Abstract
Purpose
To compare our experience with salvage laparoscopic pyeloplasty, using a matched control set of primary laparoscopic pyeloplasty patients.
Methods
We retrospectively reviewed patients who underwent laparoscopic pyeloplasty from 1996 to 2014 by a single surgeon. At least 12 months of follow-up was required. Salvage patients were matched 1:3 with primary patients. Matching was based on age ±5 years, body mass index (BMI) ±5, and type of pyeloplasty (dismembered vs. non-dismembered). Primary outcome was failure as defined as re-intervention following laparoscopic pyeloplasty (does not include temporary stenting without definitive retreatment).
Results
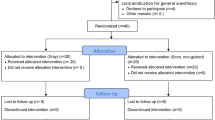
Of 128 laparoscopic pyeloplasty procedures, ten were salvage. These patients were matched to 26 patients who underwent a primary laparoscopic pyeloplasty in a 1:3 manner. One salvage pyeloplasty failed to match due to BMI, and the closest matches were made. Four salvage patients had one overlapping match, reducing the primary group to 26 patients. There were no differences in pre-, intra-, and postoperative variables between groups, except for operative time (salvage 247 min, primary 175 min, p = 0.03). With similar duration of radiologic and symptomatic follow-up, there was no significant difference in the rate of freedom from intervention.
Conclusion
When matching for factors that could affect success, salvage laparoscopic pyeloplasty performed as well as primary pyeloplasty except for a longer operative time. In experienced hands, salvage laparoscopic pyeloplasty for ureteropelvic junction obstruction recurrence after prior pyeloplasty is a safe and effective procedure, and should be considered an excellent alternative to the more commonly recommended endopyelotomy.

Similar content being viewed by others
References
Jabbour ME, Goldfischer ER, Klima WJ et al (1998) Endopyelotomy after failed pyeloplasty: the long-term results. J Urol 160(3):690–692 (discussion 692–693)
Patel T, Kellner CP, Katsumi H et al (2011) Efficacy of endopyelotomy in patients with secondary ureteropelvic junction obstruction. J Endourol 25:587–591
Varkarakis IM, Bhayani SB, Allaf ME et al (2004) Management of secondary ureteropelvic junction obstruction after failed primary laparoscopic pyeloplasty. J Urol 172:180–182
Basiri A, Behjati S, Zand S et al (2007) Laparoscopic pyeloplasty in secondary ureteropelvic junction obstruction after failed open surgery. J Endourol 21(9):1045–1051
Brito AH, Mitre AI, Srougi M (2007) Laparoscopic pyeloplasty in secondary obstruction. J Endourol 21:1481–1484
Levin BM, Herrell SD (2006) Salvage laparoscopic pyeloplasty in the worst case scenario: after both failed open repair and endoscopic salvage. J Endourol 20:808–812
Ng CS, Yost AJ, Streem SB (2003) Management of failed primary intervention for ureteropelvic junction obstruction: 12-year, single-center experience. Urology 61:291–296
Shadpour P, Haghighi R, Maghsoudi R et al (2011) Laparoscopic redo pyeloplasty after failed open surgery. Urol J 8:31–37
Shapiro EY, Cho JS, Srinivasan A et al (2009) Long-term follow-up for salvage laparoscopic pyeloplasty after failed open pyeloplasty. Urology 73:115–118
Sundaram CP, Grubb RL, Rehman J et al (2003) Laparoscopic pyeloplasty for secondary ureteropelvic junction obstruction. J Urol 169:2037–2040
Lucas SM, Sundaram CP, Wolf JS et al (2012) Factors that impact the outcome of minimally invasive pyeloplasty: results of the multi-institutional laparoscopic and robotic pyeloplasty collaborative group. J Urol 187:522–527
Autorino R, Eden C, El-Ghoneimi A et al (2014) Robot-assisted and laparoscopic repair of ureteropelvic junction obstruction: a systematic review and meta-analysis. Eur Urol 65:430–452
Tan H-J, Ye Z, Roberts WW et al (2011) Failure after laparoscopic pyeloplasty: prevention and management. J Endourol 25:1457–1462
Vannahme M, Mathur S, Davenport K et al (2014) The management of secondary pelvi-ureteric junction obstruction––a comparison of pyeloplasty and endopyelotomy. BJU Int 113:108–112
Cadeddu JA (2014) Re: The management of secondary pelvi-ureteric junction obstruction––a comparison of pyeloplasty and endopyelotomy. J Urol 192(2):450
Piaggio LA, Noh PH, González R (2007) Reoperative laparoscopic pyeloplasty in children: comparison with open surgery. J Urol 177(5):1878–1882
Niver BE, Agalliu I, Bareket R et al (2012) Analysis of robotic-assisted laparoscopic pyleloplasty for primary versus secondary repair in 119 consecutive cases. Urology 79:689–694
Atug F, Burgess SV, Castle EP et al (2006) Role of robotics in the management of secondary ureteropelvic junction obstruction. Int J Clin Pract 60:9–11
Eden C, Gianduzzo T, Chang C et al (2004) Extraperitoneal laparoscopic pyeloplasty for primary and secondary ureteropelvic junction obstruction. J Urol 172:2308–2311
Lee Z, Moore B, Giusto L et al (2015) Use of indocyanine green during robot-assisted ureteral reconstructions. Eur Urol 67:291–298
Inagaki T, Rha KH, Ong AM et al (2005) Laparoscopic pyeloplasty: current status. BJU Int 95(Suppl 2):102–105
Madi R, Roberts WW, Wolf JS (2008) Late failures after laparoscopic pyeloplasty. Urology 71:677–680
Author’s contribution
S.N. Ambani was involved in project development, data collection, analysis, and manuscript writing/editing; D. Yang was involved in data collection and analysis; and J.S. Wolf, Jr., was involved in project development, data analysis, and manuscript editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Ambani, S.N., Yang, D.Y. & Wolf, J.S. Matched comparison of primary versus salvage laparoscopic pyeloplasty. World J Urol 35, 951–956 (2017). https://doi.org/10.1007/s00345-016-1951-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-016-1951-y