Abstract
Introduction
Muscle-invasive bladder cancer (MIBC) is an aggressive disease for which treatment strategies are continuously evolving. We characterized trends in treatment modalities for MIBC from 2004 to 2013 (the “pre-immunotherapy era”) and identified predictors of receiving the current standard of care treatment: neoadjuvant chemotherapy (NAC) followed by radical cystectomy (RC).
Methods
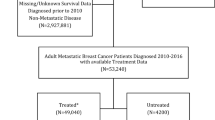
We used the National Cancer Database to identify individuals diagnosed with clinically localized MIBC from 2004 to 2013. We calculated the yearly prevalence of NAC followed by RC, RC as first treatment, trimodal therapy, chemotherapy and/or radiation alone, and no treatment. We then identified factors associated with receiving NAC prior to RC.
Results
There was a notable increase in the use of NAC followed by RC over the study period, from 3.68% in 2004 to 14.83% in 2013 (P < 0.001). Factors associated with decreased odds of receiving this regimen included being older, Black, uninsured, less educated, and more burdened by comorbidities. Rates of trimodal therapy and chemotherapy and/or radiation alone remained relatively constant (approximately 5 and 17%, respectively). There was a consistent decline in the proportion of patients who did not receive any treatment, down to 34.20% in 2013.
Conclusion
Trends in localized MIBC treatment have evolved substantially since the early 2000s, and certain patient characteristics are associated with lower odds of receiving the current standard of care. This serves as a foundation from which to judge the impact of the upcoming immunotherapy era on the treatment landscape for this disease.


Similar content being viewed by others
References
Leow JJ, Cole AP, Seisen T et al. (2017) Variations in the costs of radical cystectomy for bladder cancer in the USA. Eur Urol. https://doi.org/10.1016/j.eururo.2017.07.016
Svatek RS, Hollenbeck BK, Holmang S et al (2014) The economics of bladder cancer: costs and considerations of caring for this disease. Eur Urol 66(2):253–262
Cole AP, Dalela D, Hanske J et al (2015) Temporal trends in receipt of adequate lymphadenectomy in bladder cancer 1988–2010. Urol Oncol 33(12):504 e509–517
Leow JJ, Reese S, Trinh QD et al (2015) Impact of surgeon volume on the morbidity and costs of radical cystectomy in the USA: a contemporary population-based analysis. BJU Int 115(5):713–721
Chang SS, Bochner BH, Chou R et al (2017) Treatment of non-metastatic muscle-invasive bladder cancer: AUA/ASCO/ASTRO/SUO guideline. J Urol 198(3):552–559
Grossman HB, Natale RB, Tangen CM et al (2003) Neoadjuvant chemotherapy plus cystectomy compared with cystectomy alone for locally advanced bladder cancer. N Engl J Med 349(9):859–866
Advanced Bladder Cancer Meta-analysis C (2005) Neoadjuvant chemotherapy in invasive bladder cancer: update of a systematic review and meta-analysis of individual patient data advanced bladder cancer (ABC) meta-analysis collaboration. Eur Urol 48(2):202–205 discussion 205–206
Zaid HB, Patel SG, Stimson CJ et al (2014) Trends in the utilization of neoadjuvant chemotherapy in muscle-invasive bladder cancer: results from the National Cancer Database. Urology 83(1):75–80
Chen RC, Shipley WU, Efstathiou JA, Zietman AL (2013) Trimodality bladder preservation therapy for muscle-invasive bladder cancer. J Natl Compr Cancer Netw 11(8):952–960
Cole AP, Friedlander DF, Trinh QD (2018) Secondary data sources for health services research in urologic oncology. Urol Oncol 36(4):165–173
Lerro CC, Robbins AS, Phillips JL, Stewart AK (2013) Comparison of cases captured in the national cancer data base with those in population-based central cancer registries. Ann Surg Oncol 20(6):1759–1765
Seisen T, Sun M, Lipsitz SR et al (2017) Comparative effectiveness of trimodal therapy versus radical cystectomy for localized muscle-invasive urothelial carcinoma of the bladder. Eur Urol 72(4):483–487
Rosen JE, Hancock JG, Kim AW, Detterbeck FC, Boffa DJ (2014) Predictors of mortality after surgical management of lung cancer in the National Cancer Database. Ann Thorac Surg 98(6):1953–1960
Cole AP, Trinh QD (2017) Secondary data analysis: techniques for comparing interventions and their limitations. Curr Opin Urol 27(4):354–359
Donner A, Donald A (1987) Analysis of data arising from a stratified design with the cluster as unit of randomization. Stat Med 6(1):43–52
von der Maase H, Hansen SW, Roberts JT et al (2000) Gemcitabine and cisplatin versus methotrexate, vinblastine, doxorubicin, and cisplatin in advanced or metastatic bladder cancer: results of a large, randomized, multinational, multicenter, phase III study. J Clin Oncol 18(17):3068–3077
van de Putte EE, Mertens LS, Meijer RP et al (2016) Neoadjuvant induction dose-dense MVAC for muscle invasive bladder cancer: efficacy and safety compared with classic MVAC and gemcitabine/cisplatin. World J Urol 34(2):157–162
Choueiri TK, Jacobus S, Bellmunt J et al (2014) Neoadjuvant dose-dense methotrexate, vinblastine, doxorubicin, and cisplatin with pegfilgrastim support in muscle-invasive urothelial cancer: pathologic, radiologic, and biomarker correlates. J Clin Oncol 32(18):1889–1894
Dash A, Galsky MD, Vickers AJ et al (2006) Impact of renal impairment on eligibility for adjuvant cisplatin-based chemotherapy in patients with urothelial carcinoma of the bladder. Cancer 107(3):506–513
Griffiths G, Hall R, Sylvester R, Raghavan D, Parmar MK (2011) International phase III trial assessing neoadjuvant cisplatin, methotrexate, and vinblastine chemotherapy for muscle-invasive bladder cancer: long-term results of the BA06 30894 trial. J Clin Oncol 29(16):2171–2177
Donat SM, Shabsigh A, Savage C et al (2009) Potential impact of postoperative early complications on the timing of adjuvant chemotherapy in patients undergoing radical cystectomy: a high-volume tertiary cancer center experience. Eur Urol 55(1):177–185
Hussain SA, Palmer DH, Lloyd B et al (2012) A study of split-dose cisplatin-based neo-adjuvant chemotherapy in muscle-invasive bladder cancer. Oncol Lett 3(4):855–859
Birtle AJ, Chester JD, Jones RJ (2018) Results of POUT: a phase III randomised trial of perioperative chemotherapy versus surveillance in upper tract urothelial cancer (UTUC). J Clin Oncol 36 (suppl 6S; abstr 407)
Neoadjuvant pembrolizumab in combination with gemcitabine therapy in cis-eligible/ineligible UC subjects (NCT02365766). https://www.clinicaltrials.gov/ct2/show/NCT02365766. Accessed 27 Feb 2018
Pre-surgical study evaluating anti-PD-L1 antibody (durvalumab) plus anti-CTLA-4 (tremelimumab) in patients with muscle-invasive, high-risk urothelial carcinoma who are ineligible for cisplatin-based neoadjuvant chemotherapy (NCT02812420) https://www.clinicaltrials.gov/ct2/show/NCT02812420. Accessed 27 Feb 2018
Vetterlein MW, Wankowicz SAM, Seisen T et al (2017) Neoadjuvant chemotherapy prior to radical cystectomy for muscle-invasive bladder cancer with variant histology. Cancer 123(22):4346–4355
Cole AP, Sun M, Lipsitz SR, Sood A, Kibel AS, Trinh QD (2018) Reassessing the value of high-volume cancer care in the era of precision medicine. Cancer 124(7):1319–1321
Fletcher SA, Gild P, Cole AP et al (2018) The effect of treatment at minority-serving hospitals on outcomes for bladder cancer. Urol Oncol 36(5):238.e7–238.e17
SEER cancer stat facts: bladder cancer https://seer.cancer.gov/statfacts/html/urinb.html. Accessed 1 Mar 2018
Mak RH, Hunt D, Shipley WU et al (2014) Long-term outcomes in patients with muscle-invasive bladder cancer after selective bladder-preserving combined-modality therapy: a pooled analysis of Radiation Therapy Oncology Group protocols 8802, 8903, 9506, 9706, 9906, and 0233. J Clin Oncol 32(34):3801–3809
Acknowledgements
Quoc-Dien Trinh supported by the Brigham Research Institute Fund to Sustain Research Excellence, the Bruce A. Beal and Robert L. Beal Surgical Fellowship, the Genentech Bio-Oncology Career Development Award from the Conquer Cancer Foundation of the American Society of Clinical Oncology, a Health Services Research pilot test grant from the Defense Health Agency, the Clay Hamlin Young Investigator Award from the Prostate Cancer Foundation, and an unrestricted educational grant from the Vattikuti Urology Institute.
Author information
Authors and Affiliations
Contributions
SAF protocol/project development, data collection or management, data analysis, manuscript writing/editing. SSH protocol/project development, data collection or management, data analysis, manuscript writing/editing. MJK data collection or management, data analysis. APC data analysis, manuscript writing/editing. SB data collection or management, data analysis. PG data collection or management, data analysis. MAP data analysis, manuscript writing/editing. ASK data analysis, manuscript writing/editing. MS data analysis, manuscript writing/editing. TKC data analysis, manuscript writing/editing. QDT protocol/project development, data collection or management, data analysis, manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interest
QDT reports honoraria from Bayer and Astellas and research funding from Intuitive Surgical. ASK reports consulting fees from Sanofi and Profound Medical; GPS is a consultant for BMS, Exelixis, Bayer, Sanofi, Pfizer, Novartis, Eisai, Janssen, Amgen, Astrazeneca, Merck, Genentech, Astellas/Agensys, and reports research support to institution from Bayer, Amgen, Boehringer-Ingelheim, Merck, Sanofi, Pfizer.
Research involving human participants and/or animals
We used completely de-identified data from the National Cancer Database. No identifiable humans were involved. Our study did not involve animals. Thus, our study was exempt from formal review by the Brigham and Women’s Hospital institutional review board.
Informed consent
All patient data were de-identified/anonymous and collected from hospitals that gave their informed consent to collect this information for the database.
Rights and permissions
About this article
Cite this article
Fletcher, S.A., Harmouch, S.S., Krimphove, M.J. et al. Characterizing trends in treatment modalities for localized muscle-invasive bladder cancer in the pre-immunotherapy era. World J Urol 36, 1767–1774 (2018). https://doi.org/10.1007/s00345-018-2371-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-018-2371-y