Abstract
Purpose
F-FDOPA is a highly sensitive and specific radiopharmaceutical for pheochromocytoma and paraganglioma (PPGL) imaging. However, 18F-FDOPA might be falsely negative in these tumors, especially those related to mutations in succinate dehydrogenase genes (SDHx). The aim of the present study was to evaluate the relationship between expression of L-DOPA transporters and 18F-FDOPA PET imaging results in PPGL.
Methods
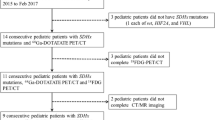
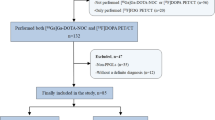
From 2007 to 2015, 175 patients with non-metastatic PPGL were evaluated by 18F-FDOPA PET/CT for initial diagnosis/staging and follow-up. 18F-FDOPA PET/CT was considered as falsely negative for at least one lesion in 10/126 (8%) patients (two sporadic, six SDHD, two SDHB PPGLs). The mRNA and protein expression levels of CD98hc and LATs were evaluated in samples with different genetic backgrounds and imaging phenotypes. The qRT-PCR and immunohistochemical analyses were performed in 14 and 16 tumor samples, respectively.
Results
The SDHx mutated samples exhibited a significant decrease in mRNA expression of LAT3 when compared to sporadic PPGLs (P = 0.042). There was also a statistical trend toward decreased CD98hc (P = 0.147) and LAT4 (P = 0.012) levels in SDHx vs sporadic PPGLs. No difference was observed for LAT1/LAT2 mRNA levels. LAT1 protein was expressed in 15 out of 16 (93.75%) SDHx tumors, regardless of the 18F-FDOPA positivity. LAT1 and CD98hc were co-expressed in 6/8 18F-FDOPA-negative PPGLs. In contrast, in one case with absence of LAT1/CD98hc, 18F-FDOPA uptake was positive and attributed to LAT4 expression.
Conclusions
We conclude that down-regulation of LAT1/CD98hc cannot explain the imaging phenotype of SDHx-related PPGLs. A reduced activity of LAT1 remains the primary hypothesis possibly due to a modification of intracellular amino acid content which may reduce 18F-FDOPA uptake.





Similar content being viewed by others
References
Imperiale A, Moussallieh FM, Roche P, Battini S, Cicek AE, Sebag F, et al. Metabolome Profiling by HRMAS NMR Spectroscopy of Pheochromocytomas and Paragangliomas Detects SDH Deficiency: Clinical and Pathophysiological Implications. Neoplasia. 2015;17:55–65. doi:10.1016/j.neo.2014.10.010.
Imperiale A, Moussallieh FM, Sebag F, Brunaud L, Barlier A, Elbayed K, et al. A new specific succinate-glutamate metabolomic hallmark in SDHx-related paragangliomas. PLoS One. 2013;8:e80539. doi:10.1371/journal.pone.0080539.
Lendvai N, Pawlosky R, Bullova P, Eisenhofer G, Patocs A, Veech RL, et al. Succinate-to-fumarate ratio as a new metabolic marker to detect the presence of SDHB/D-related paraganglioma: initial experimental and ex vivo findings. Endocrinology. 2014;155:27–32. doi:10.1210/en.2013-1549.
Richter S, Peitzsch M, Rapizzi E, Lenders JW, Qin N, de Cubas AA, et al. Krebs cycle metabolite profiling for identification and stratification of pheochromocytomas/paragangliomas due to succinate dehydrogenase deficiency. J Clin Endocrinol Metab. 2014;99:3903–11. doi:10.1210/jc.2014-2151.
Timmers HJ, Chen CC, Carrasquillo JA, Whatley M, Ling A, Havekes B, et al. Comparison of 18F-Fluoro-L-DOPA, 18F-Fluoro-Deoxyglucose, and 18F-Fluorodopamine PET and 123I-MIBG Scintigraphy in the Localization of Pheochromocytoma and Paraganglioma. J Clin Endocrinol Metab. 2009;94:4757–67.
Timmers HJ, Chen CC, Carrasquillo JA, Whatley M, Ling A, Eisenhofer G, et al. Staging and functional characterization of pheochromocytoma and paraganglioma by 18F-fluorodeoxyglucose (18F-FDG) positron emission tomography. J Natl Cancer Inst. 2012;104:700–8. doi:10.1093/jnci/djs188.
Taieb D, Sebag F, Barlier A, Tessonnier L, Palazzo FF, Morange I, et al. 18F-FDG avidity of pheochromocytomas and paragangliomas: a new molecular imaging signature? J Nucl Med. 2009;50:711–7. doi:10.2967/jnumed.108.060731.
Treglia G, Cocciolillo F, de Waure C, Di Nardo F, Gualano MR, Castaldi P, et al. Diagnostic performance of 18F-dihydroxyphenylalanine positron emission tomography in patients with paraganglioma: a meta-analysis. Eur J Nucl Med Mol Imaging. 2012;39:1144–53. doi:10.1007/s00259-012-2087-y.
Gabriel S, Blanchet EM, Sebag F, Chen CC, Fakhry N, Deveze A, et al. Functional characterization of nonmetastatic paraganglioma and pheochromocytoma by (18) F-FDOPA PET: focus on missed lesions. Clin Endocrinol. 2013;79:170–7. doi:10.1111/cen.12126.
Haase C, Bergmann R, Fuechtner F, Hoepping A, Pietzsch J. L-type amino acid transporters LAT1 and LAT4 in cancer: uptake of 3-O-methyl-6-18F-fluoro-L-dopa in human adenocarcinoma and squamous cell carcinoma in vitro and in vivo. J Nucl Med. 2007;48:2063–71. doi:10.2967/jnumed.107.043620.
Beyer SR, Mallmann RT, Jaenecke I, Habermeier A, Boissel JP, Closs EI. Identification of cysteine residues in human cationic amino acid transporter hCAT-2A that are targets for inhibition by N-ethylmaleimide. J Biol Chem. 2013;288:30411–9. doi:10.1074/jbc.M113.490698.
Taieb D, Imperiale A, Pacak K. (18)F-DOPA: the versatile radiopharmaceutical. Eur J Nucl Med Mol Imaging. 2016;43:1187–9. doi:10.1007/s00259-016-3354-0.
Archier A, Varoquaux A, Garrigue P, Montava M, Guerin C, Gabriel S, et al. Prospective comparison of Ga-DOTATATE and F-FDOPA PET/CT in patients with various pheochromocytomas and paragangliomas with emphasis on sporadic cases. Eur J Nucl Med Mol Imaging. 2015. doi:10.1007/s00259-015-3268-2.
Papin-Michault C, Bonnetaud C, Dufour M, Almairac F, Coutts M, Patouraux S, et al. Study of LAT1 expression in brain metastases: towards a better understanding of the results of positron emission tomography using amino acid tracers. PLoS One. 2016;11:e0157139. doi:10.1371/journal.pone.0157139.
Broer S. Amino acid transport across mammalian intestinal and renal epithelia. Physiol Rev. 2008;88:249–86. doi:10.1152/physrev.00018.2006.
Hyde R, Taylor PM, Hundal HS. Amino acid transporters: roles in amino acid sensing and signalling in animal cells. Biochem J. 2003;373:1–18.
Schioth HB, Roshanbin S, Hagglund MG, Fredriksson R. Evolutionary origin of amino acid transporter families SLC32, SLC36 and SLC38 and physiological, pathological and therapeutic aspects. Mol Asp Med. 2013;34:571–85. doi:10.1016/j.mam.2012.07.012.
Broer S. Targeting tumour cells at the entrance. Biochem J. 2011;439:e1–2. doi:10.1042/BJ20111484.
Broer S, Palacin M. The role of amino acid transporters in inherited and acquired diseases. Biochem J. 2011;436:193–211. doi:10.1042/BJ20101912.
Barollo S, Bertazza L, Watutantrige-Fernando S, Censi S, Cavedon E, Galuppini F, et al. Overexpression of L-type amino acid transporter 1 (LAT1) and 2 (LAT2): novel markers of neuroendocrine tumors. PLoS One. 2016;11:e0156044. doi:10.1371/journal.pone.0156044.
Lussey-Lepoutre C, Hollinshead KE, Ludwig C, Menara M, Morin A, Castro-Vega LJ, et al. Loss of succinate dehydrogenase activity results in dependency on pyruvate carboxylation for cellular anabolism. Nat Commun. 2015;6:8784. doi:10.1038/ncomms9784.
Soares-da-Silva P, Serrao MP. High- and low-affinity transport of L-leucine and L-DOPA by the hetero amino acid exchangers LAT1 and LAT2 in LLC-PK1 renal cells. Am J Physiol Renal Physiol. 2004;287:F252–61. doi:10.1152/ajprenal.00030.2004.
Kruger GM, Mosher JT, Bixby S, Joseph N, Iwashita T, Morrison SJ. Neural crest stem cells persist in the adult gut but undergo changes in self-renewal, neuronal subtype potential, and factor responsiveness. Neuron. 2002;35:657–69.
Cantor JM, Ginsberg MH. CD98 at the crossroads of adaptive immunity and cancer. J Cell Sci. 2012;125:1373–82. doi:10.1242/jcs.096040.
de la Ballina LR, Cano-Crespo S, Gonzalez-Munoz E, Bial S, Estrach S, Cailleteau L, et al. Amino acid transport associated to cluster of differentiation 98 heavy chain (CD98hc) is at the cross-road of oxidative stress and amino acid availability. J Biol Chem. 2016;291:9700–11. doi:10.1074/jbc.M115.704254.
Letouze E, Martinelli C, Loriot C, Burnichon N, Abermil N, Ottolenghi C, et al. SDH mutations establish a hypermethylator phenotype in paraganglioma. Cancer Cell. 2013;23:739–52. doi:10.1016/j.ccr.2013.04.018.
Feral CC, Nishiya N, Fenczik CA, Stuhlmann H, Slepak M, Ginsberg MH. CD98hc (SLC3A2) mediates integrin signaling. Proc Natl Acad Sci U S A. 2005;102:355–60. doi:10.1073/pnas.0404852102.
Prager GW, Feral CC, Kim C, Han J, Ginsberg MH. CD98hc (SLC3A2) interaction with the integrin beta subunit cytoplasmic domain mediates adhesive signaling. J Biol Chem. 2007;282:24477–84. doi:10.1074/jbc.M702877200.
Feral CC, Zijlstra A, Tkachenko E, Prager G, Gardel ML, Slepak M, et al. CD98hc (SLC3A2) participates in fibronectin matrix assembly by mediating integrin signaling. J Cell Biol. 2007;178:701–11. doi:10.1083/jcb.200705090.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The review did not receive any specific grant from any funding agency in the public, commercial, or not-for-profit sector.
Disclosure of potential conflicts of interest
The authors have nothing to disclose.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Feral, C.C., Tissot, F.S., Tosello, L. et al. 18F-fluorodihydroxyphenylalanine PET/CT in pheochromocytoma and paraganglioma: relation to genotype and amino acid transport system L. Eur J Nucl Med Mol Imaging 44, 812–821 (2017). https://doi.org/10.1007/s00259-016-3586-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-016-3586-z