Abstract
Purpose
To determine differences in health-related quality of life (HRQoL), survival and healthcare resource use of critically ill adults with and without sepsis.
Methods
We conducted a primary propensity score matched analysis of patients with and without sepsis enrolled in a large multicentre clinical trial. Outcomes included HRQoL at 6 months, survival to 2 years, length of ICU and hospital admission and cost of ICU and hospital treatment to 2 years.
Results
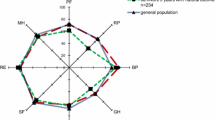
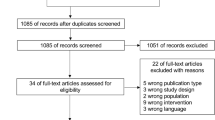
We obtained linked data for 3442 (97.3%) of 3537 eligible patients and matched 806/905 (89.0%) patients with sepsis with 806/2537 (31.7%) without. After matching, there were no significant differences in the proportion of survivors with and without sepsis reporting problems with mobility (37.8% vs. 38.7%, p = 0.86), self-care (24.7% vs. 26.0%, p = 0.44), usual activities (44.5% vs. 46.8%, p = 0.28), pain/discomfort (42.4% vs. 41.6%, p = 0.54) and anxiety/depression (36.9% vs. 37.7%, p = 0.68). There was no significant difference in survival at 2 years: 482/792 (60.9%) vs. 485/799 (60.7%) (HR 1.01, 95% CI 0.86–1.18, p = 0.94). The initial ICU and hospital admission were longer for patients with sepsis: 10.1 ± 11.9 vs. 8.0 ± 9.8 days (p < 0.0001) and 22.8 ± 21.2 vs. 19.1 ± 19.0 days, (p = 0.0003) respectively. The cost of ICU admissions was higher for patients with sepsis: A$43,345 ± 46,263 (€35,109 ± 35,043) versus 34,844 ± 38,281 (€28,223 ± 31,007), mean difference $8501 (€6885), 95% CI $4342–12,660 (€3517 ± 10,254), p < 0.001 as was the total cost of hospital treatment to 2 years: A$74,120 ± 60,750 (€60,037 ± 49,207) versus A$65,806 ± 59,856 (€53,302 ± 48,483), p = 0.005.
Conclusions
Critically ill patients with sepsis have higher healthcare resource use and costs but similar survival and HRQoL compared to matched patients without sepsis.



Similar content being viewed by others
References
Torio C, Moore, BJ (2016) National inpatient hospital costs: the most expensive conditions by payer, 2013. https://www.hcup-us.ahrq.gov/reports/statbriefs/sb204-Most-Expensive-Hospital-Conditions.jsp. Accessed 12 Dec 2017
Seventieth World Health Assembly (2017) Improving the prevention, diagnosis and clinical management of sepsis. http://apps.who.int/gb/ebwha/pdf_files/WHA70/A70_R7-en.pdf. Accessed 12 Dec 2017
Liu V, Escobar GJ, Greene JD, Soule J, Whippy A, Angus DC et al (2014) Hospital deaths in patients with sepsis from 2 independent cohorts. JAMA 312(1):90–92
Fleischmann C, Thomas-Rueddel DO, Hartmann M, Hartog CS, Welte T, Heublein S et al (2016) Hospital incidence and mortality rates of sepsis. Dtsch Arzteblatt Int 113(10):159–166
Cohen J, Vincent JL, Adhikari NK, Machado FR, Angus DC, Calandra T et al (2015) Sepsis: a roadmap for future research. Lancet Infect Dis 15(5):581–614
Zimmerman JE, Kramer AA, Knaus WA (2013) Changes in hospital mortality for United States intensive care unit admissions from 1988 to 2012. Crit Care 17(2):R81
Desai SV, Law TJ, Needham DM (2011) Long-term complications of critical care. Crit Care Med 39(2):371–379
Yende S, Austin S, Rhodes A, Finfer S, Opal S, Thompson T et al (2016) Long-term quality of life among survivors of severe sepsis: analyses of two international trials. Crit Care Med 44(8):1461–1467
Prescott HC, Costa DK (2018) Improving long-term outcomes after sepsis. Crit Care Clin 34(1):175–188
Elliott D, Davidson JE, Harvey MA, Bemis-Dougherty A, Hopkins RO, Iwashyna TJ et al (2014) Exploring the scope of post-intensive care syndrome therapy and care: engagement of non-critical care providers and survivors in a second stakeholders meeting. Crit Care Med 42(12):2518–2526
Shankar-Hari M, Ambler M, Mahalingasivam V, Jones A, Rowan K, Rubenfeld GD (2016) Evidence for a causal link between sepsis and long-term mortality: a systematic review of epidemiologic studies. Crit Care 20:101
Myburgh JA, Finfer S, Bellomo R, Billot L, Cass A, Gattas D et al (2012) Hydroxyethyl starch or saline for fluid resuscitation in intensive care. New Engl J Med 367(20):1901–1911
Patel A, Pieper K, Myburgh JA, Perkovic V, Finfer S, Yang Q et al (2017) Reanalysis of the crystalloid versus hydroxyethyl starch trial (CHEST). New Engl J Med 377(3):298–300
Taylor C, Thompson K, Finfer S, Higgins A, Jan S, Li Q et al (2016) Hydroxyethyl starch versus saline for resuscitation of patients in intensive care: long-term outcomes and cost-effectiveness analysis of a cohort from CHEST. Lancet Respir Med 4(10):818–825
Austin PC (2011) An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivar Behav Res 46(3):399–424
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) APACHE II: a severity of disease classification system. Crit Care Med 13(10):818–829
Bone RC, Balk RA, Cerra FB, Dellinger RP, Fein AM, Knaus WA et al (1992) Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest 101(6):1644–1655
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M et al (2016) The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA 315(8):801–810
EuroQol G (1990) EuroQol–a new facility for the measurement of health-related quality of life. Health Policy 16(3):199–208
Inter-Government and Funding Strategies (2011) Costs of care standards 2009/10. http://www1.health.nsw.gov.au/pds/ArchivePDSDocuments/GL2011_007.pdf. Accessed Dec 2016
Australian Government Department of Health (2012) Round 14 (2009–2010) National public cost weight tables—version 6.0x and version 5.2. http://www.health.gov.au/internet/main/publishing.nsf/Content/Round_14-cost-reports. Accessed 12 Dec 2017
Garrido MM, Kelley AS, Paris J, Roza K, Meier DE, Morrison RS et al (2014) Methods for constructing and assessing propensity scores. Health Serv Res 49(5):1701–1720
Funk MJ, Westreich D, Wiesen C, Sturmer T, Brookhart MA, Davidian M (2011) Doubly robust estimation of causal effects. Am J Epidemiol 173(7):761–767
Prescott HC, Osterholzer JJ, Langa KM, Angus DC, Iwashyna TJ (2016) Late mortality after sepsis: propensity matched cohort study. BMJ 353:i2375
Prescott HC, Langa KM, Liu V, Escobar GJ, Iwashyna TJ (2014) Increased 1-year healthcare use in survivors of severe sepsis. Am J Respir Crit Care Med 190(1):62–69
Ghelani D, Moran JL, Sloggett A, Leeson RJ, Peake SL (2009) Long-term survival of intensive care and hospital patient cohorts compared with the general Australian population: a relative survival approach. J Eval Clin Pract 15(3):425–435
Davis JS, He V, Anstey NM, Condon JR (2014) Long term outcomes following hospital admission for sepsis using relative survival analysis: a prospective cohort study of 1,092 patients with 5 year follow up. PLoS One 9(12):e112224
Iwashyna TJ, Ely EW, Smith DM, Langa KM (2010) Long-term cognitive impairment and functional disability among survivors of severe sepsis. JAMA 304(16):1787–1794
Hofhuis JG, Spronk PE, van Stel HF, Schrijvers AJ, Rommes JH, Bakker J (2008) The impact of severe sepsis on health-related quality of life: a long-term follow-up study. Anesth Analg 107(6):1957–1964
Battle CE, Davies G, Evans PA (2014) Long term health-related quality of life in survivors of sepsis in South West Wales: an epidemiological study. PLoS One 9(12):e116304
Finfer S, Bellomo R, Lipman J, French C, Dobb G, Myburgh J et al (2004) Adult population incidence of severe sepsis in Australian and New Zealand intensive care units. Intensive Care Med 30:589–596
Cohen J, Guyatt G, Bernard GR, Calandra T, Cook D, Elbourne D et al (2001) New strategies for clinical trials in patients with sepsis and septic shock. Crit Care Med 29(4):880–886
Angus DC (2010) The lingering consequences of sepsis: a hidden public health disaster? JAMA 304(16):1833–1834
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflicts of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Thompson, K., Taylor, C., Jan, S. et al. Health-related outcomes of critically ill patients with and without sepsis. Intensive Care Med 44, 1249–1257 (2018). https://doi.org/10.1007/s00134-018-5274-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-018-5274-x