Abstract
Objective
To explore the feasibility of three-dimensional (3D) transperineal ultrasound on the observation of paravaginal support in nulliparous and postpartum women.
Methods
Volume datasets were acquired in 50 nulliparous and 100 postpartum women using 3D transperineal ultrasound. Paravaginal supports were observed by studying the vaginal cross-sectional morphology. The extent of paravaginal support in specific level were evaluated by counting out at a 2 mm interval in tomographic ultrasound imaging mode in all subjects. The Mann–Whitney U test were applied to establish comparisons between the two groups.
Results
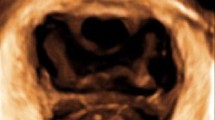
Three representative manifestations of vaginal cross-sectional morphology corresponding to different paravaginal support were presented from the dorsal side to the caudal side, both in nulliparous women and postpartum women. The extent of paravaginal support in middle vagina was 11 slices (range 9–12) in nulliparous women and 7 slices (range 4–10) in postpartum women (P < 0.05).
Conclusion
This pilot study confirmed that it was feasible to indirectly study paravaginal support by observing the vaginal cross-sectional morphology using 3D transperineal ultrasound.



Similar content being viewed by others
References
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, Monga A, Petri E, Rizk DE, Sand PK, Schaer GN (2010) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. International Urogynecological Association; International Continence Society. Neurourol Urodyn 29(1):4–20
Papa Petros P, Ulmsten U (1990) An integral theory of female urinary incontinence. Experimental and clinical considerations. Acta Obstet Gynecol Scand 153:7–31
Petros PEP, Woodman PJ (2008) The integral theory of continence. Int Urogynecol J Pelvic Floor Dysfunct 19:35–40
DeLancey JO (1992) Anatomic aspects of vaginal eversion after hysterectomy. Am J Obstet Gynecol 166:1717–1724
DeLancey J (1994) Structural support of the urethra as it relates to stress urinary incontinence: the hammock hypothesis. Am J Obstet Gynecol 170:1713–1720
van Delft K, Sultan AH, Thakar R, Schwertner-Tiepelmann N, Kluivers K (2014) The relationship between postpartum levator ani muscle avulsion and signs and symptoms of pelvic floor dysfunction. BJOG 121(9):1164–1171
Dietz HP, Pattillo Garnham A, Rojas Guzmán (2017) Is it necessary to diagnose levator avulsion on pelvic floor muscle contraction? Ultrasound Obstet Gynecol 49(2):252–256
Ying T, Li Q, Xu L, Liu F, Hu B (2012) Three-dimensional ultrasound appearance of pelvic floor in nulliparous women and pelvic organ prolapse women. Int J Med Sci 9(10):894–900
Dietz HP, Shek C, De Leon J, Steensma AB (2008) Ballooning of the levator hiatus. Ultrasound Obstet Gynecol 31(6):676–680
Dietz HP, Franco AV, Shek KL, Kirby A (2012) Avulsion injury and levator hiatal ballooning: two independent risk factors for prolapse? An observational study. Acta Obstet Gynecol Scand 91(2):211–214
Rostaminia G, White D, Hegde A, Quiroz LH, Davila GW, Shobeiri SA (2013) Levator ani deficiency and pelvic organ prolapse severity. Obstet Gynecol 121(5):1017–1024
Dietz HP, Severino M, Kamisan Atan I, Shek KL, Rojas Guzman (2016) Warping of the levator hiatus: how significant is it? Ultrasound Obstet Gynecol 48(2):239–242
Dietz HP, Shek KL (2009) Tomographic ultrasound imaging of the pelvic floor: which levels matter most? Ultrasound Obstet Gynecol 33(6):698–703
Yan Y, Dou C, Wang X, Xi Y, Hu B, Ma L, Ying T (2017) Combination of tomographic ultrasound imaging and three-dimensional magnetic resonance imaging-based model to diagnose postpartum levator avulsion. Sci Rep 7(1):11235
Dumoulin C, Peng Q, Stodkilde-Jorgensen H, Shishido K, Constantinou C (2007) Changes in levator ani anatomical configuration following physiotherapy in women with stress urinary incontinence. J Urol 178(3 Pt 1):970–977
Khatri G, Carmel ME, Bailey AA, Foreman MR, Brewington CC, Zimmern PE, Pedrosa I (2016) Postoperative imaging after surgical repair for pelvic floor dysfunction. Radiographics 36(4):1233–1256
Betschart C, Kim J, Miller JM, Ashton-Miller JA, DeLancey JO (2014) Comparison of muscle fiber directions between different levator ani muscle subdivisions: in vivo MRI measurements in women. Int Urogynecol J 25(9):1263–1268
Schofield MLA, Higgs P, Hawnaur JM (2005) MRI findings following laparoscopic sacrocolpopexy. Clin Radiol 60(3):333–339
Tunn R, Delancey JO, Howard D, Ashton-Miller JA, Quint LE (2003) Anatomic variations in the levator ani muscle, endopelvic fascia, and urethra in nulliparas evaluated by magnetic resonance imaging. Am J Obstet Gynecol 188(1):116–121
van Delft K, Thakar R, Sultan AH, Kluivers KB (2015) Does the prevalence of levator ani muscle avulsion differ when assessed using tomographic ultrasound imaging at rest vs on maximum pelvic floor muscle contraction? Ultrasound Obstet Gynecol 46(1):99–103
Macura KJ (2006) Magnetic resonance imaging of pelvic floor defects in women. Top Magn Reson Imaging 17(6):417–426
Athanasiou S, Chaliha C, Toozs-Hobson P, Salvatore S, Khullar V, Cardozo L (2007) Direct imaging of the pelvic floor muscles using two-dimensional ultrasound: a comparison of women with urogenital prolapse versus controls. BJOG 114(7):882–888
Haylen BT, Maher CF, Barber MD, Camargo S, Dandolu V, Digesu A, Goldman HB, Huser M, Milani AL, Moran PA, Schaer GN, Withagen MI (2016) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic organ prolapse (POP). Int Urogynecol J Pelvic Floor Dysfunct 27(4):655–684
Ingelman-Sundberg A, Ulmsten U (1983) Surgical treatment of female urinary stress incontinence. Contrib Gynecol Obstet 10:51–69
Richardson AC, Edmonds PB, Williams NL (1981) Treatment of stress urinary incontinence due to paravaginal fascial defect. Obstet Gynecol 57(3):357–362
Richardson AC, Lyon JB, Williams NL (1976) A new look at pelvic relaxation. Am J Obstet Gynecol 126(5):568–573
White GR (1909) Cystocele—a radical cure by suturing lateral sulci of the vagina to the white line of pelvic fascia. Int Urogynecol J Pelvic Floor Dysfunct 8(5):288–292
Martan A, Masata J, Halaska M, Otcenásek M, Svabik K (2002) Ultrasound imaging of paravaginal defects in women with stress incontinence before and after paravaginal defect repair. Ultrasound Obstet Gynecol 19(5):496–500
Nguyen JK, Hall CD, Taber E, Bhatia NN (2000) Sonographic diagnosis of paravaginal defects: a standardization of technique. Int Urogynecol J Pelvic Floor Dysfunct 11(6):341–345
Ostrzenski A, Osborne NG (1998) Ultrasonography as a screening tool for paravaginal defects in women with stress incontinence: a pilot study. Int Urogynecol J Pelvic Floor Dysfunct 9(4):195–199
Huebner M, Margulies RU, DeLancey JO (2008) Pelvic architectural distortion is associated with pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct 19(6):863–867
Tillack AA, Joe BN, Yeh BM, Jun SL, Kornak J, Zhao S, Deng D (2015) Vaginal shape at resting pelvic MRI: predictor of pelvic floor weakness? Clin Imaging 39(2):285–288
Acknowledgements
National Science Foundation of China is acknowledged for providing financial support to this work (No. 81571699).
Author information
Authors and Affiliations
Contributions
CD: project development, manuscript writing, data collection. QL: project development, data collection, manuscript writing. TY: conceptualization, funding acquisition. WS: data collection. YY: methodology. YL: data analysis. XW: data analysis.
Corresponding authors
Ethics declarations
Ethical approval
This study was approved by the Ethics Committee of Shanghai Jiao Tong University Affiliated Sixth People’s Hospital. All procedures performed in the study involving human participants were in accordance with the 1964 Helsinki declaration and its later amendments.
Conflict of interest
We declare that there are no conflict of interest.
Rights and permissions
About this article
Cite this article
Dou, C., Li, Q., Ying, T. et al. Value of transperineal ultrasound on the observation of paravaginal support. Arch Gynecol Obstet 297, 943–949 (2018). https://doi.org/10.1007/s00404-018-4659-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-018-4659-y