Abstract
Objective
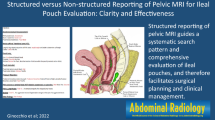
To evaluate clarity, completeness, and impact on surgical planning of MRI reporting of perianal fistulizing disease using a structured disease-specific template versus narrative reporting for planning of disease treatment by colorectal surgeons.
Materials and methods
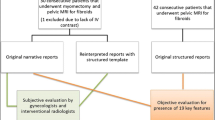
In this HIPAA-compliant, IRB-approved study with waiver of informed consent, a structured reporting template for perianal fistulizing disease MRIs was developed based on collaboration between colorectal surgeons and abdominal radiologists. The study population included 45 consecutive patients who underwent pelvic MRI for perianal fistulizing disease prior to implementation of structured reporting, and 60 consecutive patients who underwent pelvic MRI for perianal fistulizing disease after implementation of structured reporting. Objective evaluation of the reports for the presence of 12 key features was performed, as also subjective evaluation regarding the clarity and completeness of reports, and impact on surgical planning.
Results
Significantly more key features were absent in narrative reports [mean: 6.3 ± 1.8 (range 3–11)] than in structured reports [mean: 0.3 ± 0.9 (range 1–5)] (p ≤ 0.001). The use of structured reporting also increased the percentage of completeness (72.5–88.3% for surgeon 1, and 61.2–81.3% for surgeon 2; p = 0.05 and 0.03, respectively), helpfulness in surgical planning (7.1 ± 1.5–7.6 ± 1.5 for surgeon 1, and 5.8 ± 1.4–7.1 ± 1.1 for surgeon 2; p = 0.05 and p < 0.001, respectively), and clarity (7.6 ± 1.3–8.3 ± 1.1 for surgeon 1, and 5.2 ± 1.4–7.1 ± 1.3 for surgeon 2; p = 0.006 and p < 0.001, respectively) of the reports.
Conclusion
Structured MRI reports in patients with perianal fistulizing disease miss fewer key features than narrative reports. Moreover, structured reports were described as more complete and clear, and more helpful for treatment planning.




Similar content being viewed by others
References
Bink A, Benner J, Reinhardt J, et al. Structured reporting in neuroradiology: Intracranial tumors. Front Neurol 2018; 32:1–10
Ganeshan D, Duong PAT, Probyn L, et al. Structured reporting in radiology. Acad Radiol 2018; 25:66–73
de Miguel Criado J, del Salto LG, Rivas PF, et al. MR imaging evaluation of perianal fistulas: spectrum of imaging features. Radiographics 2012; 32:175–194
Abcarian H, Anal fistula principles and management, 1st ed. New York, NY: Springer, 2014:1–3
Hamadani A, Haigh PI, Liu IA, Abbas MA. Who is at risk for developing chronic anal fistula or recurrent anal sepsis after initial perianal abscess? Dis Colon Rectum 2009; 52:217–221
O’Malley RB, Al-Hawary MM, Kaza RK, Wasnik AP, Liu PS, Hussain HK. Rectal imaging: part 2, perianal fistula evaluation on pelvic MRI - what the radiologist needs to know. AJR 2012; 199:43–53
Gecse K, Khanna R, Stoker J, et al. Fistulizing crohn’s disease: diagnosis and management. United Eur Gastroenterol J 2013; 1:206–213
Beaugerie L, Carrat F, Nahon S, et al. High risk of anal and rectal cancer in patients with anal and/or perianal Crohn’s disease. Clin Gastroenterol Hepatol 2018; 16:892–899
Protyniak B, Shutt T, Farmer R. Squamous cell carcinoma originating from a Crohn's enterocutaneous fistula. Case Rep Surg 2017; 2017:1–4
Ong EM, Ghazi LJ, Schwartz DA, Mortelé KJ. Guidelines for imaging of Crohn's perianal fistulizing disease. Inflamm Bowel Dis 2015; 21:731–736
Sahni VA, Ahmad R, Burling D. Which method is best for imaging of perianal fistula? Abdom Imaging 2008; 33:26–30
Kim MJ. Transrectal ultrasonography of anorectal diseases: advantages and disadvantages. Ultrasonography 2015; 34:19-31
Burdan F, Sudol-Szopinska I, Staroslawska E, et al. Magnetic resonance imaging and endorectal ultrasound for diagnosis of rectal lesions. Eur J Med Res 2015; 20:1–14
Sharma G, Khandige G, Mohan M. Magnetic resonance imaging in perianal fistulas-a pictorial atlas. Indian J Gastroenterol 2016; 35:337–342
Parks AG, Gordon PH, Hardcastle JD. A classification of fistula‐in‐ano. Br J Surg 1976; 63:1–12
Van Assche G, Vanbeckevoort D, Bielen D, et al. Magnetic resonance imaging of the effects of infliximab on perianal fistulizing Crohn's disease. Am J Gastroenterol 2003: 98:332–339
Tutein Nolthenius CJ, Bipat S, Mearadji B, et al. MRI characteristics of proctitis in Crohn’s disease on perianal MRI. Abdom Radiol 2016; 41:1918–1930
Brook OR, Brook A, Vollmer CM, Kent TS, Sanchez N, Pedrosa I. Structured reporting of multiphasic CT for pancreatic cancer: potential effect on staging and surgical planning. Radiology 2015; 274:464–472
Nörenberg D, Sommer WH, Thasler W, et al. Structured reporting of rectal magnetic resonance imaging in suspected primary rectal cancer: potential benefits for surgical planning and interdisciplinary communication. Invest Radiol 2017; 52:232–239
Franconeri A, Fang J, Carney B, et al. Structured vs narrative reporting of pelvic MRI for fibroids: clarity and impact on treatment planning. Eur Radiol 2017; 28:3009–3017
Gassenmaier S, Armbruster M, Haasters F, et al. Structured reporting of MRI of the shoulder – improvement of report quality? Eur Radiol 2017; 27:4110–4119
Zimmerman SL, Kim W, Boonn WW. Informatics in radiology: automated structured reporting o imaging findings using at AIM standard and XML. Radiographics 2011; 31:881–887
Brady AP. Error and discrepancy in radiology: inevitable or avoidable? Insights Imaging 2017; 8:171–182
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tuncyurek, O., Garces-Descovich, A., Jaramillo-Cardoso, A. et al. Structured versus narrative reporting of pelvic MRI in perianal fistulizing disease: impact on clarity, completeness, and surgical planning. Abdom Radiol 44, 811–820 (2019). https://doi.org/10.1007/s00261-018-1858-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-018-1858-8