Abstract
Background
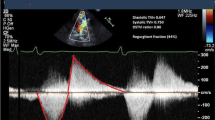
In patients with repaired Tetralogy of Fallot (rTOF), pulmonary regurgitation (PR) leads to significant morbidity. Cardiac magnetic resonance imaging (CMR) is the gold standard to assess severity of PR in rTOF patients. We compared Doppler echocardiography derived indices of PR with CMR to find the best predictive parameter for hemodynamically significant (hs) PR.
Methods
This is a retrospective analysis of echocardiogram and CMR measurements. Doppler indices obtained included: PR deceleration slope, pressure half time (PHT) and PR index. Receiver operating characteristic curve analysis was used to optimize the sensitivity and specificity of selected variables in predicting hsPR. Inter-observer variability of the Doppler parameters was assessed in a random sample of 25 Doppler spectral recordings.
Results
Our cohort (n = 96) comprised of 52 (54.2%) males. The mean (SD) age at CMR was 22.9 (10.3) years. 83.4% patients underwent complete repair with transannular patch. 78 (81%) patients had hsPR as defined by CMR PR > 20%. Doppler parameters with the values of; PR index of < 0.86, PR deceleration slope of > 375 cm/s2 and a PHT < 130 ms, demonstrated high sensitivity (93%) and high negative predictive values (98–99%). All the Doppler indices demonstrated minimal inter-observer variability (PHT = 0.9, 95% CI 0.69–0.97; PRi = 0.95, 95%CI 0.83–0.98).
Conclusion
Our data, with its high negative predictive values, show that Doppler derived echocardiography indices have an ability to rule out hsPR, as measured by CMR. PHT, PR index and deceleration slope correlate with hsPR and can be used as screening tools for further testing.


Similar content being viewed by others
References
Parker SE, Mai CT, Canfield MA, Rickard R, Wang Y, Meyer RE et al (2010) Updated National Birth Prevalence estimates for selected birth defects in the United States, 2004–2006. Birth Defects Res A 88(12):1008–1016
Lillehei CW, Cohen M, Warden HE, Read RC, Aust JB, Dewall RA et al (1955) Direct vision intracardiac surgical correction of the tetralogy of Fallot, pentalogy of Fallot, and pulmonary atresia defects; report of first ten cases. Ann Surg 142(3):418–442
Nollert G, Fischlein T, Bouterwek S, Bohmer C, Klinner W, Reichart B (1997) Long-term survival in patients with repair of tetralogy of Fallot: 36-year follow-up of 490 survivors of the first year after surgical repair. J Am Coll Cardiol 30(5):1374–1383
Murphy JG, Gersh BJ, Mair DD, Fuster V, McGoon MD, Ilstrup DM et al (1993) Long-term outcome in patients undergoing surgical repair of tetralogy of Fallot. N Engl J Med 329(9):593–599
Chaturvedi RR, Redington AN (2007) Pulmonary regurgitation in congenital heart disease. Heart 93(7):880–889
Bove EL, Byrum CJ, Thomas FD, Kavey RE, Sondheimer HM, Blackman MS et al (1983) The influence of pulmonary insufficiency on ventricular function following repair of tetralogy of Fallot. Evaluation using radionuclide ventriculography. J Thorac Cardiovasc Surg 85(5):691–696
Niezen RA, Helbing WA, van der Wall EE, van der Geest RJ, Rebergen SA, de Roos A (1996) Biventricular systolic function and mass studied with MR imaging in children with pulmonary regurgitation after repair for tetralogy of Fallot. Radiology 201(1):135–140
Gatzoulis MA, Till JA, Somerville J, Redington AN (1995) Mechanoelectrical interaction in tetralogy of Fallot. QRS prolongation relates to right ventricular size and predicts malignant ventricular arrhythmias and sudden death. Circulation 92(2):231–237
Rowe SA, Zahka KG, Manolio TA, Horneffer PJ, Kidd L (1991) Lung function and pulmonary regurgitation limit exercise capacity in postoperative tetralogy of Fallot. J Am Coll Cardiol 17(2):461–466
Kondo C, Nakazawa M, Kusakabe K, Momma K (1995) Left ventricular dysfunction on exercise long-term after total repair of tetralogy of Fallot. Circulation 92(9 Suppl):II250–II255
Gatzoulis MA, Balaji S, Webber SA, Siu SC, Hokanson JS, Poile C et al (2000) Risk factors for arrhythmia and sudden cardiac death late after repair of tetralogy of Fallot: a multicentre study. Lancet 356(9234):975–981
Geva T (2011) Repaired tetralogy of Fallot: the roles of cardiovascular magnetic resonance in evaluating pathophysiology and for pulmonary valve replacement decision support. J Cardiovasc Magn Reson 13:9
Geva T (2013) Indications for pulmonary valve replacement in repaired tetralogy of Fallot: the quest continues. Circulation 128(17):1855–1857
Rominger MB, Bachmann GF, Pabst W, Rau WS (1999) Right ventricular volumes and ejection fraction with fast cine MR imaging in breath-hold technique: applicability, normal values from 52 volunteers, and evaluation of 325 adult cardiac patients. J Magn Reson Imaging 10(6):908–918
Rebergen SA, Chin JG, Ottenkamp J, van der Wall EE, de Roos A (1993) Pulmonary regurgitation in the late postoperative follow-up of tetralogy of Fallot. Volumetric quantitation by nuclear magnetic resonance velocity mapping. Circulation 88(5 Pt 1):2257–2266
Warnes CA, Williams RG, Bashore TM, Child JS, Connolly HM, Dearani JA et al (2008) ACC/AHA 2008 guidelines for the management of adults with congenital heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Develop Guidelines on the Management of Adults With Congenital Heart Disease). Developed in Collaboration With the American Society of Echocardiography, Heart Rhythm Society, International Society for Adult Congenital Heart Disease, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Am Coll Cardiol 52(23):e143–e263
Silversides CK, Veldtman GR, Crossin J, Merchant N, Webb GD, McCrindle BW et al (2003) Pressure half-time predicts hemodynamically significant pulmonary regurgitation in adult patients with repaired tetralogy of fallot. J Am Soc Echocardiogr 16(10):1057–1062
Mercer-Rosa L, Yang W, Kutty S, Rychik J, Fogel M, Goldmuntz E (2012) Quantifying pulmonary regurgitation and right ventricular function in surgically repaired tetralogy of Fallot: a comparative analysis of echocardiography and magnetic resonance imaging. Circ Cardiovasc Imaging 5(5):637–643
Renella P, Aboulhosn J, Lohan DG, Jonnala P, Finn JP, Satou GM et al (2010) Two-dimensional and Doppler echocardiography reliably predict severe pulmonary regurgitation as quantified by cardiac magnetic resonance. J Am Soc Echocardiogr 23(8):880–886
Li W, Davlouros PA, Kilner PJ, Pennell DJ, Gibson D, Henein MY et al (2004) Doppler-echocardiographic assessment of pulmonary regurgitation in adults with repaired tetralogy of Fallot: comparison with cardiovascular magnetic resonance imaging. Am Heart J 147(1):165–172
Carminati M, Pluchinotta FR, Piazza L, Micheletti A, Negura D, Chessa M et al (2015) Echocardiographic assessment after surgical repair of tetralogy of fallot. Front Pediatr 3:3
Bhat M, Goldmuntz E, Fogel MA, Rychik J, Mercer-Rosa L (2017) Longitudinal validation of the diastolic to systolic time-velocity integral ratio as a Doppler-derived measure of pulmonary regurgitation in patients with repaired tetralogy of Fallot. Pediatr Cardiol 38(2):240–246
Festa P, Ait-Ali L, Minichilli F, Kristo I, Deiana M, Picano E (2010) A new simple method to estimate pulmonary regurgitation by echocardiography in operated fallot: comparison with magnetic resonance imaging and performance test evaluation. J Am Soc Echocardiogr 23(5):496–503
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors have no conflicts of interest.
Informed Consent
This is a retrospective study and the need for Informed consent was waived by the Institutional Review Board.
Research Involving Human and Animal Participants
This article does not contain any studies with human participants performed by any of the authors.
Rights and permissions
About this article
Cite this article
Bansal, N., Gupta, P., Joshi, A. et al. Utility of Doppler Echocardiography to Estimate the Severity of Pulmonary Valve Regurgitation Fraction in Patients with Repaired Tetralogy of Fallot. Pediatr Cardiol 40, 404–411 (2019). https://doi.org/10.1007/s00246-018-2045-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-018-2045-y