Abstract
Purpose
Autologous osteochondral transplantation is an established treatment for large-sized osteochondral lesions of the talus (OLT) with excellent short term outcomes. However, few studies assess the outcomes of autologous osteochondral transplantation at mid-term follow-up. The purpose of the current systematic review was to evaluate the clinical outcomes of the autologous osteochondral transplantation procedure in the treatment of OLT at mid-term and long-term follow-up.
Methods
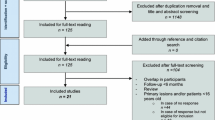
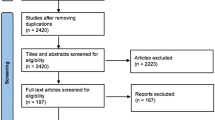
A systematic search of the MEDLINE, EMBASE and Cochrane Library databases was performed in October 2017 based on the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. Included studies were evaluated with regard to level of evidence (LOE) and quality of evidence (QOE) using the Coleman Methodology Score. Clinical outcomes, and complications were also evaluated.
Results
Eleven studies, with 500 ankles were included at a mean 62.8 months follow-up. Seven studies used the American Orthopaedic Foot and Ankle Society (AOFAS) score. The weighted mean preoperative AOFAS score was 55.1 ± 6.1, and the postoperative score was 86.2 ± 4.5, with 87.4% of patients (132 of 151) being reported as excellent or good results. In total, 53 of the 500 patients (10.6%) had complications. The most common complication was donor site morbidity with 18 patients (3.6%) at final follow-up. Thirty-one patients (6.2%) underwent reoperations, and 5 ankles (1.0%) were regarded as failed autologous osteochondral transplantation.
Conclusion
The current systematic review demonstrated that good clinical and functional outcomes can be expected following autologous osteochondral transplantation for the treatment of OLT, with a low failure rate. The results from this study show patients can be reasonably counselled to expect good clinical outcomes in the mid-term. MRI and radiographs showed restoration of articular surface as well as a minimal presence of osteoarthritis at mid-term follow-up. However, as low level and quality of evidence and the variability of the data may confound the data, further well-designed studies are necessary to determine the effectiveness of autologous osteochondral transplantation in the treatment for OLT.
Level of evidence
IV.

Similar content being viewed by others
References
Coleman BD, Khan KM, Maffulli N, Cook JL, Wark JD (2000) Studies of surgical outcome after patellar tendinopathy: clinical significance of methodological deficiencies and guidelines for future studies. Victorian Institute of Sport Tendon Study Group. Scand J Med Sci Sports 10:2–11
Dahmen J, Lambers KTA, Reilingh ML, van Bergen CJA, Stufkens SAS, Kerkhoffs GMMJ. (2017) No superior treatment for primary osteochondral defects of the talus. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4616-5
de l’Escalopier N, Barbier O, Mainard D, Mayer J, Ollat D, Versier G (2015) Outcomes of talar dome osteochondral defect repair using osteocartilaginous autografts: 37 cases of Mosaicplasty®. Orthop Traumatol Surg Res 101:97–102
Ferkel RD, Zanotti RM, Komenda GA, Sgaglione NA, Cheng MS, Applegate GR et al (2008) Arthroscopic treatment of chronic osteochondral lesions of the talus: long-term results. Am J Sports Med 36:1750–1762
Fraser EJ, Harris MC, Prado MP, Kennedy JG (2016) Autologous osteochondral transplantation for osteochondral lesions of the talus in an athletic population. Knee Surg Sports Traumatol Arthrosc 24:1272–1279
Fraser EJ, Savage-Elliott I, Yasui Y, Ackermann J, Watson G, Ross KA et al (2016) Clinical and MRI donor site outcomes following autologous osteochondral transplantation for talar osteochondral lesions. Foot Ankle Int 37:968–976
Georgiannos D, Bisbinas I, Badekas A (2016) Osteochondral transplantation of autologous graft for the treatment of osteochondral lesions of talus: 5- to 7-year follow-up. Knee Surg Sports Traumatol Arthrosc 24:3722–3729
Haleem AM, Ross KA, Smyth NA, Duke GL, Deyer TW, Do HT et al (2014) Double-plug autologous osteochondral transplantation shows equal functional outcomes compared with single-plug procedures in lesions of the talar dome: a minimum 5-year clinical follow-up. Am J Sports Med 42:1888–1895
Hangody L, Dobos J, Baló E, Pánics G, Hangody LR, Berkes I (2010) Clinical experiences with autologous osteochondral mosaicplasty in an athletic population: a 17-year prospective multicenter study. Am J Sports Med 38:1125–1133
Hangody L, Kish G, Módis L, Szerb I, Gáspár L, Diószegi Z et al (2001) Mosaicplasty for the treatment of osteochondritis dissecans of the talus: two to seven year results in 36 patients. Foot Ankle Int 22:552–558
Hannon CP, Murawski CD, Fansa AM, Smyth NA, Do H, Kennedy JG (2013) Microfracture for osteochondral lesions of the talus: a systematic review of reporting of outcome data. Am J Sports Med 41:689–695
Imhoff AB, Paul J, Ottinger B, Wörtler K, Lämmle L, Spang J et al (2011) Osteochondral transplantation of the talus: long-term clinical and magnetic resonance imaging evaluation. Am J Sports Med 39:1487–1493
Kennedy JG, Murawski CD (2011) The treatment of osteochondral lesions of the talus with autologous osteochondral transplantation and bone marrow aspirate concentrate: surgical technique. Cartilage 2:327–336
Kreuz PC, Steinwachs M, Erggelet C, Lahm A, Henle P, Niemeyer P (2006) Mosaicplasty with autogenous talar autograft for osteochondral lesions of the talus after failed primary arthroscopic management: a prospective study with a 4-year follow-up. Am J Sports Med 34:55–63
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med 151:W65-94
Marymont JV, Shute G, Zhu H, Varner KE, Paravic V, Haddad JL et al (2005) Computerized matching of autologous femoral grafts for the treatment of medial talar osteochondral defects. Foot Ankle Int 26:708–712
Marx RG, Wilson SM, Swiontkowski MF (2015) Updating the assignment of levels of evidence. J Bone Jt Surg Am 97:1–2
Moher D, Cook DJ, Jadad AR, Tugwell P, Moher M, Jones A et al (1999) Assessing the quality of reports of randomised trials: implications for the conduct of meta-analyses. Health Technol Assess 3:1–98
Paul J, Sagstetter A, Kriner M, Imhoff AB, Spang J, Hinterwimmer S (2009) Donor-site morbidity after osteochondral autologous transplantation for lesions of the talus. J Bone Jt Surg Am 91:1683–1688
Paul J, Sagstetter M, Lämmle L, Spang J, El-Azab H, Imhoff AB et al (2012) Sports activity after osteochondral transplantation of the talus. Am J Sports Med 40:870–874
Pinski JM, Boakye LA, Murawski CD, Hannon CP, Ross KA, Kennedy JG (2016) Low level of evidence and methodologic quality of clinical outcome studies on cartilage repair of the ankle. Arthroscopy 32:214–222
Ramponi L, Yasui Y, Murawski CD, Ferkel RD, DiGiovanni CW, Kerkhoffs GMMJ. et al (2016) Lesion size is a predictor of clinical outcomes after bone marrow stimulation for osteochondral lesions of the talus: a systematic review. Am J Sports Med 45:1698–1705
Ross AW, Murawski CD, Fraser EJ, Ross KA, Do HT, Deyer TW et al (2016) Autologous osteochondral transplantation for osteochondral lesions of the talus: does previous bone marrow stimulation negatively affect clinical outcome? Arthroscopy 32:1377–1383
Savage-Elliott I, Smyth NA, Deyer TW, Murawski CD, Ross KA, Hannon CP et al (2016) Magnetic resonance imaging evidence of postoperative cyst formation does not appear to affect clinical outcomes after autologous osteochondral transplantation of the talus. Arthroscopy 32:1846–1856
Scranton PE Jr, Frey CC, Feder KS (2006) Outcome of osteochondral autograft transplantation for type-V cystic osteochondral lesions of the talus. J Bone Jt Surg Br 88:614–619
Shimozono Y, Coale M, Yasui Y, O’Halloran A, Deyer TW, Kennedy JG (2017) Subchondral bone degradation following microfracture for osteochondral lesions of the talus. Am J Sports Med. https://doi.org/10.1177/0363546517739606
Valderrabano V, Leumann A, Rasch H, Egelhof T, Hintermann B, Pagenstert G (2009) Knee-to-ankle mosaicplasty for the treatment of osteochondral lesions of the ankle joint. Am J Sports Med 37(Suppl 1):105S-111S
Yoon HS, Park YJ, Lee M, Choi WJ, Lee JW (2014) Osteochondral autologous transplantation is superior to repeat arthroscopy for the treatment of osteochondral lesions of the talus after failed primary arthroscopic treatment. Am J Sports Med 42:1896–1903
Zengerink M, Struijs PA, Tol JL, van Dijk CN (2010) Treatment of osteochondral lesions of the talus: a systematic review. Knee Surg Sports Traumatol Arthrosc 18:238–246
Funding
No funding was received by any of the authors related to this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This manuscript is a systematic review and does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Shimozono, Y., Hurley, E.T., Myerson, C.L. et al. Good clinical and functional outcomes at mid-term following autologous osteochondral transplantation for osteochondral lesions of the talus. Knee Surg Sports Traumatol Arthrosc 26, 3055–3062 (2018). https://doi.org/10.1007/s00167-018-4917-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-4917-3