Abstract
Objective
The aim of this study was to evaluate the safety and effectiveness of a supervised walking program in women with primary Sjögren’s syndrome (pSS).
Methods
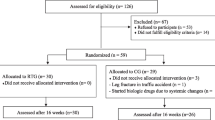
Forty-five sedentary women fulfilling the American European Consensus Criteria for pSS were randomized to a training group (TG, n = 23) or control group (CG, n = 22). Patients in the TG were submitted to supervise walking three times a week for 16 weeks. The patients of the CG were instructed to not perform any kind of regular physical exercise. Physical fitness [maximum oxygen uptake (VO2max) and distance], EULAR Sjögren’s Syndrome Disease Activity Index (ESSDAI), hematological tests, and Medical Outcomes Study 36 (SF-36) were assessed at baseline and week 16. In addition, EULAR Sjögren’s Syndrome Patient Reported Index (ESSPRI), Functional Assessment of Chronic Illness Therapy Fatigue Subscale (FACIT-fatigue), and Beck Depression Inventory (BDI) were measured prior to intervention, after 8 and 16 weeks. Patient global assessment of response to therapy was completed at the final assessment. An intent-to-treat analysis was performed.
Results
After 16 weeks, the mean change of VO2max (ml/kg/min), distance, and FACIT-fatigue were higher in the TG than in the CG (p = 0.016, p = 0.043 and p = 0.030, respectively). Improved cardiorespiratory fitness was associated with improvements in fatigue scores and physical components of quality of life (SF-36). Furthermore, improved fatigue scores were associated with reduced depression and improvements in the physical and mental components of SF-36. Overall, 95.4% of patients in the TG rated themselves as clinically improved versus 62% of the patients in the CG (p = 0.049). There was no flare in disease activity and no serious adverse events with exercise.
Conclusions
This supervised walking program was demonstrated to be feasible and safe with improvements in cardiorespiratory fitness, exercise tolerance, fatigue, and patient perception of improvement in pSS patients.
Trial registration
Clinical Trials.gov ID, number NCT02370225.


Similar content being viewed by others
References
Perandini LA, de Sá-Pinto AL, Roschel H et al (2012) Exercise as a therapeutic tool to counteract inflammation and clinical symptoms in autoimmune rheumatic diseases. Autoimmun Rev 12:218–224. https://doi.org/10.1016/j.autrev.2012.06.007
Colbert LH, Visser M, Simonsick EM et al (2004) Physical activity, exercise, and inflammatory markers in older adults: findings from the health, aging and body composition study. J Am Geriatr Soc 52:1098–1104. https://doi.org/10.1111/j.1532-5415.2004.52307.x
Mathur N, Pedersen BK (2008) Exercise as a mean to control low-grade systemic inflammation. Mediat Inflamm 2008:109502. https://doi.org/10.1155/2008/109502
Petersen AMW, Pedersen BK (2005) The anti-inflammatory effect of exercise. J Appl Physiol 98:1154–1162. https://doi.org/10.1152/japplphysiol.00164.2004
Roger-van Dartel SAA, Repping-Wuts H, Flendrie M et al (2015) The effect of aerobic exercise training on fatigue in rheumatoid arthritis: a meta-analysis. Arthritis Care Res (Hoboken) 67:1054–1062. https://doi.org/10.1002/acr
Tench CM, McCarthy J, McCurdie I et al (2003) Fatigue in systemic lupus erythematosus: a randomized controlled trial of exercise. Rheumatology 42:1050–1054. https://doi.org/10.1093/rheumatology/keg289
Carvalho MRP, De Sato EI, Tebexreni AS et al (2005) Effects of supervised cardiovascular training program on exercise tolerance, aerobic capacity, and quality of life in patients with systemic lupus erythematosus. Arthritis Rheum 53:838–844. https://doi.org/10.1002/art.21605
Robb-Nicholson LC, Daltroy L, Eaton H et al (1989) Effects of aerobic conditioning in lupus fatigue: a pilot study. Br J Rheumatol 28:500–505
Daltroy LH, Robb-Nicholson C, Iversen MD et al (1995) Effectiveness of minimally supervised home aerobic training in patients with systemic rheumatic disease. Br J Rheumatol 34:1064–1069. https://doi.org/10.1093/rheumatology/34.11.1064
Ramsey-Goldman R, Schilling EM, Dunlop D et al (2000) A pilot study on the effects of exercise in patients with systemic lupus erythematosus. Arthritis Care Res 13:262–269
Verhoeven F, Guillot X, Prati C et al (2018) Aerobic exercise for axial spondyloarthritis—its effects on disease activity and function as compared to standard physiotherapy: a systematic review and meta—analysis. Int J Rheum Dis 1:1–8. https://doi.org/10.1111/1756-185X.13385
Oliveira NC, Santos Sabbag LM dos, Sá Pinto AL de et al (2009) Aerobic exercise is safe and effective in systemic sclerosis. Int J Sports Med 30:728–732. https://doi.org/10.1055/s-0029-1224180
Pinto ALS, Oliveira NC, Gualano B et al (2011) Efficacy and safety of concurrent training in systemic sclerosis. J strength Cond Res 25:1423–1428. https://doi.org/10.1519/JSC.0b013e3181d6858b
Strömbeck BE, Theander E, Jacobsson LTH (2007) Effects of exercise on aerobic capacity and fatigue in women with primary Sjogren’s syndrome. Rheumatology 46:868–871. https://doi.org/10.1093/rheumatology/kem004
Bowman SJ, Rao V (2014) Sjögren’s syndrome. Med (Baltim) 42:162–166. https://doi.org/10.1016/j.mpmed.2013.12.002
Seror R, Ravaud P, Bowman SJ et al (2010) EULAR Sjögren’s syndrome disease activity index: development of a consensus systemic disease activity index for primary Sjögren’s syndrome. Ann Rheum Dis 69:1103–1109. https://doi.org/10.1136/ard.2009.110619
Lendrem D, Mitchell S, McMeekin P et al (2014) Health-related utility values of patients with primary Sjögren’s syndrome and its predictors. Ann Rheum Dis 73:1362–1368. https://doi.org/10.1136/annrheumdis-2012-202863
Meijer JM, Meiners PM, Huddleston Slater JJR et al (2009) Health-related quality of life, employment and disability in patients with Sjögren’s syndrome. Rheumatology 48:1077–1082. https://doi.org/10.1093/rheumatology/kep141
Cui Y, Li L, Yin R et al (2018) Depression in primary Sjögren’s syndrome: a systematic review and meta-analysis. Psychol Health Med 23:198–209. https://doi.org/10.1080/13548506.2017.1339895
Hackett KL, Gotts ZM, Ellis J et al (2017) An investigation into the prevalence of sleep disturbances in primary Sjögren’s syndrome: a systematic review of the literature. Rheumatology 56:570–580. https://doi.org/10.1093/rheumatology/kew443
Dassouki T, Benatti FB, Pinto AJ et al (2017) Objectively measured physical activity and its influence on physical capacity and clinical parameters in patients with primary Sjögren’s syndrome. Lupus 26:690–697
Ng W-F, Miller A, Bowman JS et al (2017) Physical activity but not sedentary activity is reduced in primary Sjögren’s syndrome. Rheumatol Int 37:623–631. https://doi.org/10.1007/s00296-016-3637-6
Strömbeck B, Ekdahl C, Manthorpe R, Jacobsson LTH (2003) Physical capacity in women with primary Sjögren’s syndrome: a controlled study. Arthritis Rheum 49:681–688. https://doi.org/10.1002/art.11384
Miyamoto S, Altoé R, Carletti L et al (2015) Oxygen uptake, fatigue and quality of life in primary Sjögren’s syndrome (Abstract). Scand J Rheumatol 81:366–367
Wouters EJM, van Leeuwen N, Bossema ER et al (2012) Physical activity and physical activity cognitions are potential factors maintaining fatigue in patients with primary Sjogren’s syndrome. Ann Rheum Dis 71:668–673. https://doi.org/10.1136/ard.2011.154245
Ng W-F, Bowman SJ (2010) Primary Sjogren’s syndrome: too dry and too tired. Rheumatology 49:844–853. https://doi.org/10.1093/rheumatology/keq009
Vitali C, Bombardieri S, Jonsson R et al (2002) Classification criteria for Sjögren’s syndrome: a revised version of the European criteria proposed by the American–European consensus group. Ann Rheum Dis 61:554–558
Associação Brasileira de Empresas de Pesquisa (ABEP) (2008) Critério de classificação econômica Brasil. Available at: http://www.abep.org/criterio-brasil
Valim V, Oliveira LM, Suda AL et al (2002) Peak oxygen uptake and ventilatory anaerobic threshold in fibromyalgia. J Rheumatol 29:353–357
Keyser RE, Rus V, Mikdashi JA, Handwerger BS (2010) Exploratory study on oxygen consumption on-kinetics during treadmill walking in women with systemic lupus erythematosus. Arch Phys Med Rehabil 91:1402–1409. https://doi.org/10.1016/j.apmr.2010.06.003
Keyser RE, Rus V, Cade WT et al (2003) Evidence for aerobic insufficiency in women with systemic lupus erythematosus. Arthritis Rheum 49:16–22. https://doi.org/10.1002/art.10926
Lemos MCD, Valim V, Zandonade E, Natour J (2010) Intensity level for exercise training in fibromyalgia by using mathematical models. BMC Musculoskelet Disord 11:54. https://doi.org/10.1186/1471-2474-11-54
Gaudreault N, Boulay P (2018) Cardiorespiratory fitness among adults with fibromyalgia. Breathe (Shef Engl) 14:e25–e33. https://doi.org/10.1183/20734735.019717
Fairshter RD, Walters J, Salness K et al (1983) A comparison of incremental exercise tests during cycle and treadmill ergometry. Med Sci Sports Exerc 15:549–554
Glass SGB (2007) ACSM’s Metabolic Calculations Handbook. Lippincott Williams & Wilkins, Baltimore
Hall C, Figueroa A, Fernhall B, Kanaley JA (2004) Energy expenditure of walking and running: comparison with prediction equations. Med Sci Sports Exerc 36:2128–2134
Serrano ÉV, Valim V, Miyamoto S et al (2013) Transcultural adaptation of the “EULAR sjögren’s syndrome disease activity index (ESSDAI)” into Brazilian Portuguese. Rev Bras Reumatol. https://doi.org/10.1016/j.rbr.2013.04.003
Webster K, Odom L, Peterman A et al (1999) The functional assessment of chronic illness therapy (FACIT) measurement system: validation of version 4 of the core questionnaire. Qual Life Res 8:604
Seror R, Ravaud P, Mariette X et al (2011) EULAR Sjogren’s syndrome patient reported index (ESSPRI): development of a consensus patient index for primary Sjogren’s syndrome. Ann Rheum Dis 70:968–972. https://doi.org/10.1136/ard.2010.143743
Paganotti MA, Valim V, Serrano EV et al (2015) Validation and psychometric properties of the EULAR Sjögren’s syndrome patient reported index (ESSPRI) into Brazilian Portuguese. Rev Bras Reumatol. https://doi.org/10.1016/j.rbre.2015.08.001
Gorenstein C, Andrade L (1996) Validation of a Portuguese version of the beck depression inventory and the state-trait anxiety inventory in Brazilian subjects. Brazilian J Med Biol Res 29:453–457
Ciconelli R, Ferraz M, Santos W et al (1999) Brazilian–Portuguese version of the SF-36 questionnaire: a reliable and valid quality of life outcome measure. Rev Bras Reumatol 39:143–150
Jacobsson LTH, Stro B (2007) The role of exercise in the rehabilitation of patients with systemic lupus erythematosus and patients with primary Sjögren’s syndrome. Curr Opin Rheumatol 19:197–203
Valim V, Oliveira L, Suda A et al (2003) Aerobic fitness effects in fibromyalgia. J Rheumatol 30:1060–1069
Assis MR, Silva LE, Alves AMB et al (2006) A randomized controlled trial of deep water running: clinical effectiveness of aquatic exercise to treat fibromyalgia. Arthritis Rheum 55:57–65. https://doi.org/10.1002/art.21693
Franklin BA, Whaley MH, Howley ET et al (2000) ACMS’s guidelines for exercise testing and prescription, 6th edn. Lippincott Williams & Wilkins, Philadelphia
Seror R, Theander E, Brun JG et al (2015) Validation of EULAR primary Sjogren’s syndrome disease activity (ESSDAI) and patient indexes (ESSPRI). Ann Rheum Dis 74:859–866. https://doi.org/10.1136/annrheumdis-2013-204615
Dey S, Singh RH, Dey PK (1992) Exercise training: Significance of regional alterations in serotonin metabolism of rat brain in relation to antidepressant effect of exercise. Physiol Behav 52:1095–1099. https://doi.org/10.1016/0031-9384(92)90465-E
Kasapis C, Thompson PD (2005) The effects of physical activity on serum C-reactive protein and inflammatory markers: a systematic review. J Am Coll Cardiol 45:1563–1569. https://doi.org/10.1016/J.JACC.2004.12.077
Hackett KL, Newton JL, Frith J et al (2012) Impaired functional status in primary Sjögren’s syndrome. Arthritis Care Res (Hoboken) 64:1760–1764. https://doi.org/10.1002/acr.21738
Funding
This work was supported by grants to Samira Tatiyama Miyamoto from the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior-CAPES Foundation [BEX 8831/14-9].
Author information
Authors and Affiliations
Contributions
Study conception and design: STM, VV, JN, LC, and AJP. Acquisition of data: RAG, LHS, EVS, VCA, and AMS. Data analysis and interpretation: STM, JN, VV, LC, AJP, DL, and WN. Writing: STM, JN, DL, and WN.
All authors have read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all the participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Miyamoto, S.T., Valim, V., Carletti, L. et al. Supervised walking improves cardiorespiratory fitness, exercise tolerance, and fatigue in women with primary Sjögren’s syndrome: a randomized-controlled trial. Rheumatol Int 39, 227–238 (2019). https://doi.org/10.1007/s00296-018-4213-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-018-4213-z