Abstract
Purpose
To evaluate the relationship between aortic inflammation as assessed by 18F–fluorodeoxyglucose-positron emission tomography (18F–FDG-PET) and features of plaque vulnerability as assessed by frequency domain-optical coherence tomography (FD-OCT).
Methods
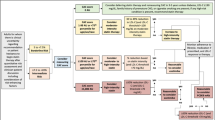
We enrolled 30 consecutive non-ST-segment elevation acute coronary syndrome patients undergoing percutaneous coronary intervention. All patients underwent three-vessel OCT before intervention and 18F–FDG-PET before discharge. Univariable and C-reactive protein (CRP)-adjusted linear regression analyses were performed between features of vulnerability [namely:lipid-rich plaques with and without macrophages and thin cap fibroatheromas (TCFA)] and 18F–FDG uptake in both ascending (AA) and descending aorta (DA) [measured either as averaged mean and maximum target-to-blood ratio (TBR) or as active slices (TBRmax ≥ 1.6)].
Results
Mean age was 62 years, and 26 patients were male. On univariable linear regression analysis TBRmean and TBRmax in DA was associated with the number of lipid-rich plaques (β = 4.22; 95%CI 0.05–8.39; p = 0.047 and β = 3.72; 95%CI 1.14–6.30; p = 0.006, respectively). TBRmax in DA was also associated with the number of lipid-rich plaques containing macrophages (β = 2.40; 95%CI 0.07–4.72; p = 0.044). A significant CRP adjusted linear association between the TBRmax in DA and the number of lipid-rich plaques was observed (CRP-adjusted β = 3.58; 95%CI -0.91-6.25; p = 0.01). TBRmax in DA showed a trend towards significant CRP-adjusted association with number of lipid-rich plaques with macrophages (CRP-adjusted β = 2.30; 95%CI -0.11-4.71; p = 0.06). We also observed a CRP-adjusted (β = 2.34; 95%CI 0.22–4.47; p = 0.031) linear association between the number of active slices in DA and the number of lipid-rich plaques. No relation was found between FDG uptake in the aorta and the number of TCFAs.
Conclusions
In patients with first NSTEACS, 18F–FDG uptake in DA is correlated with the number of OCT detected lipid-rich plaques with or without macrophages. This association may be independent from CRP values.





Similar content being viewed by others
References
Yusuf S, Reddy S, Ounpuu S, Anand S. Global burden of cardiovascular diseases: part II: variations in cardiovascular disease by specific ethnic groups and geographic regions and prevention strategies. Circulation. 2001;104:2855–64.
Virmani R, Burke AP, Farb A, Kolodgie FD. Pathology of the vulnerable plaque. J am Coll Cardiol. 2006;47:C13–8.
Virmani R, Kolodgie FD, Burke AP, Farb A, Schwartz SM. Lessons from sudden coronary death: a comprehensive morphological classification scheme for atherosclerotic lesions. Arterioscler Thromb Vasc Biol. 2000;20:1262–75.
Libby P. Inflammation in atherosclerosis. Nature. 2002;420:868–74.
Moreno PR, Falk E, Palacios IF, Newell JB, Fuster V, Fallon JT. Macrophage infiltration in acute coronary syndromes. Implications for plaque rupture. Circulation. 1994;90:775–8.
Rudd JH, Warburton EA, Fryer TD, et al. Imaging atherosclerotic plaque inflammation with [18F]-fluorodeoxyglucose positron emission tomography. Circulation. 2002;105:2708–11.
Rudd JH, Narula J, Strauss HW, et al. Imaging atherosclerotic plaque inflammation by fluorodeoxyglucose with positron emission tomography: ready for prime time? J am Coll Cardiol. 2010;55:2527–35.
Aziz K, Berger K, Claycombe K, Huang R, Patel R, Abela GS. Noninvasive detection and localization of vulnerable plaque and arterial thrombosis with computed tomography angiography/positron emission tomography. Circulation. 2008;117:2061–70.
Tatsumi M, Cohade C, Nakamoto Y, Wahl RL. Fluorodeoxyglucose uptake in the aortic wall at PET/CT: possible finding for active atherosclerosis. Radiology. 2003;229:831–7.
Tawakol A, Migrino RQ, Bashian GG, et al. In vivo 18F-fluorodeoxyglucose positron emission tomography imaging provides a noninvasive measure of carotid plaque inflammation in patients. J am Coll Cardiol. 2006;48:1818–24.
Menezes LJ, Kotze CW, Agu O, et al. Investigating vulnerable atheroma using combined (18)F-FDG PET/CT angiography of carotid plaque with immunohistochemical validation. J Nucl med. 2011;52:1698–703.
Rudd JH, Myers KS, Bansilal S, et al. (18)Fluorodeoxyglucose positron emission tomography imaging of atherosclerotic plaque inflammation is highly reproducible: implications for atherosclerosis therapy trials. J am Coll Cardiol. 2007;50:892–6.
Rudd JH, Myers KS, Bansilal S, et al. Relationships among regional arterial inflammation, calcification, risk factors, and biomarkers: a prospective fluorodeoxyglucose positron-emission tomography/computed tomography imaging study. Circ Cardiovasc Imaging. 2009;2:107–15.
Rogers IS, Nasir K, Figueroa AL, et al. Feasibility of FDG imaging of the coronary arteries: comparison between acute coronary syndrome and stable angina. JACC Cardiovasc Imaging. 2010;3:388–97.
Cheng VY, Slomka PJ, Le Meunier L, et al. Coronary arterial 18F-FDG uptake by fusion of PET and coronary CT angiography at sites of percutaneous stenting for acute myocardial infarction and stable coronary artery disease. J Nucl med. 2012;53:575–83.
Joshi NV, Vesey AT, Williams MC, et al. 18F-fluoride positron emission tomography for identification of ruptured and high-risk coronary atherosclerotic plaques: a prospective clinical trial. Lancet. 2014;383:705–13.
Yu S. Review of F-FDG synthesis and quality control. Biomed Imaging Interv J. 2006;2:e57.
Figueroa AL, Abdelbaky A, Truong QA, et al. Measurement of arterial activity on routine FDG PET/CT images improves prediction of risk of future CV events. JACC Cardiovasc Imaging. 2013;6:1250–9.
Prati F, Regar E, Mintz GS, et al. Expert review document on methodology, terminology, and clinical applications of optical coherence tomography: physical principles, methodology of image acquisition, and clinical application for assessment of coronary arteries and atherosclerosis. Eur Heart J. 2010;31:401–15.
Bucerius J, Mani V, Moncrieff C, et al. Optimizing 18F-FDG PET/CT imaging of vessel wall inflammation: the impact of 18F-FDG circulation time, injected dose, uptake parameters, and fasting blood glucose levels. Eur J Nucl med Mol Imaging. 2014;41:369–83.
Otsuka F, Joner M, Prati F, Virmani R, Narula J. Clinical classification of plaque morphology in coronary disease. Nat rev Cardiol. 2014;11:379–89.
Tearney GJ, Regar E, Akasaka T, et al. Consensus standards for acquisition, measurement, and reporting of intravascular optical coherence tomography studies: a report from the international working Group for Intravascular Optical Coherence Tomography Standardization and Validation. J am Coll Cardiol. 2012;59:1058–72.
Di Vito L, Agozzino M, Marco V, et al. Identification and quantification of macrophage presence in coronary atherosclerotic plaques by optical coherence tomography. Eur Heart J Cardiovasc Imaging. 2015;16:807–13.
Wykrzykowska J, Lehman S, Williams G, et al. Imaging of inflamed and vulnerable plaque in coronary arteries with 18F-FDG PET/CT in patients with suppression of myocardial uptake using a low-carbohydrate, high-fat preparation. J Nucl med. 2009;50:563–8.
Bucerius J, Hyafil F, Verberne HJ, et al. Position paper of the cardiovascular Committee of the European Association of nuclear medicine (EANM) on PET imaging of atherosclerosis. Eur J Nucl med Mol Imaging. 2016;43:780–92.
Tahara N, Kai H, Ishibashi M, et al. Simvastatin attenuates plaque inflammation: evaluation by fluorodeoxyglucose positron emission tomography. J am Coll Cardiol. 2006;48:1825–31.
Elkhawad M, Rudd JH, Sarov-Blat L, et al. Effects of p38 mitogen-activated protein kinase inhibition on vascular and systemic inflammation in patients with atherosclerosis. JACC Cardiovasc Imaging. 2012;5:911–22.
Marzocchi A, Taglieri N, Saia F, et al. Incidence, treatment and outcome of acute coronary syndromes: a community-based study in the era of myocardial infarction networks. Int J Cardiol. 2012;157:419–22.
Fox KA, Poole-Wilson P, Clayton TC, et al. 5-year outcome of an interventional strategy in non-ST-elevation acute coronary syndrome: the British Heart Foundation RITA 3 randomised trial. Lancet. 2005;366:914–20.
Stone JR, Bruneval P, Angelini A, et al. Consensus statement on surgical pathology of the aorta from the Society for Cardiovascular Pathology and the Association for European Cardiovascular Pathology: I. Inflammatory diseases. Cardiovasc Pathol. 2015;24:267–78.
Hattori K, Ozaki Y, Ismail TF, et al. Impact of statin therapy on plaque characteristics as assessed by serial OCT, grayscale and integrated backscatter-IVUS. JACC Cardiovasc Imaging. 2012;5:169–77.
Stone GW, Maehara A, Lansky AJ, et al. A prospective natural-history study of coronary atherosclerosis. N Engl J med. 2011;364:226–35.
Tian J, Ren X, Vergallo R, et al. Distinct morphological features of ruptured culprit plaque for acute coronary events compared to those with silent rupture and thin-cap fibroatheroma: a combined optical coherence tomography and intravascular ultrasound study. J am Coll Cardiol. 2014;63:2209–16.
Oh M, Lee CW, Lee HS, et al. Similar impact of Clopidogrel or Ticagrelor on carotid atherosclerotic plaque inflammation. Clin Cardiol. 2016;39:646–52.
Su B, Xu B, Wan J. Correlation between long-term aspirin use and F-fluorodeoxyglucose uptake in colorectal cancer measured by PET/CT. PLoS One. 2014;9:e109459.
Scholtens AM, Verberne HJ, Budde RP, Lam MG. Additional heparin Preadministration improves cardiac glucose metabolism suppression over low-carbohydrate Diet alone in (1)(8)F-FDG PET imaging. J Nucl med. 2016;57:568–73.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Funding
This work was supported by Department of Experimental, Diagnostic and Speciality Medicine - DIMES, University of Bologna and by Fanti Melloni Foundation (grant number = not applicable).
Conflict of interest
F.P. is a consultant for ST. Jude Medical. The remaining authors have no conflicts of interest to declare.
Ethical approval
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Table S1
(DOCX 13 kb)
Rights and permissions
About this article
Cite this article
Taglieri, N., Nanni, C., Ghetti, G. et al. Relation between thoracic aortic inflammation and features of plaque vulnerability in the coronary tree in patients with non-ST-segment elevation acute coronary syndrome undergoing percutaneous coronary intervention. An FDG-positron emission tomography and optical coherence tomography study. Eur J Nucl Med Mol Imaging 44, 1878–1887 (2017). https://doi.org/10.1007/s00259-017-3747-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-017-3747-8