Abstract
Introduction
In last three decades, total hip replacement in young patients became an habitual procedure. Principles of bone preservation are pushing many surgeons to implant conservative femoral components in patient younger than 65 years. Despite an overall good survivorship and clinical outcomes of conservative implants, failed cases are reported and the need to revise a conservative femoral component became an occasional procedure (with high prevalence of failed resurfacing implants).
Methods
During conservative femoral component revisions, we analyzed proximal bone stock preservation, considering the type of original component removed, aetiology of failure, timing of revision, and femoral explantation technique.
Results
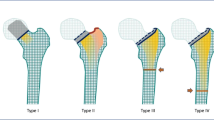
We identified four patterns of proximal femoral changes (types I–IV). We suggest, for each of them, a revision strategy directed toward a “conservative revision procedure” using conservative or primary component. Out of our 21 cases, none underwent further revision due to mechanical failure (follow-up ranging from 6 to 152 months, mean 54 months). We had two cases of re-operation: one for early septic loosening and one for prosthetic modular neck fracture.
Conclusions
If literature offers well-established guidelines to femoral revision of conventional stems, there is, on the other hand, a lack of data about revision strategies in presence of failed conservative implants. Although the mean follow-up of our procedures is still too short (4.5 years) to give final conclusions, we would leave a message: a conservative hip arthroplasty is not a “one time” opportunity for young and active people. A “conservative revision” is a valid option for at least a part of them, when an early failure of primary procedure occurred.








Similar content being viewed by others
References
Wyness L, Vale L, McCormack K, Grant A, Brazzelli M (2004) The effectiveness of metal on metal hip resurfacing: a systematic review of the available evidence published before 2002. BMC Health Serv Res 4:39
Pipino F, Keller A (2006) Tissue-sparing surgery: 25 years’ experience with femoral neck preserving hip arthroplasty. J Orthop Traumatol 7(1):36–41
Morrey BF, Adams RA, Kessler M (2000) A conservative femoral replacement for total hip arthroplasty. A prospective study. J Bone Joint Surg Br 82-B(7):952–958
Falez F, Casella F, Panegrossi G, Favetti F, Barresi C (2008) Perspectives of metaphyseal conservative stems. J Orthopaed Traumatol 9(1):49–54
Kim SM, HAN SB, Rhyu KH, Yoo JJ, Oh KJ, Yoo JH, Lee KJ, Lim SJ (2018) Periprosthetic femoral fracture as cause of early revision after short stem hip arthroplasty- a multicentric analysis. Int Orthop 42(9):2069–2076
Abdel MP, Cottino U, Mabry TM (2015) Management of periprosthetic femoral fractures following total hip arthroplasty: a review. Int Orthop 39(10):2005–2010
Amenabar T, Rahman WA, Avhad VV, Vera R, Gross AE, Kuzyk PR (2015) Vancouver type B2 and B3 periprosthetic fractures treated with revision total hip arthroplasty. Int Orthop 39(10):1927–1932
Paprosky WG, Burnett RS (2002) Assessment and classification of bone stock deficiency in revision total hip arthroplasty. Am J Orthop 31(8):459–464
Falez F, Casella F, La Cava F, Favetti F (2007) Nonunion in an unnoticed neck fracture in resurfacing total hip arthroplasty – case report. Hip International 17(13):179–182
Morlock MM, Bishop N, Ruther W, Delling G, Hahn M (2006) Biomechanical, morphological, and histological analysis of early failures in hip resurfacing arthroplasty. Proc Inst Mech Eng H 220(2):333–344
Gruen TA, McNeice GM, Amstutz HC (1979) “Modes of failure” of cemented stem-type femoral components: a radiographic analysis of loosening. Clin Orthop Relat Res 141:17–27
Amstuz HC, Campbell PA, Le Duff MJ (2004) Fracture of the neck of the femur after surface arthroplasty of the hip. J Bone Joint Surg 86A(9):1874–1877
Indelli PF, Vail TP, Dominguez D, Pickering T (2005) Resurfacing hip replacement: surgical technique and clinical results with minimum 1-year follow-up. Paper presented at 90th nation congress of Italian Orthopaedic and Traumatologic Society 9-13th of October 2005
Li D, Hu Q, Kang P, Yang J, Zhou Z, Shen B, Pei F (2018) Reconstructed the bone stock after femoral bone loss in Vancouver B3 periprosthetic femoral fractures using cortical strut allograft and impacted cancellous allograft. Int Orthop. https://doi.org/10.1007/s00264-018-3997-5
Reikeras O (2017) Femoral revision surgery using a fully hydroxyapatite-coated stem: a cohort study of twenty-two to twenty-seven years. Int Orthop 41(2):271–275
Cavagnaro L, Formica M, Basso M, Zanirato A, Divano S, Felli L (2018) Femoral revision with primary Cementless stem: a systemtic review of the literature. Muscoloskelet Surg 102(1):1–9
Canovas F, Putman S, Girard J, Roche O, Bonnomet F, Le Beguec P (2018) Global radiological score for cementless revision stem. Int Orthop 42(5):1007–1013
Rayan F, Dodd M, Haddad FS (2008) European validation of the Vancouver classification of periprosthetic proximal femoral fractures. J Bone Joint Surg Br 90B(12):1576–1579
Yu R, Hofstaetter JC, Sullivan T, Costi K, Howie DW, Solomon LB (2013) Validity and reliability of the Paprosky acetabular defect classification. Clin Orthop Relat Res 471(7):2844–2847
Affatato S, Comitini S, Fosco M, Toni A, Tigani D (2016) Radiological identification of Zweimuller-type femoral stem prosthesis in revision cases. Int Ortop 40(11):2261–2269
Author information
Authors and Affiliations
Corresponding author
Additional information
LEVEL OF EVIDENCE: III
Rights and permissions
About this article
Cite this article
Casella, F., Favetti, F., Panegrossi, G. et al. A new classification for proximal femur bone defects in conservative hip arthroplasty revisions. International Orthopaedics (SICOT) 43, 63–70 (2019). https://doi.org/10.1007/s00264-018-4233-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-4233-z