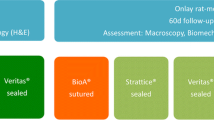
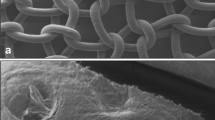
The use of a new type of prosthesis, Bard Composix (BC), constructed of two layers of polypropylene mesh (PP) and one layer of expanded polytetrafluoroethylene (ePTFE), could provide a good solution for hernia repair when both minimal adhesions and maximum collagenous infiltration are necessary. We experimentally evaluated long-term stability of this composite. In 15 Sprague-Dawley rats, a full thickness defect was created in the anterior abdominal wall and repaired with BC. Studies were performed over implantation intervals of 2, 4, and 6 months in strips obtained from the prosthesis-host tissue interfaces. Light microscopy, environmental scanning electron microscopy (ESEM), immunohistochemistry, and tensiometry were used. Overall findings provide evidence that PP and ePTFE association renders the alloy well suited for hernia repair, promoting a robust and durable alloplast-soft tissue union. At all points studied, the patch was well tolerated and meshes did not shrink, come loose, or migrate. Neovascularization continued 6 months after implantation. Ex vivo mechanical characterization demonstrated that the primary advantage of the new device stems from a low modulus of elasticity, a property that can be exploited to enhance mechanical load transfer from prosthetic materials to the relatively frail surrounding tissues. After implantation, adequate tensile strength and a low modulus of elasticity were detected in the restored zone, conferring great adaptability to the abdominal wall. In conclusion, the BC layered prosthesis proved suitable for implantation in abdominal wall defects, exhibiting favorable biocompatibility and integration with minimal side effects.
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Ferrando, J., Vidal, J., Armengol, M. et al. Experimental Evaluation of a New Layered Prosthesis Exhibiting a Low Tensile Modulus of Elasticity: Long-term Integration Response within the Rat Abdominal Wall. World J Surg 26, 409–415 (2002). https://doi.org/10.1007/s00268-001-0240-z
Issue Date:
DOI: https://doi.org/10.1007/s00268-001-0240-z