Abstract
Purpose
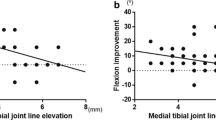
This study aimed to determine the correlation between the change in joint line height calculated from the resected bone and insert thickness during surgery and the change in limb alignment following unicompartmental knee arthroplasty (UKA). It was hypothesized that joint line elevation is correlated with the change in limb alignment.
Methods
A total of 74 consecutive patients diagnosed with either isolated medial compartmental osteoarthritis (38 patients) or spontaneous osteonecrosis of the knee (36 patients) were included. The thickness of the proximal tibial and distal femoral bony cuts was measured during surgery; using these values, the medial joint line elevation of the tibia (MJLET) and medial joint line reduction of the femur (MJLRF) were defined. The correlation between the amount of change in the hip–knee–ankle (HKA) angle before and after surgery (δHKA) and the thickness of the tibial insert (TI), MJLET, or MJLRF were evaluated.
Results
The mean values of δHKA, TI, MJLET, and MJLRF were 5.0° ± 2.6°, 8.5 ± 0.8, 4.4 ± 1.3, and 0.0 ± 1.1 mm, respectively. The δHKA had a significant, but weak-positive correlation with the TI (P = 0.02), and moderate-positive correlation with MJLET (P < 0.001). However, no correlation was observed between δHKA and MJLRF.
Conclusions
The MJLET measured during surgery had a significant moderate-positive correlation with the change in limb alignment following medial UKA. For clinical relevance, the surgeon can predict postoperative limb alignment after UKA by considering, intraoperatively, both the insert thickness and the depth of resection at the proximal tibia thus minimizing technical error to obtain an optimal alignment after UKA.
Level of evidence
Diagnostic study, level II.


Similar content being viewed by others
References
Akizuki S, Mueller JK, Horiuchi H, Matsunaga D, Shibakawa A, Komistek RD (2009) In vivo determination of kinematics for subjects having a Zimmer Unicompartmental High Flex Knee System. J Arthroplast 24(6):963–971
Aleto TJ, Berend ME, Ritter MA, Faris PM, Meneghini RM (2008) Early failure of unicompartmental knee arthroplasty leading to revision. J Arthroplast 23(2):159–163
Arguello-Cuenca JM, Vaquero-Martin J, Corella F, Calvo JA, Rodriganez L (2012) Clinical and functional outcome of unicompartmental knee arthroplasty: influence of the mechanical axis correction. Rev Esp Cir Ortop Traumatol 56(1):32–37
Hernigou P, Deschamps G (2004) Alignment influences wear in the knee after medial unicompartmental arthroplasty. Clin Orthop Relat Res 423:161–165
Herry Y, Batailler C, Lording T, Servien E, Neyret P, Lustig S (2017) Improved joint-line restitution in unicompartmental knee arthroplasty using a robotic-assisted surgical technique. Int Orthop 41(11):2265–2271
Hopgood P, Martin CP, Rae PJ (2004) The effect of tibial implant size on post-operative alignment following medial unicompartmental knee replacement. Knee 11(5):385–388
Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the Knee Society clinical rating system. Clin Orthop Relat Res 248:13–14
Kennedy WR, White RP (1987) Unicompartmental arthroplasty of the knee. Postoperative alignment and its influence on overall results. Clin Orthop Relat Res 221:278–285
Kim KT, Lee S, Kim TW, Lee JS, Boo KH (2012) The influence of postoperative tibiofemoral alignment on the clinical results of unicompartmental knee arthroplasty. Knee Surg Relat Res 24(2):85–90
Kim SJ, Bae JH, Lim HC (2012) Factors affecting the postoperative limb alignment and clinical outcome after Oxford unicompartmental knee arthroplasty. J Arthroplast 27(6):1210–1215
Klemme WR, Galvin EG, Petersen SA (1994) Unicompartmental knee arthroplasty. Sequential radiographic and scintigraphic imaging with an average five-year follow-up. Clin Orthop Relat Res 301:233–238
Kuwashima U, Okazaki K, Tashiro Y, Mizu-Uchi H, Hamai S, Okamoto S et al (2015) Correction of coronal alignment correlates with reconstruction of joint height in unicompartmental knee arthroplasty. Bone Jt Res 4(8):128–133
Ridgeway SR, McAuley JP, Ammeen DJ, Engh GA (2002) The effect of alignment of the knee on the outcome of unicompartmental knee replacement. J Bone Jt Surg Br 84(3):351–355
Scott RD, Cobb AG, McQueary FG, Thornhill TS (1991) Unicompartmental knee arthroplasty. Eight- to 12-year follow-up evaluation with survivorship analysis. Clin Orthop Relat Res 271:96–100
Squire MW, Callaghan JJ, Goetz DD, Sullivan PM, Johnston RC (1999) Unicompartmental knee replacement. A minimum 15 year followup study. Clin Orthop Relat Res 367:61–72
Tashiro Y, Matsuda S, Okazaki K, Mizu-Uchi H, Kuwashima U, Iwamoto Y (2014) The coronal alignment after medial unicompartmental knee arthroplasty can be predicted: usefulness of full-length valgus stress radiography for evaluating correctability. Knee Surg Sports Traumatol Arthrosc 22(12):3142–3149
Vasso M, Del Regno C, D’Amelio A, Viggiano D, Corona K, Schiavone Panni A (2015) Minor varus alignment provides better results than neutral alignment in medial UKA. Knee 22(2):117–121
Weale AE, Murray DW, Baines J, Newman JH (2000) Radiological changes five years after unicompartmental knee replacement. J Bone Jt Surg Br 82(7):996–1000
Weber P, Schroder C, Laubender RP, Baur-Melnyk A, von Schulze Pellengahr C, Jansson V et al (2013) Joint line reconstruction in medial unicompartmental knee arthroplasty: development and validation of a measurement method. Knee Surg Sports Traumatol Arthrosc 21(11):2468–2473
Wen PF, Guo WS, Gao FQ, Zhang QD, Yue JA, Cheng LM et al (2017) Effects of lower limb alignment and tibial component inclination on the biomechanics of lateral compartment in unicompartmental knee arthroplasty. Chin Med J (Engl) 130(21):2563–2568
Funding
No funding or external support was received by any of the authors in support of or in any relationship to the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interests to declare.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Kuroda, Y., Takayama, K., Ishida, K. et al. Medial joint line elevation of the tibia measured during surgery has a significant correlation with the limb alignment changes following medial unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 26, 3468–3473 (2018). https://doi.org/10.1007/s00167-018-4935-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-4935-1