Abstract
Background
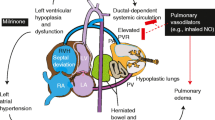
Congenital diaphragmatic hernia (CDH) is associated with lung hypoplasia, cardiac dysfunction and pulmonary hypertension. Inhaled nitric oxide (iNO) and milrinone are commonly used pulmonary vasodilators in CDH. We studied the hemodynamic effects of iNO and milrinone in infants with CDH.
Methods
A retrospective chart review was performed of all CDH infants admitted to two regional perinatal centers and infants classified into three groups: No-iNO group; iNO-responders and iNO-nonresponders. Oxygenation and hemodynamic effects of iNO and milrinone were assessed by blood gases and echocardiography.
Results
Fifty-four percent (39/72) of infants with CDH received iNO and 31% of these infants (12/39) had complete oxygenation response to iNO. Oxygenation response to iNO was not associated with a decrease in right ventricular pressures (RVP) or ECMO use. Four infants (33%) in the iNO-responder group and eight infants (30%) in the iNO-nonresponder group received milrinone. Milrinone lowered RVP and improved ejection fraction (EF). Response to iNO was associated with improved oxygenation to milrinone and increased survival following ECMO (67 vs. 20% among nonresponders).
Conclusions
Response to inhaled nitric oxide in combination with milrinone may be associated with improved oxygenation and better survival after ECMO in infants with CDH.



Similar content being viewed by others
References
Barrington KJ, Finer N, Pennaforte T, Altit G (2017) Nitric oxide for respiratory failure in infants born at or near term. Cochrane Database Syst Rev 1:CD000399. https://doi.org/10.1002/14651858.CD000399.pub3
The Neonatal Inhaled Nitric Oxide Study Group (NINOS) (1997) Inhaled nitric oxide and hypoxic respiratory failure in infants with congenital diaphragmatic hernia. Pediatrics 99(6):838–845
Snoek KG, Capolupo I, van Rosmalen J, Hout Lde J, Vijfhuize S, Greenough A, Wijnen RM, Tibboel D, Reiss IK, Consortium CE (2016) Conventional mechanical ventilation versus high-frequency oscillatory ventilation for congenital diaphragmatic hernia: a randomized clinical trial (the VICI-trial). Ann Surg 263(5):867–874. https://doi.org/10.1097/SLA.0000000000001533
Kumar VH, Swartz DD, Rashid N, Lakshminrusimha S, Ma C, Ryan RM, Morin FC 3rd (2010) Prostacyclin and milrinone by aerosolization improve pulmonary hemodynamics in newborn lambs with experimental pulmonary hypertension. J Appl Physiol 109(3):677–684. https://doi.org/10.1152/japplphysiol.01082.2009
Lakshminrusimha S, Porta NF, Farrow KN, Chen B, Gugino SF, Kumar VH, Russell JA, Steinhorn RH (2009) Milrinone enhances relaxation to prostacyclin and iloprost in pulmonary arteries isolated from lambs with persistent pulmonary hypertension of the newborn. Pediatr Crit Care Med 10(1):106–112. https://doi.org/10.1097/PCC.0b013e3181936aee
Rashid N, Morin FC 3rd, Swartz DD, Ryan RM, Wynn KA, Wang H, Lakshminrusimha S, Kumar VH (2006) Effects of prostacyclin and milrinone on pulmonary hemodynamics in newborn lambs with persistent pulmonary hypertension induced by ductal ligation. Pediatr Res 60(5):624–629. https://doi.org/10.1203/01.pdr.0000242343.84510.81
McNamara PJ, Laique F, Muang-In S, Whyte HE (2006) Milrinone improves oxygenation in neonates with severe persistent pulmonary hypertension of the newborn. J Crit Care 21(2):217–222. https://doi.org/10.1016/j.jcrc.2006.01.001
Patel N (2012) Use of milrinone to treat cardiac dysfunction in infants with pulmonary hypertension secondary to congenital diaphragmatic hernia: a review of six patients. Neonatology 102(2):130–136. https://doi.org/10.1159/000339108
Lakshminrusimha S, Keszler M, Kirpalani H, Van Meurs K, Chess P, Ambalavanan N, Yoder B, Fraga MV, Hedrick H, Lally KP, Nelin L, Cotten M, Klein J, Guilford S, Williams A, Chaudhary A, Gantz M, Gabrio J, Chowdhury D, Zaterka-Baxter K, Das A, Higgins RD (2017) Milrinone in congenital diaphragmatic hernia—a randomized pilot trial: study protocol, review of literature and survey of current practices. Matern Health Neonatol Perinatol 3:27. https://doi.org/10.1186/s40748-017-0066-9
Neonatal Inhaled Nitric Oxide Study G (1997) Inhaled nitric oxide in full-term and nearly full-term infants with hypoxic respiratory failure. N Engl J Med 336 (9):597–604. https://doi.org/10.1056/NEJM199702273360901
Aly H, Bianco-Batlles D, Mohamed MA, Hammad TA (2010) Mortality in infants with congenital diaphragmatic hernia: a study of the United States National Database. J Perinatol 30(8):553–557. https://doi.org/10.1038/jp.2009.194
Kumar VH (2015) Current concepts in the management of congenital diaphragmatic hernia in infants. Indian J Surg 77(4):313–321. https://doi.org/10.1007/s12262-015-1286-8
Reiss I, Schaible T, van den Hout L, Capolupo I, Allegaert K, van Heijst A, Gorett Silva M, Greenough A, Tibboel D, Consortium CE (2010) Standardized postnatal management of infants with congenital diaphragmatic hernia in Europe: the CDH EURO consortium consensus. Neonatology 98(4):354–364. https://doi.org/10.1159/000320622
Patel N, Kipfmueller F (2017) Cardiac dysfunction in congenital diaphragmatic hernia: Pathophysiology, clinical assessment, and management. Semin Pediatr Surg 26(3):154–158. https://doi.org/10.1053/j.sempedsurg.2017.04.001
Konduri GG, Sokol GM, Van Meurs KP, Singer J, Ambalavanan N, Lee T, Solimano A (2013) Impact of early surfactant and inhaled nitric oxide therapies on outcomes in term/late preterm neonates with moderate hypoxic respiratory failure. J Perinatol 33(12):944–949. https://doi.org/10.1038/jp.2013.83
Lakshminrusimha S (2012) The pulmonary circulation in neonatal respiratory failure. Clin Perinatol 39(3):655–683. https://doi.org/10.1016/j.clp.2012.06.006
Bassler D, Kreutzer K, McNamara P, Kirpalani H (2010) Milrinone for persistent pulmonary hypertension of the newborn. Cochrane Database Syst Rev (11):CD007802. https://doi.org/10.1002/14651858.CD007802.pub2
James AT, Bee C, Corcoran JD, McNamara PJ, Franklin O, El-Khuffash AF (2015) Treatment of premature infants with pulmonary hypertension and right ventricular dysfunction with milrinone: a case series. J Perinatol 35(4):268–273. https://doi.org/10.1038/jp.2014.208
James AT, Corcoran JD, McNamara PJ, Franklin O, El-Khuffash AF (2016) The effect of milrinone on right and left ventricular function when used as a rescue therapy for term infants with pulmonary hypertension. Cardiol Young 26(1):90–99. https://doi.org/10.1017/S1047951114002698
Putnam LR, Harting MT, Tsao K, Morini F, Yoder BA, Luco M, Lally PA, Lally KP, Congenital Diaphragmatic Hernia Study G (2016) Congenital diaphragmatic hernia defect size and infant morbidity at discharge. Pediatrics. https://doi.org/10.1542/peds.2016-2043
Paden ML, Conrad SA, Rycus PT, Thiagarajan RR, Registry E (2013) Extracorporeal life support organization registry report 2012. ASAIO J 59(3):202–210. https://doi.org/10.1097/MAT.0b013e3182904a52
Acknowledgements
This research work was performed without any support from external funding or grants. No funds were received for covering the costs to publish in open access.
Author information
Authors and Affiliations
Contributions
HSVK and SL conceived and designed the project; RD and SG provided help with IRB approval; RD, JK and SG substantially contributed to acquisition, analysis and interpretation of data; all the authors (VK, RD, JK, SG and SL) played a critical role in drafting and revising the manuscript for intellectual content.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interests to declare.
Ethical approval
This article does not contain any studies with animals performed by any of the authors.
Research involving human participants
This is a retrospective case–control study. The University at Buffalo Institutional Review Board of the State University of New York, Buffalo (MODCR00001406), and the Research Subjects Review Board at the University of Rochester, Rochester (RSRB0006718), approved the study protocol for data collection in study patients.
Rights and permissions
About this article
Cite this article
Kumar, V.H.S., Dadiz, R., Koumoundouros, J. et al. Response to pulmonary vasodilators in infants with congenital diaphragmatic hernia. Pediatr Surg Int 34, 735–742 (2018). https://doi.org/10.1007/s00383-018-4286-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-018-4286-5