Abstract
Background
Thiamine deficiency in infants is still encountered in developing countries. It may present with acute neurological manifestations of infantile encephalitic beriberi.
Objective
To review brain MRI findings in infantile encephalitic beriberi from a single institution.
Materials and methods
A retrospective review of MRI scans in 22 infants with acute-onset beriberi encephalopathy was carried out.
Results
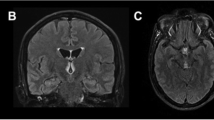
Hyperintense lesions on T2-weighted images were seen symmetrically in the putamen in all patients, in the caudate nuclei in 16/22 (73%), the thalami in 7/22 (32%) and the globi pallidi in 3/22 (14%) of the infants. Altered signal intensity lesions in the cerebral cortex were seen in 7/22 (32%). The mammillary bodies were seen in one infant and the periaqueductal gray matter in two. There was restricted diffusion in 14/22 (64%), and 6/8 children with no evidence of restriction had been imaged ≥10 days after presentation. MR spectroscopy showed increased lactate peak in 6/8 infants (75%).
Conclusion
Recognition of symmetrical T2-W hyperintense lesions in the basal ganglia with restricted diffusion and prominent lactate peak may allow early diagnosis of encephalitic beriberi in at-risk infants.






Similar content being viewed by others
References
Rao SN, Mani S, Madap K et al (2008) High prevalence of infantile encephalitic beriberi with overlapping features of Leigh’s disease. J Trop Pediatr 54:328–332
Zuccoli G, Gallucci M, Capellades J et al (2007) Wernicke encephalopathy: MR findings at clinical presentation in twenty-six alcoholic and nonalcoholic patients. AJNR Am J Neuroradiol 28:1328–1331
Kornreich L, Bron-Harlev E, Hoffmann C et al (2005) Thiamine deficiency in infants: MR findings in the brain. AJNR Am J Neuroradiol 26:1668–1674
Fattal-Valevski A, Kesler A, Sela BA et al (2005) Outbreak of life-threatening thiamine deficiency in infants in Israel caused by a defective soy-based formula. Pediatrics 115:e233–e238
Luxemburger C, White NJ, ter Kuile F et al (2003) Beri-beri: the major cause of infant mortality in Karen refugees. Trans R Soc Trop Med Hyg 97:251–255
Soukaloun D, Kounnavong S, Pengdy B et al (2003) Dietary and socio-economic factors associated with beriberi in breastfed Lao infants. Ann Trop Paediatr 23:181–186
Coats D, Shelton-Dodge K, Ou K et al (2012) Thiamine deficiency in Cambodian infants with and without beriberi. J Pediatr 161:843–847
Zuccoli G, Siddiqui N, Bailey A et al (2010) Neuroimaging findings in pediatric Wernicke encephalopathy: a review. Neuroradiology 52:523–529
Chu K, Kang DW, Kim HJ et al (2002) Diffusion-weighted imaging abnormalities in wernicke encephalopathy: reversible cytotoxic edema? Arch Neurol 59:123–127
Doherty MJ, Watson NF, Uchino K et al (2002) Diffusion abnormalities in patients with Wernicke encephalopathy. Neurology 58:655–657
White ML, Zhang Y, Andrew LG et al (2005) MR imaging with diffusion-weighted imaging in acute and chronic Wernicke encephalopathy. AJNR Am J Neuroradiol 26:2306–2310
Rugilo CA, Uribe Roca MC, Zurru MC et al (2003) Proton MR spectroscopy in Wernicke encephalopathy. AJNR Am J Neuroradiol 24:952–955
Crook MA, Sriram K (2014) Thiamine deficiency: the importance of recognition and prompt management. Nutrition 30:953–954
Desjardins P, Butterworth RF (2005) Role of mitochondrial dysfunction and oxidative stress in the pathogenesis of selective neuronal loss in Wernicke’s encephalopathy. Mol Neurobiol 31:17–25
Hazell AS, Todd KG, Butterworth RF (1998) Mechanism of neuronal cell death in Wernicke’s encephalopathy. Metab Brain Dis 13:97–122
Hegde AN, Mohan S, Lath N et al (2011) Differential diagnosis for bilateral abnormalities of the basal ganglia and thalamus. Radiographics 31:5–30
Arii J, Tanabe Y (2000) Leigh syndrome: serial MR imaging and clinical follow-up. AJNR Am J Neuroradiol 21:1502–1509
van Dongen S, Brown RM, Brown GK et al (2015) Thiamine-responsive and non-responsive patients with PDHC-E1 deficiency: a retrospective assessment. JIMD Rep 15:13–27
Qureshi UA, Wani NA, Ahmad K et al (2015) Infantile Wernicke’s encephalopathy. Arch Dis Child 100:648
Alfadhel M, Almuntashri M, Jadah RH et al (2013) Biotin-responsive basal ganglia disease should be renamed biotin-thiamine-responsive basal ganglia disease: a retrospective review of the clinical, radiological and molecular findings of 18 new cases. Orphanet J Rare Dis 8:8321
Kono S, Miyajima H, Yoshida K et al (2009) Mutations in a thiamine-transporter gene and Wernicke’s-like encephalopathy. N Engl J Med 360:1792–1794
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wani, N.A., Qureshi, U.A., Jehangir, M. et al. Infantile encephalitic beriberi: magnetic resonance imaging findings. Pediatr Radiol 46, 96–103 (2016). https://doi.org/10.1007/s00247-015-3437-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-015-3437-2