Abstract
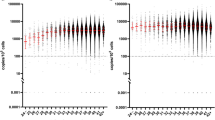
To study safety, efficacy (hemoglobin and hemoglobin F percentage increment in non-transfusion-dependent patients and decrease in transfusion frequency in transfusion-dependent patients), and determinants of response of decitabine in patients with HbE/β-thalassemia. Thirty patients of HbE/β-thalassemia (age > 18 years) were enrolled. Both transfusion-dependent (TDT) and non-transfusion-dependent (NTDT) patients were included after obtaining informed consent. Participants received 0.2 mg/kg of 5-aza-2′-deoxycytidine (decitabine) subcutaneously on 2 consecutive days a week for at least 12 weeks. Complete hemogram was done every 2 weeks and HPLC at every 4-week interval, until 2 months after last dose of drug for response assessment. Various factors like XMN1 polymorphism, IVS 1-5, alpha deletion, alpha triplication, baseline hemoglobin F, and baseline total hemoglobin were evaluated as determinants of response. Mean therapy period was 20.32 weeks. For NTDT group, peak mean increment in hemoglobin was 0.938 g/dl (p value < .001) and hemoglobin F percentage was 9.62% (p value < .001). Transfusion requirement decreased to 0.25 units compared to 0.96 units per patient per month for TDT patients over a period of last 1 year. Common side effects were respiratory tract infection (grade I/II) in three patients, chest tightness in one patient (grade I), and gastric erosion (grade III) in one patient. Decitabine is safe and efficacious in HbE/β-thalassemia.
Similar content being viewed by others
Abbreviations
- NTDT:
-
Non-transfusion-dependent thalassemia
- TDT:
-
Transfusion-dependent thalassemia
References
Premawardhena A, Fisher CA, Olivieri NF, de Silva S, Arambepola M, Perera W, O’Donnell A, Peto TEA, Viprakasit V, Merson L, Muraca G, Weatherall DJ (2005) Haemoglobin E beta thalassaemia in Sri Lanka. Lancet 366:1467–1470
Taher A, Vichinsky E, Musallam K, Cappellini MD, Viprakasit V (2013) Guidelines for the management of non-transfusion dependent thalassaemia (NTDT). Thalassaemia International Federation, Nicosia
Santos EM, Paula JF, Motta PM, Heinemann MB, Leite RC, Haddad JP, Del Puerto HL, Reis JK (2009) Comparison of three methods of DNA extraction from peripheral blood mononuclear cells and lung fragments of equines. Genet Mol Res 9:1591–1598
Bravo M, Salazar R, Arends A, Alvarez M, Velazquez D, Guevara JM, Castillo O (1999) Detection of beta thalassemia by the technique of refractory amplification of mutation systems (ARMS-PCR). Investig Clin 40(3):203–213
Bhagat S, Patra PK, Thakur AS (2012) Association between XmnI polymorphism and HbF level in sickle cell disease patients from Chhattisgarh. Int J Biomed Sci 1:36–39
Liu YT, Old JM, Miles K, Fisher CA, Weatherall DJ, Clegg JB (2000) Rapid detection of a-thalassaemia deletions and a-globin gene triplication by multiplex polymerase chain reactions. Br J Haematol 108(2):295–299
Musallam KM, Taher AT, Cappellini MD, Sankaran VG (2013) Clinical experience with fetal hemoglobin induction therapy in patients with beta-thalassemia. Blood 121(12):2199–2212
Bradai M, Pissard S, Abad MT, Dechartres A, Ribeil JA, Landais P, de Montalembert M (2007) Decreased transfusion needs associated with hydroxyurea therapy in Algerian patients with thalassemia major or intermedia. Transfusion 47(10):1830–1836
Rigano P, Pecoraro A, Calzolari R, Troia A, Acuto S, Renda D, Pantalone GR, Maggio A, Di Marzo R (2010) Desensitization to hydroxycarbamide following long-term treatment of thalassaemia intermedia as observed in vivo and in primary erythroid cultures from treated patients. Br J Haematol 151(5):509–515
Mancuso A, Maggio A, Renda D, Di Marzo R, Rigano P (2006) Treatment with hydroxycarbamide for intermedia thalassaemia: decrease of efficacy in some patients during long-term follow up. Br J Haematol 133(1):105–106
Olivieri NF, Saunthararajah Y, Thayalasuthan V et al (2011) Thalassemia Clinical Research Network. A pilot study of subcutaneous decitabine in β-thalassemia intermedia. Blood 118(10):2708–2711
Wang W, Ma ES, ,Chan AY, Prior J, Erber WN, Chan LC, Chui DH, Chong SS. Single-tube multiplex-PCR screen for anti-3.7 and anti-4.2 α-globin gene triplications. Clin Chem 49(10):1679–82
Acknowledgements
State Thalassemia Unit, IHTM, Kolkata
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Clearance: Yes, from institutional ethical committee.
Consent Taken: Yes, from all the participants in the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kalantri, S.A., Ray, R., Chattopadhyay, A. et al. Efficacy of decitabine as hemoglobin F inducer in HbE/β-thalassemia. Ann Hematol 97, 1689–1694 (2018). https://doi.org/10.1007/s00277-018-3357-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-018-3357-y