Abstract
Purpose
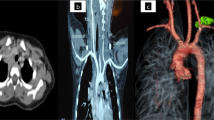
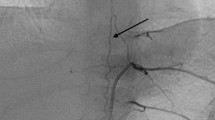
Cervicothoracic and apical thoracic neuroblastoma pose unique surgical challenges. We report our experience with the trapdoor anterior thoracotomy (TAT) approach to overcome these difficulties.
Methods
Retrospective review of our centre’s neuroblastoma database was conducted. Patients who underwent TAT at our centre were included, their demographic data and clinical reports were analyzed.
Results
A total of 21 patients underwent TAT for neuroblastoma, mean age at surgery of 3.5 (0.3–7.9) years, male to female ratio was 11:10. Fifteen patients had cervicothoracic tumors while 6 had apical thoracic tumors. All except 2 were primary tumors. They were stage M (n = 12), MS (n = 1), and L2 (n = 8). At pre-operative assessment, 19 patients had image-defined risk factor (IDRF), including dual compartmental involvement (n = 15), trachea/bronchus compression (n = 4), encasement of carotid (n = 5), subclavian (n = 11), and vertebral arteries (n = 6). Four underwent upfront surgery while 17 received pre-operative chemotherapy of 2–8 (mean 3.9) cycles. All patients accomplished gross total resection. None had MYCN amplification. The postoperative complications included Horner’s syndrome (n = 21), Klumpke’s palsy (n = 1), winged scapula (n = 1), phrenic nerve palsy (n = 1), and bronchomalacia (n = 2).
Conclusion
Gross total resection of cervicothoracic and apical thoracic neuroblastoma can be accomplished by TAT with minimal morbidity.




Similar content being viewed by others
Data availability
No data is available. Data are included in the main text.
References
Parikh D, Short M, Eshmawy M et al (2012) Surgical outcome analysis of paediatric thoracic and cervical neuroblastoma. Eur J Cardio Thorac Surg 41:630–634
Haddad M, Triglia JM, Helardot P et al (2003) Localized cervical neuroblastoma: prevention of surgical complications. Int J Pediatr Otorhinolaryngol 67:1361–1367
Brisse HJ, Blanc T, Schlelermacher G et al (2017) Radiogenomics of neuroblastomas: relationships between imaging phenotypes, tumor genomic profile and survival. PLoS ONE 12:e0185190
von Allmen D, Davidoff AM, London WB et al (2017) Impact of extent of resection on local control and survival in patients from the COG A3973 study with high-risk neuroblastoma. J Clin Oncol 35:208–216
Pranikoff T, Hirschi RB, Schnaufer L (1995) Approach to cervicothoracic neuroblastomas via a trap-door incision. J Pediatr Surg 30:546–548
Sauvat F, Brisse H, Magdeleinat P (2006) The transmanubrial approach: a new operative approach to cervicothoracic neuroblastoma in children. Surgery 139:109–114
De Corti F, Avanzini S, Cecchetto G et al (2012) The surgical approach for cervicothoracic masses in children. J Pediatr Surg 47:1662–1668
McMahon SV, Menon S, McDowell DT et al (2013) The use of the trapdoor incision for access to thoracic inlet pathology in children. J Pediatr Surg 49:1147–1151
Christison-Lagay ER, Darcy DG, Stanelle EJ et al (2014) "Trap-door" and "clamshell" surgical approaches for the management of pediatric tumors of the cervicothoracic junction and mediastinum. J Pediatr Surg 49:172–177
Monclair T, Brodeur GM, Ambros PF et al (2009) INRG Task Force: the International Neuroblastoma Risk Group (INRG) staging system: an INRG Task Force report. J Clin Oncol 27:298–303
Dartevelle PG, Chapelier AR, Macchiarini P, Lenot B, Cerrina J, Ladurie FL, Parquin FJ, Lafont D (1993) Anterior transcervical-thoracic approach for radical resection of lung tumors invading the thoracic inlet. J Thorac Cardiovasc Surg 105:1025–1034
Masaoka A, Ito Y, Yasumitsu T (1979) Anterior approach for tumor of the superior sulcus. J Thorac Cardiovasc Surg 78:413–415
Kiely EM (1994) The surgical challenge of neuroblastoma. J Pediatr Surg 29:128–133
Newman EA, Nuchtern JG (2016) Recent biologic and genetic advances in neuroblastoma: Implications for diagnostic, risk stratification, and treatment strategies. Semin Pediatr Surg 25:257–264
Grunenwald D, Spaggiari L (1997) Transmanubrial osteomuscular sparing approach for apical chest tumors. Ann Thorac Surg 63:563–566
Funding
No funding is received for this study.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data collection and analysis were performed by Chan Hon Chui. The first draft of the manuscript was written by Chan Hon Chui and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any conflict of interest.
Ethical approval
Our local audit committee has approved this retrospective study that involved secondary use of data, from a database, which is provided without any identifier.
Informed consent
Consent is not required as information is anonymized and the submission does not include images that may identify the person.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chui, C.H., Thirugnanam, A. Trapdoor anterior thoracotomy for cervicothoracic and apical thoracic neuroblastoma in children. Pediatr Surg Int 36, 891–895 (2020). https://doi.org/10.1007/s00383-020-04692-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-020-04692-2