Abstract
Purpose
To evaluate the effect of air, CO2 and contrast medium-air on the dwell time (DT) stability of sodium tetradecyl sulfate (STS) foam.
Materials and Methods
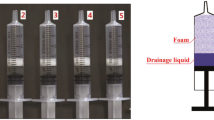
Three types of foam sclerosants (air-foam, CO2-foam, contrast-air-foam) were injected eight times into an inclined straight plastic tube (internal diameters 4 mm and 10 mm) filled with a blood substitute. Injections were captured by CCD camera, and images were transferred for digital analysis and calculation of DT.
Results
Contrast-air-foam and air-foam in a 4-mm tube showed 5.6-/3.3-fold greater DT compared to CO2-foam, respectively (P = 0.001). Contrast-air-foam in a 10-mm tube showed 2.1-fold greater DT compared to CO2-foam (P = 0.0167).
Conclusion
A mixture of air and iodinated contrast improves the stability of STS foam compared to mixtures using only air or CO2. Further, animal and clinical studies are needed to validate this in vitro result.






Similar content being viewed by others
References
Tessari L, Cavezzi A, Frullini A. Preliminary experience with a new sclerosing foam in the treatment of varicose veins. Dermatol Surg. 2001;27:58–60. https://doi.org/10.1111/j.1524-4725.2001.00192.x.
Mimura H, Fujiwara H, Hiraki T, et al. Polidocanol sclerotherapy for painful venous malformations: evaluation of safety and efficacy in pain relief. Eur Radiol. 2009;19:2474–80. https://doi.org/10.1007/s00330-009-1442-2.
Li L, Zeng X-Q, Li Y-H. Digital subtraction angiography-guided foam sclerotherapy of peripheral venous malformations. AJR Am J Roentgenol. 2010;194:W439–44. https://doi.org/10.2214/AJR.09.3416.
Li K, Liu Y-R, Chen A-W, Liu S-H. A new method for using radiopaque sclerosing foam to treat venous malformations. Dermatol Surg. 2015;41:726–30. https://doi.org/10.1097/DSS.0000000000000363.
Carugo D, Ankrett DN, O’Byrne V, et al. A novel biomimetic analysis system for quantitative characterisation of sclerosing foams used for the treatment of varicose veins. J Mater Sci Mater Med. 2013;24:1417–23. https://doi.org/10.1007/s10856-013-4913-6.
Carugo D, Ankrett DN, O’Byrne V, et al. The role of clinically-relevant parameters on the cohesiveness of sclerosing foams in a biomimetic vein model. J Mater Sci Mater Med. 2015;26:1–10. https://doi.org/10.1007/s10856-015-5587-z.
Pries AR, Neuhaus D, Gaehtgens P. Blood viscosity in tube flow: dependence on diameter and hematocrit. Am J Physiol. 1992;263:H1770–8.
Johnson LR. Essential medical physiology, 3rd edn. p 293; 2003.
Erkin A, Kosemehmetoglu K, Diler MS, Koksal C. Evaluation of the minimum effective concentration of foam sclerosant in an ex vivo study. Eur J Vasc Endovasc Surg. 2012;44:593–7. https://doi.org/10.1016/j.ejvs.2012.09.021.
Cavezzi A, Tessari L. Foam sclerotherapy techniques: different gases and methods of preparation, catheter versus direct injection. Phlebology. 2009;24:247–51. https://doi.org/10.1258/phleb.2009.009061.
Morrison N, Neuhardt DL, Rogers CR, et al. Comparisons of side effects using air and carbon dioxide foam for endovenous chemical ablation. J Vasc Surg. 2008;47:830–6. https://doi.org/10.1016/j.jvs.2007.11.020.
Cavezzi A, Tessari L. Foam sclerotherapy techniques: different gases and methods of preparation, catheter versus direct injection. Phlebology. 2009;24:247–51. https://doi.org/10.1258/phleb.2009.009061.
McMaster S. Sodium tetradecyl sulphate foam stability prior to injection: factors affecting liquid reformation. Phlebology. 2011;26:222–6. https://doi.org/10.1258/phleb.2010.010025.
Valenzuela GC, Wong K, Connor DE, et al. Foam sclerosants are more stable at lower temperatures. Eur J Vasc Endovasc Surg. 2013;46:593–9. https://doi.org/10.1016/j.ejvs.2013.08.012.
Parsi K, Exner T, Connor DE, et al. The lytic effects of detergent sclerosants on erythrocytes, platelets, endothelial cells and microparticles are attenuated by albumin and other plasma components in vitro. Eur J Vasc Endovasc Surg. 2008;36:216–23. https://doi.org/10.1016/j.ejvs.2008.03.001.
Watkins MRR. Deactivation of sodium tetradecyl sulphate injection by blood proteins. Eur J Vasc Endovasc Surg. 2011;41:521–5. https://doi.org/10.1016/j.ejvs.2010.12.012.
Hamel-Desnos C, Desnos P, Wollmann JC, et al. Evaluation of the efficacy of polidocanol in the form of foam compared with liquid form in sclerotherapy of the greater saphenous vein: initial results. Dermatol Surg. 2003;29:1170–5. https://doi.org/10.1111/j.1524-4725.2003.29398.x.
Wollmann JC. Sclerosant foams: stabilities, physical properties and rheological behavior. Phlebologie. 2010;39:208–17.
Acknowledgements
The authors thank Younes Jahangiri, M.D., for assistance in taking photographs and maintaining the data for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors. IRB approval was waved based upon the nature of the study.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hashimoto, K., Uchida, B., Horikawa, M. et al. Effects of Different Mixing Agents on the Stability of Sodium Tetradecyl Sulfate (STS) Foam: An Experimental Study. Cardiovasc Intervent Radiol 41, 1952–1957 (2018). https://doi.org/10.1007/s00270-018-2049-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-018-2049-2