Abstract
Background
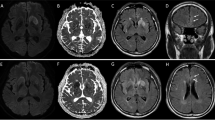
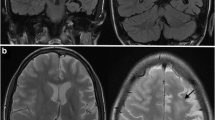
Rasmussen encephalitis (RE) is a rare devastating disease of childhood causing progressive neurological deficits and intractable seizures, typically affecting one hemisphere. Characteristic MRI features include progressive unihemispheric focal cortical atrophy and grey- or white-matter high-signal changes and basal ganglion involvement, particularly of the caudate nucleus.
Objective
To analyse the pattern of involvement of different brain structures in a series of patients with RE and to attempt clinical correlation.
Materials and methods
We reviewed the medical records and neuroimaging data of 12 patients diagnosed with RE satisfying the European Consensus Statement diagnostic criteria.
Results
The disease manifested as seizures in all patients and was refractory; epilepsia partialis continua was a notable feature (nine patients). Hemiparesis of varying grades was noted in all but one patient; none had extrapyramidal signs. Neuroimaging showed cortical involvement in the insular/periinsular regions in 11 patients. Caudate atrophy was noted in ten patients. Putaminal atrophy was seen in nine patients, six of whom had additional hyperintense signal changes.
Conclusions
Our study highlights frequent putaminal atrophy and signal changes in RE, which suggests a more extensive basal ganglion involvement than emphasized previously. Recognition of putaminal changes may be a useful additional tool in the radiological diagnosis of RE.






Similar content being viewed by others
References
Rasmussen T, Olszeweski J, Lloyd-Smith D (1958) Focal seizures due to chronic localized encephalitis. Neurology 8:435–445
Robitaille Y (1991) Neuropathological aspects of chronic encephalitis. In: Andermann F (ed) Chronic encephalitis and epilepsy – Rasmussen’s syndrome. Butterworth-Heinemann, Boston, pp 79–110
Oguni H, Andermann F, Rasmussen TB (1991) The natural history of the syndrome of chronic encephalitis and epilepsy: a study of the MNI series of forty-eight cases. In: Andermann F (ed) Chronic encephalitis and epilepsy – Rasmussen’s syndrome. Butterworth-Heinemann, Boston, pp 7–35
Vining EP, Freeman JM, Brandt J, et al (1993) Progressive unilateral encephalopathy of childhood (Rasmussen’s syndrome): a reappraisal. Epilepsia 34:639–650
Bien CG, Widman G, Urbach H, et al (2002) The natural history of Rasmussen’s encephalitis. Brain 125:1751–1759
Pardo CA, Vining EP, Guo L, et al (2004) The pathology of Rasmussen syndrome: stages of cortical involvement and neuropathological studies in 45 hemispherectomies. Epilepsia 45:516–526
Bien CG, Granata T, Antozzi C, et al (2005) Pathogenesis, diagnosis and treatment of Rasmussen encephalitis: a European consensus statement. Brain 128:454–471
Granata T, Gobbi G, Spreafico R, et al (2003) Rasmussen’s encephalitis: early characteristics allow diagnosis. Neurology 60:422–425
Bhatjiwale MG, Polkey C, Cox TC, et al (1998) Rasmussen’s encephalitis: neuroimaging findings in 21 patients with a closer look at the basal ganglia. Pediatr Neurosurg 29:142–148
Bien CG, Urbach H, Deckert M, et al (2002) Diagnosis and staging of Rasmussen’s encephalitis by serial MRI and histopathology. Neurology 58:250–257
Chiapparini L, Granata T, Farina L, et al (2003) Diagnostic imaging in 13 cases of Rasmussen’s encephalitis: can early MRI suggest the diagnosis? Neuroradiology 45:171–183
Tien RD, Ashdown BC, Lewis DV Jr, et al (1992) Rasmussen’s encephalitis: neuroimaging findings in four patients. AJR 158:1329–1332
Acknowledgement
We thank Prof. V. V. Radhakrishnan, for providing the histopathological slides.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rajesh, B., Kesavadas, C., Ashalatha, R. et al. Putaminal involvement in Rasmussen encephalitis. Pediatr Radiol 36, 816–822 (2006). https://doi.org/10.1007/s00247-006-0176-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-006-0176-4