Abstract
Background
Therapeutic variability not explained by patient clinical characteristics is a potential source of avoidable morbidity and mortality. We aimed to explore regional variability in the management and mortality of patients with non-ST-segment elevation acute coronary syndromes (NSTE-ACS).
Methods and results
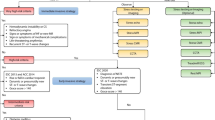
11,931 NSTE-ACS hospital survivors enrolled in two prospective registries: EPICOR [5625 patients, 555 hospitals, 20 countries in Europe (E) and Latin America (LA), September 2010–March 2011] and EPICOR Asia (6306 patients, 218 hospitals, 8 countries, June 2011–May 2012) were compared among eight pre-defined regions: Northern E (NE), Southern E (SE), Eastern E (EE); Latin America (LA); China (CN), India (IN), South-East Asia (SA), and South Korea, Hong Kong and Singapore (KS). Patient characteristics differed between regions: mean age (lowest 59 years, IN; highest 65.9 years, SE), diabetes (21.4% NE; 35.5% IN) and smoking (32% NE; 62% IN). Variations in dual antiplatelet therapy at discharge (lowest 83.1%, IN; highest 97.5%, SA), coronary angiography (53.9% SA; 90.6% KS), percutaneous coronary intervention (35.8% SA; 78.6% KS) and coronary artery bypass graft (0.7% KS; 5.7% NE) were observed. Unadjusted 2-year mortality ranged between 3.8% in KS and 11.7% in SE. Two-year, risk-adjusted mortality rates ranged between 5.1% (95% confidence interval 2.9–7.3%) in KS to 10.5% (8.3–12.7%) in LA.
Conclusion
Wide regional variations in patient features, hospital care, coronary revascularization and post-discharge mortality are present among patients hospitalized for NSTE-ACS. Focused regional interventions to improve the quality of care for NSTE-ACS patients are still needed.



Similar content being viewed by others
References
Peterson ED, Roe MT, Mulgund J, DeLong ER, Lytle BL et al (2006) Association between hospital process performance and outcomes among patients with acute coronary syndromes. JAMA 295(16):1912–1920
Bebb O, Hall M, Fox KAA, Dondo TB, Timmis A et al (2017) Performance of hospitals according to the ESC ACCA quality indicators and 30-day mortality for acute myocardial infarction: national cohort study using the United Kingdom Myocardial Ischaemia National Audit Project (MINAP) register. Eur Heart J 38(13):974–982
Schiele F, Gale CP, Simon T, Fox KAA, Bueno H, et al. (2017) Assessment of quality indicators for acute myocardial infarction in the FAST-MI (French Registry of Acute ST-Elevation or Non-ST-Elevation Myocardial Infarction) registries. Circ Cardiovasc Qual Outcomes 10(6):pii: e003336
Bueno H, Sinnaeve P, Annemans L, Danchin N, Licour M et al (2016) Opportunities for improvement in anti-thrombotic therapy and other strategies for the management of acute coronary syndromes: Insights from EPICOR, an international study of current practice patterns. Eur Heart J Acute Cardiovasc Care 5(1):3–12
Hall M, Dondo TB, Yan AT, Goodman SG, Bueno H et al (2016) Association of clinical factors and therapeutic strategies with improvements in survival following non-ST-elevation myocardial infarction, 2003–2013. JAMA 316(10):1073–1082
Bueno H, Pocock S, Medina J, Annemans L, Danchin N et al. (2017) Heterogeneity in medically managed patients with non-ST-segment elevation acute coronary syndromes. Rev Esp Cardiol. pii:S1885-585:30454–30456
Puymirat E, Battler A, Birkhead J, Bueno H, Clemmensen P et al (2013) Euro Heart Survey 2009 Snapshot: regional variations in presentation and management of patients with AMI in 47 countries. Eur Heart J Acute Cardiovasc Care 2(4):359–370
Mandelzweig L, Battler A, Boyko V, Bueno H, Danchin N et al (2006) The second Euro Heart Survey on acute coronary syndromes: characteristics, treatment, and outcome of patients with ACS in Europe and the Mediterranean Basin in 2004. Eur Heart J 27(19):2285–2293
Budaj A, Brieger D, Steg PG, Goodman SG, Dabbous OH et al (2003) Global patterns of use of antithrombotic and antiplatelet therapies in patients with acute coronary syndromes: Insights from the Global Registry of Acute Coronary Events (GRACE). Am Heart J 146(6):999–1006
Fox KA, Goodman SG, Klein W, Brieger D, Steg PG et al (2002) Management of acute coronary syndromes. Variations in practice and outcome; findings from the Global Registry of Acute Coronary Events (GRACE). Eur Heart J 23(15):1177–1189
Fox KA, Goodman S, Bigonzi F, Le Louer V, Cohen M (2000) Inter-regional differences and outcome in unstable angina; analysis of the international ESSENCE trial. Efficacy and safety of subcutaneous enoxaparin in non-Q-wave coronary events. Eur Heart J 21(17):1433–1439
Boersma E, Pieper KS, Steyerberg EW, Wilcox RG, Chang WC et al (2000) Predictors of outcome in patients with acute coronary syndromes without persistent ST-segment elevation. Results from an international trial of 9461 patients. PURSUIT Investigators Circulation 101(22):2557–2567
Bueno H, Danchin N, Tafalla M, Bernaud C, Annemans L et al (2013) EPICOR (long-tErm follow-up of antithrombotic management Patterns In acute CORonary syndrome patients) study: Rationale, design, and baseline characteristics. Am Heart J 165(1):8–14
Huo Y, Lee SW, Sawhney JP, Kim HS, Krittayaphong R et al (2015) Rationale, design, and baseline characteristics of the EPICOR Asia Study (Long-tErm follow-uP of antithrombotic management patterns In Acute CORonary Syndrome patients in Asia). Clin Cardiol 38(9):511–519
Rossello X, Huo Y, Pocock S, Van de Werf F, Chin CT et al (2017) Global geographical variations in ST-segment elevation myocardial infarction management and post-discharge mortality. Int J Cardiol 245:27–34
Pocock SJ, Huo Y, Van de Werf F, Newsome S, Chin CT et al. (2017) Predicting two-year mortality from discharge after acute coronary syndrome: an internationally-based risk score. Eur Heart J Acute Cardiovasc Care 2048872617719638 (epub ahead of print)
Von Hippel PT (2009) How to impute interactions, squares, and other transformed variables. Sociol Methodol 39:265–291
O’Connor GT, Quinton HB, Traven ND, Ramunno LD, Dodds TA et al (1999) Geographic variation in the treatment of acute myocardial infarction: the Cooperative Cardiovascular Project. JAMA 281(7):627–633
Feldman L, Steg PG, Amsallem M, Puymirat E, Sorbets E et al (2017) Editor’s choice-medically managed patients with non-ST-elevation acute myocardial infarction have heterogeneous outcomes, based on performance of angiography and extent of coronary artery disease. Eur Heart J Acute Cardiovasc Care 6(3):262–271
Schiele F, Gale CP, Bonnefoy E, Capuano F, Claeys MJ et al (2017) Quality indicators for acute myocardial infarction: a position paper of the Acute Cardiovascular Care Association. Eur Heart J Acute Cardiovasc Care 6(1):34–59
Chan MY, Du X, Eccleston D, Ma C, Mohanan PP et al (2016) Acute coronary syndrome in the Asia-Pacific region. Int J Cardiol 202:861–869
Huo Y, Thompson P, Buddhari W, Ge J, Harding S et al (2015) Challenges and solutions in medically managed ACS in the Asia-Pacific region: expert recommendations from the Asia-Pacific ACS Medical Management Working Group. Int J Cardiol 183:63–75
Acknowledgements
Editorial support was provided by Carl V Felton PhD of Prime (Knutsford, Cheshire, UK), supported by AstraZeneca. Ultimate responsibility for opinions, conclusions, and data interpretation lies with the author. X.R. has received support from the SEC-CNIC CARDIOJOVEN fellowship program.
Funding
EPICOR and EPICOR Asia are funded by AstraZeneca. Being a non-interventional study, no drugs were supplied or funded.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
H.B. has received consulting fees from Abbott, AstraZeneca, Bayer, BMS, Novartis and Pfizer; speaking fees from AstraZeneca, Bayer, BMS-Pfizer, Ferrer, Novartis, Servier and MEDSCAPE-the heart.org; and fees for research activities from AstraZeneca, BMS, Janssen, Novartis; S.P. has received research funding from AstraZeneca. F.v.d.W. has received consulting fees and research grants from Boehringer Ingelheim and Merck, and consulting fees from Roche, Sanofi-Aventis, AstraZeneca, and The Medicines Company. C.T.C. has received research support from Eli Lilly, honoraria from Medtronic, and has been a consultant or advisory board member for AstraZeneca. N.D. has received consulting or speaking fees from AstraZeneca, BMS, Boehringer-Ingelheim, GSK, MSD-Schering Plough, Novartis, Pierre Fabre, Pfizer, Roche, Sanofi-Aventis, Servier, Takeda, and The Medicines Company. J.M. and A.V. are employees of AstraZeneca. X.R., S.W-L.L. and Y.H. have nothing to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bueno, H., Rossello, X., Pocock, S. et al. Regional variations in hospital management and post-discharge mortality in patients with non-ST-segment elevation acute coronary syndrome. Clin Res Cardiol 107, 836–844 (2018). https://doi.org/10.1007/s00392-018-1254-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-018-1254-y