Abstract
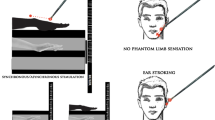
Phantom limb pain is a restricting condition for a substantial number of amputees with quite different characteristics of pain. Here, we report on a forearm amputee with constant phantom pain in the hand, in whom we could regularly elicit the rare phenomenon of referred cramping phantom pain by touching the face. To clarify the underlying mechanisms, we followed the cramp during the course of an axillary blockade of the brachial plexus. During the blockade, both phantom pain and the referred cramp were abolished, while a referred sensation of “being touched at the phantom” persisted. Furthermore, to identify the cortical substrate, we elicited the cramp during functional magnetic imaging. Imaging revealed that referred cramping phantom limb pain was associated with brain activation of the hand representation in the primary sensorimotor cortex. The results support the hypothesis that referred cramping phantom limb pain in this case is associated with a substantial brain activation in the hand area of the deafferented sensorimotor cortex. However, this alone is not sufficient to elicit referred cramping phantom limb pain. Peripheral inputs, both, from the arm nerves affected by the amputation and from the skin in the face at which the referred cramp is evoked, are a precondition for referred cramping phantom limb pain to occur, at least in this case.





Similar content being viewed by others
References
Devor M, Vaso A, Adahan HM, Vyshka G (2014) PNS origin of phantom limb sensation and pain: reply to Letter to the Editor regarding Foell et al. Peripheral origin of phantom limb pain: Is it all resolved? PAIN 155:2207–2208. https://doi.org/10.1016/j.pain.2014.08.018
Ephraim PL, Wegener ST, MacKenzie EJ, Dillingham TR, Pezzin LE (2005) Phantom pain, residual limb pain, and back pain in amputees: results of a national survey. Arch Phys Med Rehabil 86:1910–1919. https://doi.org/10.1016/j.apmr.2005.03.031 pii]
Flor H, Elbert T, Knecht S et al (1995) Phantom-limb pain as a perceptual correlate of cortical reorganization following arm amputation. Nature 375:482–484
Flor H, Nikolajsen L, Jensen TS (2006) Phantom limb pain: a case of maladaptive CNS plasticity? Nat Rev Neurosci 7:873–881. https://doi.org/10.1038/nrn1991
Flor H, Diers M, Andoh J (2013) The neural basis of phantom limb pain. Trends Cognit Sci 17:307–308
Foell J, Andoh J, Bekrater-Bodmann R, Diers M, Fuchs X, Colloca L, Flor H (2014) Peripheral origin of phantom limb pain: Is it all resolved? PAIN 155:2205–2206. https://doi.org/10.1016/j.pain.2014.08.028
Götz T, Huonker R, Miltner WH, Witte OW, Dettner K, Weiss T (2010) Task requirements change signal strength of the primary somatosensory M50: Oddball vs. one-back tasks. Psychophysiology. https://doi.org/10.1111/j.1469-8986.2010.01116.x
Kikkert S, Kolasinski J, Jbabdi S, Tracey I, Beckmann CF, Johansen-Berg H, Makin TR (2016) Revealing the neural fingerprints of a missing hand. Elife 5
Klingner CM, Hasler C, Brodoehl S, Witte OW (2010) Dependence of the negative BOLD response on somatosensory stimulus intensity. Neuroimage 53:189–195
Knecht S, Henningsen H, Elbert T et al (1995) Cortical reorganization in human amputees and mislocalization of painful stimuli to the phantom limb. Neurosci Lett 201:262–264
Knecht S, Henningsen H, Elbert T, Flor H, Hohling C, Pantev C, Taub E (1996) Reorganizational and perceptional changes after amputation. Brain 119:1213–1219
Knecht S, Henningsen H, Hohling C, Elbert T, Flor H, Pantev C, Taub E (1998) Plasticity of plasticity? Changes in the pattern of perceptual correlates of reorganization after amputation. Brain 121:717–724
Kuner R, Flor H (2017) Structural plasticity and reorganisation in chronic pain. Nat Rev Neurosci 18:20
Makin TR, Scholz J, Filippini N, Slater DH, Tracey I, Johansen-Berg H (2013) Phantom pain is associated with preserved structure and function in the former hand area. Nat Commun 4:1570. https://doi.org/10.1038/ncomms2571
Mercier C, Reilly KT, Vargas CD, Aballea A, Sirigu A (2006) Mapping phantom movement representations in the motor cortex of amputees. Brain 129:2202–2210
Preissler S, Dietrich C, Meissner W, Huonker R, Hofmann GO, Miltner WHR, Weiss T (2011) Brachial plexus block in phantom limb pain: a case report. Pain Med 12:1649–1654. https://doi.org/10.1111/j.1526-4637.2011.01247.x
Price DD, McGrath PA, Rafii A, Buckingham B (1983) The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain 17:45–56 doi. https://doi.org/10.1016/0304-3959(83)90126-4
Raffin E, Richard N, Giraux P, Reilly KT (2016) Primary motor cortex changes after amputation correlate with phantom limb pain and the ability to move the phantom limb. NeuroImage 130:134–144
Ramachandran VS (1993) Filling in gaps in perception: part II. Scotomas and phantom limbs. Curr Dir Psychol Sci 2:56–65
Ramachandran VS, Rogers-Ramachandran D, Cobb S (1995) Touching the phantom limb. Nature 377:489–490
Rolke R, Baron R, Maier C et al (2006) Quantitative sensory testing in the German Research Network on Neuropathic Pain (DFNS): Standardized protocol and reference values. Pain 123:231–243. https://doi.org/10.1016/j.pain.2006.01.041
Sens E, Knorr C, Preul C, Meissner W, Witte OW, Miltner WH, Weiss T (2013) Differences in somatosensory and motor improvement during temporary functional deafferentation in stroke patients and healthy subjects. Behav Brain Res 252:110–116
Sherman RA (ed) (1997) Phantom pain. Plenum Press, New York
Sherman RA, Gall N, Gormly J (1979) Treatment of phantom limb pain with muscular relaxation training to disrupt the pain-anxiety-tension cycle. Pain 6:47–55. https://doi.org/10.1016/0304-3959(79)90139-8
Vaso A, Adahan H-M, Gjika A, Zahaj S, Zhurda T, Vyshka G, Devor M (2014) Peripheral nervous system origin of phantom limb pain. Pain 155:1384–1391
Weiss T (2016) Plasticity and cortical reorganization associated with pain. Zeitschrift für Psychologie 224:71–79
Weiss T, Miltner WHR, Dillmann S, Meissner W, Huonker R, Nowak H (1998) Reorganization of the somatosensory cortex after amputation of the index finger. Neuro Rep 9:213–216
Weiss T, Miltner WHR, Liepert J, Meissner W, Taub E (2004) Rapid functional plasticity in the primary somatomotor cortex and perceptual changes after nerve block. Eur J Neurosci 20:3413–3423
Weiss T, Sens E, Teschner U, Meissner W, Preul C, Witte OW, Miltner WHR (2011) Deafferentation of the affected arm: a method to improve rehabilitation? Stroke 42:1363–1370. https://doi.org/10.1161/strokeaha.110.601138
Winter C, Fritzsche K, Karl A, Huse E, Larbig W, Grusser SM, Flor H (2001) The phantom and stump phenomena interview (PSPI). Schmerz 15:172–178
Acknowledgements
Thanks to Gerd F. Volk, Winfried Meissner, and Holger Hecht for help with data acquisition. This work was supported by the German Social Accident Insurance (DGUV-FR145 and FR196). DGUV neither influenced the study goals of study design; authors are fully responsible for goals, design, and results. The funding source had no involvement in the collection, analysis and interpretation of data; in the writing of the report; and in the decision to submit the article for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There is no conflict of interest for any author of this study.
Rights and permissions
About this article
Cite this article
Dietrich, C., Nehrdich, S., Zimmer, A. et al. Referred cramping phantom hand pain elicited in the face and eliminated by peripheral nerve block. Exp Brain Res 236, 1815–1824 (2018). https://doi.org/10.1007/s00221-018-5262-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-018-5262-y