Abstract
Background
Urea cycle disorders encompass several enzyme deficiencies that can result in cerebral damage, with a wide clinical spectrum from asymptomatic to severe.
Objective
The goal of this study was to correlate brain MRI abnormalities in urea cycle disorders with clinical neurological sequelae to evaluate whether MRI abnormalities can assist in guiding difficult treatment decisions.
Materials and methods
We performed a retrospective chart review of patients with urea cycle disorders and symptomatic hyperammonemia. Brain MRI images were reviewed for abnormalities that correlated with severity of clinical neurological sequelae.
Results
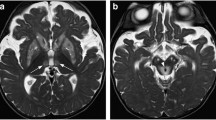
Our case series comprises six urea cycle disorder patients, five with ornithine transcarbamylase deficiency and one with citrullinemia type 1. The observed trend in distribution of brain MRI abnormalities as the severity of neurological sequelae increased was the peri-insular region first, extending into the frontal, parietal, temporal and, finally, the occipital lobes. There was thalamic restricted diffusion in three children with prolonged hyperammonemia. Prior to death, this site is typically reported to be spared in urea cycle disorders.
Conclusion
The pattern and extent of brain MRI abnormalities correlate with clinical neurological outcome in our case series. This suggests that brain MRI abnormalities may assist in determining prognosis and helping clinicians with subsequent treatment decisions.





Similar content being viewed by others
Abbreviations
- OTC:
-
Ornithine transcarbamylase deficiency
- CIT 1:
-
Citrullinemia type 1
References
Summar ML, Dobbelaere D, Brusilow S et al (2008) Diagnosis, symptoms, frequency and mortality of 260 patients with urea cycle disorders from a 21-year, multicentre study of acute hyperammonaemic episodes. Acta Paediatrica 97:1420–1425
Brusilow SW, Koehler RC, Traystman RJ et al (2010) Astrocyte glutamine synthetase: importance in hyperammonemic syndromes and potential target for therapy. Neurotherapeutics 7:452–470
Barkovich AJ (2005) Pediatric neuroimaging. Lippincott Williams & Wilkins, Philadelphia
Takanashi J, Barkovich AJ, Cheng SF et al (2003) Brain MR imaging in acute hyperammonemic encephalopathy arising from late-onset ornithine transcarbamylase deficiency. AJNR 24:390–393
Sperl W, Felber S, Skladal D et al (1997) Metabolic stroke in carbamyl phosphate synthetase deficiency. Neuropediatrics 28:229–234
Mamourian AC, du Plessis A (1991) Urea cycle defect: a case with MR and CT findings resembling infarct. Pediatr Radiol 21:594–595
Bajaj SK, Kurlemann G, Schuierer G et al (1996) CT and MRI in a girl with late-onset ornithine transcarbamylase deficiency: case report. Neuroradiology 38:796–799
Maestri NE, Clissold D, Brusilow SW (1999) Neonatal onset ornithine transcarbamylase deficiency: a retrospective analysis. J Pediatr 134:268–272
McCullough BA, Yudkoff M, Batshaw ML et al (2000) Genotype spectrum of ornithine transcarbamylase deficiency: correlation with the clinical and biochemical phenotype. Am J Med Genet 93:313–319
Nicolaides P, Liebsch D, Dale N et al (2002) Neurological outcome of patients with ornithine carbamoyltransferase deficiency. Arch Dis Child 86:54–56
Smith W, Kishnani PS, Lee B et al (2005) Urea cycle disorders: clinical presentation outside the newborn period. Crit Care Clin 21(4 Suppl):S9–S17
Bachmann C (2003) Long-term outcome of patients with urea cycle disorders and the question of neonatal screening. Eur J Pediatr 162(Suppl):S29–S33
Picca S, Dionisi-Vici C, Abeni D et al (2001) Extracorporeal dialysis in neonatal hyperammonemia: modalities and prognostic indicators. Pediatr Nephrol 16:862–867
Arnoux JB, Dupic L, Barbier V et al (2010) Neurological outcome of pediatric patients with urea cycle disorders. J Inherit Metab Dis 33(Suppl 1):S121
Msall M, Batshaw ML, Suss R et al (1984) Neurologic outcome in children with inborn errors of urea synthesis. Outcome of urea-cycle enzymopathies. N Engl J Med 310:1500–1505
Kurihara AT, Tomita M, Kobayashi K (2003) Magnetic resonance imaging in late-onset ornithine transcarbamylase deficiency. Brain Dev 25:40–44
Majoie CBLM, Mourmans JM, Akkerman EM et al (2004) Neonatal citrullinemia: comparison of conventional MR, diffusion-weighted, and diffusion tensor findings. AJNR 25:32–35
Pu Y, Li Q-F, Zeng C-M et al (2000) Increased detectability of alpha brain glutamate/glutamine in neonatal hypoxic-ischemic encephalopathy. AJNR 21:203–212
Gropman AL, Seltzer RR, Yudkoff M et al (2008) 1H MRS allows brain phenotype differentiation in sisters with late onset ornithine transcarbamylase deficiency (OTCD) and discordant clinical presentations. Mol Genet Metab 94:52–60
Gropman A (2010) Brain imaging in urea cycle disorders. Mol Genet Metab 100(Suppl 1):S20–S30
Larsen FS (2002) Cerebral blood flow in hyperammonemia: heterogeneity and starling forces in capillaries. Metab Brain Dis 17:229–235
Takahashi H, Koehler RC, Brusilow SW et al (1991) Inhibition of brain glutamine accumulation prevents cerebral edema in hyperammonemic rats. Am J Physiol 261(3 Pt 2):H825–H829
Hirata T, Koehler RC, Brusilow SW et al (1995) Preservation of cerebral blood flow responses to hypoxia and arterial pressure alterations in hyperammonemic rats. J Cereb Blood Flow Metab 15:835–844
Chen Y-F, Huang Y-C, Liu H-M et al (2001) MRI in a case of adult-onset citrullinemia. Neuroradiology 43:845–847
Kawata A, Suda M, Tanabe H (1997) Adult-onset type II citrullinemia: clinical pictures before and after liver transplantation. Intern Med 36:408–412
Kranz PG, Eastwood JD (2009) Does diffusion-weighted imaging represent the ischemic core? An evidence-based systematic review. AJNR 30:1206–1212
Anderson JM, Brodsky MC (2010) Protracted cortical visual loss in a child with ornithine transcarbamylase deficiency. J Neuroopthalmol 30:99–101
Snebold NG, Rizzo JF, Lessell S et al (1987) Transient visual loss in ornithine transcarbamoylase deficiency. Am J Ophthalmol 104:407–412
Gropman AL, Fricke ST, Seltzer RR et al (2008) 1H MRS identifies symptomatic and asymptomatic subjects with partial ornithine transcarbamylase deficiency. Mol Genet Metab 95:21–30
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bireley, W.R., Van Hove, J.L.K., Gallagher, R.C. et al. Urea cycle disorders: brain MRI and neurological outcome. Pediatr Radiol 42, 455–462 (2012). https://doi.org/10.1007/s00247-011-2253-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-011-2253-6