Abstract
Rationale and objective
Estradiol decline has been associated with depression and anxiety in post-menopausal women. Agomelatine (Ago) is an agonist of the melatonergic MT1/MT2 receptors and an antagonist of the serotonergic 5-HT2c receptors. The present study aimed to evaluate the effects of combining Ago with 17β-estradiol (E2) on ovariectomy (OVX)-induced depressive- and anxiety-like behaviors in young adult female rats.
Methods
OVX rats were treated with Ago (40 mg/kg/day, p.o.) for 10 days starting 1 week after surgery alone or combined with two doses of E2 (40 μg/kg/day, s.c.) given before behavioral testing.
Results
Co-administration of E2 enhanced the anti-depressant and anxiolytics effects of Ago as evidenced by decreased immobility time in the forced swimming test, as well as increased time spent in the open arms and number of entries to open arms in the elevated plus-maze. In parallel, Ago increased hippocampal norepinephrine, dopamine, melatonin, and brain-derived neurotrophic factor (BDNF). Meanwhile, Ago-treated rats exhibited reduced hippocampal nuclear factor kappa beta (NF-kB) P65 expression and pro-inflammatory cytokine level. Ago upregulated estrogen receptor (ER α and β) mRNA expression in the hippocampus of OVX rats and elevated serum estradiol levels. Co-administration of E2 with Ago synergistically decreased NF-kB P65 expression and pro-inflammatory cytokines, and increased BDNF levels.
Conclusion
E2 augmented the neuroprotective effect of Ago in OVX rats via its anti-inflammatory and neurotrophic effects. The combined treatment of E2 and Ago should be further investigated as a treatment of choice for depression, anxiety, and sleep disturbances associated with menopause.








Similar content being viewed by others
References
AlAhmed S, Herbert J (2010) Effect of agomelatine and its interaction with the daily corticosterone rhythm on progenitor cell proliferation in the dentate gyrus of the adult rat. Neuropharmacology 59:375–379. https://doi.org/10.1016/j.neuropharm.2010.05.008
Ali AA (2016) Comparative study on the activity of agomelatine and/or curcumin against development of depression in rats. Acta Psychopathol 2:1–13. https://doi.org/10.4172/2469-6676.100059
Arevalo MA, Azcoitia I, Garcia-Segura LM (2015) The neuroprotective actions of oestradiol and oestrogen receptors. Nat Rev Neurosci 16:17–29
Autry AE, Monteggia LM (2012) Brain-derived neurotrophic factor and neuropsychiatric disorders. Pharmacol Rev 64:238–258. https://doi.org/10.1124/pr.111.005108
Baber RJ, Panay N, Fenton A (2016) 2016 IMS recommendations on women’s midlife health and menopause hormone therapy. Climacteric 19:109–150. https://doi.org/10.3109/13697137.2015.1129166
Bourin M, Mocaër E, Porsolt R (2004) Antidepressant-like activity of S 20098 (agomelatine) in the forced swimming test in rodents: involvement of melatonin and serotonin receptors. J Psychiatry Neurosci 29:126–133
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254. https://doi.org/10.1016/0003-2697(76)90527-3
Casarrubea M, Roy V, Sorbera F, Magnusson MS, Santangelo A, Arabo A, Crescimanno G (2013) Temporal structure of the rat’s behavior in elevated plus maze test. Behav Brain Res 237:290–299. https://doi.org/10.1016/j.bbr.2012.09.049
Chou C-H, Ko H-C, Wu JY-W, Chang FM, Tung YY (2015) Effect of previous diagnoses of depression, menopause status, vasomotor symptoms, and neuroticism on depressive symptoms among climacteric women: a 30-month follow-up. Taiwan J Obstet Gynecol 54:385–389. https://doi.org/10.1016/j.tjog.2015.03.004
Cos S, Gonzalez A, Martinez-Campa C, Mediavilla M, Alonso-Gonzalez C, Sanchez-Barcelo E (2008) Melatonin as a selective estrogen enzyme modulator. Curr Cancer Drug Targets 8:691–702. https://doi.org/10.2174/156800908786733469
De Berardis D, Fornaro M, Serroni N et al (2015) Agomelatine beyond borders: current evidences of its efficacy in disorders other than major depression. Int J Mol Sci 16:1111–1130. https://doi.org/10.3390/ijms16011111
Duman RS, Aghajanian GK, Sanacora G, Krystal JH (2016) Synaptic plasticity and depression: new insights from stress and rapid-acting antidepressants. Nat Med 22:238–249. https://doi.org/10.1038/nm.4050
Estrada-Camarena E, Lopez-Rubalcava C, Vega-Rivera N et al (2010) Antidepressant effects of estrogens: a basic approximation. Behav Pharmacol 21:451–464. https://doi.org/10.1097/FBP.0b013e32833db7e9
Faraguna U, Vyazovskiy VV, Nelson AB, Tononi G, Cirelli C (2008) A causal role for brain-derived neurotrophic factor in the homeostatic regulation of sleep. J Neurosci 28:4088–4095. https://doi.org/10.1523/JNEUROSCI.5510-07.2008
Felger JC (2017) Imaging the role of inflammation in mood and anxiety-related disorders. Curr Neuropharmacol 15:533–558. https://doi.org/10.2174/1570159X15666171123201142
Franklin TC, Xu C, Duman RS (2017) Depression and sterile inflammation: essential role of danger associated molecular patterns. Brain Behav Immun 72:2–13. https://doi.org/10.1016/j.bbi.2017.10.025
Hansen CH, Larsen LW, Sørensen AM, Halling-Sørensen B, Styrishave B (2017) The six most widely used selective serotonin reuptake inhibitors decrease androgens and increase estrogens in the H295R cell line. Toxicol In Vitro 41:1–11. https://doi.org/10.1016/j.tiv.2017.02.001
Hassan WA, Rahman ZA (2016) Possible protective effects of agomelatine against paracetamol induced toxicity in rats. International Journal of Scientific and Research Publications 6:471–479
Hickie IB, Rogers NL (2011) Novel melatonin-based therapies: potential advances in the treatment of major depression. Lancet 378:621–631. https://doi.org/10.1016/S0140-6736(11)60095-0
Holm L, Liang W, Thorsell A, Hilke S (2014) Acute effects on brain cholecystokinin-like concentration and anxiety-like behaviour in the female rat upon a single injection of 17β-estradiol. Pharmacol Biochem Behav 122:222–227. https://doi.org/10.1016/j.pbb.2014.04.004
Huang P, Gao T, Dong Z, Zhou C, Lai Y, Pan T, Liu Y, Zhao X, Sun X, Hua H, Wen G, Gao L, Lv Z (2018) Neural circuitry among connecting the hippocampus, prefrontal cortex and basolateral amygdala in a mouse depression model: associations correlations between BDNF levels and BOLD – fMRI signals. Brain Res Bull 142:107–115. https://doi.org/10.1016/j.brainresbull.2018.06.019
Ibrahim WW, Safar MM, Khattab MM, Agha AM (2016) 17β-Estradiol augments antidepressant efficacy of escitalopram in ovariectomized rats: neuroprotective and serotonin reuptake transporter modulatory effects. Psychoneuroendocrinology 74:240–250. https://doi.org/10.1016/j.psyneuen.2016.09.013
Jehan S, Masters-Isarilov A, Salifu I et al (2015) Sleep disorders in postmenopausal women. J Sleep Disord Ther 4. https://doi.org/10.4172/2167-0277.1000212
Jehan S, Jean-Louis G, Zizi F et al (2017) Sleep, melatonin, and the menopausal transition: what are the links? Sleep Sci 10:11–18. https://doi.org/10.5935/1984-0063.20170003
Khajuria DK, Razdan R, Mahapatra DR (2012) Description of a new method of ovariectomy in female rats. Revista Brasileira de Reumatologia 52:462–466
Kiss Á, Delattre AM, Pereira SIR, Carolino RG, Szawka RE, Anselmo-Franci JA, Zanata SM, Ferraz AC (2012) 17β-Estradiol replacement in young, adult and middle-aged female ovariectomized rats promotes improvement of spatial reference memory and an antidepressant effect and alters monoamines and BDNF levels in memory- and depression-related brain areas. Behav Brain Res 227:100–108. https://doi.org/10.1016/j.bbr.2011.10.047
Lalert L, Kruevaisayawan H, Amatyakul P, Ingkaninan K, Khongsombat O (2018) Neuroprotective effect of Asparagus racemosus root extract via the enhancement of brain-derived neurotrophic factor and estrogen receptor in ovariectomized rats. J Ethnopharmacol 225:336–341. https://doi.org/10.1016/j.jep.2018.07.014
Lasota A (2004) Experimental osteoporosis- different methods of ovariectomy in female white rats. Roczniki Akademii Medycznej w Białymstoku (1995) 49:129–131
Liu Y, Ni C, Li Z, Yang N, Zhou Y, Rong X, Qian M, Chui D, Guo X (2017) Prophylactic melatonin attenuates Isoflurane-induced cognitive impairment in aged rats through hippocampal melatonin receptor 2 – cAMP response element binding signalling. Basic Clin Pharmacol Toxicol 120:219–226. https://doi.org/10.1111/bcpt.12652
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and. Methods 25:402–408. https://doi.org/10.1006/meth.2001.1262
Loiseau F, Le Bihan C, Hamon M, Thiébot MH (2006) Effects of melatonin and agomelatine in anxiety-related procedures in rats: interaction with diazepam. Eur Neuropsychopharmacol 16:417–428. https://doi.org/10.1016/j.euroneuro.2005.11.007
Lopes J, Arnosti D, Trosko JE et al (2016) Melatonin decreases estrogen receptor binding to estrogen response elements sites on the OCT4 gene in human breast cancer stem cells. Genes Cancer 7. https://doi.org/10.18632/genesandcancer.107
Lu J, Xu Y, Hu W, Gao Y, Ni X, Sheng H, Liu Y (2014) Exercise ameliorates depression-like behavior and increases hippocampal BDNF level in ovariectomized rats. Neurosci Lett 573:13–18. https://doi.org/10.1016/j.neulet.2014.04.053
Maldonado-Bouchard S, Peters K, Woller SA, Madahian B, Faghihi U, Patel S, Bake S, Hook MA (2016) Inflammation is increased with anxiety- and depression-like signs in a rat model of spinal cord injury. Brain Behav Immun 51:176–195. https://doi.org/10.1016/j.bbi.2015.08.009
Mbchb JS, Lecturer C (2016) Maturitas depression in midlife women. Maturitas 94:149–154. https://doi.org/10.1016/j.maturitas.2016.09.004
Millan MJ, Gobert A, Lejeune F, Dekeyne A, Newman-Tancredi A, Pasteau V, Rivet JM, Cussac D (2003) The novel melatonin agonist agomelatine (S20098) is an antagonist at 5-hydroxytryptamine2C receptors, blockade of which enhances the activity of frontocortical dopaminergic and adrenergic pathways. J Pharmacol Exp Ther 306:954–964. https://doi.org/10.1124/jpet.103.051797
Millan MJ, Brocco M, Gobert A, Dekeyne A (2005) Anxiolytic properties of agomelatine, an antidepressant with melatoninergic and serotonergic properties: role of 5-HT2C receptor blockade. Psychopharmacology 177:448–458. https://doi.org/10.1007/s00213-004-1962-z
Miller AH, Raison CL (2016) The role of inflammation in depression: from evolutionary imperative to modern treatment target. Nat Rev Immunol 16:22–34
Modder U, Riggs B, Spelsberg T et al (2004) Dose-response of estrogen on bone versus the uterus in ovariectomized mice. Eur J Endocrinol:503–510. https://doi.org/10.1530/eje.0.1510503
Molteni R, Macchi F, Zecchillo C, Dell’Agli M, Colombo E, Calabrese F, Guidotti G, Racagni G, Riva MA (2013) Modulation of the in fl ammatory response in rats chronically treated with the antidepressant agomelatine. Eur Neuropsychopharmacol 23:1645–1655. https://doi.org/10.1016/j.euroneuro.2013.03.008
Murphy AJ, Guyre PM, Pioli PA (2010) Estradiol suppresses NF- B activation through coordinated regulation of let-7a and miR-125b in primary human macrophages. J Immunol 184:5029–5037
Nadar JS, Kale PP, Kadu PK, Prabhavalkar K, Dhangar R (2018) Potentiation of antidepressant effects of agomelatine and bupropion by hesperidin in mice. Neurol Res Int 2018:1–7. https://doi.org/10.1155/2018/9828639
Plesničar BK (2014) Efficacy and tolerability of agomelatine in the treatment of depression. Patient Prefer Adherence 8:603–612. https://doi.org/10.2147/PPA.S42789
Racagni G, Riva MA, Molteni R, Musazzi L, Calabrese F, Popoli M, Tardito D (2011) Mode of action of agomelatine: synergy between melatonergic and 5-HT 2C receptors. World J Biol Psychiatry 12:574–587
Raedler TJ (2011) Inflammatory mechanisms in major depressive disorder. Curr Opin Psychiatry 24:519–525. https://doi.org/10.1097/YCO.0b013e32834b9db6
Rakofsky JJ, Holtzheimer PE, Nemeroff CB (2009) Emerging targets for antidepressant therapies. Curr Opin Chem Biol 13:291–302. https://doi.org/10.1016/j.cbpa.2009.04.617
Rasheed NOA, El Sayed NS, El-khatib AS (2018) Progress in neuropsychopharmacology & biological psychiatry targeting central β 2 receptors ameliorates streptozotocin-induced neuroin fl ammation via inhibition of glycogen synthase kinase3 pathway in mice. Prog Neuro-Psychopharmacol Biol Psychiatry 86:65–75. https://doi.org/10.1016/j.pnpbp.2018.05.010
Riazi K, Galic MA, Kentner AC, Reid AY, Sharkey KA, Pittman QJ (2015) Microglia-dependent alteration of glutamatergic synaptic transmission and plasticity in the hippocampus during peripheral inflammation. J Neurosci 35:4942–4952. https://doi.org/10.1523/JNEUROSCI.4485-14.2015
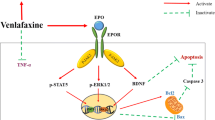
Saad MA, El-Sahar AE, Sayed RH et al (2019) Venlafaxine mitigates depressive-like behavior in ovariectomized rats by activating the EPO/EPOR/JAK2 signaling pathway and increasing the serum estradiol level. Neurotherapeutics 16:404–415. https://doi.org/10.1007/s13311-018-00680-6
Sales S, Ureshino RP, Pereira RT d S et al (2010) Effects of 17β-estradiol replacement on the apoptotic effects caused by ovariectomy in the rat hippocampus. Life Sci 86:832–838. https://doi.org/10.1016/j.lfs.2010.04.002
Sárvári M, Kalló I, Hrabovszky E, Solymosi N, Rodolosse A, Liposits Z (2016) Long-term estrogen receptor beta agonist treatment modifies the hippocampal transcriptome in middle-aged ovariectomized rats. Front Cell Neurosci 10. https://doi.org/10.3389/fncel.2016.00149
Selli J, Unal D, Mercantepe F, Akaras N, Kabayel R, Unal B, Atilay H (2016) Protective effects of beta glucan in brain tissues of post-menopausal rats: a histochemical and ultra-structural study. Gynecol Endocrinol 32:234–239. https://doi.org/10.3109/09513590.2015.1110139
Seo SY, Moon J-Y, Kang S-Y, Kwon OS, Kwon S, Bang S, Kim SP, Choi KH, Ryu Y (2018) An estradiol-independent BDNF-NPY cascade is involved in the antidepressant effect of mechanical acupuncture instruments in ovariectomized rats. Sci Rep 8:5849. https://doi.org/10.1038/s41598-018-23824-2
Sharma R, Sharma NK, Thungapathra M (2017) Resveratrol regulates body weight in healthy and ovariectomized rats. Nutr Metab (Lond) 14:30. https://doi.org/10.1186/s12986-017-0183-5
Shirayama Y, Chen AC-H, Nakagawa S, Russell DS, Duman RS (2002) Brain-derived neurotrophic factor produces antidepressant effects in behavioral models of depression. J Neurosci 22:3251–3261. https://doi.org/10.1523/JNEUROSCI.22-08-03251.2002
Su Q, Cheng Y, Jin K, Cheng J, Lin Y, Lin Z, Wang L, Shao B (2016) Estrogen therapy increases BDNF expression and improves post-stroke depression in ovariectomy-treated rats. Exp Ther Med 12:1843–1848. https://doi.org/10.3892/etm.2016.3531
Tchekalarova J, Atanasova D, Kortenska L, Atanasova M, Lazarov N (2018) Chronic agomelatine treatment prevents comorbid depression in the post-status epilepticus model of acquired epilepsy through suppression of inflammatory signaling. Neurobiol Dis 115:127–144. https://doi.org/10.1016/j.nbd.2018.04.005
Tuma J, Strubbe JH, Mocaër E, Koolhaas JM (2005) Anxiolytic-like action of the antidepressant agomelatine (S 20098) after a social defeat requires the integrity of the SCN. Eur Neuropsychopharmacol 15:545–555. https://doi.org/10.1016/j.euroneuro.2005.02.004
Vegeto E, Belcredito S, Etteri S, Ghisletti S, Brusadelli A, Meda C, Krust A, Dupont S, Ciana P, Chambon P, Maggi A (2003) Estrogen receptor- mediates the brain antiinflammatory activity of estradiol. Proc Natl Acad Sci 100:9614–9619. https://doi.org/10.1073/pnas.1531957100
Vegeto E, Benedusi V, Maggi A (2008) Estrogen anti-inflammatory activity in brain: a therapeutic opportunity for menopause and neurodegenerative diseases. Front Neuroendocrinol 29:507–519. https://doi.org/10.1016/j.yfrne.2008.04.001
Walf AA, Frye CA (2006) A review and update of mechanisms of estrogen in the hippocampus and amygdala for anxiety and depression behavior. Neuropsychopharmacology 31:1097–1111. https://doi.org/10.1038/sj.npp.1301067
Walsh RN, Cummins RA (1976) The open-field test: a critical review. Psychol Bull 83:482–504. https://doi.org/10.1037/0033-2909.83.3.482
Yang J, Jin HJ, Mocaër E, Seguin L, Zhao H, Rusak B (2016) Agomelatine affects rat suprachiasmatic nucleus neurons via melatonin and serotonin receptors. Life Sci 155:147–154. https://doi.org/10.1016/j.lfs.2016.04.035
Yanguas-Casás N, Brocca ME, Azcoitia I, et al (2019) Estrogenic regulation of neuroprotective and neuroinflammatory mechanisms: implications for depression and cognition. In: Brinton R., Genazzani A., Simoncini T., Stevenson J. (eds) Sex Steroids' Effects on Brain, Heart and Vessels. ISGE Series. Springer, Cham
Zemo Gamo F, Djiogue S, Magloire KWGJ et al (2017) Fourteen days post-ovariectomy estrogens decline is associated with anxiogenic effects on Wistar rats. J Pharm Pharmacol 5:869–876. https://doi.org/10.17265/2328-2150/2017.12.004
Zhou B, Xie S, Hu J, Sun X, Guan H, Deng Y (2014) Paroxetine increased the serum estrogen in postmenopausal women with depressive and anxiety symptoms. Open J Depress 3:184–194
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The protocol of this study complies with the US National Institute of Health (NIH publication No. 85-23, revised 2011) and approved by the Committee of Animal Care and Use of Faculty of Pharmacy, Cairo University (Permit number: PT 2035).
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
El-Khatib, Y.A., Sayed, R.H., Sallam, N.A. et al. 17β-Estradiol augments the neuroprotective effect of agomelatine in depressive- and anxiety-like behaviors in ovariectomized rats. Psychopharmacology 237, 2873–2886 (2020). https://doi.org/10.1007/s00213-020-05580-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-020-05580-2