Abstract
Purpose
Porous tantalum (PT) has been widely used in orthopaedic applications for low modulus of elasticity, excellent biocompatibility, and the microstructures similar to cancellous bone. In order to improve the biological activity of PT, biologically active factors can be combined with the material. The purpose of this study was to investigate if bone morphogenetic protein 7 (BMP-7) modifications could enhance the repairing of cartilage of PT in osteochondral defect in medial femoral condyle of rabbits.
Methods
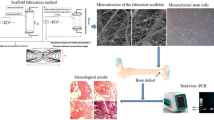
A cylindrical osteochondral defect model was created on the animal medial femoral condyle of and filled as follows: PT modified with BMP-7 for MPT group, non-modified PT for the PT group, while no implants were used for the blank group. The regenerated osteochondral tissue was assessed and analyzed by histological observations at four, eight and 16 weeks post-operation and evaluated in an independent and blinded manner by five different observers using a histological score. Osteochondral and subchondral bone defect repair was assessed by micro-CT scan at 16 weeks post-operation, while the biomechanical test was performed at 16 weeks post-operation.
Results
Briefly, higher overall histological score was observed in the MPT group compared to PT group. Furthermore, more new osteochondral tissue and bone formed at the interface and inside the inner pores of scaffolds of the MPT group compared to PT group. Additionally, the micro-CT data suggested that the new bone volume fractions and the quantity and quality of trabecular bone, as well as the maximum release force of the bone, were higher in the MPT group compared to PT group.
Conclusions
We demonstrated that the applied modified PT with BMP-7 promotes excellent subchondral bone regeneration and may serve as a novel approach for osteochondral defects repair.









Similar content being viewed by others
References
Bouwmeester SJ, Beckers JM, Kuijer R, Linden AJ, Bulstra SK (1997) Long-term results of rib perichondrial grafts for repair of cartilage defects in the human knee. Int Orthop 21(5):313–317
Gillogly SD (2003) Treatment of large full-thickness chondral defects of the knee with autologous chondrocyte implantation. Arthroscopy 19(Suppl 1):147–153
Marcacci M, Kon E, Zaffagnini S, Vascellari A, Neri MP, Iacono F (2003) New cell-based technologies in bone and cartilage tissue engineering. I. Bone reconstruction. Chir Organi Mov 88(1):33–42
Henderson I, Tuy B, Oakes B (2004) Reoperation after autologous chondrocyte implantation. Indications and findings. J Bone Joint Surg Br 86(2):205–211
Marin E, Fedrizzi L, Zagra L (2010) Porous metallic structures for orthopaedic applications: a short review of materials and technologies. Eur Orthop Traumatol 1(3–4):103–109
Helm AT, Kerin C, Ghalayini SRA, Mclauchlan GJ (2009) Preliminary results of an uncemented trabecular metal tibial component in total knee arthroplasty. J Arthroplast 24(6):941–944
Cardaropoli F, Alfieri V, Caiazzo F, Sergi V (2012) Manufacturing of porous biomaterials for dental implant applications through selective laser melting. Adv Mater Res 535-537(3):1222–1229
Bobyn JD, Poggie RA, Krygier JJ, Lewallen DG, Hanssen AD, Lewis RJ, Unger AS, O'Keefe TJ, Christie MJ, Nasser S, Wood JE, Stulberg SD, Tanzer M (2004) Clinical validation of a structural porous tantalum biomaterial for adult reconstruction. J Bone Joint Surg 86-A Suppl 2(suppl 2):123–129
Matsuno H, Yokoyama A, Watari F, Uo M, Kawasaki T (2001) Biocompatibility and osteogenesis of refractory metal implants, titanium, hafnium, niobium, tantalum and rhenium. Biomaterials 22(11):1253–1262
Bobyn JD, Stackpool GH, Hacking SA, Tanzer M, Krygier JJ (1999) Characteristics of bone ingrowth and interface mechanics of a new porous tantalum biomaterial. J Bone Joint Surg Br 81(5):907–914
Findlay DM, Welldon K, Atkins GJ, Howie DW, Zannettino AC, Bobyn D (2004) The proliferation and phenotypic expression of human osteoblasts on tantalum metal. Biomaterials 25(12):2215–2227
Johansson CB, Hansson HA, Albrektsson T (1990) Qualitative interfacial study between bone and tantalum, niobium or commercially pure titanium. Biomaterials 11(4):277–280
Zhang M, Wang GL, Zhang HF, Hu XD, Shi XY, Li S, Lin W (2014) Repair of segmental long bone defect in a rabbit radius nonunion model: comparison of cylindrical porous titanium and hydroxyapatite scaffolds. Artif Organs 38(6):493–502
Periasamy K, Watson WS, Mohammed A, Murray H, Walker B, Patil S, Meek RM (2011) A randomised study of peri-prosthetic bone density after cemented versus trabecular fixation of a polyethylene acetabular component. J Bone Joint Surg Br 93(8):1033–1044
Harrison AK, Gioe TJ, Simonelli C, Tatman PJ, Schoeller MC (2010) Do porous tantalum implants help preserve bone: evaluation of tibial bone density surrounding tantalum tibial implants in TKA. Clin Orthop Relat Res 468(10):2739–2745
Amanatullah DF, Farac R, McDonald TJ, Moehring HD, Cesare PED (2013) Subtrochanteric Fracture following removal of a porous tantalum implant. Case Rep Orthop: 946745
Sinclair SK, Konz GJ, Dawson JM, Epperson RT, Bloebaum RD (2012) Host bone response to polyetheretherketone versus porous tantalum implants for cervical spinal fusion in a goat model. Spine 37(10):E571–E580
Wang H, Li Q, Wang Q, Shi W, Gan H, Song H, Wang Z (2017) Enhanced repair of segmental bone defects in rabbit radius by porous tantalum scaffolds modified with the RGD peptide. J Mater Sci Mater Med 28(3):50
Sakou T (1998) Bone morphogenetic proteins: from basic studies to clinical approaches. Bone 22(6):591–603
Chubinskaya S, Merrihew C, Cs-Szabo G, Mollenhauer J, McCartney J, Rueger DC, Kuettner KE (2000) Human articular chondrocytes express osteogenic protein-1. J Histochem Cytochem 48(2):239–250
Mori H, Kondo E, Kawaguchi Y, Kitamura N, Nagai N, Iida H, Yasuda K (2013) Development of a salmon-derived crosslinked atelocollagen sponge disc containing osteogenicprotein-1 for articular cartilage regeneration: in vivo evaluations with rabbits. BMC Musculoskelet Disord 14(1):174
Chubinskaya S, Kawakami M, Rappoport L, Matsumoto T, Migita N, Rueger DC (2007) Anti-catabolic effect of OP-1 in chronically compressed intervertebral discs. J Ortho Res 25(4):517–530
Mason JM, Grande DA, Barcia M, Grant R, Pergolizzi RG, Breitbart AS (1998) Expression of human bone morphogenic protein 7 in primary rabbit periosteal cells: potential utility in gene therapy for osteochondral repair. Gene Ther 5(8):1098–1104
Mason JM, Breitbart AS, Barcia M, Porti D, Pergolizzi RG, Grande DA (2000) Cartilage and bone regeneration using gene enhanced tissue engineering. Clin Orthop Relat Res 379(379 Suppl):S171–S178
Vinall RL, Lo SH, Reddi AH (2002) Regulation of articular chondrocyte phenotype by bone morphogenetic protein-7, Interleukin-1, and cellular context is dependent on the cytoskeleton. Exp Cell Res 272(1):32–44
Moran ME, Kim HK, Salter RB (1992) Biological resurfacing of full-thickness defects in patellar articular cartilage of the rabbit. Investigation of autogenous periosteal grafts subjected to continuous passive motion. J Bone Joint Surg Br 74(5):659–667
Niederauer GG, Slivka MA, Leatherbury NC, Korvick DL, Harroff HH, Ehler WC, Dunn CJ, Kieswetter K (2000) Evaluation of multiphase implants for repair of focal osteochondral defects in goats. Biomaterials 21(24):2561–2574
Duan K, Hu YX, Long K, Toms A, Burt HM, Oxland TR, Masri BA, Duncan CP, Garbuz DS, Wang R (2012) Effect of alendronate-containing coatings on osteointergration into porous tantalum in a cortical bone model. Nano Life 2 (01):l-12
Wang JC, Yu WD, Sandhu HS, Tam V, Delamarter RB (1998) A comparison of magnetic resonance and computed tomographicimage quality after the implantation of tantalum and titanium spinal instrumentation. Spine 23(15):1684–1688
Zardiackas LD, Parsell DE, Dillon LD, Mitchell DW, Nunnery LA, Poggie R (2001) Structure, metallurgy, and mechanical properties of a porous tantalum foam. J Biomed Mater Res 58(2):180–187
Papanna MC, Al-Hadithy N, Somanchi BV, Sewell MD, Robinson PM, Khan SA, Wilkes RA (2012) The use of bone morphogenic protein-7 (OP-1) in the management of resistant non-unions in the upper and lower limb. Injury 43(7):1135–1140
Zamurovic N, Cappellen D, Rohner D, Susa M (2004) Coordinated activation of notch, Wnt, and transforming growth factor-beta signaling pathways in bone morphogenic protein 2-induced osteogenesis. Notch target gene Hey1 inhibits mineralization and Runx2 transcriptional activity. J Biol Chem 279(36):37704–37715
Holland TA, Bodde EW, Cuijpers VM, Baggett LS, Tabata Y, Mikos AG, Jansen JA (2007) Degradable hydrogel scaffolds for in vivo delivery of single and dual growth factors in cartilage repair. Osteoarthr Cartil 15(2):187–197
Nagura I, Fujioka H, Kokubu T, Makino T, Sumi Y, Kurosaka M (2007) Repair of osteochondral defects with a new porous synthetic polymer scaffold. J Bone Joint Surg Br 89(2):258–264
Pei M, He F, Boyce BM, Kish VL (2009) Repair of full-thickness femoral condyle cartilage defects using allogeneic synovial cell-engineered tissue constructs. Osteoarthr Cartil 17(6):714–722
Huang X, Yang D, Yan W, Shi Z, Feng J, Gao Y, Weng W, Yan S (2007) Osteochondral repair using the combination of fibroblast growth factor and amorphous calcium phosphate/poly (L-lactic acid) hybrid materials. Biomaterials 28(20):3091–3100
van der Stok J, Koolen MK, de Maat MP, Yavari SA, Alblas J, Patka P, Verhaar JA, van Lieshout EM, Zadpoor AA, Weinans H, Jahr H (2015) Full regeneration of segmental bone defects using porous titanium implants loaded with BMP-2 containing fibrin gels. Eur Cell Mater 29(4):141–153
Niederauer GG, Slivka MA, Leatherbury NC, Korvick DL, Harroff HH, Ehler WC, Dunn CJ, Kieswetter K (2000) Evaluation of multiphase implants for repair of focal osteochondral defects in goats. Biomaterials 21(24):2561–2574
Lavery K, Hawley S, Swain P, Rooney R, Falb D, Alaoui-Ismaili MH (2009) New insights into BMP-7 mediated osteoblastic differentiation of primary human mesenchymal stem cells. Bone 45(1):27–41
Bobyn JD, Toh KK, Hacking SA, Tanzer M, Krygier JJ (1999) Tissue response to porous tantalum acetabular cups: a canine model. J Arthroplasty 14(3):347–354
Duan X, Zhu X, Dong X, Yang J, Huang F, Cen S, Leung F, Fan H, Xiang Z (2013) Repair of large osteochondral defects in a beagle model with a novel type I collagen/glycosaminoglycan-porous titanium biphasic scaffold. Mater Sci Eng C Mater Biol Appl 33(7):3951–3957
Jamil K, Chua KH, Joudi S, Ng SL, Yahaya NH (2015) Development of a cartilage composite utilizing porous tantalum, fibrin,and rabbit chondrocytes for treatment of cartilage defect. J Orthop Surg Res 10:27
Gordon WJ, Conzemius MG, Birdsall E, Wannemuehler Y, Mallapragada S, Lewallen DG, Yaszemski MJ, O'Driscoll SW (2005) Chondroconductive potential of tantalum trabecular metal. J Biomed Mater Res 75(2):229–233
Wang Q, Zhang H, Li Q, Ye L, Gan H, Liu Y, Wang H, Wang Z (2015) Biocompatibility and osteogenic properties of porous tantalum. Exp Ther Med 9(3):780–786
Depprich R, Zipprich H, Ommerborn M, Mahn E, Lammers L, Handschel J, Naujoks C, Wiesmann HP, Kübler NR, Meyer U (2008) Osseointegration of zirconia implants: an SEM observation of the bone-implant interface. Head Face Med 4(1):25
Acknowledgements
We thank Dr. Jun Wang from Xijing Hosipital affiliated, Fourth Military Medical University of China for technical help in micro-CT.
Funding
This study was funded by the National Key Technology Support Program of China (Contract Grant No. 2012BAE06B03).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in this study involving animals were in accordance with the ethical standards of the institution at which the study was conducted.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Wang, Q., Zhang, H., Gan, H. et al. Application of combined porous tantalum scaffolds loaded with bone morphogenetic protein 7 to repair of osteochondral defect in rabbits*. International Orthopaedics (SICOT) 42, 1437–1448 (2018). https://doi.org/10.1007/s00264-018-3800-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-3800-7