Abstract
Purpose
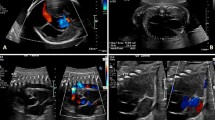
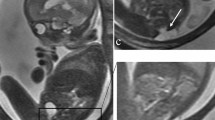
Antenatally diagnosed ventriculomegaly (VM) requires the balance of risks of neurological injury with premature delivery. The purpose of this study was to evaluate outcomes related to early elective delivery due to fetal VM at our institution.
Methods
We retrospectively assessed 120 babies (2008–2012) with antenatally diagnosed fetal VM. Inclusion criteria for (“early”) cohort were (1) elective delivery occurred for expedited neurosurgical intervention between 32 and 36 weeks EGA and (2) fetal VM noted on official antenatal ultrasound. The comparative “near term” cohort differed only in that delivery occurred at 37+ weeks EGA. Statistical significance for comparative analyses set a priori at p < 0.05.
Results
Babies electively delivered early had a lower birthweight (p < 0.0001), greater ventricle width (p < 0.0001), and underwent initial CSF diversion sooner (p = 0.014). The early cohort (n = 22), compared to near term (n = 50), had a lower birthweight (p < 0.0001), greater ventricle width (p < 0.0001), and underwent initial CSF diversion sooner (p = 0.014). The early cohort required more repeat procedures: (45 vs. 22% p = 0.021), and VPS removals after VPS infections (41 vs. 12%, p = 0.010). Additionally, newborn respiratory failure (32 vs. 6%, p = 0.037) was more common. Finally, of four babies who died in the early cohort, 2/4 died for prematurity-associated pulmonary hypoplasia.
Conclusions
While early elective delivery for fetal VM expedites intervention for rapidly expanding ventricles, few benefits were identified. Our study concluded those infants that were delivered earlier had increased VPS infections, repeat neurosurgical procedures, and medical co-morbidities. A multi-institutional prospective observational study would be needed in order to confirm the clinical implications of such practice.


Similar content being viewed by others
References
Ashton DM (2010) Elective delivery at less than 39 weeks. Curr Opin Obstet Gynecol 22(6):506–510. https://doi.org/10.1097/GCO.0b013e3283404eb4
Bruinsma N, Stobberingh EE, Herpers MJ, Vles JS, Weber BJ, Gavilanes DA (2000) Subcutaneous ventricular catheter reservoir and ventriculoperitoneal drain-related infections in preterm infants and young children. Clin Microbiol Infect 6(4):202–206. https://doi.org/10.1046/j.1469-0691.2000.00052.x
Cardoza JD, Goldstein RB, Filly RA (1988) Exclusion of fetal ventriculomegaly with a single measurement: the width of the lateral ventricular atrium. Radiology 169(3):711–714. https://doi.org/10.1148/radiology.169.3.3055034
Carnaghan H, Pereira S, James CP, Charlesworth PB, Ghionzoli M, Mohamed E et al (2014) Is early delivery beneficial in gastroschisis? J Pediatr Surg 49:928–933; discussion 933
Engle WA (2008) Surfactant-replacement therapy for respiratory distress in the preterm and term neonate. Pediatrics 121(2):419–432. https://doi.org/10.1542/peds.2007-3283
Engle WA, Kominiarek MA (2008) Late preterm infants, early term infants, and timing of elective deliveries. Clin Perinatol 35:325–341, vi
Engle WA, Tomashek KM (2007) Wallman C: {“late-preterm”} infants: a population at risk. Pediatrics 120(6):1390–1401. https://doi.org/10.1542/peds.2007-2952
Goynumer G, Yayla M, Arisoy R, Turkmen O (2014) The criterion value of fetal cerebral lateral ventricular atrium width for diagnosis of ventriculomegaly. Clin Exp Obstet Gynecol 41:67–71
Hadidi A, Subotic U, Goeppl M, Waag K-LL (2008) Early elective cesarean delivery before 36 weeks vs late spontaneous delivery in infants with gastroschisis. J Pediatr Surg 43(7):1342–1346. https://doi.org/10.1016/j.jpedsurg.2007.12.050
Hidaka N, Ishii K, Kanazawa R, Miyagi A, Irie A, Hayashi S, Mitsuda N (2014) Perinatal characteristics of fetuses with borderline ventriculomegaly detected by routine ultrasonographic screening of low-risk populations. J Obstet Gynaecol Res 40(4):1030–1036. https://doi.org/10.1111/jog.12298
Jensen JR, White WM, Coddington CC (2013) Maternal and neonatal complications of elective early-term deliveries. Mayo Clin Proc 88(11):1312–1317. https://doi.org/10.1016/j.mayocp.2013.07.009
Logghe HL, Mason GC, Thornton JG, Stringer MD (2005) A randomized controlled trial of elective preterm delivery of fetuses with gastroschisis. J Pediatr Surg 40(11):1726–1731. https://doi.org/10.1016/j.jpedsurg.2005.07.047
Madar J, Richmond S, Hey E (1999) Surfactant-deficient respiratory distress after elective delivery at “term”. Acta Paediatr 88(11):1244–1248. https://doi.org/10.1080/080352599750030365
Pople IK, Bayston R, Hayward RD (1992) Infection of cerebrospinal fluid shunts in infants: a study of etiological factors. J Neurosurg 77(1):29–36. https://doi.org/10.3171/jns.1992.77.1.0029
Spader HS, Hertzler DA, Kestle JR, Jay R-C (2015) Risk factors for infection and the effect of an institutional shunt protocol on the incidence of ventricular access device infections in preterm infants. J Neurosurg Pediatr 15(2):156–160. https://doi.org/10.3171/2014.9.PEDS14215
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Additional information
Portions of this work were presented as a poster at the AANS/CNS Section on Pediatric Neurological Surgery in Seattle, WA on Dec. 8–11, 2015.
Rights and permissions
About this article
Cite this article
Morgan, C.D., Ladner, T.R., Yang, G.L. et al. Early elective delivery for fetal ventriculomegaly: are neurosurgical and medical complications mitigated by this practice?. Childs Nerv Syst 34, 829–835 (2018). https://doi.org/10.1007/s00381-017-3662-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-017-3662-0