Abstract
Background
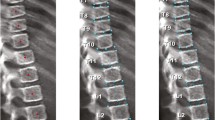
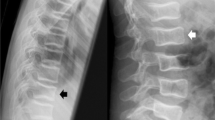
The Genant semiquantitative (GSQ) method has been a standard procedure for diagnosis of vertebral fractures in adults but has only recently been shown to be of clinical utility in children. Observer agreement using the GSQ method in this age group has not been described.
Objective
To evaluate observer agreement on vertebral readability and vertebral fracture diagnosis using the GSQ method in pediatric vertebral morphometry.
Materials and methods
Spine radiographs of 186 children with acute lymphoblastic leukemia were evaluated independently by three radiologists using the same GSQ methodology as in adults. A subset of 100 radiographs was evaluated on two occasions.
Results
An average of 4.7% of vertebrae were unreadable for the three radiologists. Intraobserver Cohen’s kappa (κ) on readability ranged from 0.434 to 0.648 at the vertebral level and from 0.416 to 0.611 at the patient level, while interobserver κ for readability had a range of 0.330 to 0.504 at the vertebral level and 0.295 to 0.467 at the patient level. Intraobserver κ for the presence of vertebral fracture had a range of 0.529 to 0.726 at the vertebral level and was 0.528 to 0.767 at the patient level. Interobserver κ for fracture at the vertebral level ranged from 0.455 to 0.548 and from 0.433 to 0.486 at the patient level.
Conclusion
Most κ values for both intra- and interobserver agreement in applying the GSQ method to pediatric spine radiographs were in the moderate to substantial range, comparable to the performance of the technique in adult studies. The GSQ method should be considered for use in pediatric research and clinical practice.




Similar content being viewed by others
References
Genant HK, Wu CY, van Kuijk C et al (1993) Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res 8:137–148
Wu CY, Li J, Jergas M et al (1995) Comparison of semiquantitative and quantitative techniques for the assessment of prevalent and incident vertebral fractures. Osteoporos Int 5:354–370
Takada M, Wu CY, Lang TF et al (1998) Vertebral fracture assessment using the lateral scoutview of computed tomography in comparison with radiographs. Osteoporos Int 8:197–203
Wu C, van Kuijk C, Li J et al (2000) Comparison of digitized images with original radiography for semiquantitative assessment of osteoporotic fractures. Osteoporos Int 11:25–30
Grados F, Roux C, de Vernejoul MC et al (2001) Comparison of four morphometric definitions and a semiquantitative consensus reading for assessing prevalent vertebral fractures. Osteoporos Int 12:716–722
Damiano J, Kolta S, Porcher R et al (2006) Diagnosis of vertebral fractures by vertebral fracture assessment. J Clin Densitom 9:66–71
Shousboe JT, DeBold CR (2006) Reliability and accuracy of vertebral fracture assessment with densitometry compared to radiography in clinical practice. Osteoporos Int 17:281–289
Fuerst T, Wu C, Genant HK et al (2009) Evaluation of vertebral fracture assessment by dual X-ray absorptiometry in a multicenter setting. Osteoporos Int 20:1199–1205
Sanfelix-Genoves J, Arana E, Sanfelix-Gimeno G et al (2011) Agreement between semi-automatic radiographic morphometry and Genant semi-quantitative method in the assessment of vertebral fracture. Osteoporos Int 23:2129–2134
Cooper C, Dennison EM, Leufkens HG et al (2004) Epidemiology of childhood fractures in Britain: a study using the general practice research database. J Bone Miner Res 19:1976–1981
Clark P, Letts M (2001) Trauma to the thoracic and lumbar spine in the adolescent. Can J Surg 44:337–345
Olmez N, Kaya T, Gunaydin R et al (2005) Intra- and interobserver variability of Kleerekoper’s method in vertebral fracture assessment. Clin Rheumatol 24:215–218
Guglielmi G, Diacinti D, van Kuikl C et al (2008) Vertebral morphometry: current methods and recent advances. Eur Radiol 18:1484–1496
Lentle BC, Brown JP, Khan A et al (2007) Recognizing and reporting vertebral fractures: reducing the risk of future osteoporotic fractures. Can Assoc Radiol J 58:27–36
Schousboe JT, Vokes T, Broy SB et al (2008) Vertebral fracture assessment: the 2007 ISCD official positions. J Clin Densitom 11:92–108
Genant HK, Jergas M, Palermo L et al (1996) Comparison of semiquantitative visual and quantitative morphometric assessment of prevalent and incident vertebral fractures in osteoporosis. J Bone Miner Res 11:984–996
Halton J, Gaboury I, Grant R et al (2009) Advanced vertebral fracture among newly diagnosed children with acute lymphoblastic leukemia: results of the Canadian Steroid-associated Osteoporosis in the Pediatric Population (STOPP) Research Program. J Bone Miner Res 24:1326–1334
Huber AM, Gaboury I, Cabral DA et al (2010) Prevalent vertebral fractures among children initiating glucocorticoid therapy for the treatment of rheumatic disorders. Arthritis Care Res 62:516–528
Ward LM (2005) Osteoporosis due to glucocorticoid use in children with chronic illness. Horm Res 64:209–221
Mäkitie O, Doria AS, Henriques F et al (2005) Radiographic vertebral morphology: a diagnostic tool in pediatric osteoporosis. J Pediatr 146:395–401
Land C, Rauch F, Munns CF et al (2006) Vertebral morphometry in children and adolescents with osteogenesis imperfecta: effect of intravenous pamidronate treatment. Bone 39:901–906
Sumnik Z, Land C, Rieger-Wettengl G et al (2004) Effect of pamidronate treatment on vertebral deformity in children with primary osteoporosis. Horm Res 61:137–142
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Cohen J (1968) Weighted kappa: nominal scale agreement with provision for scaled disagreement or partial credit. Psychol Bull 70:213–220
Rea JA, Li J, Blake GM et al (2000) Visual assessment of vertebral deformity by X-ray absorptiometry: a highly predictive method to exclude vertebral deformity. Osteoporos Int 11:660–668
Mayranpaa MK, Helenius I, Valta H et al (2007) Bone densitometry in the diagnosis of vertebral fractures in children: accuracy of vertebral fracture assessment. Bone 41:353–359
Rea JA, Chen MB, Li J et al (2000) Morphometric x-ray absorptiometry and morphometric radiography of the spine: a comparison of prevalent vertebral deformity identification. J Bone Miner Res 15:564–574
Chapurlat RD, Duboeuf F, Marion-Audibert HO et al (2006) Effectiveness of instant vertebral assessment to detect prevalent vertebral fracture. Osteoporos Int 17:1189–1195
Hospers IC, van der Laan JG, Zeebregts CJ et al (2009) Vertebral fracture assessment in supine position: comparison by using conventional semiquantitative radiography and visual radiography. Radiology 251:822–828
Gwet K (2002) Inter-rater reliability: dependency on trait prevalence and marginal homogeneity. Stat Methods Inter-rater Reliab Assess 2:1–9
Black DM, Palermo L, Nevitt MC et al (1995) Comparison of methods for defining prevalent vertebral deformities: the Study of Osteoporotic Fractures. J Bone Miner Res 10:890–902
Fechtenbaum J, Cropet C, Kolta S et al (2005) Reporting of vertebral fracture on spine x-rays. Osteoporos Int 16:1823–1826
Pearson D, Horton B, Green DJ et al (2006) Vertebral morphometry by DXA: a comparison of supine lateral and decubitus lateral densitometers. J Clin Densitom 9:295–301
Siminoski K, Lee K-C, Jen H et al (2011) Anatomical distribution of vertebral fractures: comparison of pediatric and adult spines. Osteoporos Int 23:1999–2008
Szulc P, Munoz F, Sornay-Rendu E et al (2000) Comparison of morphometric assessment of prevalent vertebral deformities in women using different reference data. Bone 27:841–846
Jackson SA, Tenenhouse A, Robertson L (2000) Vertebral fracture definition from population-based data: preliminary results from the Canadian Multicenter Osteoporosis Study (CaMos). Osteoporos Int 11:680–687
Gaca AM, Barnhart HX, Bisset GS (2010) Evaluation of wedging of lower thoracic and upper lumbar vertebral bodies in the pediatric population. AJR Am J Roentgenol 194:516–520
Alos N, Grant RM, Ramsay T et al (2012) High incidence of vertebral fractures in children with acute lymphoblastic leukemia 12 months after the initiation of therapy. J Clin Oncol 30:2760–2767
Grados F, Fechtenbaum J, Flipon E et al (2009) Radiographic methods for evaluating osteoporotic vertebral fractures. Joint Bone Spine 76:241–247
Hanrahan CJ, Shah LM (2011) MRI of spinal bone marrow: part 2, T1-weighted imaging-based differential diagnosis. AJR Am J Roentgenol 197:1309–1321
Acknowledgments
The STeroid-associated Osteoporosis in the Pediatric Population (STOPP) Consortium: Alberta Children’s Hospital, Calgary, Canada: Reinhard Kloiber, Victor Lewis, Julian Midgley, Paivi Miettunen, David Stephure; British Columbia Women’s Hospital and Health Sciences Center, Vancouver, Canada: Brian C. Lentle; British Columbia Children’s Hospital, Vancouver, Canada: David Cabral, David B. Dix, Kristin Houghton, Helen R. Nadel; Brock University, St. Catharines, Canada: John Hay; Children’s Hospital of Eastern Ontario, Ottawa, Canada: Ciaran Duffy, Janusz Feber, Jacqueline Halton, Roman Jurencak, Mary Ann Matzinger, Johannes Roth, Nazih Shenouda, Leanne M. Ward; London Health Sciences Centre, London, Canada: Elizabeth Cairney, Cheril Clarson, Guido Filler, Joanne Grimmer, Scott McKillop, Keith Sparrow, Robert Stein; IWK Health Center, Halifax, Canada: Elizabeth Cummings, Conrad Fernandez, Adam M. Huber, Bianca Lang, Kathy O’Brien; McMaster Children’s Hospital, Hamilton, Canada: Steve Arora, Stephanie Atkinson, Ronald Barr, Craig Coblentz, Peter B. Dent, Maggie Larché, Colin Webber; Montreal Children’s Hospital, Montreal, Canada: Sharon Abish, Lorraine Bell, Claire LeBlanc, Celia Rodd, Rosie Scuccimarri; Ottawa Hospital Research Institute, Ottawa, Canada: David Moher, Tim Ramsay; Shriners Hospital for Children, Montreal, Canada: Francis Glorieux, Frank Rauch; Ste. Justine Hospital, Montreal, Canada: Nathalie Alos, Josee Dubois, Caroline Laverdiere, Veronique Phan, Claire Saint-Cyr; Stollery Children’s Hospital, Edmonton, Canada: Robert Couch, Janet Ellsworth, Maury Pinsk, Kerry Siminoski, Beverly Wilson; Universite de Sherbrooke, Sherbrooke, Canada: Isabelle Gaboury; Toronto Hospital for Sick Children, Toronto, Canada: Martin Charron, Diane Hebert, Ronald Grant; Winnipeg Children’s Hospital, Winnipeg, Canada: Tom Blydt-Hansen, Sara Israels, Kiem Oen, Martin Reed, Shayne Taback.
This study was primarily funded by an operating grant from the Canadian Institutes for Health Research. Additional funding for this work has been provided to Dr. Leanne Ward by the Canadian Institutes for Health Research New Investigator Program, the Canadian Child Health Clinician Scientist Career Enhancement Program and by a University of Ottawa Research Chair Award. The study has also been partially funded by the Children’s Hospital of Eastern Ontario and Women and Children’s Health Research Institute, University of Alberta.
STOPP would like to thank the following:
The children and their families who participated in the study and without whom the STOPP research program would not have been possible.
The research associates who took care of the patients: Claude Belleville, Ronda Blasco, Erika Bloomfield, Dan Catte, Heather Cosgrove, Valerie Gagne, Diane Laforte, Maritza Laprise, Josie MacLennan, Natacha Gaulin Marion, Germaine McInnes, Amanda Mullins, Eileen Pyra, Catherine Riddell and Aleasha Warner.
The research nurses and support staff from the various Divisions of Nephrology, Oncology, Rheumatology and Radiology who have contributed to the care of the children enrolled in the study.
The research associates who managed the study at the Children’s Hospital of Eastern Ontario: Steve Anderson, Victor Konji, Catherine Riddell, Maya Scharke, Elizabeth Sykes and Monica Tomiak.
Conflict of interest
None.
Author information
Authors and Affiliations
Consortia
Corresponding author
Rights and permissions
About this article
Cite this article
Siminoski, K., Lentle, B., Matzinger, M.A. et al. Observer agreement in pediatric semiquantitative vertebral fracture diagnosis. Pediatr Radiol 44, 457–466 (2014). https://doi.org/10.1007/s00247-013-2837-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-013-2837-4