Abstract
Purpose
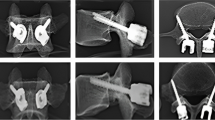
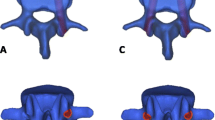
To study the exact distribution of bone cement around augmented fenestrated pedicle screws in both lumbar and sacral vertebrae of patients with low bone quality.
Methods
A total of 37 patients with instrumented lumbar fusion were investigated. 3D computed tomography virtual models of the injected cement and screws were obtained. The models were computed for their centroid (i.e. their average mass centre point), and their coordinates (x, y, z) were projected on their respective screw-transversal and screw-longitudinal planes for further analysis.
Results
The results showed better bone cement homogeneous distribution around the screws in lumbar (L4 and L5) than in sacral (S1) vertebrae. In the lumbar region, the centroids were transversally projected near the transversal centre of symmetry of the screws. On the other hand, in the sacral region, the cement flowed preferentially outside the centre of symmetry of the screws, into the sacral ala.
Conclusions
The results confirm the different flow behaviours of bone cement in lumbar versus sacra vertebrae. The computer methodology followed in this study helps to understand the clinical monitoring observations and lays the foundations for better positioning of the screws and specific vertebrae-oriented screw designs.





Similar content being viewed by others
References
Piñera AR, Duran C, Lopez B et al (2011) Instrumented lumbar arthrodesis in elderly patients: prospective study using cannulated cemented pedicle screw instrumentation. Eur Spine J 20(3):408–414. https://doi.org/10.1007/s00586-011-1907-2
Rajaee SS, Bae HW, Kanim LE, Delamarter RB (2012) Spinal fusion in the United States: analysis of trends from 1998 to 2008. Spine 37(1):67–76. https://doi.org/10.1097/BRS.0b013e31820cccfb
Li G, Patil CG, Lad SP et al (2008) Effects of age and comorbidities on complication rates and adverse outcomes after lumbar laminectomy in elderly patients. Spine 33(11):1250–1255. https://doi.org/10.1097/BRS.0b013e3181714a44
Raffo CS, Lauerman WC (2006) Predicting morbidity and mortality of lumbar spine arthrodesis in patients in their ninth decade. Spine 31(1):99–103. https://doi.org/10.1097/01.brs.0000192678.25586.e5.
Daubs MD, Lenke LG, Cheh G et al (2007) Adult spinal deformity surgery: complications and outcomes in patients over age 60. Spine 32(20):2238–2244. https://doi.org/10.1097/BRS.0b013e31814cf24a
Esses SI, Sachs BL, Dreyzin V (1993) Complications associated with the technique of pedicle screw fixation: a selected survey of ABS members. Spine 18(15):2231–2239
Polly DW, Orchowski JR, Ellenbogen RG (1998) Revision pedicle screws. Bigger, longer shims—what is best? Spine 23(12):1374–1379
von Strempel A, Kühle J, Plitz W (1994) Stability of pedicle screws. 2: maximum pullout force with reference to bone density. Z Orthop Ihre Grenzgeb 132(1):82–86
Wang W, Baran GR, Garg H et al (2014) The benefits of cement augmentation of pedicle screw fixation are increased in osteoporotic bone: a finite element analysis. Spine Deform 2(4):248–259. https://doi.org/10.1016/j.jspd.2014.03.002
Wittenberg RH, Lee KS, Shea M et al (1993) Effect of screw diameter, insertion technique, and bone cement augmentation of pedicular screw fixation strength. Clin Orthop Relat Res 296(296):278–287. https://doi.org/10.1097/00003086-199311000-00045
Pfeifer BA, Krag MH, Johnson C (1994) Repair of failed transpedicle screw fixation: a biomechanical study comparing polymethylmethacrylate, milled bone, and matchstick bone reconstruction. Spine 19(3):350–353
Tan JS, Kwon BK, Dvorak MF et al (2004) Pedicle screw motion in the osteoporotic spine after augmentation with laminar hooks, sublaminar wires, or calcium phosphate cement: a comparative analysis. Spine 29(16):1723–1730. https://doi.org/10.1097/01.BRS.0000134569.63542.49
Renner SM, Lim TH, Kim WJ et al (2004) Augmentation of pedicle screw fixation strength using an injectable calcium phosphate cement as a function of injection timing and method. Spine 29(11):E212–E216
Yi X, Wang Y, Lu H, Li C, Zhu T (2008) Augmentation of pedicle screw fixation strength using an injectable calcium sulphate cement: an in vivo study. Spine 33(23):2503–2509. https://doi.org/10.1097/BRS.0b013e318184e750
Liu D, Wu ZX, Pan XM et al (2011) Biomechanical comparison of different techniques in primary spinal surgery in osteoporotic cadaveric lumbar vertebrae: expansive pedicle screw versus polymethylmethacrylate-augmented pedicle screw. Arch Orthop Trauma Surg 131(9):1227–1232. https://doi.org/10.1007/s00402-011-1290-9.
Chang MC, Liu CL, Chen TH (2008) Polymethylmethacrylate augmentation of pedicle screw for osteoporotic spinal surgery: a novel technique. Spine 33(10):E317–E324. https://doi.org/10.1097/BRS.0b013e31816f6c73
Choma TJ, Pfeiffer FM, Swope RW, Hirner JP (2012) Pedicle screw design and cement augmentation in osteoporotic vertebrae: effects of fenestrations and cement viscosity on fixation and extraction. Spine 37(26):E1628–E1632. https://doi.org/10.1097/BRS.0b013e3182740e56
Liebschner MAK, Rosenberg WS, Keaveny TM (2001) Effects of bone cement volume and distribution on vertebral stiffness after vertebroplasty. Spine 26(14):1547–1554. https://doi.org/10.1097/00007632-200107150-00009
Elder BD, Lo SF, Holmes C et al (2015) The biomechanics of pedicle screw augmentation with cement. Spine J 15(6):1432–1445. https://doi.org/10.1016/j.spinee.2015.03.016
Blattert TR, Glasmacher S, Riesner HJ, Josten C (2009) Revision characteristics of cement-augmented, cannulated-fenestrated pedicle screws in the osteoporotic vertebral body: a biomechanical in vitro investigation. J Neurosurg Spine 11(1):23–27. https://doi.org/10.3171/2009.3.SPINE08625
Sarzier JS, Evans AJ, Cahill DW (2002) Increased pedicle screw pullout strength with vertebroplasty augmentation in osteoporotic spines. J Neurosurg 96(3):309–312
Wilkes RA, Mackinnon JG, Thomas WG (1994) Neurological deterioration after cement injection into a vertebral body. J Bone Joint Surg Br 76(1):155
Garg MK, Kharb S (2013) Dual energy X-ray absorptiometry: pitfalls in measurement and interpretation of bone mineral density. Indian J Endocrinol Metab 17(2):203–210. https://doi.org/10.4103/2230-8210.109659
Zindrick MR, Wiltse LL, Widell EH et al (1986) A biomechanical study of intrapeduncular screw fixation in the lumbosacral spine. Clin Orthop Relat Res 203:99–112
Martín-Fernández M, López-Herradón A, Piñera AR et al (2017) Potential risks of using cement-augmented screws for spinal fusion in patients with low bone quality. Spine J 17(8):1192–1199. https://doi.org/10.1016/j.spinee.2017.04.029
Ebraheim N, Sabry FF, Nadim Y, Xu R, Yeasting RA (2000) Internal architecture of the sacrum in the elderly: an anatomic and radiographic study. Spine 25(3):292–297
Acknowledgments
The institutional support received through project 2017SGR253 is acknowledged (Agència de Gestiò d’Ajuts Universitaris i de Recerca, Generalitat de Catalunya, Spain).
Funding
This work received public funding through project DPI2016-77768-R (Ministerio de Economía y Competitividad, Spain).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
González, S.G., Bastida, G.C., Vlad, M.D. et al. Analysis of bone cement distribution around fenestrated pedicle screws in low bone quality lumbosacral vertebrae. International Orthopaedics (SICOT) 43, 1873–1882 (2019). https://doi.org/10.1007/s00264-018-4115-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-4115-4