Abstract
Introduction
Surgical equipment, and especially the so-called ‘splash basins’ that are used intraoperatively, are a potential source of bacterial contamination in primary total hip arthroplasty (THA). With this risk in mind, many commercially available draping kits include plastic bags that can be used to collect fluid or to temporarily store instruments. Following this rationale, we hypothesised that first: the fluid collection bags are a potential reservoir of bacteria and second: there is a time dependency for bacterial contamination.
Materials and methods
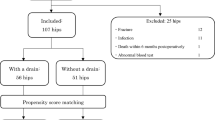
After ethics approval, we investigated in a prospective, internally controlled, non-blinded trial 43 patients who received primary THA. At the beginning of the surgery, we took deep, representative, intracapsular tissue samples, which served as negative controls. At the end of surgery, tissue samples were taken from the bottom of the ‘fluid collection bag’ for microbiological analysis.
Results
All 86 control samples were negative. Out of the samples taken from the bags, a pathogen could be detected in four patients (9.3%). All pathogens were detected after a surgery time lasting longer than 90 min.
Conclusion
We were able to show that fluid collection bags are a potential reservoir for bacteria in THA when surgery time was greater than a 90-min threshold. Our data suggest that the risks from fluid collection bags outweigh the advantages of using them. Therefore, we recommend against the use of fluid collection bags intraoperatively in primary THA.

Similar content being viewed by others
References
Kapadia BH, Banerjee S, Cherian JJ, Bozic KJ, Mont MA (2016) The economic impact of periprosthetic infections after total hip arthroplasty at a specialized tertiary-care center. J Arthroplast 31(7):1422–1426. https://doi.org/10.1016/j.arth.2016.01.021
Kapadia BH, McElroy MJ, Issa K, Johnson AJ, Bozic KJ, Mont MA (2014) The economic impact of periprosthetic infections following total knee arthroplasty at a specialized tertiary-care center. J Arthroplast 29(5):929–932. https://doi.org/10.1016/j.arth.2013.09.017
Parisi TJ, Konopka JF, Bedair HS (2017) What is the long-term economic societal effect of periprosthetic infections after THA? A Markov analysis. Clin Orthop Relat Res 475(7):1891–1900. https://doi.org/10.1007/s11999-017-5333-6
Webb BG, Lichtman DM, Wagner RA (2008) Risk factors in total joint arthroplasty: comparison of infection rates in patients with different socioeconomic backgrounds. Orthopedics 31(5):445
Shohat N, Parvizi J (2017) Prevention of periprosthetic joint infection: examining the recent guidelines. J Arthroplast 32(7):2040–2046. https://doi.org/10.1016/j.arth.2017.02.072
Wimmer MD, Randau TM, Friedrich MJ, Ploeger MM, Schmolder J, Strauss AC, Pennekamp PH, Vavken P, Gravius S (2016) Outcome predictors in prosthetic joint infections—validation of a risk stratification score for prosthetic joint infections in 120 cases. Acta Orthop Belg 82(1):143–148
Shirley OC, Bayan A, Zhu M, Dalton JP, Wiles S, Young SW (2017) Do surgical helmet systems affect intraoperative wound contamination? A randomised controlled trial. Arch Orthop Trauma Surg 137(11):1565–1569. https://doi.org/10.1007/s00402-017-2795-7
Al-Maiyah M, Bajwa A, Mackenney P, Port A, Gregg PJ, Hill D, Finn P (2005) Glove perforation and contamination in primary total hip arthroplasty. J Bone Jt Surg Br 87(4):556–559. https://doi.org/10.1302/0301-620X.87B4.15744
Beldame J, Lagrave B, Lievain L, Lefebvre B, Frebourg N, Dujardin F (2012) Surgical glove bacterial contamination and perforation during total hip arthroplasty implantation: when gloves should be changed. Orthop Traumatol Surg Res 98(4):432–440. https://doi.org/10.1016/j.otsr.2011.10.015
Davis N, Curry A, Gambhir AK, Panigrahi H, Walker CR, Wilkins EG, Worsley MA, Kay PR (1999) Intraoperative bacterial contamination in operations for joint replacement. J Bone Jt Surg Br 81(5):886–889
Kaya I, Ugras A, Sungur I, Yilmaz M, Korkmaz M, Cetinus E (2012) Glove perforation time and frequency in total hip arthroplasty procedures. Acta Orthop Traumatol Turc 46(1):57–60
Mulcahy DM, McCormack D, McElwain JP (1994) Intraoperative suction catheter tip contamination. J R Coll Surg Edinb 39(6):371–373
Robinson AH, Drew S, Anderson J, Bentley G, Ridgway GL (1993) Suction tip contamination in the ultraclean-air operating theatre. Ann R Coll Surg Engl 75(4):254–256
Anto B, McCabe J, Kelly S, Morris S, Rynn L, Corbett-Feeney G (2006) Splash basin bacterial contamination during elective arthroplasty. J Infect 52(3):231–232. https://doi.org/10.1016/j.jinf.2005.06.013
Glait SA, Schwarzkopf R, Gould S, Bosco J, Slover J (2011) Is repetitive intraoperative splash basin use a source of bacterial contamination in total joint replacement? Orthopedics 34(9):e546–e549. https://doi.org/10.3928/01477447-20110714-06
Gehrke T, Parvizi J (2014) Proceedings of the international consensus meeting on periprosthetic joint infection. Foreword. J Orthop Res 32(Suppl 1):S2–S3. https://doi.org/10.1002/jor.22543
Wimmer MD, Randau TM, Petersdorf S, Pagenstert GI, Weisskopf M, Wirtz DC, Gravius S (2013) Evaluation of an interdisciplinary therapy algorithm in patients with prosthetic joint infections. Int Orthop 37(11):2271–2278. https://doi.org/10.1007/s00264-013-1995-1
Krenn V, Morawietz L, Perino G, Kienapfel H, Ascherl R, Hassenpflug GJ, Thomsen M, Thomas P, Huber M, Kendoff D, Baumhoer D, Krukemeyer MG, Natu S, Boettner F, Zustin J, Kolbel B, Ruther W, Kretzer JP, Tiemann A, Trampuz A, Frommelt L, Tichilow R, Soder S, Muller S, Parvizi J, Illgner U, Gehrke T (2014) Revised histopathological consensus classification of joint implant related pathology. Pathol Res Pract 210(12):779–786. https://doi.org/10.1016/j.prp.2014.09.017
Gundtoft PH, Pedersen AB, Varnum C, Overgaard S (2017) Increased mortality after prosthetic joint infection in primary THA. Clin Orthop Relat Res. https://doi.org/10.1007/s11999-017-5289-6
Jamsen E, Furnes O, Engesaeter LB, Konttinen YT, Odgaard A, Stefansdottir A, Lidgren L (2010) Prevention of deep infection in joint replacement surgery. Acta Orthop 81(6):660–666. https://doi.org/10.3109/17453674.2010.537805
Lidwell OM (1986) Clean air at operation and subsequent sepsis in the joint. Clin Orthop Relat Res 211:91–102
Urquhart DM, Hanna FS, Brennan SL, Wluka AE, Leder K, Cameron PA, Graves SE, Cicuttini FM (2010) Incidence and risk factors for deep surgical site infection after primary total hip arthroplasty: a systematic review. J Arthroplast 25(8):1216–1222. https://doi.org/10.1016/j.arth.2009.08.011 (e1211–1213)
Baird RA, Nickel FR, Thrupp LD, Rucker S, Hawkins B (1984) Splash basin contamination in orthopaedic surgery. Clin Orthop Relat Res 187:129–133
Zimmerli W, Trampuz A, Ochsner PE (2004) Prosthetic-joint infections. N Engl J Med 351(16):1645–1654. https://doi.org/10.1056/NEJMra040181
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The study was approved by the institutional review board of the University of Bonn, Bonn, Germany, Faculty of Medicine (IRB # 200/16).
Conflict of interest
The author(s) declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Ploeger, M.M., Jacobs, C., Gathen, M. et al. Fluid collection bags pose a threat for bacterial contamination in primary total hip arthroplasty: a prospective, internally controlled, non-blinded trial. Arch Orthop Trauma Surg 138, 1159–1163 (2018). https://doi.org/10.1007/s00402-018-2970-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-018-2970-5