Abstract
Purpose of the study
To describe the observable MRI changes in the urogenital sinus during the second stage of labor and delivery by comparing the changes in the positions of the anatomical structures of the maternal perineum using MRI-based vector 3-D models.
Materials and methods
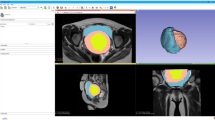
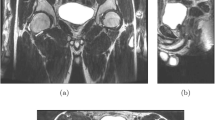
Seven pregnant women underwent 3-D MRI sequences using a Philips 1 T Panorama open MRI during the pre-labor period and during the second stage of labor. A 3-D vector reconstruction platform (BABYPROGRESS, France) enabled the transformation of volumes of 2-D images into finite element meshes. The polygonal meshes labeled with the principal components of the urogenital sinus were used as part of a biomechanical study of the pressure exerted on the perineum during fetal descent.
Results
The expansion of the urogenital sinus was observed in all patients. Qualitative stretching was observed toward the rear and bottom of the iliococcygeus, pubococcygeus, puborectalis and obturator internus muscles. Significant length differences were measured along the iliococcygeus and pubococcygeus muscles but not along the tendinous arch of the levator ani or the puborectalis muscle. The inversion of the levator ani muscle curvature was accompanied by the transmission of pressure generated during fetal descent to the pubic muscle insertions and the descent of the tendinous arch of the levator ani.
Conclusion
Mechanical pressures responsible for the tensioning of the constituent muscles of the urogenital sinus were qualitatively identified during the second stage of labor. MRI-based vector 3-D models allow the quantitative assessment of levator ani muscle stretching during labor, but 2-D MRI is not sufficient for describing perineal expansion. Vector 3-D models from larger scale studies have the potential to aid in the calibration of a realistic simulation based on the consideration of the reaction of each muscular element. These models offer perspectives to enhance our knowledge regarding perineal expansion during childbirth as a risk factor for postpartum perineal defects.




Similar content being viewed by others
Abbreviations
- MRI:
-
Magnetic resonance imaging
- UGS:
-
Urogenital sinus
- TALA:
-
Tendinous arch of levator ani
- ICM:
-
Iliococcygeus muscle
- PCM:
-
Pubococcygeus muscle
- PRM:
-
Puborectalis muscle
- IRB:
-
Institutional review board
- ANSM:
-
French National Agency for Drug and Medical Product Safety
References
Ami O, Chabrot P, Jardon K, Rocas D, Delmas V, Boyer L, Mage G (2011) Detection of cephalopelvic disproportion using a virtual reality model: a feasibility study of three cases. J Radiol 92:40–45. doi:10.1016/j.jradio.2009.05.001
Ami O, Chabrot P, Rabischong B, Rocas D, Delmas V, Boyer L, Mage G (2010) Tridimensional vector animation from fetal MRI as a simulation of delivery. J Radiol 91:515–517
Arenholt LTS, Pedersen BG, Glavind K, Glavind-Kristensen M, DeLancey JOL (2016) Paravaginal defect: anatomy, clinical findings, and imaging. Int Urogynecol J. doi:10.1007/s00192-016-3096-3
Bamberg C, Deprest J, Sindhwani N, Teichgräberg U, Güttler F, Dudenhausen JW, Kalache KD, Henrich W (2016) Evaluating fetal head dimension changes during labor using open magnetic resonance imaging. J Perinat Med. doi:10.1515/jpm-2016-0005
Bamberg C, Rademacher G, Güttler F, Teichgräber U, Cremer M, Bührer C, Spies C, Hinkson L, Henrich W, Kalache KD, Dudenhausen JW (2012) Human birth observed in real-time open magnetic resonance imaging. Am J Obstet Gynecol 206:505.e1–505.e6. doi: 10.1016/j.ajog.2012.01.011
Buttin R, Zara F, Shariat B, Redarce T, Grangé G (2013) Biomechanical simulation of the fetal descent without imposed theoretical trajectory. Comput Methods Programs Biomed 111:389–401. doi:10.1016/j.cmpb.2013.04.005
Cosson M, Rubod C, Vallet A, Witz J-F, Brieu M (2011) Biomechanical modeling of pelvic organ mobility: towards personalized medicine. Bull Acad Natl Méd 195:1869–1883 (discussion 1883)
Delmas V, Ami O, Iba-Zizen M-T (2010) Dynamic study of the female levator ani muscle using MRI 3D vectorial modeling. Bull Acad Natl Méd 194:969–980 (discussion 981–982)
Dietz HP, Lanzarone V (2005) Measuring engagement of the fetal head: validity and reproducibility of a new ultrasound technique. Ultrasound Obstet Gynecol Off J Int Soc Ultrasound Obstet Gynecol 25:165–168. doi:10.1002/uog.1765
Dietz HP, Shek KL (2009) Levator defects can be detected by 2D translabial ultrasound. Int Urogynecol J Pelvic Floor Dysfunct 20:807–811. doi:10.1007/s00192-009-0839-4
Eisenberg VH, Chantarasorn V, Shek KL, Dietz HP (2010) Does levator ani injury affect cystocele type? Ultrasound Obstet Gynecol Off J Int Soc Ultrasound Obstet Gynecol 36:618–623. doi:10.1002/uog.7712
Güttler FV, Heinrich A, Rump J, de Bucourt M, Schnackenburg B, Bamberg C, Hamm B, Teichgräber UK (2012) Magnetic resonance imaging of the active second stage of labour: proof of principle. Eur Radiol 22:2020–2026. doi:10.1007/s00330-012-2455-9
Howard D, Makhlouf M (2016) Can pelvic floor dysfunction after vaginal birth be prevented? Int Urogynecol J. doi:10.1007/s00192-016-3117-2
Hoyte L, Brubaker L, Fielding JR, Lockhart ME, Heilbrun ME, Salomon CG, Ye W, Brown MB, Pelvic Floor Disorders Network (2009) Measurements from image-based three dimensional pelvic floor reconstruction: a study of inter- and intraobserver reliability. J Magn Reson Imaging JMRI 30:344–350. doi:10.1002/jmri.21847
Hoyte L, Damaser MS (2007) Magnetic resonance-based female pelvic anatomy as relevant for maternal childbirth injury simulations. Ann N Y Acad Sci 1101:361–376. doi:10.1196/annals.1389.018
Hoyte L, Ye W, Brubaker L, Fielding JR, Lockhart ME, Heilbrun ME, Brown MB, Warfield SK, Pelvic Floor Disorders Network (2011) Segmentations of MRI images of the female pelvic floor: a study of inter- and intra-reader reliability. J Magn Reson Imaging JMRI 33:684–691. doi:10.1002/jmri.22478
Lamblin G, Mayeur O, Giraudet G, Jean Dit Gautier E, Chene G, Brieu M, Rubod C, Cosson M (2016) Pathophysiological aspects of cystocele with a 3D finite elements model. Arch Gynecol Obstet. doi:10.1007/s00404-016-4150-6
Lapeer R, Audinis V, Gerikhanov Z, Dupuis O (2014) A computer-based simulation of obstetric forceps placement. Med Image Comput Comput-Assist Interv MICCAI Int Conf Med Image Comput Comput-Assist Interv 17:57–64
Lee S-L, Tan E, Khullar V, Gedroyc W, Darzi A, Yang G-Z (2009) Physical-based statistical shape modeling of the levator ani. IEEE Trans Med Imaging 28:926–936. doi:10.1109/TMI.2009.2012894
Lepage J, Cosson M, Mayeur O, Brieu M, Rubod C (2016) The role of childbirth research simulators in clinical practice. Int J Gynaecol Obstet Off Organ Int Fed Gynaecol Obstet 132:234–235. doi:10.1016/j.ijgo.2015.07.017
Lepage J, Jayyosi C, Lecomte-Grosbras P, Brieu M, Duriez C, Cosson M, Rubod C (2015) Biomechanical pregnant pelvic system model and numerical simulation of childbirth: impact of delivery on the uterosacral ligaments, preliminary results. Int Urogynecol J 26:497–504. doi:10.1007/s00192-014-2498-3
da Leroy L, Lúcio A, de Lopes MHBM (2016) Risk factors for postpartum urinary incontinence. Rev Esc Enferm UP 50:200–207. doi:10.1590/S0080-623420160000200004
Lien K-C, Morgan DM, Delancey JOL, Ashton-Miller JA (2005) Pudendal nerve stretch during vaginal birth: a 3D computer simulation. Am J Obstet Gynecol 192:1669–1676. doi:10.1016/j.ajog.2005.01.032
Li X, Kruger JA, Nash MP, Nielsen PMF (2010) Effects of nonlinear muscle elasticity on pelvic floor mechanics during vaginal childbirth. J Biomech Eng 132:111010. doi:10.1115/1.4002558
Miller JM, Low LK, Zielinski R, Smith AR, DeLancey JOL, Brandon C (2015) Evaluating maternal recovery from labor and delivery: bone and levator ani injuries. Am J Obstet Gynecol 213:188.e1–188.e11. doi:10.1016/j.ajog.2015.05.001
Oliveira DA, Parente MPL, Calvo B, Mascarenhas T, Natal Jorge RM (2016) Numerical simulation of the damage evolution in the pelvic floor muscles during childbirth. J Biomech 49:594–601. doi:10.1016/j.jbiomech.2016.01.014
Shi M, Shang S, Xie B, Wang J, Hu B, Sun X, Wu J, Hong N (2016) MRI changes of pelvic floor and pubic bone observed in primiparous women after childbirth by normal vaginal delivery. Arch Gynecol Obstet 294:285–289. doi:10.1007/s00404-016-4023-z
Silva MET, Oliveira DA, Roza TH, Brandão S, Parente MPL, Mascarenhas T, Natal Jorge RM (2015) Study on the influence of the fetus head molding on the biomechanical behavior of the pelvic floor muscles, during vaginal delivery. J Biomech 48:1600–1605. doi:10.1016/j.jbiomech.2015.02.032
Tracy PV, DeLancey JO, Ashton-Miller JA (2016) A geometric capacity-demand analysis of maternal levator muscle stretch required for vaginal delivery. J Biomech Eng 138:021001. doi:10.1115/1.4032424
Unger CA, Weinstein MM, Pretorius DH (2011) Pelvic floor imaging. Obstet Gynecol Clin North Am 38:23–43. doi:10.1016/j.ogc.2011.02.002
van Veelen A, Schweitzer K, van der Vaart H (2014) Ultrasound assessment of urethral support in women with stress urinary incontinence during and after first pregnancy. Obstet Gynecol 124:249–256. doi:10.1097/AOG.0000000000000355
Vergeldt TFM, Notten KJB, Stoker J, Fütterer JJ, Beets-Tan RG, Vliegen RFA, Schweitzer KJ, Mulder FEM, van Kuijk SMJ, Roovers JPWR, Kluivers KB, Weemhoff M (2016) Comparison of translabial three-dimensional ultrasound with magnetic resonance imaging for measurement of levator hiatal biometry at rest. Ultrasound Obstet Gynecol Off J Int Soc Ultrasound Obstet Gynecol 47:636–641. doi:10.1002/uog.14949
Wijma J, Weis Potters AE, van der Mark TW, Tinga DJ, Aarnoudse JG (2007) Displacement and recovery of the vesical neck position during pregnancy and after childbirth. Neurourol Urodyn 26:372–376. doi:10.1002/nau.20354
Zacharin RF (1968) The anatomic supports of the female urethra. Obstet Gynecol 32:754–759
Zacharin RF (1977) Abdominoperineal urethral suspension: a 10-year experience in the management of recurrent stress incontinence of urine. Obstet Gynecol 50:1–8
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Maran, JC., Cassagnes, L., Delmas, V. et al. Comparative anatomy on 3-D MRI of the urogenital sinus and the periurethral area before and during the second stage of labor during childbirth. Surg Radiol Anat 40, 371–380 (2018). https://doi.org/10.1007/s00276-017-1925-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-017-1925-9