Abstract
Background
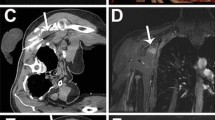
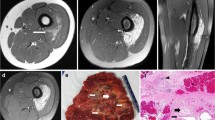
Fibro-adipose vascular anomaly (FAVA) is a complex vascular malformation that typically presents with persistent pain, discomfort, contracture and other disabling symptoms. There are no minimally invasive treatment options to effectively control these symptoms. Image-guided percutaneous cryoablation, which has been used to control pain in people with cancer, could be used for similar indications in FAVA.
Objective
To assess the role of image-guided percutaneous cryoablation for control of symptoms in FAVA lesions.
Materials and methods
We conducted a retrospective cohort study of 20 children and young adults with FAVA who underwent percutaneous cryoablation at 26 sites, from September 2013 to August 2015. The outcome was based on the brief pain inventory scoring (BPI), concurrent symptoms, clinical response and patient satisfaction.
Results
After cryoablation there was significant improvement in pain, which dropped by 3 points (pain now) to 3.7 points (pain in the last 24 h). Most patients indicated that pain interfered less in their everyday social life. Concurrent symptoms like swelling, physical limitations and skin hyperesthesia also improved. Clinical response was greatest at 2–5 months follow-up after cryoablation, with acceptable patient satisfaction thereafter. Technical response was 100%. There were no major complications.
Conclusion
Image-guided percutaneous cryoablation is a safe and effective option for treatment of symptomatic FAVA lesions.


Similar content being viewed by others
References
Alomari AI, Spencer SA, Arnold RW et al (2014) Fibro-adipose vascular anomaly: clinical-radiologic-pathologic features of a newly delineated disorder of the extremity. J Pediatr Orthop 34:109–117
Callstrom MR, Charboneau JW (2007) Image-guided palliation of painful metastases using percutaneous ablation. Tech Vasc Interv Radiol 10:120–131
Cornelis F, Neuville A, Labreze C et al (2013) Percutaneous cryotherapy of vascular malformation: initial experience. Cardiovasc Interv Radiol 36:853–856
Erinjeri JP, Clark TW (2010) Cryoablation: mechanism of action and devices. J Vasc Interv Radiol 21:S187–S191
Cleeland CS, Gonin R, Hatfield AK et al (1994) Pain and its treatment in outpatients with metastatic cancer. N Engl J Med 330:592–596
Daut RL, Cleeland CS, Flanery RC (1983) Development of the Wisconsin Brief Pain Questionnaire to assess pain in cancer and other diseases. Pain 17:197–210
Mendoza T, Mayne T, Rublee D et al (2006) Reliability and validity of a modified Brief Pain Inventory short form in patients with osteoarthritis. Eur J Pain 10:353–361
Goldberg SN, Grassi CJ, Cardella JF et al (2005) Image-guided tumor ablation: standardization of terminology and reporting criteria. J Vasc Interv Radiol 16:765–778
Moore W, Kolnick D, Tan J et al (2010) CT guided percutaneous cryoneurolysis for post thoracotomy pain syndrome: early experience and effectiveness. Acad Radiol 17:603–606
Moorjani N, Zhao F, Tian Y et al (2001) Effects of cryoanalgesia on post-thoracotomy pain and on the structure of intercostal nerves: a human prospective randomized trial and a histological study. Eur J Cardiothorac Surg 20:502–507
Leiria TL, Glavinovic T, Armour JA et al (2011) Longterm effects of cardiac mediastinal nerve cryoablation on neural inducibility of atrial fibrillation in canines. Auton Neurosci 161:68–74
Lessard AM, Gilchrist J, Schaefer L et al (2009) Palliation of recurrent Ewing sarcoma of the pelvis with cryoablation and somatosensory-evoked potentials. J Pediatr Hematol Oncol 31:18–21
Littrup PJ, Ahmed A, Aoun HD et al (2007) CT-guided percutaneous cryotherapy of renal masses. J Vasc Interv Radiol 18:383–392
Tuncali K, Morrison PR, Winalski CS et al (2007) MRI-guided percutaneous cryotherapy for soft-tissue and bone metastases: initial experience. AJR Am J Roentgenol 189:232–239
Littrup PJ, Bang HJ, Currier BP et al (2013) Soft-tissue cryoablation in diffuse locations: feasibility and intermediate term outcomes. J Vasc Interv Radiol 24:1817–1825
Philip A, Gupta S, Ahrar K et al (2013) A spectrum of nerve injury after thermal ablation: a report of four cases and review of the literature. Cardiovasc Interv Radiol 36:1427–1435
Tsoumakidou G, Buy X, Garnon J et al (2011) Percutaneous thermal ablation: how to protect the surrounding organs. Tech Vasc Interv Radiol 14:170–176
Bing F, Garnon J, Tsoumakidou G et al (2014) Imaging-guided percutaneous cryotherapy of bone and soft-tissue tumors: what is the impact on the muscles around the ablation site? AJR Am J Roentgenol 202:1361–1365
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Shaikh, R., Alomari, A.I., Kerr, C.L. et al. Cryoablation in fibro-adipose vascular anomaly (FAVA): a minimally invasive treatment option. Pediatr Radiol 46, 1179–1186 (2016). https://doi.org/10.1007/s00247-016-3576-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-016-3576-0