Abstract
Background
Managing recurrent shoulder instability in an athlete of any age is challenging. The pediatric literature regarding recurrence of instability is difficult to interpret because of the variable treatment protocols and varying ages. The adult literature suggests that bone loss on the humerus, glenoid or both, as detected by CT, has high rates of recurrence following surgical intervention.
Objective
The purpose of this study was to evaluate risk factors for recurrence following arthroscopic capsulorrhaphy in adolescent athletes using preoperative MR arthrograms.
Materials and methods
We reviewed a retrospective shoulder instability database for adolescents (age ≤18 years), who underwent an isolated arthroscopic capsulorrhaphy from 2006 to 2011. We recorded preoperative MRI measurements regarding the dimensions of the glenohumeral joint, as well as glenoid, humeral and labral pathologies. We performed statistical analysis to determine MRI findings that might have predicted recurrence of shoulder instability following capsulorrhaphy.
Results
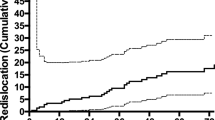
We reviewed a total of 50 patients (13–18 years) and found 22 patients (44%) to have recurrent instability following capsulorrhaphy. Presence of glenoid bone loss or a bipolar bone lesion (defined as bone loss on both the glenoid and humerus) significantly predicted recurrence of shoulder instability (both P=0.03). There was not a threshold size of glenoid bone loss or bipolar lesion that predicted recurrence. All remaining glenohumeral dimensions or presence or size of an isolated Hill-Sachs did not significantly predict recurrence of instability.
Conclusion
Athletes ≤18 years old have a high rate of failure following arthroscopic capsulorrhaphy in the presence of glenoid bone loss or a bipolar lesion on MRI. Surgeons should consider addressing these lesions in adolescent athletes with shoulder instability. Additionally, MRI is a valid imaging tool to diagnose and measure osseous lesions of the shoulder.


Similar content being viewed by others
References
Bottoni CR, Wilckens JH, DeBerardino TM et al (2002) A prospective, randomized evaluation of arthroscopic stabilization versus nonoperative treatment in patients with acute, traumatic, first-time shoulder dislocations. Am J Sports Med 30:576–580
Kirkley A, Werstine R, Ratjek A, Griffin S (2005) Prospective randomized clinical trial comparing the effectiveness of immediate arthroscopic stabilization versus immobilization and rehabilitation in first traumatic anterior dislocations of the shoulder: long-term evaluation. Arthroscopy 21:55–63
Cordischi K, Li X, Busconi B (2009) Intermediate outcomes after primary traumatic anterior shoulder dislocation in skeletally immature patients aged 10 to 13 years. Orthopedics. https://doi.org/10.3928/01477447-20090728-34
Deitch J, Mehlman CT, Foad SL et al (2003) Traumatic anterior shoulder dislocation in adolescents. Am J Sports Med 31:758–763
Wagner KT, Lyne ED (1983) Adolescent traumatic dislocations of the shoulder with open epiphyses. J Pediatr Orthop 3:61–62
Postacchini F, Gumina S, Cinotti G (2000) Anterior shoulder dislocation in adolescents. J Shoulder Elb Surg 9:470–474
Marans HJ, Angel KR, Schemitsch EH, Wedge JH (1992) The fate of traumatic anterior dislocation of the shoulder in children. J Bone Joint Surg Am 74:1242–1244
Baumgartner G, Slongo T, Kohler G et al (2003) Traumatic shoulder dislocation in children and adolescents. Eur J Trauma 29:375–378
Olds M, Ellis R, Donaldson K et al (2015) Risk factors which predispose first-time traumatic anterior shoulder dislocations to recurrent instability in adults: a systematic review and meta-analysis. Br J Sports Med 49:913–922
Jones KJ, Wiesel B, Ganley TJ, Wells L (2007) Functional outcomes of early arthroscopic Bankart repair in adolescents aged 11 to 18 years. J Pediatr Orthop 27:209–213
Heyworth BE, Kocher MS (2013) Shoulder instability in the young athlete. AAOS Instr Course Lect 62:435–444
Boileau P, Villalba M, Héry JY et al (2006) Risk factors for recurrence of shoulder instability after arthroscopic Bankart repair. J Bone Joint Surg Am 88:1755–1763
Park MJ, Tjoumakaris FP, Garcia G et al (2011) Arthroscopic remplissage with Bankart repair for the treatment of glenohumeral instability with Hill-Sachs defects. Arthroscopy 27:1187–1194
Di Giacomo G, Itoi E, Burkhart SS (2014) Evolving concept of bipolar bone loss and the Hill-Sachs lesion: from “engaging/non-engaging” lesion to “on-track/off-track” lesion. Arthroscopy 30:90–98
McNeil JW, Beaulieu-Jones BR, Bernhardson AS et al (2017) Classification and analysis of attritional glenoid bone loss in recurrent anterior shoulder instability. Am J Sports Med 45:767–774
Saliken DJ, Bornes TD, Bouliane MJ et al (2015) Imaging methods for quantifying glenoid and Hill-Sachs bone loss in traumatic instability of the shoulder: a scoping review. BMC Musculoskelet Disord 16:164
Friedman RJ, Black J, Galante JO et al (1994) Current concepts in orthopaedic biomaterials and implant fixation. Instr Course Lect 43:233–255
Cohen J (1960) A coefficient of agreement for nominal scales. Educ Psychol Meas 20:37–46
Kim S-H, Ha K-I, Cho Y-B et al (2003) Arthroscopic anterior stabilization of the shoulder: two to six-year follow-up. J Bone Joint Surg Am 85:1511–1518
Burkhart SS, De Beer JF (2000) Traumatic glenohumeral bone defects and their relationship to failure of arthroscopic Bankart repairs: significance of the inverted-pear glenoid and the humeral engaging Hill-Sachs lesion. Arthroscopy 16:677–694
Hartzler RU, Bui CNH, Jeong WK et al (2016) Remplissage of an off-track Hill-Sachs lesion is necessary to restore biomechanical glenohumeral joint stability in a bipolar bone loss model. Arthroscopy 32:2466–2476
Gyftopoulos S, Hasan S, Bencardino J et al (2012) Diagnostic accuracy of MRI in the measurement of glenoid bone loss. AJR Am J Roentgenol 199:873–878
Gyftopoulos S, Beltran LS, Bookman J, Rokito A (2015) MRI evaluation of bipolar bone loss using the on-track off-track method: a feasibility study. AJR Am J Roentgenol 205:848–852
Caprise PA, Sekiya JK (2006) Open and arthroscopic treatment of multidirectional instability of the shoulder. Arthroscopy 22:1126–1131
Rockwood C, Matsen F (2009) The shoulder, 4th edn. Saunders/Elsevier, Philadelphia
Walton J, Paxinos A, Tzannes A et al (2002) The unstable shoulder in the adolescent athlete. Am J Sports Med 30:758–767
Yiannakopoulos CK, Mataragas E, Antonogiannakis E (2007) A comparison of the spectrum of intra-articular lesions in acute and chronic anterior shoulder instability. Arthroscopy 23:985–990
Robinson CM, Howes J, Murdoch H et al (2006) Functional outcome and risk of recurrent instability after primary traumatic anterior shoulder dislocation in young patients. J Bone Joint Surg Am 88:2326–2336
Ellis HB, Seiter M, Wise K, Wilson P (2017) Glenoid bone loss in traumatic glenohumeral instability in the adolescent population. J Pediatr Orthop 37:30–35
Lau BC, Conway D, Curran PF et al (2017) Bipolar bone loss in patients with anterior shoulder dislocation: a comparison of adolescents versus adult patients. Arthroscopy 33:1755–1761
Olds M, Donaldson K, Ellis R, Kersten P (2016) In children 18 years and under, what promotes recurrent shoulder instability after traumatic anterior shoulder dislocation? A systematic review and meta-analysis of risk factors. Br J Sports Med 50:1135–1141
Brody AS, Frush DP, Huda W, Brent RL (2007) American Academy of Pediatrics Section on Radiology. Radiation risk to children from computed tomography. Pediatrics 120:677–682
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Hughes, J.L., Kruk, P., Bastrom, T.P. et al. Magnetic resonance imaging predictors of shoulder instability in adolescents. Pediatr Radiol 49, 365–371 (2019). https://doi.org/10.1007/s00247-018-4318-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-4318-2