Abstract
Objectives
To test whether multidetector computed tomography (MDCT) could completely replace transoesophageal echocardiography (TEE) to detect left atrial appendage (LAA) thrombi in atrial fibrillation (AF) patients using a large sample size.
Methods
783 patients with AF who underwent MDCT and TEE before catheter ablation were retrospectively included. Demographic data were obtained. Two radiologists blinded to clinical data made the imaging diagnosis.
Results
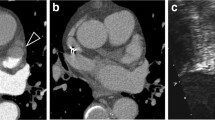
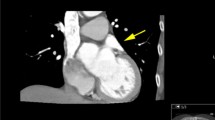
Most of the patients (96.2 %) had a CHA2DS2-VASc score (congestive heart failure, hypertension, age ≥ 75 years old (doubled), diabetes, stroke/transient ischaemic attack/thromboembolism (doubled), vascular disease, age 65–74 years, female sex) ≤ 3. Eight thrombi were identified by TEE, all of which were detected by MDCT; no thrombus was observed with TEE without the observation of filling defects by late-phase MDCT scanning in any of the patients. Using TEE as reference standard, the sensitivity, specificity, positive predictive value and negative predictive value of MDCT for thrombus detection were 100 %, 95.74 % (95 % CI 94.33 %–97.15 %), 19.51 % (95 % CI 16.73 %–22.29 %) and 100 %, respectively.
Conclusions
For AF patients with low risk of stroke, when MDCT images showed no filling defect in the late phase, TEE prior to catheter ablation can be avoided.
Key Points
• MDCT can help detect the presence of LAA thrombus.
• TEE can be avoided when late-phase MDCT shows no filling defect.
• TEE is required in patients whose MDCT images indicate thrombus.



Similar content being viewed by others
Abbreviations
- AF:
-
Atrial fibrillation
- CA:
-
Catheter ablation
- CHA2DS2-VASc:
-
Congestive heart failure, hypertension, age ≥ 75 years (doubled), diabetes previous stroke/transient ischaemic attack/thromboembolism (doubled), vascular disease, age 65–74 years, and sex category (female)
- CHF:
-
Congestive heart failure
- LAA:
-
Left atrial appendage
- LAD:
-
Left atrial dimension
- LVEDD:
-
Left ventricular end-diastolic dimension
- LVEF:
-
Left ventricular ejection fraction
- MDCT:
-
Multidetector computed tomography
- SEC:
-
Spontaneous echo contrast
- TEE:
-
Transoesophageal echocardiography
- TIA:
-
Transient ischaemic attack
- VASc:
-
Vascular diseases
References
European Heart Rhythm A, European Cardiac Arrhythmia S, American College of Cardiology et al (2007) HRS/EHRA/ECAS expert Consensus Statement on catheter and surgical ablation of atrial fibrillation: recommendations for personnel, policy, procedures and follow-up. A report of the Heart Rhythm Society (HRS) Task Force on catheter and surgical ablation of atrial fibrillation. Heart Rhythm 4:816–861
Hilberath JN, Oakes DA, Shernan SK, Bulwer BE, D'Ambra MN, Eltzschig HK (2010) Safety of transesophageal echocardiography. J Am Soc Echocardiogr 23:1115–1127
Chen J, Yang ZG, Xu HY, Shi K, Long QH, Guo YK (2017) Assessments of pulmonary vein and left atrial anatomical variants in atrial fibrillation patients for catheter ablation with cardiac CT. Eur Radiol 27:660–670
Boucebci S, Pambrun T, Velasco S, Duboe PO, Ingrand P, Tasu JP (2016) Assessment of normal left atrial appendage anatomy and function over gender and ages by dynamic cardiac CT. Eur Radiol 26:1512–1520
Budoff MJ, Shittu A, Hacioglu Y et al (2014) Comparison of transesophageal echocardiography versus computed tomography for detection of left atrial appendage filling defect (thrombus). Am J Cardiol 113:173–177
Dorenkamp M, Sohns C, Vollmann D et al (2013) Detection of left atrial thrombus during routine diagnostic work-up prior to pulmonary vein isolation for atrial fibrillation: role of transesophageal echocardiography and multidetector computed tomography. Int J Cardiol 163:26–33
Gottlieb I, Pinheiro A, Brinker JA et al (2008) Diagnostic accuracy of arterial phase 64-slice multidetector CT angiography for left atrial appendage thrombus in patients undergoing atrial fibrillation ablation. J Cardiovasc Electrophysiol 19:247–251
Gudrun M, Feuchtner M, Dichtl W et al (2008) Diagnostic accuracy of cardiac 64-slice computed tomography in detecting atrial thrombi: comparative study with transesophageal echocardiography and cardiac surgery. Invest Radiol 43:794–801
Hur J, Kim YJ, Lee HJ et al (2009) Cardiac computed tomographic angiography for detection of cardiac sources of embolism in stroke patients. Stroke 40:2073–2078
Hur J, Kim YJ, Ha JW et al (2009) Left atrial appendage thrombi in stroke patients: Detection with two-phase cardiac CT angiography versus transesophageal echocardiography. Radiology 251:683–690
Kim YY, Klein AL, Halliburton SS et al (2007) Left atrial appendage filling defects identified by multidetector computed tomography in patients undergoing radiofrequency pulmonary vein antral isolation: a comparison with transesophageal echocardiography. Am Heart J 154:1199–1205
Maltagliati A, Pontone G, Annoni A et al (2011) Multidetector computed tomography vs multiplane transesophageal echocardiography in detecting atrial thrombi in patients candidate to radiofrequency ablation of atrial fibrillation. Int J Cardiol 152:251–254
Martinez MW, Kirsch J, Williamson EE et al (2009) Utility of nongated multidetector computed tomography for detection of left atrial thrombus in patients undergoing catheter ablation of atrial fibrillation. JACC Cardiovasc Imaging 2:69–76
Patel A, Au E, Donegan K et al (2008) Multidetector row computed tomography for identification of left atrial appendage filling defects in patients undergoing pulmonary vein isolation for treatment of atrial fibrillation: comparison with transesophageal echocardiography. Heart Rhythm 5:253–260
Sawit ST, Garcia-Alvarez A, Suri B et al (2012) Usefulness of cardiac computed tomographic delayed contrast enhancement of the left atrial appendage before pulmonary vein ablation. Am J Cardiol 109:677–684
Tang RB, Dong JZ, Zhang ZQ et al (2008) Comparison of contrast enhanced 64-slice computed tomography and transesophageal echocardiography in detection of left atrial thrombus in patients with atrial fibrillation. J Interv Card Electrophysiol 22:199–203
Madan A, Yan W, Byrne P et al (2016) Significance of left atrial appendage filling defects on cardiac CT prior to pulmonary vein isolation for atrial fibrillation. Int J Cardiol 203:520–522
Lazoura O, Ismail TF, Pavitt C et al (2016) A low-dose, dual-phase cardiovascular CT protocol to assess left atrial appendage anatomy and exclude thrombus prior to left atrial intervention. Int J Cardiovasc Imaging 32:347–354
Zou H, Zhang Y, Tong J, Liu Z (2015) Multidetector computed tomography for detecting left atrial/left atrial appendage thrombus: a meta-analysis. Intern Med J 45:1044–1053
Romero J, Husain SA, Kelesidis I, Sanz J, Medina HM, Garcia MJ (2013) Detection of left atrial appendage thrombus by cardiac computed tomography in patients with atrial fibrillation: a meta-analysis. Circ Cardiovasc Imaging 6:185–194
Martinez MW, Lin G, Williamson EE, Brady PA (2009) Dual source computed tomography with delayed imaging for left atrial appendage thrombus compared with transoesophageal echocardiography. Heart 95:460
Kim SC, Chun EJ, Choi SI et al (2010) Differentiation between spontaneous echocardiographic contrast and left atrial appendage thrombus in patients with suspected embolic stroke using two-phase multidetector computed tomography. Am J Cardiol 106:1174–1181
January CT, Wann LS, Alpert JS et al (2014) 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association task force on practice guidelines and the Heart Rhythm Society. J Am Coll Cardiol 64:e1–76
Jakobs TF, Becker CR, Ohnesorge B et al (2002) Multislice helical CT of the heart with retrospective ECG gating: reduction of radiation exposure by ECG-controlled tube current modulation. Eur Radiol 12:1081–1086
Hur J, Kim YJ, Lee HJ et al (2011) Dual-enhanced cardiac CT for detection of left atrial appendage thrombus in patients with stroke: a prospective comparison study with transesophageal echocardiography. Stroke 42:2471–2477
Hur J, Kin YJ, Lee HJ et al (2012) Cardioembolic stroke: dual-energy cardiac CT for differentiation of left atrial appendage thrombus and circulatory stasis. Radiology 263:688–695
Sadanandan S, Sherrid MV (2000) Clinical and echocardiographic characteristics of left atrial spontaneous echo contrast in sinus rhythm. J Am Coll Cardiol 35:1932–1938
Calkins H, Kuck KH, Cappato R et al (2012) 2012 HRS/EHRA/ECAS Expert consensus statement on catheter and surgical ablation of atrial fibrillation: recommendations for patient selection, procedural techniques, patient management and follow-up, definitions, endpoints, and research trial design. Europace 14:528–606
Acknowledgements
The authors thank Lei Han for MDCT consulting services.
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Min Tang.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• diagnostic study
• performed at one institution
Rights and permissions
About this article
Cite this article
Zhai, Z., Tang, M., Zhang, S. et al. Transoesophageal echocardiography prior to catheter ablation could be avoided in atrial fibrillation patients with a low risk of stroke and without filling defects in the late-phase MDCT scan: A retrospective analysis of 783 patients. Eur Radiol 28, 1835–1843 (2018). https://doi.org/10.1007/s00330-017-5172-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-017-5172-6