Abstract
Summary
This study investigated the efficacy of annual zoledronic acid (ZOL) administration against previously treated recompression vertebral fractures (RVF) and new vertebral fractures (NVF) in initial percutaneous kyphoplasty (PKP) patients with osteoporotic vertebral compression fractures (OVCF) over a 3-year follow-up period.
Introduction
Although PKP achieves a satisfactory outcome, previously treated RVF and NVF can limit its effectiveness. The annual infusion of ZOL over 3 years can improve fracture protection, particularly in the vertebrae. We hypothesized that ZOL can reduce the incidence of RVFs and/or NVFs, and improve the clinical outcomes of PKP.
Methods
This was a placebo-controlled, double-blind prospective trial of 154 PKP patients (mean age: 70 years) with OVCFs. Patients were randomly assigned to receive a single infusion of ZOL (5 mg) or placebo (78 ZOL vs. 76 placebo) at 1 week, 12 months, and 24 months after surgery. Patients were followed-up for 36 months.
Results
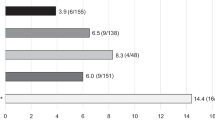
ZOL treatment lowered the risk of RVF by ~ 65% over the 36-month period when compared to placebo controls (6.41% in ZOL vs. 18.42% in placebo groups; relative risk, 0.35; 95% CI, 0.13 to 0.92). ZOL also reduced the risk of NVF by ~ 73% (3.85% in ZOL vs. 14.47% in placebo groups; relative risk, 0.27; 95% CI, 0.08 to 0.92). ZOL also significantly reduced the vertebral height lost rate (HLR) at 12, 24, and 36 months. ZOL also improved the visual analog scale (VAS), Oswestry disability index (ODI) scores, and bone mineral density (BMD).
Conclusion
Annual ZOL administration significantly lowers the risk of RVFs and NVFs, improving the clinical outcome of initial PKP in patients with OVCFs over a 3-year follow-up period.
Trial registration
ChiCTR2000029307




Similar content being viewed by others
References
Curtis EM, Moon RJ, Dennison EM, Harvey NC, Cooper C (2016) Recent advances in the pathogenesis and treatment of osteoporosis. Clin Med (London, England) 16(4):360–364. https://doi.org/10.7861/clinmedicine.16-4-360
Johnell O, Kanis JA (2006) An estimate of the worldwide prevalence and disability associated with osteoporotic fractures. Osteoporos Int 17(12):1726–1733. https://doi.org/10.1007/s00198-006-0172-4
Pluijm SM, Dik MG, Jonker C, Deeg DJ, van Kamp GJ, Lips P (2002) Effects of gender and age on the association of apolipoprotein E epsilon4 with bone mineral density, bone turnover and the risk of fractures in older people. Osteoporos Int 13(9):701–709. https://doi.org/10.1007/s001980200096
Robbins J, Hirsch C, Whitmer R, Cauley J, Harris T (2001) The association of bone mineral density and depression in an older population. J Am Geriatr Soc 49(6):732–736. https://doi.org/10.1046/j.1532-5415.2001.49149.x
Lyles KW (2001) Osteoporosis and depression: shedding more light upon a complex relationship. J Am Geriatr Soc 49(6):827–828. https://doi.org/10.1046/j.1532-5415.2001.49162.x
Tosteson AN, Gabriel SE, Grove MR, Moncur MM, Kneeland TS, Melton LJ 3rd (2001) Impact of hip and vertebral fractures on quality-adjusted life years. Osteoporos Int 12(12):1042–1049. https://doi.org/10.1007/s001980170015
Adachi JD, Ioannidis G, Olszynski WP, Brown JP, Hanley DA, Sebaldt RJ, Petrie A, Tenenhouse A, Stephenson GF, Papaioannou A, Guyatt GH, Goldsmith CH (2002) The impact of incident vertebral and non-vertebral fractures on health related quality of life in postmenopausal women. BMC Musculoskelet Disord 3:11. https://doi.org/10.1186/1471-2474-3-11
Chang W, Zhang X, Jiao N, Yuwen P, Zhu Y, Zhang F, Chen W (2017) Unilateral versus bilateral percutaneous kyphoplasty for osteoporotic vertebral compression fractures: a meta-analysis. Medicine (Baltimore) 96(17):e6738. https://doi.org/10.1097/md.0000000000006738
Garfin SR, Yuan HA, Reiley MA (2001) New technologies in spine: kyphoplasty and vertebroplasty for the treatment of painful osteoporotic compression fractures. Spine 26(14):1511–1515. https://doi.org/10.1097/00007632-200107150-00002
Belkoff SM, Mathis JM, Fenton DC, Scribner RM, Reiley ME, Talmadge K (2001) An ex vivo biomechanical evaluation of an inflatable bone tamp used in the treatment of compression fracture. Spine 26(2):151–156. https://doi.org/10.1097/00007632-200101150-00008
Bouza C, Lopez T, Magro A, Navalpotro L, Amate JM (2006) Efficacy and safety of balloon kyphoplasty in the treatment of vertebral compression fractures: a systematic review. Eur Spine J 15(7):1050–1067. https://doi.org/10.1007/s00586-005-0048-x
Eck JC, Nachtigall D, Humphreys SC, Hodges SD (2008) Comparison of vertebroplasty and balloon kyphoplasty for treatment of vertebral compression fractures: a meta-analysis of the literature. Spine J 8(3):488–497. https://doi.org/10.1016/j.spinee.2007.04.004
Trout AT, Kallmes DF (2006) Does vertebroplasty cause incident vertebral fractures? A review of available data. AJNR Am J Neuroradiol 27(7):1397–1403
Lamy O, Uebelhart B, Aubry-Rozier B (2014) Risks and benefits of percutaneous vertebroplasty or kyphoplasty in the management of osteoporotic vertebral fractures. Osteoporos Int 25(3):807–819. https://doi.org/10.1007/s00198-013-2574-4
Jansen JP, Bergman GJD, Huels J, Olson M (2011) The efficacy of bisphosphonates in the prevention of vertebral, hip, and nonvertebral-nonhip fractures in osteoporosis: a network meta-analysis. Semin Arthritis Rheum 40(4):275–284. https://doi.org/10.1016/j.semarthrit.2010.06.001
Byun JH, Jang S, Lee S, Park S, Yoon HK, Yoon BH, Ha YC (2017) The efficacy of bisphosphonates for prevention of osteoporotic fracture: an update meta-analysis. J Bone Metab 24(1):37–49. https://doi.org/10.11005/jbm.2017.24.1.37
Maricic M (2010) The role of zoledronic acid in the management of osteoporosis. Clin Rheumatol 29(10):1079–1084. https://doi.org/10.1007/s10067-010-1486-3
Kim YY, Rhyu KW (2010) Recompression of vertebral body after balloon kyphoplasty for osteoporotic vertebral compression fracture. Eur Spine J 19(11):1907–1912. https://doi.org/10.1007/s00586-010-1479-6
Hou Y, Yao Q, Zhang G, Ding L, Huang H (2018) Polymethylmethacrylate distribution is associated with recompression after vertebroplasty or kyphoplasty for osteoporotic vertebral compression fractures: a retrospective study. PLoS One 13(6):e0198407. https://doi.org/10.1371/journal.pone.0198407
Black DM, Delmas PD, Eastell R, Reid IR, Boonen S, Cauley JA, Cosman F, Lakatos P, Leung PC, Man Z, Mautalen C, Mesenbrink P, Hu H, Caminis J, Tong K, Rosario-Jansen T, Krasnow J, Hue TF, Sellmeyer D, Eriksen EF, Cummings SR, Trial HPF (2007) Once-yearly zoledronic acid for treatment of postmenopausal osteoporosis. N Engl J Med 356(18):1809–1822. https://doi.org/10.1056/NEJMoa067312
Heo DH, Chin DK, Yoon YS, Kuh SU (2009) Recollapse of previous vertebral compression fracture after percutaneous vertebroplasty. Osteoporos Int 20(3):473–480. https://doi.org/10.1007/s00198-008-0682-3
Black DM, Palermo L, Nevitt MC, Genant HK, Christensen L, Cummings SR (1999) Defining incident vertebral deformity: a prospective comparison of several approaches. The Study of Osteoporotic Fractures Research Group. J Bone Miner Res 14(1):90–101. https://doi.org/10.1359/jbmr.1999.14.1.90
Jensen MP, Karoly P, Braver S (1986) The measurement of clinical pain intensity: a comparison of six methods. Pain 27(1):117–126. https://doi.org/10.1016/0304-3959(86)90228-9
Fairbank JC, Couper J, Davies JB, O’Brien JP (1980) The Oswestry low back pain disability questionnaire. Physiotherapy 66(8):271–273
Reginster J, Minne HW, Sorensen OH, Hooper M, Roux C, Brandi ML, Lund B, Ethgen D, Pack S, Roumagnac I, Eastell R (2000) Randomized trial of the effects of risedronate on vertebral fractures in women with established postmenopausal osteoporosis. Vertebral Efficacy with Risedronate Therapy (VERT) Study Group. Osteoporos Int 11(1):83–91. https://doi.org/10.1007/s001980050010
Harris ST, Watts NB, Genant HK, McKeever CD, Hangartner T, Keller M, Chesnut CH 3rd, Brown J, Eriksen EF, Hoseyni MS, Axelrod DW, Miller PD (1999) Effects of risedronate treatment on vertebral and nonvertebral fractures in women with postmenopausal osteoporosis: a randomized controlled trial. Vertebral Efficacy With Risedronate Therapy (VERT) Study Group. Jama 282(14):1344–1352. https://doi.org/10.1001/jama.282.14.1344
Chesnut CH 3rd, Skag A, Christiansen C, Recker R, Stakkestad JA, Hoiseth A, Felsenberg D, Huss H, Gilbride J, Schimmer RC, Delmas PD (2004) Effects of oral ibandronate administered daily or intermittently on fracture risk in postmenopausal osteoporosis. J Bone Miner Res Off J Am Soc Bone Miner Res 19(8):1241–1249. https://doi.org/10.1359/jbmr.040325
Miller PD, McClung MR, Macovei L, Stakkestad JA, Luckey M, Bonvoisin B, Reginster JY, Recker RR, Hughes C, Lewiecki EM, Felsenberg D, Delmas PD, Kendler DL, Bolognese MA, Mairon N, Cooper C (2005) Monthly oral ibandronate therapy in postmenopausal osteoporosis: 1-year results from the MOBILE study. J Bone Miner Res 20(8):1315–1322. https://doi.org/10.1359/jbmr.050313
Reginster JY, Adami S, Lakatos P, Greenwald M, Stepan JJ, Silverman SL, Christiansen C, Rowell L, Mairon N, Bonvoisin B, Drezner MK, Emkey R, Felsenberg D, Cooper C, Delmas PD, Miller PD (2006) Efficacy and tolerability of once-monthly oral ibandronate in postmenopausal osteoporosis: 2 year results from the MOBILE study. Ann Rheum Dis 65(5):654–661. https://doi.org/10.1136/ard.2005.044958
Hadji P, Gamerdinger D, Spieler W, Kann PH, Loeffler H, Articus K, Möricke R, Ziller V (2012) Rapid Onset and Sustained Efficacy (ROSE) study: results of a randomised, multicentre trial comparing the effect of zoledronic acid or alendronate on bone metabolism in postmenopausal women with low bone mass. Osteoporos Int 23(2):625–633. https://doi.org/10.1007/s00198-011-1583-4
Black DM, Reid IR, Cauley JA, Cosman F, Leung PC, Lakatos P, Lippuner K, Cummings SR, Hue TF, Mukhopadhyay A, Tan M, Aftring RP, Eastell R (2015) The effect of 6 versus 9 years of zoledronic acid treatment in osteoporosis: a randomized second extension to the HORIZON-Pivotal Fracture Trial (PFT). Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research 30(5):934–944. https://doi.org/10.1002/jbmr.2442
Bell KJ, Hayen A, Glasziou P, Irwig L, Eastell R, Harrison SL, Black DM, Bauer DC (2016) Potential usefulness of BMD and bone turnover monitoring of zoledronic acid therapy among women with osteoporosis: secondary analysis of randomized controlled trial data. Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research 31(9):1767–1773. https://doi.org/10.1002/jbmr.2847
Jacques RM, Boonen S, Cosman F, Reid IR, Bauer DC, Black DM, Eastell R (2012) Relationship of changes in total hip bone mineral density to vertebral and nonvertebral fracture risk in women with postmenopausal osteoporosis treated with once-yearly zoledronic acid 5 mg: the HORIZON-Pivotal Fracture Trial (PFT). J Bone Miner Res 27(8):1627–1634. https://doi.org/10.1002/jbmr.1644
Brown DB, Gilula LA, Sehgal M, Shimony JS (2004) Treatment of chronic symptomatic vertebral compression fractures with percutaneous vertebroplasty. AJR Am J Roentgenol 182(2):319–322. https://doi.org/10.2214/ajr.182.2.1820319
Crandall D, Slaughter D, Hankins PJ, Moore C, Jerman J (2004) Acute versus chronic vertebral compression fractures treated with kyphoplasty: early results. Spine J 4(4):418–424. https://doi.org/10.1016/j.spinee.2004.01.003
Kaufmann TJ, Jensen ME, Schweickert PA, Marx WF, Kallmes DF (2001) Age of fracture and clinical outcomes of percutaneous vertebroplasty. AJNR Am J Neuroradiol 22(10):1860–1863
Hey HW, Tan JH, Tan CS, Tan HM, Lau PH, Hee HT (2015) Subsequent vertebral fractures post cement augmentation of the thoracolumbar spine: does it correlate with level-specific bone mineral density scores? Spine 40(24):1903–1909. https://doi.org/10.1097/brs.0000000000001066
Kim MJ, Lindsey DP, Hannibal M, Alamin TF (2006) Vertebroplasty versus kyphoplasty: biomechanical behavior under repetitive loading conditions. Spine 31(18):2079–2084. https://doi.org/10.1097/01.brs.0000231714.15876.76
Pflugmacher R, Schroeder RJ, Klostermann CK (2006) Incidence of adjacent vertebral fractures in patients treated with balloon kyphoplasty: two years’ prospective follow-up. Acta Radiol (Stockholm, Sweden : 1987) 47(8):830–840. https://doi.org/10.1080/02841850600854928
Johnell O, Oden A, Caulin F, Kanis JA (2001) Acute and long-term increase in fracture risk after hospitalization for vertebral fracture. Osteoporos Int 12(3):207–214. https://doi.org/10.1007/s001980170131
Kaptoge S, Armbrecht G, Felsenberg D, Lunt M, O'Neill TW, Silman AJ, Reeve J (2004) When should the doctor order a spine X-ray? Identifying vertebral fractures for osteoporosis care: results from the European Prospective Osteoporosis Study (EPOS). Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research 19(12):1982–1993. https://doi.org/10.1359/jbmr.040901
Boger A, Heini P, Windolf M, Schneider E (2007) Adjacent vertebral failure after vertebroplasty: a biomechanical study of low-modulus PMMA cement. Eur Spine J 16(12):2118–2125. https://doi.org/10.1007/s00586-007-0473-0
Pitton MB, Herber S, Bletz C, Drees P, Morgen N, Koch U, Bohm B, Eckardt A, Duber C (2008) CT-guided vertebroplasty in osteoprotic vertebral fractures: incidence of secondary fractures and impact of intradiscal cement leakages during follow-up. Eur J Radiol 18(1):43–50. https://doi.org/10.1007/s00330-007-0694-y
Hansson TH, Roos BO, Nachemson A (1975) Development of osteopenia in the fourth lumbar vertebra during prolonged bed rest after operation for scoliosis. Acta Orthop Scand 46(4):621–630. https://doi.org/10.3109/17453677508989244
Genant HK, Delmas PD, Chen P, Jiang Y, Eriksen EF, Dalsky GP, Marcus R, San Martin J (2007) Severity of vertebral fracture reflects deterioration of bone microarchitecture. Osteoporos Int 18(1):69–76. https://doi.org/10.1007/s00198-006-0199-6
Lips P, Cooper C, Agnusdei D, Caulin F, Egger P, Johnell O, Kanis JA, Liberman U, Minne H, Reeve J, Reginster JY, de Vernejoul MC, Wiklund I (1997) Quality of life as outcome in the treatment of osteoporosis: the development of a questionnaire for quality of life by the European Foundation for Osteoporosis. Osteoporos Int 7(1):36–38. https://doi.org/10.1007/bf01623457
Li HM, Zhang RJ, Gao H, Jia CY, Zhang JX, Dong FL, Shen CL (2018) New vertebral fractures after osteoporotic vertebral compression fracture between balloon kyphoplasty and nonsurgical treatment PRISMA. Medicine (Baltimore) 97(40):e12666. https://doi.org/10.1097/md.0000000000012666
Zhang J, Zhang T, Xu X, Cai Q, Zhao D (2019) Zoledronic acid combined with percutaneous kyphoplasty in the treatment of osteoporotic compression fracture in a single T12 or L1 vertebral body in postmenopausal women. Osteoporos Int 30(7):1475–1480. https://doi.org/10.1007/s00198-019-04896-w
Shi C, Zhang M, Cheng AY, Huang ZF (2018) Percutaneous kyphoplasty combined with zoledronic acid infusion in the treatment of osteoporotic thoracolumbar fractures in the elderly. Clin Interv Aging 13:853–861. https://doi.org/10.2147/CIA.S146871
Huang ZF, Xiao SX, Liu K, Xiong W (2019) Effectiveness analysis of percutaneous kyphoplasty combined with zoledronic acid in treatment of primary osteoporotic vertebral compression fractures. Pain Physician 22(1):63–68
Funding
The study was supported by Kunshan Social Development Science and Technology Project (CN) (KS18068), Beijing Bethune Charitable Foundation (CN) (B19338ES), and Suzhou Key Clinical Diagnosis and Treatment Technology Project (CN) (LCZX202024).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lu, K., Yin, Y., Li, C. et al. Efficacy of annual zoledronic acid in initial percutaneous kyphoplasty patients with osteoporotic vertebral compression fractures: a 3-year follow-up study. Osteoporos Int 32, 1429–1439 (2021). https://doi.org/10.1007/s00198-020-05816-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-020-05816-z