Abstract
Objective
To investigate 90-day mortality rate of RC for bladder cancer in a nationwide population-based study.
Design, setting, and participants
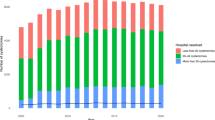
We used mandatory hospital discharge forms of all patients submitted to RC due to bladder cancer in Spain during 2011–2015 (n = 12,154 in 196 hospitals). At present, a centralization policy for RC has not been issued by the health authorities.
Outcome measurements and statistical analysis
We calculated in-hospital, 30-, 60- and 90-day mortality. Average annual RC volume was used as a continuous variable (log-transformed) and also grouped into deciles to identify any potential non-linear relationships. Logistic regression model with mixed effect was performed adjusting for year of surgery, comorbidity, surgical approach, type of admission, age, sex, and hospital size.
Results and limitation
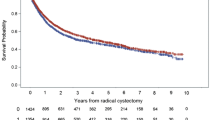
Overall 90-day mortality rate was 6.5%. Lowest mortality rates (3.3% at 90 days) are achieved in hospitals doing more than 38 cases per year. The 90-day adjusted mortality rate is associated with annual average RC volume with a 20.6% decrease per 10 extra RCs/year (95% CI 12.3–28.1% p < 0.001). High Charlson comorbidity index, advanced age, and open surgical approach were the clinical variables associated with higher mortality.
Conclusions
Our study identifies an inverse association between 90-day mortality and hospital volume. High-volume hospitals achieve lower mortality rate within 90 days.


Similar content being viewed by others
Abbreviations
- RC:
-
Radical cystectomy
References
Gore JL, Wright JL, Daratha KB, Roberts KP, Lin DW, Wessells H, Porter M (2012) Hospital-level variation in the quality of urologic cancer surgery. Cancer 118:987–996
Gierth M, Zeman F, Denzinger S, Vetterlein MW, Fisch M, Bastian PJ, Syring I, Ellinger J, Muller SC, Herrmann E, Gilfrich C, May M, Pycha A, Wagenlehner FM, Vallo S, Bartsch G, Haferkamp A, Grimm MO, Roigas J, Protzel C, Hakenberg OW, Fritsche HM, Burger M, Aziz A, Mayr R (2018) Influence of body mass index on clinical outcome parameters, complication rate and survival after radical cystectomy: evidence from a prospective European multicentre study. Urol Int 101:16–24
Milenkovic U, Akand M, Moris L, Demaegd L, Muilwijk T, Bekhuis Y, Laenen A, Van Cleynenbreugel B, Everaerts W, Van Poppel H, Dumez H, Albersen M, Joniau S (2018) Impact of neoadjuvant chemotherapy on short-term complications and survival following radical cystectomy. World J Urol. https://doi.org/10.1007/s00345-018-2584-0
Ghodoussipour S, Ahmadi N, Hartman N, Cacciamani G, Miranda G, Cai J, Schuckman A, Djaladat H, Gill I, Daneshmand S, Desai M (2018) Factors influencing intraoperative conversion from planned orthotopic to non-orthotopic urinary diversion during radical cystectomy. World J Urol. https://doi.org/10.1007/s00345-018-2582-2
Hollenbeck BK, Daignault S, Dunn RL, Gilbert S, Weizer AZ, Miller DC (2007) Getting under the hood of the volume-outcome relationship for radical cystectomy. J Urol 177:2095–2099
Hautmann RE, de Petriconi RC, Volkmer BG (2010) Lessons learned from 1000 neobladders: the 90-day complication rate. J Urol 184:990–994
Aziz A, May M, Burger M, Palisaar RJ, Trinh QD, Fritsche HM, Rink M, Chun F, Martini T, Bolenz C, Mayr R, Pycha A, Nuhn P, Stief C, Novotny V, Wirth M, Seitz C, Noldus J, Gilfrich C, Shariat SF, Brookman-May S, Bastian PJ, Denzinger S, Gierth M, Roghmann F, PROMETRICS 2011 research group (2014) Prediction of 90-day mortality after radical cystectomy for bladder cancer in a prospective European multicenter cohort. Eur Urol 66:156–163
Hounsome LS, Verne J, McGrath JS, Gillatt DA (2015) Trends in operative caseload and mortality rates after radical cystectomy for bladder cancer in England for 1998–2010. Eur Urol 67:1056–1062
Birkmeyer JD, Siewers AE, Finlayson EV, Stukel TA, Lucas FL, Batista I, Welch HG, Wennberg DE (2002) Hospital volume and surgical mortality in the United States. N Engl J Med 346:1128–1137
Konety BR, Allareddy V, Modak S, Smith B (2006) Mortality after major surgery for urologic cancers in specialized urology hospitals: are they any better? J Clin Oncol 24:2006–2012
Finks JF, Osborne NH, Birkmeyer JD (2011) Trends in hospital volume and operative mortality for high-risk surgery. N Engl J Med 364:2128–2137
Rosario DJ (2015) Mortality following radical cystectomy: a good start, but how low can we go? Eur Urol 67:1063–1065
Deyo RA, Cherkin DC, Ciol MA (1992) Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 45:613–619
Burger M, Catto JW, Dalbagni G, Grossman HB, Herr H, Karakiewicz P, Kassouf W, Kiemeney LA, La Vecchia C, Shariat S, Lotan Y (2013) Epidemiology and risk factors of urothelial bladder cancer. Eur Urol 63:234–241
Isbarn H, Jeldres C, Zini L, Perrotte P, Baillargeon-Gagne S, Capitanio U, Shariat SF, Arjane P, Saad F, McCormack M, Valiquette L, Peloquin F, Duclos A, Montorsi F, Graefen M, Karakiewicz PI (2009) A population based assessment of perioperative mortality after cystectomy for bladder cancer. J Urol 182:70–77
Zakaria AS, Santos F, Dragomir A, Tanguay S, Kassouf W, Aprikian AG (2014) Postoperative mortality and complications after radical cystectomy for bladder cancer in Quebec: a population-based analysis during the years 2000–2009. Can Urol Assoc J 8:259–267
Author information
Authors and Affiliations
Contributions
CL: project development, manuscript writing, data collection; AG: data collection, manuscript editing; VH: manuscript editing; GF: manuscript editing; EP: data analysis; SP: data analysis, manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Llorente, C., Guijarro, A., Hernandez, V. et al. Effect of hospital volume on 90-day mortality after radical cystectomy for bladder cancer in Spain. World J Urol 38, 1221–1228 (2020). https://doi.org/10.1007/s00345-019-02874-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-019-02874-9