Abstract
Purpose
Both the striatal-thalamo-cortical (STC) circuit and cerebello-thalamo-cortical (CTC) circuit play a critical role in Parkinson’s disease (PD).
Methods
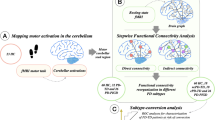
Resting-state functional MRI was used to assess functional connectivity (FC) focusing on the basal ganglia (BG) and cerebellum among early-stage drug-naïve PD patients with tremor-dominant (TD) PD patients with postural instability and gait dysfunction (PIGD) and healthy controls (HCs).
Results
Compared to HCs, both PD subgroups had higher FC between the cerebellum and paracentral lobule, sensorimotor areas; lower FC between the BG and superior frontal gyrus, and within the BG circuit; PD-TD patients showed higher FC between the BG and fusiform, paracentral lobule, cerebellum Lobule VI, and between the cerebellum and supplementary motor areas (SMA), insula; lower FC between the BG and rectus, sensorimotor areas, and within the cerebellum circuit; PD-PIGD patients showed higher FC between the cerebellum and middle frontal gyrus, precuneus; lower FC between the BG and cerebellum Crus II. Besides, compared to PD-PIGD patients and HCs, PD-TD patients had higher FC between the BG and calcarine region. In all PD patients, FC in paracentral lobule, SMA, and cerebellum Lobule VI positively correlated with tremor scores, and FC in calcarine area positively correlated with tremor scores, but negatively correlated with PIGD scores.
Conclusion
Our findings mainly suggested that the BG and cerebellum had hyper-connectivity with the cortical motor cortex, and the BG had prominent hyper-connectivity with the visual cortex in early-stage PD-TD patients. These findings may be helpful for facilitating the further understanding of potential mechanisms in the early-stage PD-TD. However, our results are preliminary, and further investigations are needed.



Similar content being viewed by others
References
Schiess MC, Suescun J (2015) Clinical determinants of progression of Parkinson disease: predicting prognosis by subtype. JAMA Neurol 72(8):859–860. https://doi.org/10.1001/jamaneurol.2015.1067
Berardelli A, Rothwell JC, Thompson PD, Hallett M (2001) Pathophysiology of bradykinesia in Parkinson's disease. Brain 124(Pt 11):2131–2146
Suchowersky O, Reich S, Perlmutter J, Zesiewicz T, Gronseth G, Weiner WJ, Quality Standards Subcommittee of the American Academy of N (2006) Practice parameter: diagnosis and prognosis of new onset Parkinson disease (an evidence-based review): report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology 66(7):968–975. https://doi.org/10.1212/01.wnl.0000215437.80053.d0
Piccinin CC, Campos LS, Guimaraes RP, Piovesana LG, MCA DS, Azevedo PC, Campos BM, de Rezende TJR, Amato-Filho A, Cendes F, D'Abreu A (2017) Differential pattern of cerebellar atrophy in tremor-predominant and akinetic/rigidity-predominant Parkinson's disease. Cerebellum (London, England) 16(3):623–628. https://doi.org/10.1007/s12311-016-0834-5
Lewis MM, Du G, Sen S, Kawaguchi A, Truong Y, Lee S, Mailman RB, Huang X (2011) Differential involvement of striato- and cerebello-thalamo-cortical pathways in tremor- and akinetic/rigid-predominant Parkinson’s disease. Neuroscience 177:230–239. https://doi.org/10.1016/j.neuroscience.2010.12.060
Guan X, Xuan M, Gu Q, Xu X, Huang P, Wang N, Shen Z, Xu J, Luo W, Zhang M (2017) Influence of regional iron on the motor impairments of Parkinson’s disease: a quantitative susceptibility mapping study. J Magn Reson Imaging : JMRI 45(5):1335–1342. https://doi.org/10.1002/jmri.25434
Selikhova M, Williams DR, Kempster PA, Holton JL, Revesz T, Lees AJ (2009) A clinico-pathological study of subtypes in Parkinson’s disease. Brain 132(Pt 11):2947–2957. https://doi.org/10.1093/brain/awp234
Braak H, Del Tredici K, Rub U, de Vos RA, Jansen Steur EN, Braak E (2003) Staging of brain pathology related to sporadic Parkinson’s disease. Neurobiol Aging 24(2):197–211
Helmich RC, Hallett M, Deuschl G, Toni I, Bloem BR (2012) Cerebral causes and consequences of parkinsonian resting tremor: a tale of two circuits? Brain 135(Pt 11):3206–3226. https://doi.org/10.1093/brain/aws023
Hou Y, Yang J, Luo C, Ou R, Song W, Liu W, Gong Q, Shang H (2016) Patterns of striatal functional connectivity differ in early and late onset Parkinson’s disease. J Neurol 263:1993–2003. https://doi.org/10.1007/s00415-016-8211-3
Buhmann C, Glauche V, Sturenburg HJ, Oechsner M, Weiller C, Buchel C (2003) Pharmacologically modulated fMRI--cortical responsiveness to levodopa in drug-naive hemiparkinsonian patients. Brain 126(Pt 2):451–461
Hughes AJ, Daniel SE, Kilford L, Lees AJ (1992) Accuracy of clinical diagnosis of idiopathic Parkinson’s disease: a clinico-pathological study of 100 cases. J Neurol Neurosurg Psychiatry 55(3):181–184
Jankovic J, McDermott M, Carter J, Gauthier S, Goetz C, Golbe L, Huber S, Koller W, Olanow C, Shoulson I, Stern M, Tanner C, Weiner W, Parkinson Study Group (1990) Variable expression of Parkinson’s disease: a base-line analysis of the DATATOP cohort. The Parkinson Study Group. Neurology 40(10):1529–1534
Katzman R, Zhang MY, Ouang Ya Q, Wang ZY, Liu WT, Yu E, Wong SC, Salmon DP, Grant I (1988) A Chinese version of the mini-mental state examination; impact of illiteracy in a Shanghai dementia survey. J Clin Epidemiol 41(10):971–978
Helmich RC, Derikx LC, Bakker M, Scheeringa R, Bloem BR, Toni I (2010) Spatial remapping of cortico-striatal connectivity in Parkinson’s disease. Cereb Cortex 20(5):1175–1186
Luo C, Song W, Chen Q, Zheng Z, Chen K, Cao B, Yang J, Li J, Huang X, Gong Q, Shang HF (2014) Reduced functional connectivity in early-stage drug-naive Parkinson’s disease: a resting-state fMRI study. Neurobiol Aging 35(2):431–441. https://doi.org/10.1016/j.neurobiolaging.2013.08.018
O'Callaghan C, Hornberger M, Balsters JH, Halliday GM, Lewis SJ, Shine JM (2016) Cerebellar atrophy in Parkinson’s disease and its implication for network connectivity. Brain 139(Pt 3):845–855. https://doi.org/10.1093/brain/awv399
Wu T, Hallett M (2013) The cerebellum in Parkinson’s disease. Brain 136(Pt 3):696–709. https://doi.org/10.1093/brain/aws360
Balsters JH, Laird AR, Fox PT, Eickhoff SB (2014) Bridging the gap between functional and anatomical features of cortico-cerebellar circuits using meta-analytic connectivity modeling. Hum Brain Mapp 35(7):3152–3169. https://doi.org/10.1002/hbm.22392
Wu T, Long X, Wang L, Hallett M, Zang Y, Li K, Chan P (2011) Functional connectivity of cortical motor areas in the resting state in Parkinson’s disease. Hum Brain Mapp 32(9):1443–1457. https://doi.org/10.1002/hbm.21118
Weil RS, Schrag AE, Warren JD, Crutch SJ, Lees AJ, Morris HR (2016) Visual dysfunction in Parkinson’s disease. Brain 139(11):2827–2843. https://doi.org/10.1093/brain/aww175
Uc EY, Rizzo M, Anderson SW, Qian S, Rodnitzky RL, Dawson JD (2005) Visual dysfunction in Parkinson disease without dementia. Neurology 65(12):1907–1913. https://doi.org/10.1212/01.wnl.0000191565.11065.11
Davidsdottir S, Cronin-Golomb A, Lee A (2005) Visual and spatial symptoms in Parkinson’s disease. Vis Res 45(10):1285–1296. https://doi.org/10.1016/j.visres.2004.11.006
Owen AM (2004) Cognitive dysfunction in Parkinson’s disease: the role of frontostriatal circuitry. The Neuroscientist 10(6):525–537. https://doi.org/10.1177/1073858404266776
Jokinen P, Karrasch M, Bruck A, Johansson J, Bergman J, Rinne JO (2013) Cognitive slowing in Parkinson’s disease is related to frontostriatal dopaminergic dysfunction. J Neurol Sci 329(1–2):23–28. https://doi.org/10.1016/j.jns.2013.03.006
Ma LY, Chen XD, He Y, Ma HZ, Feng T (2017) Disrupted brain network hubs in subtype-specific Parkinson’s disease. Eur Neurol 78(3–4):200–209. https://doi.org/10.1159/000477902
Habas C, Kamdar N, Nguyen D, Prater K, Beckmann CF, Menon V, Greicius MD (2009) Distinct cerebellar contributions to intrinsic connectivity networks. J Neurosci 29(26):8586–8594. https://doi.org/10.1523/JNEUROSCI.1868-09.2009
Buckner RL, Krienen FM, Castellanos A, Diaz JC, Yeo BT (2011) The organization of the human cerebellum estimated by intrinsic functional connectivity. J Neurophysiol 106(5):2322–2345. https://doi.org/10.1152/jn.00339.2011
Eisinger RS, Hess CW, Martinez-Ramirez D, Almeida L, Foote KD, Okun MS, Gunduz A (2017) Motor subtype changes in early Parkinson’s disease. Parkinsonism Relat Disord 43:67–72. https://doi.org/10.1016/j.parkreldis.2017.07.018
Fereshtehnejad SM, Zeighami Y, Dagher A, Postuma RB (2017) Clinical criteria for subtyping Parkinson’s disease: biomarkers and longitudinal progression. Brain 140(7):1959–1976. https://doi.org/10.1093/brain/awx118
Rosenberg-Katz K, Herman T, Jacob Y, Giladi N, Hendler T, Hausdorff JM (2013) Gray matter atrophy distinguishes between Parkinson disease motor subtypes. Neurology 80(16):1476–1484. https://doi.org/10.1212/WNL.0b013e31828cfaa4
Chen HM, Wang ZJ, Fang JP, Gao LY, Ma LY, Wu T, Hou YN, Zhang JR, Feng T (2015) Different patterns of spontaneous brain activity between tremor-dominant and postural instability/gait difficulty subtypes of Parkinson’s disease: a resting-state fMRI study. CNS Neurosci Ther 21(10):855–866. https://doi.org/10.1111/cns.12464
Deng X, Xiao B, Li HH, Lo YL, Chew LM, Prakash KM, Tan EK (2015) Sexual dysfunction is associated with postural instability gait difficulty subtype of Parkinson’s disease. J Neurol 262(11):2433–2439. https://doi.org/10.1007/s00415-015-7855-8
Mohl B, Berman BD, Shelton E, Tanabe J (2017) Levodopa response differs in Parkinson’s motor subtypes: a task-based effective connectivity study. J Comp Neurol 525(9):2192–2201. https://doi.org/10.1002/cne.24197
Katz M, Luciano MS, Carlson K, Luo P, Marks WJ Jr, Larson PS, Starr PA, Follett KA, Weaver FM, Stern MB, Reda DJ, Ostrem JL, group CSPs (2015) Differential effects of deep brain stimulation target on motor subtypes in Parkinson’s disease. Ann Neurol 77(4):710–719. https://doi.org/10.1002/ana.24374
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was funded by the National Nature Science Foundation of China (No. 81571247) and the Fundamental Research Funds for the Central Universities (No. 2012017yjsy195).
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
ESM 1
(DOCX 128 kb)
Rights and permissions
About this article
Cite this article
Hou, Y., Ou, R., Yang, J. et al. Patterns of striatal and cerebellar functional connectivity in early-stage drug-naïve patients with Parkinson’s disease subtypes. Neuroradiology 60, 1323–1333 (2018). https://doi.org/10.1007/s00234-018-2101-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-018-2101-6