Abstract
Background
The imaging features of Huntington disease are well known in adults, unlike in juvenile-onset Huntington disease.
Objective
To conduct a morphometric magnetic resonance imaging (MRI) analysis in three juvenile Huntington disease patients (ages 2, 4 and 6 years old) to determine whether quantitative cerebral and cerebellar morphological metrics may provide diagnostically interesting patterns of cerebellar and cerebellar atrophy.
Materials and methods
We report the cases of three siblings with extremely early presentations of juvenile Huntington disease associated with dramatic expansions of the morbid paternal allele from 43 to more than 100 CAG trinucleotide repeats. Automatic segmentation of MRI images of the cerebrum and cerebellum was performed and volumes of cerebral substructures and cerebellar lobules of juvenile Huntington disease patients were compared to those of 30 normal gender- and age-matched controls. Juvenile Huntington disease segmented volumes were compared to those of age-matched controls by using a z-score.
Results
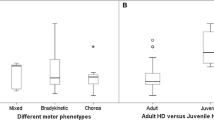
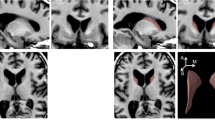
Three cerebral substructures (caudate nucleus, putamen and globus pallidus) demonstrated a reduction in size of more than three standard deviations from the normal mean although it was not salient in one of them at clinical reading and was not diagnosed. The size of cerebellum lobules, cerebellum grey matter and cerebellum cortex was reduced by more than two standard deviations in the three patients. The cerebellar atrophy was predominant in the posterior lobe.
Conclusion
Our study sheds light on atrophic cerebral and cerebellar structures in juvenile Huntington disease. Automatic segmentations of the cerebellum provide patterns that may be of diagnostic interest in this disease.




Similar content being viewed by others
References
Gómez-Tortosa E, del Barrio A, García Ruiz PJ et al (1998) Severity of cognitive impairment in juvenile and late-onset Huntington disease. Arch Neurol 55:835–843
Nicolas G, Devys D, Goldenberg A et al (2011) Juvenile Huntington disease in an 18-month-old boy revealed by global developmental delay and reduced cerebellar volume. Am J Med Genet A 155A:815–818
Letort D, Gonzalez-Alegre P (2013) Huntington’s disease in children. Handb Clin Neurol 113:1913–1917
Montoya A, Price BH, Menear M et al (2006) Brain imaging and cognitive dysfunctions in Huntington’s disease. J Psychiatry Neurosci 31:21–29
Ho VB, Chuang HS, Rovira MJ et al (1995) Juvenile Huntington disease: CT and MR features. AJNR Am J Neuroradiol 16:1405–1412
Schapiro M, Cecil KM, Doescher J et al (2004) MR imaging and spectroscopy in juvenile Huntington disease. Pediatr Radiol 34:640–643
Fennema-Notestine C, Archibald SL, Jacobson MW et al (2004) In vivo evidence of cerebellar atrophy and cerebral white matter loss in Huntington disease. Neurology 63:989–995
Kassubek J, Gaus W, Landwehrmeyer GB (2004) Evidence for more widespread cerebral pathology in early HD: an MRI-based morphometric analysis. Neurology 62:523–524
Rüb U, Hoche F, Brunt ER et al (2013) Degeneration of the cerebellum in Huntington’s disease (HD): possible relevance for the clinical picture and potential gateway to pathological mechanisms of the disease process. Brain Pathol 23(2):165–177
Diedrichsen J (2006) A spatially unbiased atlas template of the human cerebellum. Neuroimage 33:127–138
Narayanan PL, Warton C, Rosella Boonzaier N et al (2016) Improved segmentation of cerebellar structures in children. J Neurosci Methods 262:1–13
Focke NK, Trost S, Paulus W et al (2014) Do manual and voxel-based morphometry measure the same? A proof of concept study. Front Psychiatry 5:39
Manjón JV, Coupé P (2016) volBrain: an online MRI brain volumetry system. Front Neuroinform 10:30
Romero JE, Coupé P, Giraud R et al (2017) CERES: a new cerebellum lobule segmentation method. Neuroimage 147:916–924
Ashburner J, Friston KJ (2005) Unified segmentation. Neuroimage 26:839–851
Eskildsen SF, Coupé P, Fonov V et al (2012) BEaST: brain extraction based on nonlocal segmentation technique. Neuroimage 59:2362–2373
Romero JE, Manjón JV, Tohka J et al (2015) NABS: non-local automatic brain hemisphere segmentation. Magn Reson Imaging 33:474–484
Warner JP, Barron LH, Brock DJ (1993) A new polymerase chain reaction (PCR) assay for the trinucleotide repeat that is unstable and expanded on Huntington’s disease chromosomes. Mol Cell Probes 7:235–239
(1993) A novel gene containing a trinucleotide repeat that is expanded and unstable on Huntington’s disease chromosomes. The Huntington’s Disease Collaborative Research Group. Cell 72:971–983
Ranen NG, Stine OC, Abbott MH et al (1995) Anticipation and instability of IT-15 (CAG)n repeats in parent-offspring pairs with Huntington disease. Am J Hum Genet 57:593–602
Moser AD, Epping E, Espe-Pfeifer P, Martin E, Zhorne L, Mathews K et al (2017) A survey-based study identifies common but unrecognized symptoms in a large series of juvenile Huntington’s disease. Neurodegener Dis Manag 7:307–315
Ribaï P, Nguyen K, Hahn-Barma V et al (2007) Psychiatric and cognitive difficulties as indicators of juvenile huntington disease onset in 29 patients. Arch Neurol 64:813–819
Yoon G, Kramer J, Zanko A et al (2006) Speech and language delay are early manifestations of juvenile-onset Huntington disease. Neurology 67:1265–1267
Cloud LJ, Rosenblatt A, Margolis RL et al (2012) Seizures in juvenile Huntington’s disease: frequency and characterization in a multicenter cohort. Mov Disord 27:1797–1800
Aziz NA, van der Burg JMM, Landwehrmeyer GB et al (2008) Weight loss in Huntington disease increases with higher CAG repeat number. Neurology 71:1506–1513
Fusar-Poli P, Radua J, Frascarelli M et al (2014) Evidence of reporting biases in voxel-based morphometry (VBM) studies of psychiatric and neurological disorders. Hum Brain Mapp 35:3052–3065
Kühn S, Romanowski A, Schubert F et al (2012) Reduction of cerebellar grey matter in Crus I and II in schizophrenia. Brain Struct Funct 217:523–529
Harris GJ, Pearlson GD, Peyser CE et al (1992) Putamen volume reduction on magnetic resonance imaging exceeds caudate changes in mild Huntington’s disease. Ann Neurol 31:69–75
Aylward EH, Brandt J, Codori AM et al (1994) Reduced basal ganglia volume associated with the gene for Huntington’s disease in asymptomatic at-risk persons. Neurology 44:823–828
Aggleton JP, Mishkin M (1986) The amygdala: Sensory gateway to the emotions. In: Plutchik R, Kellerman H (eds) Biological foundations of emotion. Academic Press, New York, p 281–299
Anderson AK, Phelps EA (2001) Lesions of the human amygdala impair enhanced perception of emotionally salient events. Nature 411:305–309
Lange KW, Sahakian BJ, Quinn NP et al (1995) Comparison of executive and visuospatial memory function in Huntington’s disease and dementia of Alzheimer type matched for degree of dementia. J Neurol Neurosurg Psychiatry 58:598–606
Lawrence AD, Sahakian BJ, Hodges JR et al (1996) Executive and mnemonic functions in early Huntington’s disease. Brain J Neurol 119(Pt 5):1633–1645
Bollen E, Reulen JP, Den Heyer JC et al (1986) Horizontal and vertical saccadic eye movement abnormalities in Huntington’s chorea. J Neurol Sci 74:11–22
Hansotia P, Wall R, Berendes J (1985) Sleep disturbances and severity of Huntington’s disease. Neurology 35:1672–1674
Jeste DV, Barban L, Parisi J (1984) Reduced Purkinje cell density in Huntington’s disease. Exp Neurol 85:78–86
Rodda RA (1981) Cerebellar atrophy in Huntington’s disease. J Neurol Sci 50:147–157
Vinken P, Bruyn G (1987) Extrapyramidal disorders. Elsevier Science Health Science Division, Amsterdam
Rosas HD, Koroshetz WJ, Chen YI et al (2003) Evidence for more widespread cerebral pathology in early HD: an MRI-based morphometric analysis. Neurology 60:1615–1620
Vonsattel JP, DiFiglia M (1998) Huntington disease. J Neuropathol Exp Neurol 57:369–384
Vonsattel JP, Myers RH, Stevens TJ et al (1985) Neuropathological classification of Huntington’s disease. J Neuropathol Exp Neurol 44:559–577
Rees EM, Farmer R, Cole JH et al (2014) Cerebellar abnormalities in Huntington’s disease: a role in motor and psychiatric impairment? Mov Disord 29:1648–1654
Harper PS (1991) Huntington’s disease. WB Saunders, Philadelphia, p 1–15
Jervis GA (1963) Huntington’s chorea in childhood. Arch Neurol 9:244–257
Markham CH, Knox JW (1965) Observations on Huntington’s chorea in childhood. J Pediatr 67:46–57
Byers RK, Gilles FH, Fung C (1973) Huntington’s disease in children. Neuropathologic study of four cases. Neurology 23:561–569
Vonsattel JPG, Keller C, Cortes Ramirez EP (2011) Huntington’s disease - neuropathology. Handb Clin Neurol 100:83–100
Rasmussen A, Macias R, Yescas P et al (2000) Huntington disease in children: genotype-phenotype correlation. Neuropediatrics 31:190–194
Gencik M, Hammans C, Strehl H et al (2002) Chorea Huntington: a rare case with childhood onset. Neuropediatrics 33:90–92
Milunsky JM, Maher TA, Loose BA et al (2003) XL PCR for the detection of large trinucleotide expansions in juvenile Huntington’s disease. Clin Genet 64:70–73
Nahhas FA, Garbern J, Krajewski KM et al (2005) Juvenile onset Huntington disease resulting from a very large maternal expansion. Am J Med Genet A 137A:328–331
Seneca S, Fagnart D, Keymolen K et al (2004) Early onset Huntington disease: a neuronal degeneration syndrome. Eur J Pediatr 163:717–721
Sakazume S, Yoshinari S, Oguma E et al (2009) A patient with early onset Huntington disease and severe cerebellar atrophy. Am J Med Genet A 149A:598–601
Fyfe I (2016) Dementia: cerebellar atrophy has disease-specific patterns. Nat Rev Neurol 12:188
Crooks R, Mitchell T, Thom M (2000) Patterns of cerebellar atrophy in patients with chronic epilepsy: a quantitative neuropathological study. Epilepsy Res 41:63–73
Hagemann G, Lemieux L, Free SL et al (2002) Cerebellar volumes in newly diagnosed and chronic epilepsy. J Neurol 249:1651–1658
Guo CC, Tan R, Hodges JR et al (2016) Network-selective vulnerability of the human cerebellum to Alzheimer’s disease and frontotemporal dementia. Brain J Neurol 139:1527–1538
Deckel AW (1995) Is Huntington’s disease of cerebellar/brainstem origin? Lancet 345:263–264
Squitieri F, Pustorino G, Cannella M et al (2003) Highly disabling cerebellar presentation in Huntington disease. Eur J Neurol 10:443–444
Acknowledgments
The authors thank Nikki Sabourin-Gibbs of Rouen University Hospital for editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Electronic supplementary material
ESM 1
(DOCX 17 kb)
Rights and permissions
About this article
Cite this article
Hedjoudje, A., Nicolas, G., Goldenberg, A. et al. Morphological features in juvenile Huntington disease associated with cerebellar atrophy — magnetic resonance imaging morphometric analysis. Pediatr Radiol 48, 1463–1471 (2018). https://doi.org/10.1007/s00247-018-4167-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-4167-z