Abstract
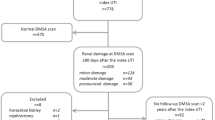
Background: Renal cortical scintigraphic studies challenge the role of vesicoureteric reflux in renal scar development, emphasizing instead the part played by acute pyelonephritis. Objective: To determine the prevalence of renal cortical defects in a child cohort 2 years after the child’s first diagnosed urinary tract infection and to analyze the relationship of these defects with acute illness variables, primary vesicoureteric reflux and recurrent infections. Materials and methods: In a prospective cohort study, 193 children younger than 5 years with their first proven urinary tract infection underwent renal sonography, voiding cystourethrogram, and renal cortical scintigraphy within 15 days of diagnosis. Two years later, 150 of the 193 children, or 77.7%, had a further renal cortical scintigram, including 75, or 86.2%, of the 87 children who had acute scintigraphic defects. The relationship of cortical defects to age, gender, pre-treatment symptom duration, hospitalization, presence and grade of vesicoureteric reflux, and recurrent urinary tract infections was evaluated. Results: Overall, 20 of the 150 (13.3%; 95% confidence interval (CI) 8.3, 19.8) children had persistent defects 2 years after infection. This included 20 of 75 (26.7%; 95% CI 17.1, 38.1) with initially abnormal scintigrams. No new defects were detected. Although acute defects were more common in the young, those with persistent defects were older (median ages 16.4 vs. 6.8 months, P=0.004) than those with transient abnormalities. After adjustment for age, persistent defects were no longer associated with gender and were not predicted by acute illness variables, primary vesicoureteric reflux or recurrent infections. Conclusions: Renal cortical scintigraphic defects persisted in approximately one-quarter of young children after their first proven urinary tract infection. The associated clinical features, however, failed to predict scar formation. It is possible that some of the scintigraphic defects preceded the infection by arising from either previously undiagnosed acute pyelonephritis or from underlying congenital dysplasia. The etiology of scars may be best addressed by determining whether prevention of urinary tract infections from birth avoids post-natal scar acquisition or extension.
Similar content being viewed by others
References
Winberg J, Anderson HJ, Bergstrom T, et al (1974) Epidemiology of symptomatic urinary tract infection in childhood. Acta Paediatr Scand Suppl 252:1–20
Haddon R, Barnett PLJ, Grimwood K, et al (1999) Bacteraemia in febrile children presenting to a paediatric emergency department. Med J Aust 170:475–478
Jacobson SH, Eklof O, Eriksson CG, et al (1989) Development of hypertension and uraemia after pyelonephritis in childhood: 27-year follow-up. BMJ 299:703–706
Smellie JM, Prescod NP, Shaw PJ, et al (1998) Childhood reflux and urinary infection: a follow-up of 10–41 years in 226 adults. Pediatr Nephrol 12:727–736
Martinell J, Claesson I, Lidin-Janson G, et al (1995) Urinary infection, reflux and renal scarring in females continuously followed for 13–38 years. Pediatr Nephrol 9:131–136
Bailey RR (1993) Vesico-ureteric reflux and reflux nephropathy. Kidney Int 44 [Suppl 42]:S80–S85
Goldraich NP, Ramos OL, Goldraich IH (1989) Urography vs. DMSA scan in children with vesicoureteric reflux. Pediatr Nephrol 3:1–35
Smellie JM, Ransley PG, Normand IC, et al (1985) Development of new renal scars: a collaborative study. BMJ 290:1957–1960
Benador A, Benador N, Slosman DO, et al (1994) Cortical scintigraphy in the evaluation of renal parenchymal changes in children with pyelonephritis. J Pediatr 124:17–20
Smellie JM, Rigden SP, Prescod NP (1995) Urinary tract infection: a comparison of four methods of investigation. Arch Dis Child 72:247–250
Jakobsson B, Jacobson SH, Hjalmas K (1999) Vesico-ureteric reflux and other risk factors for renal damage: identification of high- and low-risk children. Acta Paediatr Suppl 431:31–39
Assael BM, Guez S, Marra G, et al (1998) Congenital reflux nephropathy: a follow-up of 108 cases diagnosed prenatally. Br J Urol 82:252–257
McIlroy PJ, Abbott GD, Anderson NG, et al (2000) Outcome of primary vesicoureteric reflux detected following fetal renal pelvic dilatation. J Paediatr Child Health 36:569–573
Stock JA, Wilson D, Hanna MK (1998) Congenital reflux nephropathy and severe unilateral fetal reflux. J Urol 160:1017–1018
Merrick MV, Notghi A, Chalmers N, et al (1995) Long-term follow-up to determine the prognostic value of imaging after urinary tract infections. 2. Scarring. Arch Dis Child 72:393–396
Jakobsson B, Berg U, Svensson L (1994) Renal scarring after acute pyelonephritis. Arch Dis Child 70:111–115
Stokland E, Hellstrom M, Jacobsson B, et al (1996) Renal damage one year after first urinary tract infection: role of dimercaptosuccinic acid scintigraphy. J Pediatr 129:815–820
Ditchfield MR, De Campo JF, Cook DJ, et al (1994) Vesicoureteral reflux: an accurate predictor of acute pyelonephritis in child urinary tract infection? Radiology 190:413–415
Dick PT (1996) Routine diagnostic imaging for childhood urinary tract infections: a systematic overview. J Pediatr 128:15–22
Beattie TJ, McKenzie JR (1994) Renal scarring after acute pyelonephritis. Arch Dis Child 71:386–387
Jakobsson B, Svensson L (1997) Transient pyelonephritic changes on 99mTechenetium-dimercaptosuccinic acid scan for at least five months after infection. Acta Paediatr 86:803–807
Ditchfield MR, Summerville D, Grimwood K, et al (2002) Time course of transient cortical scintigraphic defects associated with acute pyelonephritis. Pediatr Radiol 32:849–852
Ditchfield MR, de Campo JF, Nolan TM, et al (1994) Risk factors in the development of early renal cortical defects in children with urinary tract infection. AJR 162:1393–1397
Ditchfield MR, de Campo JF (1993) How to do it: the MCU in children. Aust Radiol 37:69–72
Lebowitz RL, Olbing H, Parkkulainen KV, et al (1985) International system of radiographic grading of vesicoureteric reflux. International reflux study in children. Pediatr Radiol 15:105–109
Traisman ES, Conway JJ, Traisman HS, et al (1986) The localization of urinary tract infection with 99mTc glucoheptonate scintigraphy. Pediatr Radiol 16:403–406
Clarke SE, Smellie JM, Prescod N, et al (1996) Technetium-99m DMSA studies in pediatric urinary tract infection. J Nucl Med 37:823–828
Jones CL, Walker RG, Powell HR (1993) Recent advances in the management of vesico-ureteric reflux. J Paediatr Child Health 19:325–327
Wennerstrom M, Hansson S, Jodal U, et al (2000) Primary and acquired renal scarring in boys and girls with urinary tract infection. J Pediatr 136:30–34
Hoberman A, Wald ER, Hickey RW, et al (1999) Oral versus initial intravenous therapy for urinary tract infections in young febrile children. Pediatrics 104:79–86
Hoberman A, Charron M, Hickey RW, et al (2003) Imaging studies after a first febrile urinary tract infection in young children. N Engl J Med 348:195–202
Obling H, Claesson I, Ebel KD, et al (1992) Renal scars and parenchymal thinning in children with vesicoureteral reflux: a 5-year report of the international reflux study in children (European branch). J Urol 148:1653–1656
Weiss R, Duckett J, Spitzer A (1992) Results of a randomized clinical trial of medical versus surgical management of infants and children with graded III and IV primary vesicoureteral reflux (United States). The international reflux study in Children. J Urol 148:1667–1673
Goldraich NP, Goldraich IH (1992). Follow-up of conservatively treated children with high- and low-grade vesicoureteric reflux: a prospective study. J Urol 148:1688–1692
Vernon SJ, Coulthard MG, Lambert HJ, et al (1997) New renal scarring in children who at age 3 and 4 years had had normal scans with dimercaptosuccinic acid: follow-up study. BMJ 315:905–908
Goldman M, Lahat E, Strauss S, et al (2000) Imaging after urinary tract infection in male neonates. Pediatrics 105:1232–1235
Benador D, Benador N, Slosman D, et al (1997) Are younger children at highest risk of renal sequelae after pyelonephritis? Lancet 349:17–19
Van der Voort JH, Edwards AG, Roberts R, et al (2002) Unexplained extra visits to general practitioners before the diagnosis of first urinary tract infection: a case-control study. Arch Dis Child 87:530–533
Buonomo C, Treves ST, Jones B, et al (1993) Silent renal damage in symptom-free siblings of children with vesicoureteral reflux: assessment with technetium Tc99m dimercaptosuccinic acid scintigraphy. J Pediatr 122:721–723
Polito C, La Manna A, Rambaldi PF, et al (2000) High incidence of a generally small kidney and primary vesicoureteral reflux. J Urol 164:479–482
Cascio S, Yoneda A, Chertin B, et al (2003). Renal parenchymal damage in sibling vesicoureteric reflux. Acta Paediatr 92:17–20
Craig JC, Irwig LM, Knight JF, et al (2000) Does treatment of vesicoureteric reflux in childhood prevent end-stage renal disease attributable to reflux nephropathy? Pediatrics 105:1236–1241
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported by the Murdoch Children’s Research Institute
Rights and permissions
About this article
Cite this article
Ditchfield, M.R., Grimwood, K., Cook, D.J. et al. Persistent renal cortical scintigram defects in children 2 years after urinary tract infection. Pediatr Radiol 34, 465–471 (2004). https://doi.org/10.1007/s00247-004-1182-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-004-1182-z