Abstract
Objectives
Postoperative pancreatic fistula (POPF) is a major complication and main cause of mortality after pancreaticoduodenectomy (PD). Afferent loop decompression technique (ALDT) has theoretical feasibility to reduce the rate of POPF. The aim of this study is to determine whether ALDT is a protective factor for POPF.
Methods
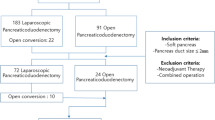
A total of 492 consecutive patients who underwent PD between January 2012 and December 2014 were identified from a prospective database. All data were extracted and events were judged based on medical records. Propensity score matching was conducted to balance several variables. Univariate and multivariate analyses were performed, respectively, to investigate the independent risk factors for pancreatic fistula. ALDT required a nasogastric tube with multiple side holes to be placed deep into the afferent jejunal limb. The rationale for this technique was to prevent pancreatic fistula by decreasing intraluminal pressure in the afferent jejunal loop by placement of the nasogastric tube and the application of continuous low-pressure suction after surgery.
Results
The total rate of POPF for the entire cohort was 30.7%, and ISGPS grade-A/B/C POPF rates were 18.1, 10.6 and 2.0%, respectively. In-hospital mortality was 1.6%. Among the 331 patients who received ALDT, 89 developed pancreatic leakage (26.9 vs. 38.5% for non-ALDT; P = 0.009) and eight developed biliary leakage (2.4 vs. 6.2% for non-ALDT; P = 0.035). Apart from ALDT, decreased preoperative ALT, soft pancreas, long operative time and tumour presence in the lower common bile duct (as opposed to the pancreas) were identified as other independent risk factors for POPF following multivariate logistic regression analysis.
Conclusions
ALDT may reduce the incidence of POPF after PD.

Similar content being viewed by others
References
Whipple AO, Parsons WB, Mullins CR (1935) Treatment of carcinoma of the ampulla of vater. Ann Surg 102(4):763–779
Cameron JL, Pitt HA, Yeo CJ, Lillemoe KD, Kaufman HS, Coleman J (1993) One hundred and forty-five consecutive pancreaticoduodenectomies without mortality. Ann Surg 217(5):430–438
Yoshioka R, Yasunaga H, Hasegawa K, Horiguchi H, Fushimi K, Aoki T, Sakamoto Y, Sugawara Y, Kokudo N (2014) Impact of hospital volume on hospital mortality, length of stay and total costs after pancreaticoduodenectomy. Br J Surg 101(5):523–529
Lai EC, Lau SH, Lau WY (2009) Measures to prevent pancreatic fistula after pancreatoduodenectomy: a comprehensive review. Arch Surg 144(11):1074–1080
Gaujoux S, Cortes A, Couvelard A, Noullet S, Clavel L, Rebours V, Levy P, Sauvanet A, Ruszniewski P, Belghiti J (2010) Fatty pancreas and increased body mass index are risk factors of pancreatic fistula after pancreaticoduodenectomy. Surgery 148(1):15–23
Mathur A, Pitt HA, Marine M, Saxena R, Schmidt CM, Howard TJ, Nakeeb A, Zyromski NJ, Lillemoe KD (2007) Fatty pancreas: a factor in postoperative pancreatic fistula. Ann Surg 246(6):1058–1064
Kollmar O, Moussavian MR, Bolli M, Richter S, Schilling MK (2007) Pancreatojejunal leakage after pancreas head resection: anatomic and surgeon-related factors. J Gastrointest Surg 11(12):1699–1703
Bassi C, Falconi M, Molinari E, Mantovani W, Butturini G, Gumbs AA, Salvia R, Pederzoli P (2003) Duct-to-mucosa versus end-to-side pancreaticojejunostomy reconstruction after pancreaticoduodenectomy: results of a prospective randomized trial. Surgery 134(5):766–771
Winter JM, Cameron JL, Campbell KA, Chang DC, Riall TS, Schulick RD, Choti MA, Coleman J, Hodgin MB, Sauter PK, Sonnenday CJ, Wolfgang CL, Marohn MR, Yeo CJ (2006) Does pancreatic duct stenting decrease the rate of pancreatic fistula following pancreaticoduodenectomy? Results of a prospective randomized trial. J Gastrointest Surg 10(9):1280–1290
Xiong JJ, Tan CL, Szatmary P, Huang W, Ke NW, Hu WM, Nunes QM, Sutton R, Liu XB (2014) Meta-analysis of pancreaticogastrostomy versus pancreaticojejunostomy after pancreaticoduodenectomy. Br J Surg 101(10):1196–1208
Xiong JJ, Altaf K, Mukherjee R, Huang W, Hu WM, Li A, Ke NW, Liu XB (2012) Systematic review and meta-analysis of outcomes after intraoperative pancreatic duct stent placement during pancreaticoduodenectomy. Br J Surg 99(8):1050–1061
Hartwig W, Vollmer CM, Fingerhut A, Yeo CJ, Neoptolemos JP, Adham M, Andren-Sandberg A, Asbun HJ, Bassi C, Bockhorn M, Charnley R, Conlon KC, Dervenis C, Fernandez-Cruz L, Friess H, Gouma DJ, Imrie CW, Lillemoe KD, Milicevic MN, Montorsi M, Shrikhande SV, Vashist YK, Izbicki JR, Buchler MW (2014) Extended pancreatectomy in pancreatic ductal adenocarcinoma: definition and consensus of the International Study Group for Pancreatic Surgery (ISGPS). Surgery 156(1):1–14
Wei J, Liu X, Wu J, Xu W, Zhou J, Lu Z, Chen J, Guo F, Gao W, Li Q, Jiang K, Dai C, Miao Y (2015) Modified one-layer duct-to-mucosa pancreaticojejunostomy reduces pancreatic fistula after pancreaticoduodenectomy. Int Surg. https://doi.org/10.9738/INTSURG-D-15-00094.1
Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J, Neoptolemos J, Sarr M, Traverso W, Buchler M (2005) Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery 138(1):8–13
Wente MN, Veit JA, Bassi C, Dervenis C, Fingerhut A, Gouma DJ, Izbicki JR, Neoptolemos JP, Padbury RT, Sarr MG, Yeo CJ, Buchler MW (2007) Postpancreatectomy hemorrhage (PPH): an International Study Group of Pancreatic Surgery (ISGPS) definition. Surgery 142(1):20–25
Wente MN, Bassi C, Dervenis C, Fingerhut A, Gouma DJ, Izbicki JR, Neoptolemos JP, Padbury RT, Sarr MG, Traverso LW, Yeo CJ, Buchler MW (2007) Delayed gastric emptying (DGE) after pancreatic surgery: a suggested definition by the International Study Group of Pancreatic Surgery (ISGPS). Surgery 142(5):761–768
Li SQ, Liang LJ, Peng BG, Lu MD, Lai JM, Li DM (2007) Bile leakage after hepatectomy for hepatolithiasis: risk factors and management. Surgery 141(3):340–345
Besselink MG, van Rijssen LB, Bassi C, Dervenis C, Montorsi M, Adham M, Asbun HJ, Bockhorn M, Strobel O, Buchler MW, Busch OR, Charnley RM, Conlon KC, Fernandez-Cruz L, Fingerhut A, Friess H, Izbicki JR, Lillemoe KD, Neoptolemos JP, Sarr MG, Shrikhande SV, Sitarz R, Vollmer CM, Yeo CJ, Hartwig W, Wolfgang CL, Gouma DJ, International Study Group on Pancreatic Surgery (2017) Definition and classification of chyle leak after pancreatic operation: a consensus statement by the International Study Group on Pancreatic Surgery. Surgery 161(2):365–372
Winter JM, Cameron JL, Campbell KA, Arnold MA, Chang DC, Coleman J, Hodgin MB, Sauter PK, Hruban RH, Riall TS, Schulick RD, Choti MA, Lillemoe KD, Yeo CJ (2006) 1423 pancreaticoduodenectomies for pancreatic cancer: a single-institution experience. J Gastrointest Surg 10(9):1199–1211
Kimura W, Miyata H, Gotoh M, Hirai I, Kenjo A, Kitagawa Y, Shimada M, Baba H, Tomita N, Nakagoe T, Sugihara K, Mori M (2014) A pancreaticoduodenectomy risk model derived from 8575 cases from a national single-race population (Japanese) using a web-based data entry system: the 30-day and in-hospital mortality rates for pancreaticoduodenectomy. Ann Surg 259(4):773–780
El Nakeeb A, Salah T, Sultan A, El Hemaly M, Askr W, Ezzat H, Hamdy E, Atef E, El Hanafy E, El-Geidie A, Abdel Wahab M, Abdallah T (2013) Pancreatic anastomotic leakage after pancreaticoduodenectomy. Risk factors, clinical predictors, and management (single center experience). World J Surg 37(6):1405–1418. https://doi.org/10.1007/s00268-013-1998-5
El Nakeeb A, Askr W, Mahdy Y, Elgawalby A, El Sorogy M, Abu Zeied M, Abdallah T, Abd Elwahab M (2015) Delayed gastric emptying after pancreaticoduodenectomy. Risk factors, predictors of severity and outcome. A single center experience of 588 cases. J Gastrointest Surg 19(6):1093–1100
Pratt WB, Callery MP, Vollmer CM Jr (2008) Risk prediction for development of pancreatic fistula using the ISGPF classification scheme. World J Surg 32(3):419–428. https://doi.org/10.1007/s00268-007-9388-5
van der Gaag NA, Rauws EA, van Eijck CH, Bruno MJ, van der Harst E, Kubben FJ, Gerritsen JJ, Greve JW, Gerhards MF, de Hingh IH, Klinkenbijl JH, Nio CY, de Castro SM, Busch OR, van Gulik TM, Bossuyt PM, Gouma DJ (2010) Preoperative biliary drainage for cancer of the head of the pancreas. N Engl J Med 362(2):129–137
Pessaux P, Sauvanet A, Mariette C, Paye F, Muscari F, Cunha AS, Sastre B, Arnaud JP (2011) External pancreatic duct stent decreases pancreatic fistula rate after pancreaticoduodenectomy: prospective multicenter randomized trial. Ann Surg 253(5):879–885
Figueras J, Sabater L, Planellas P, Munoz-Forner E, Lopez-Ben S, Falgueras L, Sala-Palau C, Albiol M, Ortega-Serrano J, Castro-Gutierrez E (2013) Randomized clinical trial of pancreaticogastrostomy versus pancreaticojejunostomy on the rate and severity of pancreatic fistula after pancreaticoduodenectomy. Br J Surg 100(12):1597–1605
Chen Y, Ke N, Tan C, Zhang H, Wang X, Mai G, Liu X (2015) Continuous versus interrupted suture techniques of pancreaticojejunostomy after pancreaticoduodenectomy. J Surg Res 193(2):590–597
Tani M, Kawai M, Hirono S, Okada KI, Miyazawa M, Shimizu A, Kitahata Y, Yamaue H (2014) Randomized clinical trial of isolated Roux-en-Y versus conventional reconstruction after pancreaticoduodenectomy. Br J Surg 101(9):1084–1091
Hatzigeorgiadis A, Boulas KA, Barettas N, Papageorgiou I, Blouhos K (2014) Tube pancreatico- duodenostomy for management of a severe penetrating pancreaticoduodenal injury. JOP 15(3):250–253
Motoi F, Egawa S, Rikiyama T, Katayose Y, Unno M (2012) Randomized clinical trial of external stent drainage of the pancreatic duct to reduce postoperative pancreatic fistula after pancreaticojejunostomy. Br J Surg 99(4):524–531
Williamsson C, Karlsson N, Sturesson C, Lindell G, Andersson R, Tingstedt B (2015) Impact of a fast-track surgery programme for pancreaticoduodenectomy. Br J Surg 102(9):1133–1141
Kunstman JW, Klemen ND, Fonseca AL, Araya DL, Salem RR (2013) Nasogastric drainage may be unnecessary after pancreaticoduodenectomy: a comparison of routine vs selective decompression. J Am Coll Surg 217(3):481–488
Ausania F, Snowden CP, Prentis JM, Holmes LR, Jaques BC, White SA, French JJ, Manas DM, Charnley RM (2012) Effects of low cardiopulmonary reserve on pancreatic leak following pancreaticoduodenectomy. Br J Surg 99(9):1290–1294
El Nakeeb A, Sultan AM, Salah T, El Hemaly M, Hamdy E, Salem A, Moneer A, Said R, AbuEleneen A, Abu Zeid M, Abdallah T, Abdel Wahab M (2013) Impact of cirrhosis on surgical outcome after pancreaticoduodenectomy. World J Gastroenterol 19(41):7129–7137
Polanco PM, Zenati MS, Hogg ME, Shakir M, Boone BA, Bartlett DL, Zeh HJ, Zureikat AH (2016) An analysis of risk factors for pancreatic fistula after robotic pancreaticoduodenectomy: outcomes from a consecutive series of standardized pancreatic reconstructions. Surg Endosc 30(4):1523–1529
Acknowledgements
This study was funded by the National Natural Science Foundation of China (Grant No. 81272382&81672449), the Innovation Capability Development Project of Jiangsu Province (No. BM2015004 to YM), and by the Jiangsu Province Funding Programme for Six Major Talent Summit, China (Grant No.2014-WSW-006). The authors gratefully appreciate Dr. Christopher Halloran for review of the manuscript. The approval number is 2018-SR-070.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Yin, J., Lu, Z., Wu, P. et al. Afferent Loop Decompression Technique is Associated with a Reduction in Pancreatic Fistula Following Pancreaticoduodenectomy. World J Surg 42, 3726–3735 (2018). https://doi.org/10.1007/s00268-018-4679-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-018-4679-6