Abstract
Introduction and hypothesis
During vaginal hysterectomy, extraperitoneal uterosacral ligament suspension (ULS) bites can be taken before removing the uterus. We evaluated this modified extraperitoneal ULS for vault prolapse prevention.
Methods
Study period was 3.5 years. Fifty-one women with third- and fourth-degree prolapse were enrolled. An inverted V incision was made on the anterior vaginal wall and continued as a semicircular incision on the posterior vaginal wall. Lateral vaginal mucosa was pushed up to expose the cardinal–uterosacral ligament complex. The first ULS suture, using polypropylene no. 1, was taken in the upper-most exposed area of the uterosacral ligament. The second suture, using polyglactin no. 1 or 0, was taken 0.5–1 cm below the first suture. During placement of both sutures, traction on the cervix was maintained. The cardinal–uterosacral ligament complex was clamped, dissected, and ligated 1 cm below the second suture. Vaginal hysterectomy was completed. Ends of the ULS suture were fastened to the vault via vesicovaginal and rectovaginal septum using polypropylene within and polyglactin outside vaginal mucosa.
Results
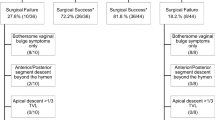
Prolapse stage was 3 in 42 cases and 4 in nine. Duration of operation ranged from 60 to 120 min. Blood loss was 100–300 ml. During follow-up (average 2.3 years) four (8.3%), cases had stage 1 pelvic organ prolapse (POP), three were lost to follow-up, and 44 (91.6%) had no POP.
Conclusions
Using the cervix as a traction device is a good option when performing extraperitoneal ULS during vaginal hysterectomy to prevent vault prolapse.






Similar content being viewed by others
Abbreviations
- ULS:
-
Uterosacral ligament suspension
References
Chung CP, Miskimins R, Kuehl TJ, Yandell PM, Shull BL. Permanent suture used in uterosacral ligament suspension offers better anatomical support than delayed absorbable suture. Int Urogynecol J. 2012;23:223–7. https://doi.org/10.1007/s00192-011-1556-3.
Dwyer PL, Fatton B. Bilateral extraperitoneal uterosacral suspension: a new approach to correct posthysterectomy vaginal vault prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19:283–92. https://doi.org/10.1007/s00192-007-0435-4.
Cvach K, Dwyer P. Surgical management of pelvic organ prolapse: abdominal and vaginal approaches. World J Urol. 2011. https://doi.org/10.1007/s00345-011-0776-y.
Shull BL, Bachofen C, Coates KW, Kuehl TJ. A transvaginal approach to repair of apical and other associated sites of pelvic organ prolapse with uterosacral ligaments. Am J Obstet Gynecol. 2000;183:1365–73; discussion 1373-4. https://doi.org/10.1067/mob.2000.110910.
Yazdany T, Bhatia N. Uterosacral ligament vaginal vault suspension: anatomy, outcome and surgical considerations. Curr Opin Obstet Gynecol. 2008;20:484–8. https://doi.org/10.1097/GCO.0b013e32830eb8c6.
Fatton B, Dwyer PL, Achtari C, Tan PK. Bilateral extraperitoneal uterosacral vaginal vault suspension: a 2-year follow-up longitudinal case series of 123 patients. Int Urogynecol J Pelvic Floor Dysfunct. 2009;20:427–34. https://doi.org/10.1007/s00192-008-0791-8.
Ow LL, Walsh CE, Rajamaheswari N, Dwyer PL. Technique of extraperitoneal uterosacral ligament suspension for apical suspension. Int Urogynecol J. 2016;27:637–9. https://doi.org/10.1007/s00192-015-2873-8.
Acknowledgements
We express our heartfelt thanks to Dr. Ranita Roy Chowdhury, Assistant Professor, Dr. Srijoni Chowdhury, Clinical Tutor, and other members of the unit for helping conduct this study.
Author information
Authors and Affiliations
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Pal, M., Bandyopadhyay, S. Modified extraperitoneal uterosacral ligament suspension for prevention of vault prolapse after vaginal hysterectomy. Int Urogynecol J 30, 633–637 (2019). https://doi.org/10.1007/s00192-018-3669-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-018-3669-4