Abstract
Purpose
The use of soy products is common in young children with cow milk allergy (CMA). The aim was to examine prospectively the association between infantile consumption of soy-based formula, growth parameters and early pubertal signs, in comparison to cow milk-based formula.
Methods
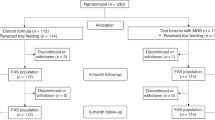
A nested case–control study was conducted, selected from a cohort of infants prospectively followed from birth until the age of 3 years for eating habits and the development of IgE-mediated CMA. Infants who consumed only soy-based formula were included in the soy group. The control group was randomly selected from those without IgE-CMA and not receiving soy formula. Study participants were reevaluated between ages 7.8 and 10.5 years by an interview, nutritional intake by 3 days diaries, and height, weight, and pubertal signs by physical examination.
Results
The soy-fed group included 29 participants (17 males), median age 8.92 years IQR (8.21, 9.42). The control group included 60 participants (27 males), median age 8.99 years IQR (8.35, 9.42). The groups had comparable height and BMI z scores (− 0.17 ± 1.08 versus − 0.16 ± 1.01, p = 0.96, and 0.67 ± 1.01 versus 0.53 ± 1.02, p = 0.56, for soy and control groups, respectively). Four (three males and one female) from the soy-group (13.8%) and eight females from the control-group (13.3%) had early pubertal signs (p = 0.95). No association was detected between puberty and infantile nutrition, after controlling for BMI and family data. No association with puberty or differences between groups were found in current daily consumption of soy, micronutrients, energy, carbohydrates, fat, and protein.
Conclusions
This is the first prospective, physical examination-based study, demonstrating no association between infantile soy-based formula consumption and growth and puberty parameters.
Similar content being viewed by others
References
Messina M, Messina V (2010) The role of soy in vegetarian diets. Nutrients 2:855–888. https://doi.org/10.3390/nu2080855
Rossen LM, Simon AE, Herrick KA (2016) Types of infant formulas consumed in the United States. Clin Pediatr (Phila) 55:278–285. https://doi.org/10.1177/0009922815591881
Vandenplas Y, De Greef E, Devreker T (2014) Treatment of cow’s milk protein allergy. Pediatr Gastroenterol Hepatol Nutr 17:1–5. https://doi.org/10.5223/pghn.2014.17.1.1
Patisaul HB, Jefferson W (2010) The pros and cons of phytoestrogens. Front Neuroendocrinol 31:400–419. https://doi.org/10.1016/j.yfrne.2010.03.003
Setchell KD, Zimmer-Nechemias L, Cai J, Heubi JE (1997) Exposure of infants to phyto-oestrogens from soy-based infant formula. Lancet 350:23–27. https://doi.org/10.1016/S0140-6736(96)09480-9
Biro FM, Greenspan LC, Galvez MP (2012) Puberty in girls of the 21st century. J Pediatr Adolesc Gynecol 25:289–294. https://doi.org/10.1016/j.jpag.2012.05.009
Carel JC, Lahlou N, Roger M, Chaussain JL (2004) Precocious puberty and statural growth. Hum Reprod Update 10:135–147. https://doi.org/10.1093/humupd/dmh012
Downing J, Bellis MA (2009) Early pubertal onset and its relationship with sexual risk taking, substance use and anti-social behaviour: a preliminary cross-sectional study. BMC Public Health 9:446. https://doi.org/10.1186/1471-2458-9-446
Prentice P, Viner R (2013) Pubertal timing and adult obesity and cardiometabolic risk in women and men: a systematic review and meta-analysis. Int J Obes (Lond) 37:1036–1043. https://doi.org/10.1038/ijo.2012.177
Collaborative Group on Hormonal Factors in Breast Cancer (2012) Menarche, menopause, and breast cancer risk: individual participant meta-analysis, including 118 964 women with breast cancer from 117 epidemiological studies. Lancet Oncol 13:1141–1151. https://doi.org/10.1016/S1470-2045(12)70425-4
Strom BL, Schinnar R, Ziegler EE et al (2001) Exposure to soy-based formula in infancy and endocrinological and reproductive outcomes in young adulthood. JAMA 286:807–814
Cao Y, Calafat AM, Doerge DR et al (2009) Isoflavones in urine, saliva and blood of infants: data from a pilot study on the estrogenic activity of soy formula. J Expo Sci Environ Epidemiol 19:223–234. https://doi.org/10.1038/jes.2008.44
Segovia-Siapco G, Pribis P, Messina M, Oda K, Sabaté J (2014) Is soy intake related to age at onset of menarche? A cross-sectional study among adolescents with a wide range of soy food consumption. Nutr J 13:54. https://doi.org/10.1186/1475-2891-13-54
Cheng G, Remer T, Prinz-Langenohl R, Blaszkewicz M, Degen GH, Buyken AE (2010) Relation of isoflavones and fiber intake in childhood to the timing of puberty. Am J Clin Nutr 92:556–564. https://doi.org/10.3945/ajcn.2010.29394
Giampietro PG, Bruno G, Furcolo G et al (2004) Soy protein formulas in children: no hormonal effects in long-term feeding. J Pediatr Endocrinol Metab 17:191–196
Andres A, Moore MB, Linam LE, Casey PH, Cleves MA, Badger TM (2015) Compared with feeding infants breast milk or cow-milk formula, soy formula feeding does not affect subsequent reproductive organ size at 5 years of age. J Nutr 145:871–875. https://doi.org/10.3945/jn.114.206201
Freni-Titulaer LW, Cordero JF, Haddock L, Lebrón G, Martínez R, Mills JL (1986) Premature thelarche in Puerto Rico. A search for environmental factors. Am J Dis Child 140:1263–1267
Zung A, Glaser T, Kerem Z, Zadik Z (2008) Breast development in the first 2 years of life: an association with soy-based infant formulas. J Pediatr Gastroenterol Nutr 46:191–195. https://doi.org/10.1097/MPG.0b013e318159e6ae
Kim J, Kim S, Huh K, Kim Y, Joung H, Park M (2011) High serum isoflavone concentrations are associated with the risk of precocious puberty in Korean girls. Clin Endocrinol (Oxf) 75:831–835. https://doi.org/10.1111/j.1365-2265.2011.04127.x
Adgent MA, Daniels JL, Rogan WJ et al (2012) Early-life soy exposure and age at menarche. Paediatr Perinat Epidemiol 26:163–175. https://doi.org/10.1111/j.1365-3016.2011.01244.x
Katz Y, Rajuan N, Goldberg MR et al (2010) Early exposure to cow’s milk protein is protective against IgE-mediated cow’s milk protein allergy. J Allergy Clin Immunol 126:77–82. https://doi.org/10.1016/j.jaci.2010.04.020
Kuczmarski RJ, Ogden CL, Grummer-Strawn LM et al (2000) CDC growth charts: United States. Adv Data 314:1–27
Marshall WA, Tanner JM (1969) Variations in pattern of pubertal changes in girls. Arch Dis Child 44:291–303
Marshall WA, Tanner JM (1970) Variations in the pattern of pubertal changes in boys. Arch Dis Child 45:13–23
Tzameret [computer program] (2010) Version 2. Jerusalem: Israeli Ministry of Health
National Agricultural Library, United States Department of Agriculture United States: Food and Nutrition Information Center. DRI tables and application reports; Available at: http://www.nal.usda.gov/sites/default/files/fnic_uploads//recommended_intakes_individuals.pdf. Accessed 22 Nov 2017
Biro FM, Galvez MP, Greenspan LC et al (2010) Pubertal assessment method and baseline characteristics in a mixed longitudinal study of girls. Pediatrics 126:e583–e590. https://doi.org/10.1542/peds.2009-3079
Garibaldi L, Chemaitilly W (2015) Disorders of pubertal development. In: Kliegman RM, Stanton BF,, Schor NF, Behrman RE, eds. Nelson textbook of pediatrics St. Geme JW, 20th edn. Elsevier, Philadelphia, pp 2656–2662
Wohlfahrt-Veje C, Mouritsen A, Hagen CP et al (2016) Pubertal onset in boys and girls is influenced by pubertal timing of both parents. J Clin Endocrinol Metab 101:2667–2674. https://doi.org/10.1210/jc.2016-1073
Sloboda DM, Hart R, Doherty DA, Pennell CE, Hickey M (2007) Age at menarche: influences of prenatal and postnatal growth. J Clin Endocrinol Metab 92:46–50. https://doi.org/10.1210/jc.2006-1378
Kaplowitz PB (2008) Link between body fat and the timing of puberty. Pediatrics 121:S208–S217. https://doi.org/10.1542/peds.2007-1813F
Kale A, Deardorff J, Lahiff M et al (2015) Breastfeeding versus formula-feeding and girls’ pubertal development. Matern Child Health J 19:519–27. https://doi.org/10.1007/s10995-014-1533-9 .
Villamor E, Jansen EC (2016) Nutritional determinants of the timing of puberty. Annu Rev Public Health 37:33–46. https://doi.org/10.1146/annurev-publhealth-031914-122606
Bacil EDA, Mazzardo O, Rech CR, Legnani RF, dos de Campos SW (2015) Physical activity and biological maturation: a systematic review. Revista Paulista de Pediatria 33:114–121. https://doi.org/10.1016/j.rpped.2014.11.003
Baranowski T (2013) 24-h recall and diet record methods. In: Willett W (ed) Nutritional epidemiology, 3rd edn. Oxford University Press, New York, pp 49–69
Ministry of Health. Mabat Youth- First Israeli National Health and Nutrition Survey. Available at: https://www.health.gov.il/PublicationsFiles/Mabat_2003-2004-b.pdf. Accessed 22 Nov 2017
Vandenplas Y, Castrellon PG, Rivas R et al (2014) Safety of soya-based infant formulas in children. Br J Nutr 111:1340–1360. https://doi.org/10.1017/S0007114513003942
Acknowledgements
The authors would like to thank Dr. Aliza Stark for her help in manuscript editing and Dr. Tomer Ziv for the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no reported conflicts of interest for any of the authors.
Source of funding
Michael R. Goldberg is supported by a Kamea grant from the Ministry of Health, Israel. No honorarium, grant, or other form of payment was given to produce the manuscript.
Research registration
Website: https://clinicaltrials.gov/ ID Number: NCT02908971.
Rights and permissions
About this article
Cite this article
Sinai, T., Ben-Avraham, S., Guelmann-Mizrahi, I. et al. Consumption of soy-based infant formula is not associated with early onset of puberty. Eur J Nutr 58, 681–687 (2019). https://doi.org/10.1007/s00394-018-1668-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-018-1668-3