Abstract
Objective
The aim of this study was to assess the safety and efficacy of extended liver venous deprivation (eLVD), i.e. combination of right portal vein embolisation and right (accessory right) and middle hepatic vein embolisation before major hepatectomy for future remnant liver (FRL) functional increase.
Methods
eLVD was performed in non-cirrhotic patients referred for major hepatectomy in a context of small FRL (baseline FRL <25% of the total liver volume or FRL function <2.69%/min/m2). All patients underwent 99mTc-mebrofenin hepatobiliary scintigraphy (HBS) and computed tomographic evaluations.
Results
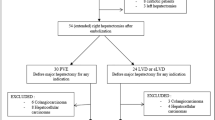
Ten consecutive patients underwent eLVD before surgery for liver metastases (n = 8), Klatskin tumour (n = 1) and gallbladder carcinoma (n = 1). FRL function increased by 64.3% (range = 28.1-107.5%) at day 21. In patients with serial measurements, maximum FRL function was at day 7 (+65.7 ± 16%). The FRL volume increased by +53.4% at 7 days (+25 ± 8 cc/day). Thirty-one days (range = 22-45 days) after eLVD, 9/10 patients were resected. No post-hepatectomy liver failure was reported. Two grade II and one grade III complications (Dindo-Clavien classification) occurred. No patient died with-in 90 days following surgery.
Conclusions
eLVD is safe and provides a marked and very rapid increase in liver function, unprecedented for an interventional radiology procedure.
Key Points
• eLVD is safe
• eLVD provides a marked and very rapid increase in liver function
• After eLVD, the FRL-F increased by 64.3% (28.1-107.5%) at day 21
• After eLVD, the maximum FRL-F was obtained at day 7 (+65.7 ± 16%)
• After eLVD, the FRL volume increased by +53.4% at 7 days (+25 ± 8 cc/day)






Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- PVE:
-
portal vein embolisation
- FRL:
-
future remnant liver
- FRL-V:
-
future remnant liver volume
- FRL-F:
-
future remnant liver function
- HV:
-
hepatic vein
- HVE:
-
hepatic vein embolisation
- ALPPS:
-
associating liver partition and portal vein ligation for staged hepatectomy
- MHV:
-
middle hepatic vein
- PHLF:
-
post-hepatectomy liver failure
- LVD:
-
liver venous deprivation
- eLVD:
-
extended liver venous deprivation
- HBS:
-
hepatobiliary scintigraphy
- AST:
-
aspartate aminotransferase
- ALT:
-
serum alanine aminotransferase
- GGT:
-
gamma-glutamyl-transpeptidase
- ALP:
-
alkaline phosphatase
- PT:
-
prothrombin time
- LDLT:
-
living donor liver transplantation
References
Abulkhir A, Limongelli P, Healey AJ et al (2008) Preoperative portal vein embolization for major liver resection: a meta-analysis. Ann Surg 247:49–57
de Graaf W, van Lienden KP, van den Esschert JW, Bennink RJ, van Gulik TM (2011) Increase in future remnant liver function after preoperative portal vein embolization. Br J Surg 98:825–834
Asencio JM, Vaquero J, Olmedilla L, Garcia Sabrido JL (2013) "Small-for-flow" syndrome: shifting the "size" paradigm. Med Hypotheses 80:573–577
Cieslak KP, Olthof PB, van Lienden KP et al (2015) Assessment of liver function using (99m)Tc-mebrofenin hepatobiliary scintigraphy in ALPPS (associating liver partition and portal vein ligation for staged hepatectomy). Case Rep Gastroenterol 9:353–360
Zappa M, Dondero F, Sibert A, Vullierme MP, Belghiti J, Vilgrain V (2009) Liver regeneration at day 7 after right hepatectomy: global and segmental volumetric analysis by using CT. Radiology 252:426–432
van Lienden KP, van den Esschert JW, de Graaf W et al (2013) Portal vein embolization before liver resection: a systematic review. Cardiovasc Intervent Radiol 36:25–34
Pommier R, Ronot M, Cauchy F et al (2014) Colorectal liver metastases growth in the embolized and non-embolized liver after portal vein embolization: influence of initial response to induction chemotherapy. Ann Surg Oncol 21:3077–3083
Schnitzbauer AA, Lang SA, Goessmann H et al (2012) Right portal vein ligation combined with in situ splitting induces rapid left lateral liver lobe hypertrophy enabling 2-staged extended right hepatic resection in small-for-size settings. Ann Surg 255:405–414
Schadde E, Raptis DA, Schnitzbauer AA et al (2015) Prediction of mortality after ALPPS stage-1: an analysis of 320 patients from the International ALPPS Registry. Ann Surg 262:780–785, discussion 785-786
Hwang S, Lee SG, Ko GY et al (2009) Sequential preoperative ipsilateral hepatic vein embolization after portal vein embolization to induce further liver regeneration in patients with hepatobiliary malignancy. Ann Surg 249:608–616
Guiu B, Chevallier P, Denys A et al (2016) Simultaneous trans-hepatic portal and hepatic vein embolization before major hepatectomy: the liver venous deprivation technique. Eur Radiol. doi:10.1007/s00330-016-4291-9
Nakamura S, Tsuzuki T (1981) Surgical anatomy of the hepatic veins and the inferior vena cava. Surg Gynecol Obstet 152:43–50
Sano K, Makuuchi M, Miki K et al (2002) Evaluation of hepatic venous congestion: proposed indication criteria for hepatic vein reconstruction. Ann Surg 236:241–247
Akamatsu N, Sugawara Y, Kaneko J et al (2003) Effects of middle hepatic vein reconstruction on right liver graft regeneration. Transplantation 76:832–837
de Graaf W, Bennink RJ, Vetelainen R, van Gulik TM (2010) Nuclear imaging techniques for the assessment of hepatic function in liver surgery and transplantation. J Nucl Med 51:742–752
Petrowsky H (2016) Does volume translate in function in interstage associating liver partition and portal vein ligation for staged hepatectomy?: Commentary on "Drop of total liver function in the interstages of the new associating liver partition and portal vein ligation for staged hepatectomy technique: analysis of the auxiliary liver by hepatobiliary iminodiacetic acid scintigraphy". Ann Surg 263, e35
de Graaf W, van Lienden KP, Dinant S et al (2010) Assessment of future remnant liver function using hepatobiliary scintigraphy in patients undergoing major liver resection. J Gastrointest Surg 14:369–378
Truant S, Baillet C, Deshorgue AC et al (2016) Drop of total liver function in the interstages of the new associating liver partition and portal vein ligation for staged hepatectomy technique: analysis of the "Auxiliary Liver" by HIDA scintigraphy. Ann Surg 263:e33–34
Oldhafer F, Ringe KI, Timrott K et al (2016) Monitoring of liver function in a 73-year old patient undergoing 'Associating Liver Partition and Portal vein ligation for Staged hepatectomy': case report applying the novel liver maximum function capacity test. Patient Saf Surg 10:16
Truant S, Baillet C, Deshorgue AC et al (2016) Hepatobiliary scintigraphy in ALPPS: a response. Ann Surg. doi:10.1097/SLA.0000000000001941
Shindoh J, Vauthey JN, Zimmitti G et al (2013) Analysis of the efficacy of portal vein embolization for patients with extensive liver malignancy and very low future liver remnant volume, including a comparison with the associating liver partition with portal vein ligation for staged hepatectomy approach. J Am Coll Surg 217:126–133, discussion 133-124
Bennink RJ, Dinant S, Erdogan D et al (2004) Preoperative assessment of postoperative remnant liver function using hepatobiliary scintigraphy. J Nucl Med 45:965–971
Ekman M, Fjälling M, Friman S, Carlson S, Volkmann R (1996) Liver uptake function measured by IODIDA clearance rate in liver transplant patients and healthy volunteers. Nucl Med Commun 17:235–242
Croome KP, Hernandez-Alejandro R, Parker M, Heimbach J, Rosen C, Nagorney DM (2015) Is the liver kinetic growth rate in ALPPS unprecedented when compared with PVE and living donor liver transplant? A multicentre analysis. HPB (Oxford) 17:477–484
Scatton O, Plasse M, Dondero F, Vilgrain V, Sauvanet A, Belghiti J (2008) Impact of localized congestion related to venous deprivation after hepatectomy. Surgery 143:483–489
De Baere T, Roche A, Elias D, Lasser P, Lagrange C, Bousson V (1996) Preoperative portal vein embolization for extension of hepatectomy indications. Hepatology 24:1386–1391
Guiu B, Bize P, Gunthern D, Demartines N, Halkic N, Denys A (2013) Portal vein embolization before right hepatectomy: improved results using n-Butyl-Cyanoacrylate compared to microparticles plus coils. Cardiovasc Intervent Radiol. doi:10.1007/s00270-013-0565-7
Balzan S, Belghiti J, Farges O et al (2005) The "50-50 criteria" on postoperative day 5: an accurate predictor of liver failure and death after hepatectomy. Ann Surg 242:824–828, discussion 828-829
Mullen JT, Ribero D, Reddy SK et al (2007) Hepatic insufficiency and mortality in 1,059 noncirrhotic patients undergoing major hepatectomy. J Am Coll Surg 204:854–862, discussion 862-854
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Mise Y, Hasegawa K, Satou S et al (2011) Venous reconstruction based on virtual liver resection to avoid congestion in the liver remnant. Br J Surg 98:1742–1751
Ko GY, Hwang S, Sung KB, Gwon DI, Lee SG (2010) Interventional oncology: new options for interstitial treatments and intravascular approaches: right hepatic vein embolization after right portal vein embolization for inducing hypertrophy of the future liver remnant. J Hepatobiliary Pancreat Sci 17:410–412
Schadde E, Ardiles V, Slankamenac K et al (2014) ALPPS offers a better chance of complete resection in patients with primarily unresectable liver tumors compared with conventional-staged hepatectomies: results of a multicenter analysis. World J Surg 38:1510–1519
Truant S, Scatton O, Dokmak S et al (2015) Associating liver partition and portal vein ligation for staged hepatectomy (ALPPS): impact of the inter-stages course on morbi-mortality and implications for management. Eur J Surg Oncol 41:674–682
Buac S, Schadde E, Schnitzbauer AA, Vogt K, Hernandez-Alejandro R (2016) The many faces of ALPPS: surgical indications and techniques among surgeons collaborating in the international registry. HPB (Oxford) 18:442–448
Dinant S, de Graaf W, Verwer BJ et al (2007) Risk assessment of posthepatectomy liver failure using hepatobiliary scintigraphy and CT volumetry. J Nucl Med 48:685–692
Erdogan D, Heijnen BHM, Bennink RJ et al (2004) Preoperative assessment of liver function: a comparison of 99mTc-mebrofenin scintigraphy with indocyanine green clearance test. Liver Int 24:117–123
Dinant S, Graaf W, Verwer BJ et al (2007) Risk assessment of posthepatectomy liver failure using hepatobiliary scintigraphy and CT volumetry. J Nucl Med 48:685–692
Kwon AH, Matsui Y, Kaibori M, Kamiyama Y (2004) Functional hepatic regeneration following hepatectomy using galactosyl-human serum albumin liver scintigraphy. Transplant Proc 36:2257–2260
Imai K, Benitez CC, Allard MA et al (2015) Failure to achieve a 2-stage hepatectomy for colorectal liver metastases: how to prevent it? Ann Surg 262:772–778, discussion 778-779
Acknowledgements
The authors thank Dr. Hélène de Forges for editing and writing assistance, Dr. Julie Carr for revising the English, Dr. Raphael Tetreau for the CT-scan acquisitions and Prof. Samir Jaber for his helpful assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Prof. Boris Guiu.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Funding
The authors state that this work has not received any funding.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Ethical approval
Institutional Review Board approval was obtained.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Methodology
• retrospective
• observational study
• performed at one institution
Rights and permissions
About this article
Cite this article
Guiu, B., Quenet, F., Escal, L. et al. Extended liver venous deprivation before major hepatectomy induces marked and very rapid increase in future liver remnant function. Eur Radiol 27, 3343–3352 (2017). https://doi.org/10.1007/s00330-017-4744-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-017-4744-9