Abstract
Aims
There is a controversy as to the relative efficacy of 177Lu prostate specific membrane antigen (PSMA) radioligand therapy (RLT) and third-line treatment for patients with metastatic castration-resistant prostate cancer (mCRPC). The aim of our systematic review was to elucidate whether 177Lu-PSMA RLT and third-line treatment have similar effects and adverse effects (PROSPERO ID CRD42017067743).
Methods
The review followed Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines. Searches in Pubmed and Embase selected articles up to September 2017. A search in ClinicalTrials.gov indicated ongoing studies. The meta-analysis used the random-effects model.
Results
Twelve studies including 669 patients reported 177Lu-PSMA RLT. Overall, 43% of the patients had a maximum decline of PSA of ≥50% following treatment with 177Lu-PSMA RLT. The treatment with 177Lu-PSMA-617 and 177Lu-PSMA for imaging and therapy (I&T) had mainly transient adverse effects. Sixteen studies including 1338 patients reported third-line treatment. Overall, 21% of the patients had a best decline of PSA of ≥50% following third-line treatment. After third-line treatment with enzalutamide and cabazitaxel, adverse effects caused discontinuation of treatment for 10% to 23% of the patients. 177Lu-PSMA RLT gave a best PSA decline ≥50% more often than third-line treatment (mean 44% versus 22%, p = 0.0002, t test). 177Lu-PSMA RLT gave objective remission more often than third-line treatment (overall 31 of 109 patients versus 43 of 275 patients, p = 0.004, χ2 test). Median survival was longer after 177Lu-PSMA RLT than after third-line treatment, but the difference was not statistically significant (mean 14 months versus 12 months, p = 0.32, t test). Adverse effects caused discontinuation of treatment more often for third-line treatment than for 177Lu-PSMA RLT (22 of 66 patients versus 0 of 469 patients, p < 0.001, χ2 test).
Conclusions
As for patients with mCRPC, treatment with 177Lu-PSMA-617 RTL and 177Lu-PSMA I&T gave better effects and caused fewer adverse effects than third-line treatment.
Similar content being viewed by others

Introduction
Prostate cancer (PC) is the most frequent non-cutaneous cancer and the second most frequent cause of cancer deaths for adult men. A worldwide estimate of PC in 2008 implied 899,000 new cases and 258,000 PC deaths [1]. Most patients with PC who die, die of metastatic PC (mPC) [2]. Six drugs increase overall survival for patients with metastatic castration-resistant prostate cancer (mCRPC) [3,4,5,6,7,8]. Patients with symptomatic mCRPC have initially been treated with docetaxel [3, 9]. Abiraterone, enzalutamide, cabazitaxel, sipoleucel, and 223radium increase overall survival for patients who had failed treatment with docetaxel [4,5,6,7,8, 10]. However, randomized trials have not evaluated the drugs for patients with failure in response to second-line treatment following recurrence after docetaxel. Therefore, European Association of Urology (EAU)/European Society of Radiotherapy and Oncology (ESTRO) guidelines do not recommend third-line treatment of mCRPC [11]. Due to unmet needs, the St. Gallen Advanced Prostate Cancer Consensus Conference (APCCC) 2017 gathered a representative group of experts for summarizing their opinions about treatment of advanced PC [12]. APCCC 2017 favored third-line treatment with cabazitaxel and with androgen receptor (AR) and AR signaling inhibitors.
Of PC, poorly differentiated, metastatic, and hormone-refractory adenocarcinomas of the prostate express prostate-specific membrane antigen (PSMA) [13]. 68Ga-PSMA HBED-CC PET/CT detects sites of cancer lesions for most patients with mCRPC [14, 15]. Patients with a positive 68Ga-PSMA HBED-CC PET/CT might be treated with 177Lu-PSMA radioligand therapy (RLT) [16]. 177Lu-J591 is a macromolecular radiolabeled humanized monoclonal antibody that targets the extracellular part of PSMA. 177Lu-J591 has a modest effect and causes frequent serious myelosuppression. 177Lu-PSMA-617 and 177Lu-PSMA I&T are small-molecule inhibitors of PSMA that give better effects and cause less adverse effects than 177Lu-J591.117Lu-PSMA RLT is mainly used as a compassionate treatment of patients with end-stage mCRPC [17]. For a patient with only lymph node metastatic CRPC, 177Lu-PSMA-617 RLT reduced PSA more than salvage radiotherapy and abiraterone [18]. In contrast, APCCC 2017 did not refer to 177Lu-PSMA RLT [19].
The discrepancy motivated us to carry out a systematic review comparing the two types of treatment [20]. The null hypothesis for our analyses was that 177Lu-PSMA RLT and third-line treatment of mCRPC have similar effects. The PROSPERO database registered our systematic review as CRD42017067743.
Material and methods
Our systematic review evaluated the null hypothesis by comparing outcome following the two types of treatment.
Search strategy
The systematic review followed guidelines of the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) [21]. We selected articles that reported patients with mCRPC given 177Lu-PSMA RLT or third-line treatment and evaluated at least one effect measure. Reviewers undertook searches in Pubmed and Embase for articles published until September 2017. Two reviewers (FEvE and IV) searched independently for articles that reported 177Lu-PSMA RLT. A Pubmed search combined MESH terms and free text words: {(“prostat* neoplasm* [Mesh] OR prostate cancer) AND (prostate specific membrane antigen [Mesh] OR PSMA) AND (*lutetium [Mesh] OR *lu)}. The reviewers undertook a similar search in Embase. Two reviewers (FEvE and GR) searched independently for articles that reported third-line treatment. A Pubmed search combined MESH terms and free text words: {(“prostat* neoplasm* [Mesh] OR prostate cancer) AND (abiraterone [Mesh] OR enzalutamide [Mesh] OR cabazitaxel [Mesh]) AND (third line treatment OR third line therapy)}. The reviewers undertook a similar search in Embase. We used previous systematic reviews as external validation of our literature searches [16, 22, 23]. A reviewer (FEvE) also undertook a manual search and also a search for ongoing studies in ClinicalTrials.gov.
Study selection
As regards 177Lu-PSMA RLT, we selected original research articles that reported ≥10 patients treated for mCRPC. Of several articles from a single center or a group of centers, we included the articles that reported the most patients. However, if the second of two articles from a center evaluated >50% of the patients who were not reported in the first article, we included both articles. We excluded articles that reported only biodistribution or dosimetry of 177Lu-PSMA RLT, and articles that used therapy with radioligands other than 177Lu-PSMA.
As regards third-line treatment, we selected original research articles that reported ≥10 patients treated for mCRPC. We selected articles of first- to third-line treatments that used only life-prolonging drugs. We included an article by Caffo et al. [24] that reported different sequences of drugs for the second- and third-line treatment. We also included an article by Brasso et al. [25] that summarized four previous articles of enzalutamide. Further, we included an article that reported cabazitaxel for patients who previously had failed with an AR inhibitor or an AR signaling inhibitor. Of articles that combined second- and third-line treatments or third- and fourth-line treatments, we included the articles that reported the third-line treatment separately. We excluded articles that reported only adverse effects.
Data extraction
Of data from the selected articles, we extracted baseline characteristics such as year of publication, name of the first author, number of patients, and numbers of patients with metastases in lymph nodes, bones, and visceral organs. In the articles, surgical or medical castration implied serum testosterone was reduced to levels <50 ng/dL or <1.7 nmol/L. Hence, patients had CRPC if they had progression of PC despite castration levels of testosterone. We extracted treatment characteristics from articles of 177Lu-PSMA RLT such as number of previous treatments of mCRPC, median/mean PSA at start of 177Lu-PSMA RLT, type of 177Lu-PSMA RLT, median/mean number of cycles of treatment, median/mean interval between cycles, and median/mean administered activity of 177Lu for each cycle. We extracted treatment characteristics in articles of third-line treatment such as the drugs used as first-, second-, and third-line treatment, median/mean PSA at start of the third-line treatment, and dosage of the third-line drug. We extracted data on the frequency of severe adverse effects as graded by the National Cancer Institute Common Terminology Criteria for Adverse Events (CTCAE) version 4 for grade 3 and 4 hematologic and non-hematologic adverse effects.
The articles followed guidelines 2 by the Prostate Cancer Trials Working Group (PCWG2) [26]. As treatment endpoints in the articles, we extracted the frequency of best PSA decline of ≥50%, the frequency of objective response, and overall survival. The articles classified objective response by Response Evaluation Criteria in Solid Tumor (RECIST) 1.1 [27]. We combined complete remission (CR) and partial remission (PR) as objective remission. The articles defined overall survival as survival from start of treatment to death of any cause or to end of follow-up.
The selection of articles served as quality control.
A reviewer (FEvE) contacted principal authors for complementary information of selected articles.
Statistical analysis
We undertook patient-based evaluations for each study and used parametric and non-parametric statistics in our evaluations. The articles calculated the frequency of treatment response as the proportion of responders of all patients. For articles with more than one response evaluation, we selected the highest frequency of response. The articles calculated the frequency of serious adverse effects as the proportion of patients with grade 3 to 4 adverse effect of all patients. We used the random-effects model in our meta-analysis because we assumed patients and treatments had hidden heterogeneity. We undertook funnel plots of the articles with the two types of treatment to evaluate articles for publication bias [28]. The meta-analysis generated forest plots of the articles to summarize the frequency of a best PSA decline of ≥50%. Forest plots were based on the software program metaprop for STATA, as described previously [29]. The metaprop analyses were based on the random-effects model. As for overall survival, we calculated the median and the interquartile range for the median overall survival reported in the articles. We used χ2 tests as we compared proportions of frequencies in the two groups of treatments and t tests as we compared distributions of frequencies. We considered a p value <0.05 as statistically significant.
One author (FEvE) performed all statistical analyses using the software STATA 14.2 (StataCorp., College Station, TX, USA).
Results
Studies of 177Lu-PSMA RLT
A search for articles of 177Lu-PSMA RLT gave 63 hits. The selected 12 articles consisted of 669 patients (Fig. 1a and Table 1) [30,31,32,33,34,35,36,37,38,39,40,41]. The median of the median/mean age in the articles was 70 years [25% and 75% interquartile range (IQR) 69–71 years]. The median of the median/mean pretreatment PSA was 130 ng/ml (IQR 77–306 ng/ml). Ten articles reported patients with end-stage mCRPC and two articles reported a heterogeneous group of patients [34, 40]. Nine articles used 177Lu-PSMA-617 RLT, two articles used 177Lu-J591 [30, 31], and one article used 177Lu-PSMA I&T [32]. A third of the patients underwent one cycle, the second third underwent two cycles, and the last third underwent three or more cycles. Nine articles administered 177Lu activity of approximately 6 G becquerel (GBq) for each cycle. During the study period, one article increased the administered 177Lu activity from 1.1 GBq to 6.0 GBq [37], one article from 4 to 6 GBq [33], and one article increased the administered activity from 3.7 to 7.4 GBq [32].
Overall, the articles reported the frequency decline of best PSA ≥50% for 1687 of 2007 (84%) of the patients.
Efficacy
We undertook a funnel plot of the frequency of best PSA decline of ≥50% in the articles of 177Lu-PSMA RLT (Fig. 2a). The funnel plot did not indicate the articles had a publication bias. A forest plot of the articles summarized the frequency of best PSA decline of ≥50% for the two main types of 177Lu radioligands (Fig. 3). Overall, 44% [95% confidence intervals (CIs) 31–51%] of the patients had a best PSA decline of ≥50%. As for 177Lu-PSMA-617 RLT and 177Lu-PSMA I&T combined, 51% (95% CI: 43–60%) of the patients had a best PSA decline of ≥50%. Of evaluable articles, a median of 29% (IQR 8–36%) of the patients had objective remission. With an increasing number of cycles, the frequency of objective remission increased [37, 38]. In evaluable articles, the patients had a median overall survival of 14 months. Tagawa et al. [31] found median overall survival following treatment with 177Lu-J591 was 17 months. Ahmadzadefar et al. [35] found that patients with a best PSA decline of ≥50% after the third cycle of 177Lu-PSMA RLT lived significantly longer than patients with less extensive decline of PSA (17 months versus 10 months, p = 0.001, log-rank test). In evaluable articles, the mean of the median overall survival after 177Lu-PSMA RLT was 14 months. In two articles, overall survival remained above 50% during the follow-up [34, 37].
Forest plot showing the frequency of a best PSA decline of ≥50% in 12 articles with 177Lu-PSMA RLT, 177Lu-PSMA-617, and 177Lu-PSMA I&T (10 articles) gave a higher frequency of a best PSA decline of ≥50% than given by 177Lu-PSMA-J591 (2 articles). The forest plot shows pooled estimates of the frequency of a best PSA decline of ≥50% with 95% confidence intervals shown as a line
Adverse effects
The three forms for 177Lu-PSMA RLT differed in adverse effects. Bander et al. [30] and Tagawa et al. [31] found that 10 of 35 patients and 21 of 47 patients, respectively, developed severe thrombocytopenia after treatment with 177Lu-J591. The patients were given platelet transfusions. Thus, 31 of 82 (39%) of the patients treated with 177Lu-J591 developed grade 3 or 4 thrombocytopenia in contrast to 6 of 243 (2%) of the patients treated with 177Lu-PSMA-617 and 177Lu-PSMA I&T (p < 0.001, χ2 test with one degree of freedom) [32, 33, 37, 38, 41]. Rahbar et al. [38] found that 8% of the patients treated with 177Lu-PSMA-617 RLT developed xerostomia.
Studies of third-line treatment
A search for articles of third-line treatment gave 40 hits. The selected 16 articles included 1338 patients (Fig. 1b and Table 2) [24, 25, 42,43,44,45,46,47,48,49,50,51,52,53,54,55]. All articles reported retrospective cohort studies. The median of the median/mean age at diagnosis was 70 years (IQR 69–71 years). The median of the median/mean pretreatment PSA was 130 ng/ml (IQR 77–306 ng/ml). In all articles, docetaxel was the first systemic treatment. Patients with failure to respond docetaxel were treated with abiraterone, enzalutamide, and cabazitaxel. Most articles used abiraterone before enzalutamide, but a subgroup of patients in one article were given enzalutamide as the first AR pathway inhibitor [24]. Third-line treatment was abiraterone for 288 (21%) patients [24, 42, 43, 49, 50, 53], enzalutamide for 596 (45%) patients [24, 25, 48, 51, 52], and cabazitaxel for 454 (34%) patients [44,45,46, 48, 51, 54]. As for the third-line treatment, the dose for abiraterone was 1000 mg/day and 160 mg/day for enzalutamide. For cabazitaxel, the dose was 20 or 25 mg/m2 body surface intravenously every 3 weeks. Sella et al. [28] gave patients treated with cabazitaxel prophylaxis with granulocyte-colony stimulating factor (G-CSF).
Efficacy
A funnel plot evaluated the articles of third-line treatment for the frequency of best PSA decline of ≥50% after the treatment. A funnel plot of cabazitaxel articles did not indicate publication bias (Fig. 2b). A forest plot shows the frequency of best PSA decline of ≥50% according to the sequences of second- and third-line drugs (Fig. 4). Summarizing the findings in all articles, 21% (95% CI 16–27%) of the patients had a PSA decline of ≥50%. After third-line treatment, the pooled frequency of best PSA decline of ≥50% was 4% with abiraterone, 20% with enzalutamide, and 29% with cabazitaxel. Hence, cabazitaxel caused a best decline of PSA of ≥50% more often than AR and AR signaling inhibitors (29% versus 19%, p = 0.001, χ2 test with one degree of freedom). In seven articles, the median frequency of objective remission was 15% (IQR 13–20%). Patients with a best PSA decline of ≥50% after treatment with enzalutamide lived longer than patients with a smaller best decline of PSA [25]. In evaluable articles, the median of the median overall survival was 11 months (range 7–20 months). An article showed that background clinical characteristics such a performance status, level of hemoglobin, and activity of serum alkaline phosphatase had a significant impact on overall survival.
Forest plot regarding the frequency of a best PSA decline of ≥50% in 16 articles of third-line treatment. The frequency of a best PSA decline of ≥50% increased summarizing 3 articles with abiraterone, 5 articles with enzalutamide, and 8 articles with cabazitaxel. The forest plot shows pooled estimates of the frequency of best PSA decline of ≥50%, with the 95% confidence interval shown as a line
Adverse effects
The third-line drugs differed in adverse effects. Most articles did not report adverse effects. Loriot et al. [42] showed that 3 of 30 (10%) patients stopped treatment with enzalutamide due to adverse effects. Later, the patients were treated with abiraterone and it did not cause similar adverse effects. Kongsted et al. [53] found that 15 of 66 (23%) patients treated with cabazitaxel stopped the treatment due to adverse effects.
Comparison of 177Lu-PSMA RLT and third-line treatment
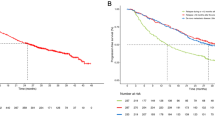
The articles of 177Lu-PSMA RLT and third-line treatment did not compare the outcomes head-to-head. Neither was 177Lu-PSMA RLT reported as third-line treatment. So, we could only indirectly compare 177Lu-PSMA RLT and third-line treatment. In the articles of the two types of treatment, the age at diagnosis was similar (the mean of the median age was 71 versus 69 years, p = 0.20, t test). Articles of 177Lu-PSMA RLT had higher pre-treatment PSA values than articles of third-line treatment, but the difference was not statistically significant (the mean of the median PSA level was 247 ml versus 197 ng/ml, p = 0.48, t test). Despite the similarities, 177Lu-PSMA RLT caused a best decline of PSA ≥50% twice as often as the third-line treatment (mean frequency 44% versus 22%, p = 0.0002, t test; Table 3). Figure 5a shows that the best PSA decline ≥50% differed between patients in the two groups of treatments. 177Lu-PSMA RLT also caused a higher frequency of objective remission than third-line treatment (Fig. 5b). Overall, 31 of 109 patients versus 43 of 275 patients had objective remission (p < 0.001, χ2 test with one degree of freedom). Figure 5c shows that patients given 177Lu-PSMA RLT tended to live longer than patients given third-line treatment (median of 14 months versus 11 months), but the difference was not statistically significant. Third-line treatment was stopped more often than 177Lu-PSMA RLT (22 of 66 patients versus 0 of 469 patients, p < 0.001, χ2 test with one degree of freedom).
Discussion
In our comparisons, up to half the patients given 177Lu-PSMA RLT obtained a best PSA decline of ≥50%, whereas up to a third of the patients given third-line treatment obtained such a decline of PSA. Specifically, 177Lu-PSMA-617 RLT and 177Lu-PSMA I&T reduced PSA ≥50% more often and caused fewer adverse effects than cabazitaxel.
Our literature search for 177Lu-PSMA RLT and third-line treatment differed because different specialists gave the treatments to different groups of patients. But we undertook similar statistical analyses of clinical characteristics and outcomes for both types of treatments in our meta-analysis of the selected articles. Funnel plots did not indicate publication bias in the articles regarding the two types of treatment. The forest plots gave robust findings regarding 177Lu-J591, and third-line therapy with abiraterone and enzalutamide.
Our systematic review found a higher response rate for 177Lu-PSMA RLT than the previous systematic review by Calopedos et al. [16]. The difference may be due to differences in selection of articles. Our systematic review included more recent articles than the previous review and excluded data reported only as abstracts. Furthermore, our systematic review evaluated the selection of articles with funnel plots, and included boxplots of the frequency of objective remission and overall survival as end-points for effect of the treatment. Anyway, both systematic review supported that 177Lu-PSMA RLT is effective as treatment of mCRPC [16]. 177Lu-PSMA-617 RLT and 177Lu-PSMA I&T caused a best PSA decline of ≥50% more often and caused less adverse effects than 177Lu-J591. Articles of 177Lu-PSMA-617 RLT and 177Lu-PSMA I&T reported mainly transitory adverse effects. Reviews of dosimetry and practical aspects indicated that 177Lu-PSMA RLT was safe [13, 56]. Typically, for the articles in our review, 177Lu-PSMA RLT was administered at 8-week intervals with an activity of 6 GBq of 177Lu for each cycle. The typical intervals and 177Lu activities were in accordance with recommendations by the German Society of Nuclear Medicine [57]. However, the low number of cycles for two thirds of the patients was not optimal, and neither was the recommended interval and activity for 177Lu-PSMA-RLT. A recent trial escalated the activity for each cycle from 6 to 9.3 GBq [58]. An Austrian study gave three cycles of 7.4 GBq with 4-week intervals. Also, a third study proposed a shorter interval between cycles [40]. An Australian trial gave an 177Lu activity of 4–8 GBq for each cycle and used 6-week intervals between the cycles (ACTRN12615000912583), presented as an abstract for the ESMO conference 2017 (Abstract 7850, Ann Oncol 2017, 28 suppl 5, v269–v294).
As for third-line treatment, our systematic review reported poorer overall survival than the review by Maines et al. [22]. The previous review summarized survival after failure to first-line docetaxel, whereas our review summarized survival from start of third-line treatment. The systematic review and meta-analysis by Maines et al. also differed with an Italian multicenter study regarding the impact cabazitaxel given as second- or third-line treatment had on overall survival [22, 24]. Most specialist at APCCC 2017 voted for cabazitaxel as third-line treatment. In contrast in our review, nearly half the reported patients had enzalutamide as third-line treatment and cabazitaxel was third-line treatment only for a third of the patients. As for patients given abiraterone as third-line treatment, the outcome suggested a cross-resistance after second-line treatment with enzalutamide.
Given as third-line treatment, cabazitaxel reduced the best PSA decline of ≥50% more often than abiraterone and enzalutamide, but caused more adverse effects and did not increase overall survival.
The third-line treatment in our articles followed general practice. All articles used a sequence of monotherapies with docetaxel as the first systemic treatment. All articles used standard dose for the third-line drugs. Today, cabazitaxel may cause less adverse effects than those reported following cabazitaxel in our review. Trials comparing 20-mg/m2 and 25-mg/m2 body surface dose levels of cabazitaxel showed non-inferiority for the low dose [59]. Accordingly, APCCC 2017 preferred the low dose of cabazitaxel combined with G-CSF prophylaxis from the start of treatment [12]. Thus, the articles of third-line treatment pointed to the real effect of the treatment.
The systematic review of Calopedos et al. [16] compared the outcome following 177Lu-PSMA RLT with the outcome following cabazitaxel as reported in the TROPIC trial [4]. In contrast, we compared articles of cohort studies of 177Lu-PSMA RLT and of third-line treatment using the same statistical methodology. Our comparison might give a more realistic estimate of the difference between the two types of treatment. Our findings contradicted conventional assumptions of inferiority or non-inferiority for 177Lu-PSMA RLT compared with third-line treatment. APCCC 2017 recommended third-line treatment only with drugs known to prolong life as second-line treatment [12]. But in our review, 177Lu-PSMA RLT was more effective than third-line treatment despite being given later in the treatment sequence for mCRPC. Correspondingly, 177Lu-PSMA-617 RLT gave better PSA decline than abiraterone in a recent case report [18].
Our systematic review is a correlate to APCCC 2017 [12, 19]. For glu-ureido-based inhibitor 177Lu-PSMA RLT, our evidence was articles including 582 patients from 9 centers. Our evidence for cabazitaxel as third-line treatment was articles including 454 patients from 9 centers. We find it irrational that APCCC 2017 insisted that the effect of 177Lu-PSMA RLT should be proven in a randomized trial whereas the APCCC 2017 recommended third-line treatment without such a proof of effect. Evidence-based medicine prefers to base treatment decisions on a systematic review as alternative to the opinion of the (medical oncology) experts. In absence of randomized trials, oncologists should choose between 177Lu-PSMA-617 RLT and third-line treatment based on effects and adverse effects of the treatments [20]. APCCC 2017 voted that patients with end-stage mCRPC should be treated with carboplatin-containing regimens [12]. However, information regarding carboplatin-containing regimens is sparse. A preference for carboplatin-containing regimens for end-stage mCRPC implies that the PC has small cell/neuroendocrine histology. But the assumption has not been proven.
ClinicalTrials.gov registered ongoing studies of 177Lu-PSMA RLT (NCT03042468, NCT03042312,). Twenty-five ongoing studies are evaluating the aspects of third-line treatment [37]. ClinicalTrials.gov also registered five studies of third-line treatment (NCT02729103, NCT01718353, NCT02254785, NCT02485691, and NCT02125357). Ongoing studies aim to define the best schedule for 177Lu-PSMA RLT. The study NCT03042468 is evaluating dose escalation of 177Lu activity from 1.85 to 11.6 GBq for each cycle, given at 2-week intervals. A German study reported dose escalation of 177Lu activity for each cycle from 4 to 9.3 GBq [58]. Other studies examine new roles for 177Lu-PSMA RLT. An ongoing study is evaluating 177Lu-PSMA RLT for patients with lymph node metastatic CRPC. Similarly, APCCC 2017 argued for trials that compare 177Lu-PSMA RLT and third-line treatment [19]. 177Lu-PSMA RLT is also being examined as part of combination therapy. A case report described outcome following treatment with a combination of 177Lu-PSMA-617 RLT and EBRT [60]. An ongoing study (NCT00916123) is evaluating 177Lu-J591 combined with docetaxel.
In recent years, management of PC has changed rapidly [11, 61, 62]. AR and AR signaling inhibitors cause less adverse effects than docetaxel. Therefore, today, AR and AR signaling inhibitors may be the first systemic treatment of castration-naïve mPC and mCRPC [63,64,65,66,67]. Initiation of androgen deprivation therapy (ADT) may also be combined with docetaxel [53, 54]. Thus, our analyses of post-docetaxel treatment remain relevant for patients with CRPC today where initiation of ADT is combined with docetaxel.
Our systematic review and meta-analysis has limitations. The articles mainly used 177Lu-PSMA RLT for patients with end-stage PC. So, the review did not evaluate the efficacy for patients in an earlier phase of PC. Background factors may be important for overall survival after third-line treatment, but the articles rarely reported these characteristics. The articles summarized overall survival from start of 177Lu-PSMA RLT or start of third-line treatment and not from a common point in the progression of the disease such as the diagnosis of mCRPC. As the articles had a short follow-up, our review did not assess long-term effects and adverse effects of 177Lu-PSMA RLT.
Conclusion
177Lu-PSMA RLT had better effects and caused less adverse effects than third-line treatment.
References
Center MM, Jemal A, Lortet-Tieulent J, Ward E, Ferlay J, Brawley O, et al. International variation in prostate cancer incidence and mortality rates. Eur Urol. 2012;61:1079–92.
Patrikidou A, Loriot Y, Eymard JC, Albiges L, Massard C, Ileana E, et al. Who dies from prostate cancer? Prostate Cancer Prostatic Dis. 2014;17:348–52.
Tannock IF, de Wit R, Berry WR, Horti J, Pluzanska A, Chi KN, et al. Docetaxel plus prednisone or mitoxantrone plus prednisone for advanced prostate cancer. N Engl J Med. 2004;351:1502–12.
de Bono JS, Oudard S, Ozguroglu M, Hansen S, Machiels JP, Kocak I, et al. Prednisone plus cabazitaxel or mitoxantrone for metastatic castration-resistant prostate cancer progressing after docetaxel treatment: a randomised open-label trial. Lancet. 2010;376:1147–54.
de Bono JS, Logothetis CJ, Molina A, Fizazi K, North S, Chu L, et al. Abiraterone and increased survival in metastatic prostate cancer. N Engl J Med. 2011;364:1995–2005.
Scher HI, Fizazi K, Saad F, Taplin ME, Sternberg CN, Miller K, et al. Increased survival with enzalutamide in prostate cancer after chemotherapy. N Engl J Med. 2012;367:1187–97.
Sartor O, Coleman R, Nilsson S, Heinrich D, Helle SI, O’Sullivan JM, et al. Effect of radium-223 dichloride on symptomatic skeletal events in patients with castration-resistant prostate cancer and bone metastases: results from a phase 3, double-blind, randomised trial. Lancet Oncol. 2014;15:738–46.
Kantoff PW, Higano CS, Shore ND, Berger ER, Small EJ, Penson DF, et al. Sipuleucel-T immunotherapy for castration-resistant prostate cancer. N Engl J Med. 2010;363:411–22.
Berthold DR, Pond GR, Soban F, de Wit R, Eisenberger M, Tannock IF. Docetaxel plus prednisone or mitoxantrone plus prednisone for advanced prostate cancer: updated survival in the TAX 327 study. J Clin Oncol. 2008;26:242–5.
Summers N, Vanderpuye-Orgle J, Reinhart M, Gallagher M, Sartor O. Efficacy and safety of post-docetaxel therapies in metastatic castration-resistant prostate cancer: a systematic review of the literature. Curr Med Res Opin. 2017:1–14.
Cornford P, Bellmunt J, Bolla M, Briers E, De Santis M, Gross T, et al. EAU-ESTRO-SIOG guidelines on prostate cancer. Part II: treatment of relapsing, metastatic, and castration-resistant prostate cancer. Eur Urol. 2017;71:630–42.
Gillessen S, Attard G, Beer TM, Beltran H, Bossi A, Bristow R, et al. Management of Patients with Advanced Prostate Cancer: The Report of the Advanced Prostate Cancer Consensus Conference APCCC 2017. Eur Urol 2017.
Kopka K, Benesova M, Barinka C, Haberkorn U, Babich J. Glu-Ureido-based inhibitors of prostate-specific membrane antigen: lessons learned during the development of a novel class of low-molecular-weight Theranostic radiotracers. J Nucl Med. 2017;58:17S–26S.
Perera M, Papa N, Christidis D, Wetherell D, Hofman MS, Murphy DG, et al. Sensitivity, specificity, and predictors of positive 68Ga-prostate-specific membrane antigen positron emission tomography in advanced prostate cancer: a systematic review and meta-analysis. Eur Urol. 2016;70:926–37.
von Eyben FE, Picchio M, von Eyben R, Rhee H, Bauman G. 68Ga-labeled prostate-specific membrane antigen ligand positron emission tomography/computed tomography for prostate cancer: a systematic review and meta-analysis. Eur Urol Focus 2016.
Calopedos RJS, Chalasani V, Asher R, Emmett L, Woo HH. Lutetium-177-labelled anti-prostate-specific membrane antigen antibody and ligands for the treatment of metastatic castrate-resistant prostate cancer: a systematic review and meta-analysis. Prostate Cancer Prostatic Dis. 2017;20:352–60.
Fendler WP, Rahbar K, Herrmann K, Kratochwil C, Eiber M. 177Lu-PSMA Radioligand therapy for prostate cancer. J Nucl Med. 2017;58:1196–200.
von Eyben FE, Kiljunen T, Joensuu T, Kairemo K, Uprimny C, Virgolini I. 177Lu-PSMA-617 radioligand therapy for a patient with lymph node metastatic prostate cancer. Oncotarget. 2017;8:66112–6.
Gillessen S, de Bono JS, Sartor O, Omlin AG. Reply to Finn E. von Eyben, Irene Virgolini and Giandomenico Roviello’s Letter to the Editor re: Silke Gillessen, Gerhardt Attard, Tomasz M. Beer, et al. Management of Patients with Advanced Prostate Cancer: The Report of the Advanced Prostate Cancer Consensus Conference APCCC 2017. Eur Urol. In press. https://doi.org/10.1016/j.eururo.2017.06.002. Eur Urol. 2017.
von Eyben FE, Virgolini I, Roviello G. Re: Silke Gillessen, Gerhardt Attard, Tomasz M. Beer, et al. Management of Patients with Advanced Prostate Cancer: The Report of the Advanced Prostate Cancer Consensus Conference APCCC 2017. Eur Urol. In press. https://doi.org/10.1016/j.eururo.2017.06.002. Eur Urol. 2017.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med. 2009;151:W65–94.
Maines F, Caffo O, Veccia A, Trentin C, Tortora G, Galligioni E, et al. Sequencing new agents after docetaxel in patients with metastatic castration-resistant prostate cancer. Crit Rev Oncol Hematol. 2015;96:498–506.
Roviello G, Petrioli R, Laera L, Francini E. The third line of treatment for metastatic prostate cancer patients: option or strategy? Crit Rev Oncol Hematol. 2015;95:265–71.
Caffo O, De Giorgi U, Fratino L, Alesini D, Zagonel V, Facchini G, et al. Clinical outcomes of castration-resistant prostate cancer treatments administered as third or fourth line following failure of docetaxel and other second-line treatment: results of an Italian multicentre study. Eur Urol. 2015;68:147–53.
Brasso K, Thomsen FB, Schrader AJ, Schmid SC, Lorente D, Retz M, et al. Enzalutamide antitumour activity against metastatic castration-resistant prostate cancer previously treated with docetaxel and Abiraterone: a multicentre analysis. Eur Urol. 2015;68:317–24.
Scher HI, Morris MJ, Basch E, Heller G. End points and outcomes in castration-resistant prostate cancer: from clinical trials to clinical practice. J Clin Oncol. 2011;29:3695–704.
Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45:228–47.
Sterne JA, Sutton AJ, Ioannidis JP, Terrin N, Jones DR, Lau J, et al. Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ. 2011;343:d4002.
Nyaga VN, Arbyn M, Aerts M. Metaprop: a Stata command to perform meta-analysis of binomial data. Arch Public Health. 2014;72:39.
Bander NH, Milowsky MI, Nanus DM, Kostakoglu L, Vallabhajosula S, Goldsmith SJ. Phase I trial of 177lutetium-labeled J591, a monoclonal antibody to prostate-specific membrane antigen, in patients with androgen-independent prostate cancer. J Clin Oncol. 2005;23:4591–601.
Tagawa ST, Milowsky MI, Morris M, Vallabhajosula S, Christos P, Akhtar NH, et al. Phase II study of Lutetium-177-labeled anti-prostate-specific membrane antigen monoclonal antibody J591 for metastatic castration-resistant prostate cancer. Clin Cancer Res. 2013;19:5182–91.
Heck MM, Retz M, D’Alessandria C, Rauscher I, Scheidhauer K, Maurer T, et al. Systemic Radioligand therapy with (177)Lu labeled prostate specific membrane antigen ligand for imaging and therapy in patients with metastatic castration resistant prostate cancer. J Urol. 2016;196:382–91.
Kratochwil C, Giesel FL, Stefanova M, Benesova M, Bronzel M, Afshar-Oromieh A, et al. PSMA-targeted radionuclide therapy of metastatic castration-resistant prostate cancer with 177Lu-labeled PSMA-617. J Nucl Med. 2016;57:1170–6.
Kulkarni HR, Singh A, Schuchardt C, Niepsch K, Sayeg M, Leshch Y, et al. PSMA-based Radioligand therapy for metastatic castration-resistant prostate cancer: the Bad Berka experience since 2013. J Nucl Med. 2016;57:97S–104S.
Ahmadzadehfar H, Wegen S, Yordanova A, Fimmers R, Kurpig S, Eppard E, et al. Overall survival and response pattern of castration-resistant metastatic prostate cancer to multiple cycles of radioligand therapy using [177Lu]Lu-PSMA-617. Eur J Nucl Med Mol Imaging. 2017;44:1448–54.
Brauer A, Grubert LS, Roll W, Schrader AJ, Schafers M, Bogemann M, et al. 177Lu-PSMA-617 radioligand therapy and outcome in patients with metastasized castration-resistant prostate cancer. Eur J Nucl Med Mol Imaging. 2017;44:1663–70.
Fendler WP, Reinhardt S, Ilhan H, Delker A, Boning G, Gildehaus FJ, et al. Preliminary experience with dosimetry, response and patient reported outcome after 177Lu-PSMA-617 therapy for metastatic castration-resistant prostate cancer. Oncotarget. 2017;8:3581–90.
Rahbar K, Ahmadzadehfar H, Kratochwil C, Haberkorn U, Schafers M, Essler M, et al. German multicenter study investigating 177Lu-PSMA-617 Radioligand therapy in advanced prostate cancer patients. J Nucl Med. 2017;58:85–90.
Rahbar K, Boegemann M, Yordanova A, Eveslage M, Schafers M, Essler M, et al. PSMA targeted radioligandtherapy in metastatic castration resistant prostate cancer after chemotherapy, abiraterone and/or enzalutamide. A retrospective analysis of overall survival. Eur J Nucl Med Mol Imaging. 2018;45:12–9.
Scarpa L, Buxbaum S, Kendler D, Fink K, Bektic J, Gruber L, et al. The 68Ga/177Lu theragnostic concept in PSMA targeting of castration-resistant prostate cancer: correlation of SUVmax values and absorbed dose estimates. Eur J Nucl Med Mol Imaging. 2017;44:788–800.
Yadav MP, Ballal S, Tripathi M, Damle NA, Sahoo RK, Seth A, et al. 177Lu-DKFZ-PSMA-617 therapy in metastatic castration resistant prostate cancer: safety, efficacy, and quality of life assessment. Eur J Nucl Med Mol Imaging. 2017;44:81–91.
Loriot Y, Bianchini D, Ileana E, Sandhu S, Patrikidou A, Pezaro C, et al. Antitumour activity of abiraterone acetate against metastatic castration-resistant prostate cancer progressing after docetaxel and enzalutamide (MDV3100). Ann Oncol. 2013;24:1807–12.
Noonan KL, North S, Bitting RL, Armstrong AJ, Ellard SL, Chi KN. Clinical activity of abiraterone acetate in patients with metastatic castration-resistant prostate cancer progressing after enzalutamide. Ann Oncol. 2013;24:1802–7.
Pezaro CJ, Omlin AG, Altavilla A, Lorente D, Ferraldeschi R, Bianchini D, et al. Activity of cabazitaxel in castration-resistant prostate cancer progressing after docetaxel and next-generation endocrine agents. Eur Urol. 2014;66:459–65.
Sella A, Sella T, Peer A, Berger R, Frank SJ, Gez E, et al. Activity of cabazitaxel after docetaxel and abiraterone acetate therapy in patients with castration-resistant prostate cancer. Clin Genitourin Cancer. 2014;12:428–32.
Al Nakouzi N, Le Moulec S, Albiges L, Wang C, Beuzeboc P, Gross-Goupil M, et al. Cabazitaxel remains active in patients progressing after docetaxel followed by novel androgen receptor pathway targeted therapies. Eur Urol. 2015;68:228–35.
Azad AA, Eigl BJ, Murray RN, Kollmannsberger C, Chi KN. Efficacy of enzalutamide following abiraterone acetate in chemotherapy-naive metastatic castration-resistant prostate cancer patients. Eur Urol. 2015;67:23–9.
Cheng HH, Gulati R, Azad A, Nadal R, Twardowski P, Vaishampayan UN, et al. Activity of enzalutamide in men with metastatic castration-resistant prostate cancer is affected by prior treatment with abiraterone and/or docetaxel. Prostate Cancer Prostatic Dis. 2015;18:122–7.
Sonpavde G, Bhor M, Hennessy D, Bhowmik D, Shen L, Nicacio L, et al. Sequencing of Cabazitaxel and Abiraterone acetate after docetaxel in metastatic castration-resistant prostate cancer: treatment patterns and clinical outcomes in multicenter community-based US oncology practices. Clin Genitourin Cancer. 2015;13:309–18.
Wissing MD, Coenen JL, van den Berg P, Westgeest HM, van den Eertwegh AJ, van Oort IM, et al. CAST: a retrospective analysis of cabazitaxel and abiraterone acetate sequential treatment in patients with metastatic castrate-resistant prostate cancer previously treated with docetaxel. Int J Cancer. 2015;136:E760–72.
Badrising SK, van der Noort V, van den Eertwegh AJ, Hamberg P, van Oort IM, van den Berg HP, et al. Prognostic parameters for response to enzalutamide after docetaxel and abiraterone treatment in metastatic castration-resistant prostate cancer patients; a possible time relation. Prostate. 2016;76:32–40.
Davies RS, Smith C, Lester JF. Third-line enzalutamide following docetaxel and Abiraterone in metastatic castrate-resistant prostate cancer. Anticancer Res. 2016;36:1799–803.
Kongsted P, Svane IM, Lindberg H, Bisbjerg R, Daugaard G, Sengelov L. Cabazitaxel as second-line or third-line therapy in patients with metastatic castration-resistant prostate cancer. Anti-Cancer Drugs. 2016;27:695–701.
Bando Y, Hinata N, Terakawa T, Furukawa J, Harada KI, Nakano Y, et al. Activity of cabazitaxel in patients with metastatic castration-resistant prostate cancer after treatment with single or dual regimens of novel androgen receptor-targeting agents. Med Oncol. 2017;34:163.
de Bono JS, Chowdhury S, Feyerabend S, Elliott T, Grande E, Melhem-Bertrandt A, et al. Antitumour activity and safety of enzalutamide in patients with metastatic castration-resistant prostate cancer previously treated with Abiraterone acetate plus prednisone for >/=24 weeks in Europe. Eur Urol 2017.
Emmett L, Willowson K, Violet J, Shin J, Blanksby A, Lee J. Lutetium 177 PSMA radionuclide therapy for men with prostate cancer: a review of the current literature and discussion of practical aspects of therapy. J Med Radiat Sci. 2017;64:52–60.
Fendler WP, Kratochwil C, Ahmadzadehfar H, Rahbar K, Baum RP, Schmidt M, et al. 177Lu-PSMA-617 therapy, dosimetry and follow-up in patients with metastatic castration-resistant prostate cancer. Nuklearmedizin. 2016;55:123–8.
Rathke H, Giesel FL, Flechsig P, Kopka K, Mier W, Hohenfellner M, et al. Repeated Lu-177-PSMA-617 radioligand therapy using treatment activities up to 9.3 GBq. J Nucl Med. 2017.
Eisenberger M, Hardy-Bessard AC, Kim CS, Geczi L, Ford D, Mourey L, et al. Phase III Study Comparing a Reduced Dose of Cabazitaxel (20 mg/m2) and the Currently Approved Dose (25 mg/m2) in Postdocetaxel Patients With Metastatic Castration-Resistant Prostate Cancer-PROSELICA. J Clin Oncol. 2017;135:3198–206.
Wei X, Schlenkhoff C, Schwarz B, Essler M, Ahmadzadehfar H. Combination of 177Lu-PSMA-617 and external radiotherapy for the treatment of cerebral metastases in patients with castration-resistant metastatic prostate cancer. Clin Nucl Med. 2017;42:704–6.
Fizazi K. Biennial report on genitourinary cancers. Eur J Cancer. 2016;66:125–30.
Estevez SV, Herranz UA, Calvo OF, Afonso Afonso FJ, Couto LS, Quintela ML, et al. Prostate cancer perspectives after chaarted: optimizing treatment sequence. Crit Rev Oncol Hematol. 2016;107:119–27.
Ryan CJ, Smith MR, de Bono JS, Molina A, Logothetis CJ, de Souza P, et al. Abiraterone in metastatic prostate cancer without previous chemotherapy. N Engl J Med. 2013;368:138–48.
Taplin ME, Armstrong AJ, Lin P, Krivoshik A, Phung, Parli T, et al. Clinical Outcomes of Chemotherapy-Naive Men with Metastatic Castration-Resistant Prostate Cancer and Low Baseline PSA Treated with Enzalutamide vs Placebo. J Urol. 2017;198:1324–32.
Fizazi K, Tran N, Fein L, Matsubara N, Rodriguez-Antolin A, Alekseev BY, et al. Abiraterone plus prednisone in metastatic, castration-sensitive prostate cancer. N Engl J Med. 2017;377:352–60.
Sweeney CJ, Chen YH, Carducci M, Liu G, Jarrard DF, Eisenberger M, et al. Chemohormonal therapy in metastatic hormone-sensitive prostate cancer. N Engl J Med. 2015;373:737–46.
Poorthuis MHF, Vernooij RWM, van Moorselaar RJA, de Reijke TM. First-line non-cytotoxic therapy in chemotherapy-naive patients with metastatic castration-resistant prostate cancer: a systematic review of 10 randomised clinical trials. BJU Int. 2017;119:831–45.
Funding
The review has no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest.
Ethical approval
All patients had given written informed consent to therapy and imaging studies. Apart from one article, this review does not analyze studies with human participants performed by any of the authors. One of the authors (IR) is co-author for the study by Scarpa et al. [47]. In that study, the application of 177Lu-PSMA-617 had been approved by the institutional tumor board, and the treatment with PSMA-617 RLT had followed all regulations of the Austrian Agency for Radiation Protection.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
von Eyben, F.E., Roviello, G., Kiljunen, T. et al. Third-line treatment and 177Lu-PSMA radioligand therapy of metastatic castration-resistant prostate cancer: a systematic review. Eur J Nucl Med Mol Imaging 45, 496–508 (2018). https://doi.org/10.1007/s00259-017-3895-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-017-3895-x