Abstract
Introduction and hypothesis
Pelvic floor disorders affect many women in high-income countries. Since little is known about such disorders in Africa, this study aimed at assessing the prevalence and risk factors in an Ethiopian community. We also assessed the validity of a prolapse questionnaire.
Methods
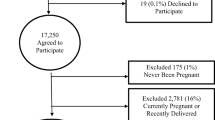
A community-based cross-sectional study was conducted among 395 women, recruited by a systematic random sampling technique. Women were interviewed about symptoms of urinary incontinence, faecal incontinence and pelvic organ prolapse by female nurses. Additionally, pelvic examinations were performed in 294 (74.2 %) participants to assess anatomical prolapse using the simplified Pelvic Organ Prolapse Quantification staging system. Descriptive statistics and logistic regression analyses were employed.
Results
The median age of participants was 35.0 years. Thirty-one women reported urinary incontinence (7.8 %), 25 (6.3 %) symptomatic pelvic organ prolapse and 2 (0.5 %) faecal incontinence. Anatomical pelvic organ prolapse stage II–IV was detected in 162 (55.1 %) of women who underwent pelvic examination. The questionnaire for prolapse assessment had poor validity (38.3 % sensitivity and 95.4 % specificity) even in cases of clinically relevant prolapse (stage III or IV). After adjustment, carrying heavy objects for 5 or more hours a day, history of prolonged labour and highland rural residence were associated with anatomical pelvic organ prolapse.
Conclusions
Self-reported incontinence seems low in northwest Ethiopia. The prevalence of symptomatic prolapse was low despite a high prevalence of prolapse signs. Notably, heavy carrying and prolonged labour increased the risk of anatomical prolapse stage II–IV. The methods of assessing pelvic floor disorders in a low-income context need further development.
Similar content being viewed by others
References
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J et al (2010) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J 21:5–26
Hunskaar S, Lose G, Sykes D, Voss S (2004) The prevalence of urinary incontinence in women in four European countries. BJU Int 93:324–330
Nelson R, Norton N, Cautley E, Furner S (1995) Community-based prevalence of anal incontinence. JAMA 274:559–561
Bharucha AE, Zinsmeister AR, Locke GR, Seide BM, McKeon K, Schleck CD et al (2005) Prevalence and burden of fecal incontinence: a population-based study in women. Gastroenterology 129:42–49
Whitcomb EL, Rortveit G, Brown JS, Creasman JM, Thom DH, Van Den Eeden SK et al (2009) Racial differences in pelvic organ prolapse. Obstet Gynecol 114:1271–1277
Nygaard I, Barber MD, Burgio KL, Kenton K, Meikle S, Schaffer J et al (2008) Prevalence of symptomatic pelvic floor disorders in US women. JAMA 300:1311–1316
Lukacz ES, Lawrence JM, Contreras R, Nager CW, Luber KM (2006) Parity, mode of delivery, and pelvic floor disorders. Obstet Gynecol 107:1253–1260
Ojengbede OA, Morhason-Bello IO, Adedokun BO, Okonkwo NS, Kolade CO (2011) Prevalence and the associated trigger factors of urinary incontinence among 5000 black women in sub-Saharan Africa: findings from a community survey. BJU Int 107:1793–1800
Walker GJ, Gunasekera P (2011) Pelvic organ prolapse and incontinence in developing countries: review of prevalence and risk factors. Int Urogynecol J 22:127–135
Scherf C, Morison L, Fiander A, Ekpo G, Walraven G (2002) Epidemiology of pelvic organ prolapse in rural Gambia, West Africa. BJOG 109:431–436
Iyoke CA, Ezugwu FO, Onah HE (2010) Prevalence and correlates of maternal morbidity in Enugu, South-East Nigeria. Afr J Reprod Health 14:121–130
Rortveit G, Brown JS, Thom DH, Van Den Eeden SK, Creasman JM, Subak LL (2007) Symptomatic pelvic organ prolapse: prevalence and risk factors in a population-based, racially diverse cohort. Obstet Gynecol 109:1396–1403
Rortveit G, Daltveit AK, Hannestad YS, Hunskaar S, Norwegian EPINCONT Study (2003) Urinary incontinence after vaginal delivery or cesarean section. N Engl J Med 348:900–907
Rortveit G, Hannestad YS, Daltveit AK, Hunskaar S (2001) Age- and type-dependent effects of parity on urinary incontinence: the Norwegian EPINCONT study. Obstet Gynecol 98:1004–1010
Fenner DE, Trowbridge ER, Patel DA, Fultz NH, Miller JM, Howard D et al (2008) Establishing the prevalence of incontinence study: racial differences in women’s patterns of urinary incontinence. J Urol 179:1455–1460
Thom DH, van den Eeden SK, Ragins AI, Wassel-Fyr C, Vittinghof E, Subak LL et al (2006) Differences in prevalence of urinary incontinence by race/ethnicity. J Urol 175:259–264
Ethiopia Demographic and Health Survey Report. Central Statistical Agency and ICF International 2011
Muleta M, Fantahun M, Tafesse B, Hamlin EC, Kennedy RC (2007) Obstetric fistula in rural Ethiopia. East Afr Med J 84:525–533
Lukman Y (1995) Utero-vaginal prolapse: a rural disability of the young. East Afr Med J 72:2–9
Kiros K, Mariam DH, Zemenfes D (2000) Genitourinary prolapse and joint hypermobility in Ethiopian women. East Afr Med J 77:640–643
Fantahun M, Kumbi S, Degu G, Kebede Y, Admasu M, Haile W et al (2001) Dabat Rural Health Project, North West Ethiopia: report of the baseline survey. Ethiop J Health Dev 15
Hannestad YS, Rortveit G, Sandvik H, Hunskaar S et al (2000) A community-based epidemiological survey of female urinary incontinence: the Norwegian EPINCONT study. Epidemiology of incontinence in the county of Nord-Trøndelag. J Clin Epidemiol 53:1150–1157
Sandvik H, Seim A, Vanvik A, Hunskaar S (2000) A severity index for epidemiological surveys of female urinary incontinence: comparison with 48-hour pad-weighing tests. Neurourol Urodyn 19:137–145
Manonai J, Mouritsen L, Palma P, Contreras-Ortiz O, Korte J, Swift S (2011) The inter-system association between the simplified pelvic organ prolapse quantification system (S-POP) and the standard pelvic organ prolapse quantification system (POPQ) in describing pelvic organ prolapse. Int Urogynecol J 22:347–352
Madombwe JP, Knight S (2010) High prevalence of urinary incontinence and poor knowledge of pelvic floor exercises among women in Ladysmith. S Afr J Obstet Gynaecol 16
Minassian VA, Drutz HP, Al-Badr A (2003) Urinary incontinence as a worldwide problem. Int J Gynaecol Obstet 82:327–338
Amaro JL, Macharelli CA, Yamamoto H, Kawano PR, Padovani CV, Agostinho AD (2009) Prevalence and risk factors for urinary and fecal incontinence in Brazilian women. Int Braz J Urol 35:592–597
Gjerde JL, Rortveit G, Muleta M, Blystad A (2012) Silently waiting to heal: experiences among women living with urinary incontinence in northwest Ethiopia. Int Urogynecol J. doi:10.1007/s00192-012-1951-4
Wusu-Ansah OK, Opare-Addo HS (2008) Pelvic organ prolapse in rural Ghana. Int J Gynaecol Obstet 103:121–124
Barber MD, Neubauer NL, Klein-Olarte V (2006) Can we screen for pelvic organ prolapse without a physical examination in epidemiologic studies? Am J Obstet Gynecol 195:942–948
Tegerstedt G, Miedel A, Maehle-Schmidt M, Nyren O, Hammarström M (2005) A short-form questionnaire identified genital organ prolapse. J Clin Epidemiol 58:41–46
Acknowledgments
We appreciate the Swift group for providing us a DVD for demonstration of the S-POPQ pelvic examination. We also extend our heartfelt thanks to study participants and data collectors. This study was funded by the Western Norway Regional Health Authority and the Nordic Urogynecological Association.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
The study was conducted in Gondar, Ethiopia.
Rights and permissions
About this article
Cite this article
Megabiaw, B., Adefris, M., Rortveit, G. et al. Pelvic floor disorders among women in Dabat district, northwest Ethiopia: a pilot study. Int Urogynecol J 24, 1135–1143 (2013). https://doi.org/10.1007/s00192-012-1981-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-1981-y