FSFI: S1: 23.8 ± 9.7 (p < 0.003); S2: 25.3 ± 7.5 (p < 0.03); K: 29.1 ± 4.5) as well as a lower physical component score (SF-36: S1: 51.3 ± 8.6 (p < 0.02); S2: 51.7 ± 7.8 (p < 0.05); K: 54.2 ± 6.6) and had a significantly reduced body image (EORTC-QLQ-CX24: S1: 75.7 (p < 0.001); S2: 76.5 (p < 0.001), K:89.2). Sexual functioning was not affected by conization in the observational period over 6 months; however, sexual worry was impacted. Over temporal progression women who underwent conization worried more. Regression analysis revealed a cervical dysplasia to impact sexual function.
Conclusion
Data suggest that women with the diagnosis of a cervical dysplasia are impaired in their sexual function as well as general and cervix-related quality of life, mostly independent of conization or further observation. To improve salutogenesis in the long run, the communication on dysplasia and its treatment strategy at the beginning, as well as part of aftercare, or psychosomatic intervention, might be treatment options for women at risk.





Similar content being viewed by others
References
Schneider A et al (2000) Screening for high-grade cervical intra-epithelial neoplasia and cancer by testing for high-risk HPV, routine cytology or colposcopy. Int J Cancer 89(6):529–534
Melnikow J et al (1998) Natural history of cervical squamous intraepithelial lesions: a meta-analysis. Obstet Gynecol 92((4, Part 2)):727–735
Schneider A et al (2007) Sekundäre Prävention des Zervixkarzinoms: aktueller Stand der Diagnostik. Der Gynäkologe 40(5):377–388
Robert Koch Institut (2014) Neuerungen in den aktuellen Empfehlungen der Ständigen Impfkomission am RKI vom August 2014. Epid Bull 35:342–350
Wozniak J et al (2000) Comparison of the CO2 laser and leep–loop method in treatment of changes in uterine cervix. Laser Technol VI Appl 4238:93–95
Mathevet P et al (1994) A randomized prospective study comparing three techniques of conization: cold knife, laser, and leep. Gynecol Oncol 54(2):175–179
Jancar N, Ponikvar BM, Tomsic S (2016) Cold-knife conisation and large loop excision of transformation zone significantly increase the risk for spontaneous preterm birth: a population-based cohort study. Eur J Obstet Gynecol Reprod Biol 203:245–249
Carter J et al (2012) Contemporary quality of life issues affecting gynecologic cancer survivors. Hematol Oncol Clin North Am 26(1):169–194
Bennett N et al (2016) Cancer, benign gynecology, and sexual function-issues and answers. J Sex Med 13(4):519–537
Correa CS et al (2016) Sexual function of women surviving cervical cancer. Arch Gynecol Obstet 293(5):1053–1063
Song T et al (2012) Sexual function after surgery for early-stage cervical cancer: is there a difference in it according to the extent of surgical radicality? J Sex Med 9(6):1697–1704
Phd JW, Msc AP, Mrcgp DS (1995) Psychological consequences of positive results in cervical cancer screening. Psychol Health 10(3):185–194
Lerman C et al (1991) Adverse psychologic consequences of positive cYtologic cervical screening. Am J Obstet Gynecol 165(3):658–662
Sporn NJ et al (2015) Sexual health communication between cancer survivors and providers: how frequently does it occur and which providers are preferred? Psychooncology 24(9):1167–1173
Bober SL, Carter J, Falk S (2013) Addressing female sexual function after cancer by internists and primary care providers. J Sex Med 10(Suppl 1):112–119
Rosen R, Brown C, Heiman J, Leiblum S, Meston C, Shabsigh R, Ferguson D, D’Agostino R (2000) The female sexual function index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther 26(2):191–208
Berner M et al (2004) Überprüfung der Gültigkeit und Zuverlässigkeit des deutschen Female Sexual Function Index (FSFI-d). Geburtshilfe Frauenheilkd 64(3):293–303
Wiegel M, Meston C, Rosen R (2005) The female sexual function index (FSFI): cross-validation and development of clinical cutoff scores. J Sex Marital Ther 31(1):1–20
Bullinger M, Kirchberger I, Ware J (1995) Der deutsche SF-36 Health Survey Übersetzung und psychometrische Testung eines krankheitsübergreifenden Instruments zur Erfassung der gesundheitsbezogenen Lebensqualität. Zeitschrift für Gesundheitswissenschaften = J Public Health 3(1):21–36
Brazier JE et al (1992) Validating the SF-36 health survey questionnaire: new outcome measure for primary care. BMJ 305(6846):160–164
Carter J et al (2010) A 2-year prospective study assessing the emotional, sexual, and quality of life concerns of women undergoing radical trachelectomy versus radical hysterectomy for treatment of early-stage cervical cancer. Gynecol Oncol 119(2):358–365
Benedict C et al (2016) Body image and sexual function in women after treatment for anal and rectal cancer. Psychooncology 25(3):316–323
Donovan KA, Thompson LM, Hoffe SE (2010) Sexual function in colorectal cancer survivors. Cancer Control 17(1):44–51
Morreale MK (2011) The impact of cancer on sexual function. Adv Psychosom Med 31:72–82
Khalil J et al (2015) Impact of cervical cancer on quality of life: beyond the short term (Results from a single institution): quality of life in long-term cervical cancer survivors: results from a single institution. Gynecol Oncol Res Pract 2:7
Bober SL, Varela VS (2012) Sexuality in adult cancer survivors: challenges and intervention. J Clin Oncol 30(30):3712–3719
Maseroli E et al (2016) Which are the male factors associated with female sexual dysfunction (FSD)? Andrology 4(5):911–920
Singer S et al (2010) Patients’ acceptance and psychometric properties of the EORTC QLQ-CX24 after surgery. Gynecol Oncol 116(1):82–87
Lindau ST, Abramsohn EM, Matthews AC (2015) A manifesto on the preservation of sexual function in women and girls with cancer. Am J Obstet Gynecol 213(2):166–174
Lindau ST, Gavrilova N, Anderson D (2007) Sexual morbidity in very long term survivors of vaginal and cervical cancer: a comparison to national norms. Gynecol Oncol 106(2):413–418
Acknowledgements
We thank all participants in the study, as well as the staff from the dysplasia consultation and outpatient clinics supporting this study.
Author information
Authors and Affiliations
Contributions
JH data collection, data management, data analysis, manuscript writing, manuscript editing. JB project development, patient recruitment, manuscript editing. TB data analysis, manuscript editing. CD patient recruitment, manuscript editing. JH project development, patient recruitment, manuscript editing. ND patient recruitment, manuscript editing. SS project development, manuscript editing. CS project development, manuscript editing. JR project development, manuscript editing. TCS project development, manuscript writing, manuscript editing. SS project development, data collection, data analysis, manuscript writing, manuscript editing
Corresponding author
Ethics declarations
Conflict of interest
There is no conflict of interest by any author. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Ethical standards
This study was approved by the local ethical committee in Heidelberg (S-399/2015), Leipzig (091/17-lk) and Regensburg (16-377-103). All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Heinzler, J., Brucker, J., Bruckner, T. et al. Impact of a cervical dysplasia and its treatment on quality of life and sexual function. Arch Gynecol Obstet 298, 737–745 (2018). https://doi.org/10.1007/s00404-018-4853-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-018-4853-y