Abstract
Purpose
Holmium laser enucleation of the prostate (HoLEP) has become a popular alternative to TURP for desobstructive prostate surgery. The prevalence of incidental prostate cancer (iPCa) during surgery varies depending on many preoperative factors. To evaluate whether the surgical procedure itself (HoLEP vs. TURP) influences iPCa detection, we performed a case-by-case matched-pair analysis.
Methods
Preoperative patient age, total PSA, and prostate volume were used as matching criteria. Descriptive statistics were used to confirm matching quality. Parameters were analyzed by Fisher’s exact test and T test or Mann–Whitney U test for dichotomous and continuous variables, respectively. Uni- and multivariate logistic regression analyses were performed to identify predictors for iPCa detection.
Results
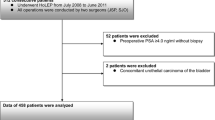
60 out of 136 patients after HoLEP and 60 out of 1220 patients after bipolar TURP (bTURP) could be included. Mean patient age was 71.5 and 70.3 years in the HoLEP and bTURP group, respectively. Median preoperative total PSA was 4.42 ng/ml for HoLEP and 4.33 ng/ml for bTURP patients. Median preoperative prostate volume was 75.0 cc in both groups. Mean percentage of tissue removed by HoLEP and bTURP was 63.5 and 49.5% (p < 0.001), respectively. IPCa was found in 23.3% of HoLEP specimens compared to 8.3% in bTURP (p = 0.043). PSA density was the only independent predictor for iPCa detection.
Conclusions
In this first matched-pair analysis, HoLEP provides a significantly higher iPCa detection rate than bTURP. This might be a result of a more efficient tissue removal during HoLEP. PSA density was the only independent risk factor for iPCa.
Similar content being viewed by others
References
Ahyai S, Gilling P, Kaplan SA et al (2010) Meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic enlargement. Eur Urol 58:384–397
Cornu JN, Ahyai S, Bachmann A et al (2015) A systematic review and meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic obstruction: an update. Eur Urol 67(6):1066–1096
Kuntz RM, Lehrich K, Ahyai S (2004) Does perioperative outcome of transurethral holmium laser enucleation of the prostate depend on prostate size? J Endourol 18:183–188
Kuntz RM, Lehrich K, Ahyai S (2008) Holmium laser enucleation of the prostate versus open prostatectomy for prostates greater than 100 grams: 5-year follow-up results of a randomised clinical trial. Eur Urol 53(1):160–166
Kuntz RM, Lehrich K, Ahyai S (2004) Transurethral holmium laser enucleation of the prostate compared with transvesical open prostatectomy: 18-month follow-up of a randomized trial. J Endourol 18(2):189–191
Gravas S, Bach T, Drake M et al (2017) Guidelines on the management of non-neurogenic male lower urinary tract symptoms (LUTS), incl. Benign prostatic obstruction (BPO). http://uroweb.org/wp-content/uploads/13-Non-Neurogenic-Male- LUTS_2017_web.pdf
Mottet N, Bellmunt J, Briers E et al (2017) EAU-ESTRO-ESUR-SIOG guidelines on prostate cancer. http://uroweb.org/wp-content/uploads/09-Prostate-Cancer_2017_web.pdf
Serefoglu EC, Altinova S, Ugras NS, Akincioglu E, Asil E, Balbay MD (2013) How reliable is 12-core prostate biopsy procedure in the detection of prostate cancer? Can Urol Assoc J 7(5–6):E293–E298
Naspro R, Freschi M, Salonia A et al (2004) Holmium laser enucleation versus transurethral resection of the prostate. Are histological findings comparable? J Urol 171(3):1203–1206
Argyropoulos A, Doumas K, Farmakis A, Aristas O, Kontogeorgos G, Lykourinas M (2005) Characteristics of patients with stage T1b incidental prostate cancer. Scand J Urol Nephrol 39(4):289–293
Jones JS, Follis HW, Johnson JR (2009) Probability of finding T1a and T1b (incidental) prostate cancer during TURP has decreased in the PSA era. Prostate Cancer Prostatic Dis 12(1):57–60
Melchior S, Hadaschik B, Thüroff S, Thomas C, Gillitzer R, Thüroff J (2009) Outcome of radical prostatectomy for incidental carcinoma of the prostate. BJU Int 103(11):1478–1481
Nunez R, Hurd KJ, Noble BN, Castle EP, Andrews PE, Humphreys MR (2011) Incidental prostate cancer revisited: early outcomes after holmium laser enucleation of the prostate. Int J Urol 18(7):543–547
Voigt S, Hüttig F, Koch R et al (2011) Risk factors for incidental prostate cancer who should not undergo vaporization of the prostate for benign prostate hyperplasia? Prostate 71(12):1325–1331
Kim M, Song SH, Ku JH, Oh SJ, Paick JS (2014) Prostate cancer detected after Holmium laser enucleation of prostate (HoLEP): significance of transrectal ultrasonography. Int Urol Nephrol 46(11):2079–2085
Rivera ME, Frank I, Viers BR, Rangel LJ, Krambeck AE (2014) Holmium laser enucleation of the prostate and perioperative diagnosis of prostate cancer: an outcomes analysis. J Endourol 28(6):699–703
Sakamoto H, Matsumoto K, Hayakawa N et al (2014) Preoperative parameters to predict incidental (T1a and T1b) prostate cancer. Can Urol Assoc J 8(11–12):815–820
Otto B, Barbieri C, Lee R et al (2014) Incidental prostate cancer in transurethral resection of the prostate specimens in the modern era. Adv Urol 627290
Bhojani N, Boris RS, Monn MF, Mandeville JA, Lingeman JE (2015) Coexisting prostate cancer found at the time of holmium laser enucleation of the prostate for benign prostatic hyperplasia: predicting its presence and grade in analyzed tissue. J Endourol 29(1):41–46
Elkoushy MA, Elshal AM, Elhilali MM (2015) Incidental prostate cancer diagnosis during holmium laser enucleation: assessment of predictors, survival, and disease progression. Urology 86(3):552–557
Herlemann A, Wegner K, Roosen A et al (2017) “Finding the needle in a haystack”: oncologic evaluation of patients treated for LUTS with holmium laser enucleation of the prostate (HoLEP) versus transurethral resection of the prostate (TURP). World J Urol 35(11):1777–1782
Skolarikos A, Rassweiler J, de la Rosette JJ et al (2016) Safety and efficacy of bipolar versus monopolar transurethral resection of the prostate in patients with large prostates or severe lower urinary tract symptoms: post hoc analysis of a european multicenter randomized controlled trial. J Urol 195(3):677–684
Starkman JS, Santucci RA (2005) Comparison of bipolar transurethral resection of the prostate with standard transurethral prostatectomy: shorter stay, earlier catheter removal and fewer complications. BJU Int 95(1):69–71
Fung BT, Li SK, Yu CF, Lau BE, Hou SS (2005) Prospective randomized controlled trial comparing plasmakinetic vaporesection and conventional transurethral resection of the prostate. Asian J Surg 28(1):24–28
De Sio M, Autorino R, Quarto G et al (2006) Gyrus bipolar versus standard monopolar transurethral resection of the prostate: a randomized prospective trial. Urology 67(1):69–72
Jhanwar A, Sinha RJ, Bansal A, Prakash G, Singh K, Singh V (2017) Outcomes of transurethral resection and holmium laser enucleation in more than 60 g of prostate: a prospective randomized study. Urol Ann 9(1):45–50
Bach T, Geavlete B, Pfeiffer D, Wendt-Nordahl G, Michel MS, Gross AJ (2009) TURP in patients with biopsy-proven prostate cancer: sensitivity for cancer detection. Urology 73(1):100–104
Author information
Authors and Affiliations
Contributions
B. Rosenhammer: project development, data collection and analysis, and manuscript writing. E.M. Lausenmeyer: project development, data collection, and manuscript editing. R. Mayr: manuscript editing. M. Burger: manuscript editing. C. Eichelberg: project development, and manuscript writing and editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare to have no conflicts of interest. There was no funding for this study.
Research involving human participants and/or animals
This article does not contain any studies with animals performed by any of the authors.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study protocol (#17-777-101) was approved by the ethics committee of the University of Regensburg.
Informed consent
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Rosenhammer, B., Lausenmeyer, E.M., Mayr, R. et al. HoLEP provides a higher prostate cancer detection rate compared to bipolar TURP: a matched-pair analysis. World J Urol 36, 2035–2041 (2018). https://doi.org/10.1007/s00345-018-2353-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-018-2353-0