Abstract
Purpose
Physical examination, laboratory tests, ultrasound, conventional radiography, multislice computed tomography (MSCT), and diagnostic laparoscopy are used for diagnosing blunt abdominal trauma. In this article, we investigate and evaluate the usefulness and limitations of various diagnostic modalities on the basis of a comprehensive review of the literature.
Methods
We searched commonly used databases in order to obtain information about the aforementioned diagnostic modalities. Relevant articles were included in the literature review. On the basis of the results of our comprehensive analysis of the literature and a current case, we offer a diagnostic algorithm.
Results
A total of 86 studies were included in the review. Ecchymosis of the abdominal wall (seat belt sign) is a clinical sign that has a high predictive value. Laboratory values such as those for haematocrit, haemoglobin, base excess or deficit, and international normalised ratio (INR) are prognostic parameters that are useful in guiding therapy. Extended focused assessment with sonography for trauma (eFAST) has become a well established component of the trauma room algorithm but is of limited usefulness in the diagnosis of blunt abdominal trauma. Compared with all other diagnostic modalities, MSCT has the highest sensitivity and specificity. Diagnostic laparoscopy is an invasive technique that may also serve as a therapeutic tool and is particularly suited for haemodynamically stable patients with suspected hollow viscus injuries.
Conclusions
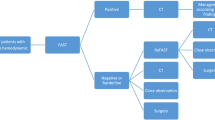
MSCT is the gold standard diagnostic modality for blunt abdominal trauma because of its high sensitivity and specificity in detecting relevant intra-abdominal injuries. In many cases, however, clinical, laboratory and imaging findings must be interpreted jointly for an adequate evaluation of a patient’s injuries and for treatment planning since these data supplement and complement one another. Patients with blunt abdominal trauma should be admitted for clinical observation over a minimum period of 24 h since there is no investigation that can reliably rule out intra-abdominal injuries.


Similar content being viewed by others
Change history
14 August 2020
A Correction to this paper has been published: https://doi.org/10.1007/s00068-020-01456-4
References
Iaselli F, et al. Bowel and mesenteric injuries from blunt abdominal trauma: a review. Radiol Med. 2015;120(1):21–322.
Norcross ED, et al. Application of American College of Surgeons’ field triage guidelines by pre-hospital personnel. J Am Coll Surg. 1995;181(6):539–44.
Rossaint R, et al. The European guideline on management of major bleeding and coagulopathy following trauma: fourth edition. Crit Care. 2016;20(1):100.
Vailas MG, et al. Seatbelt sign in a case of blunt abdominal trauma; what lies beneath it? BMC Surg. 2015;15:121.
McStay C, et al. Hollow viscus injury. J Emerg Med. 2009;37(3):293–9.
Chandler CF, Lane JS, Waxman KS. Seatbelt sign following blunt trauma is associated with increased incidence of abdominal injury. Am Surg. 1997;63(10):885–8.
Jones EL, et al. Intra-abdominal injury following blunt trauma becomes clinically apparent within 9 hours. J Trauma Acute Care Surg. 2014;76(4):1020–3.
Allgower M, Burri C. “Shock index”. Dtsch Med Wochenschr. 1967;92(43):1947–50.
Liu N, et al. An intelligent scoring system and its application to cardiac arrest prediction. IEEE Trans Inf Technol Biomed. 2012;16(6):1324–31.
Mitra B, et al. Trauma patients with the ‘triad of death’. Emerg Med J. 2012;29(8):622–5.
Wang SY, et al. An outcome prediction model for exsanguinating patients with blunt abdominal trauma after damage control laparotomy: a retrospective study. BMC Surg. 2014;14:24.
Ibrahim I, et al. Is arterial base deficit still a useful prognostic marker in trauma? A systematic review. Am J Emerg Med. 2016;34(3):626–35.
Davis JW, Kaups KL. Base deficit in the elderly: a marker of severe injury and death. J Trauma. 1998;45(5):873–7.
Mutschler M, et al. Renaissance of base deficit for the initial assessment of trauma patients: a base deficit-based classification for hypovolemic shock developed on data from 16,305 patients derived from the TraumaRegister DGU(R). Crit Care. 2013;17(2):R42.
Johansson PI, et al. Thrombelastography and tromboelastometry in assessing coagulopathy in trauma. Scand J Trauma Resusc Emerg Med. 2009;17:45.
Brohi K, Cohen MJ, Davenport RA. Acute coagulopathy of trauma: mechanism, identification and effect. Curr Opin Crit Care. 2007;13(6):680–5.
Hunt H, et al. (2015) Thromboelastography (TEG) and rotational thromboelastometry (ROTEM) for trauma induced coagulopathy in adult trauma patients with bleeding. Cochrane Database Syst Rev. 2015;2:CD010438.
Greenfield RH, Bessen HA, Henneman PL. Effect of crystalloid infusion on hematocrit and intravascular volume in healthy, nonbleeding subjects. Ann Emerg Med. 1989;18(1):51–5.
Stamler KD. Effect of crystalloid infusion on hematocrit in nonbleeding patients, with applications to clinical traumatology. Ann Emerg Med. 1989;18(7):747–9.
Genoa Update on Colorectal Polyp. Proceedings of the advanced course in coloproctology: the colorectal polyps, from genetics to surgery. Genoa, Italy, 11–12 March 2004. Tech Coloproctol, 2004. 8 Suppl 2: p. s239–314.
Thorson CM, et al. Admission hematocrit and transfusion requirements after trauma. J Am Coll Surg. 2013;216(1):65–73.
Mahajan A, et al. Utility of serum pancreatic enzyme levels in diagnosing blunt trauma to the pancreas: a prospective study with systematic review. Injury. 2014;45(9):1384–93.
Sabzghabaei A, et al. The accuracy of urinalysis in predicting intra-abdominal injury following blunt traumas. Emerg (Tehran). 2016;4(1):11–5.
Scalea TM, et al. Focused assessment with sonography for trauma (FAST): results from an international consensus conference. J Trauma. 1999;46(3):466–72.
Moore CL, Copel JA. Point-of-care ultrasonography. N Engl J Med. 2011;364(8):749–57.
Montoya J, et al. From FAST to E-FAST: an overview of the evolution of ultrasound-based traumatic injury assessment. Eur J Trauma Emerg Surg. 2016;42(2):119–26.
Surgeons, A.C.o., Advanced Trauma Life Support. Vol. 9. 2014: Urban and Fischer Verlag/Elsevier.
Unfallchirurgie, D.G.f., S3—Leitlinie Polytrauma und Schwerverletztenversorgung. 2016: AWMF.
Stawicki SP. Trends in nonoperative management of traumatic injuries: a synopsis. Int J Crit Illn Inj Sci. 2017;7(1):38–57.
Wilkerson RG, Stone MB. Sensitivity of bedside ultrasound and supine anteroposterior chest radiographs for the identification of pneumothorax after blunt trauma. Acad Emerg Med. 2010;17(1):11–7.
Nandipati KC, et al. Extended focused assessment with sonography for trauma (EFAST) in the diagnosis of pneumothorax: experience at a community based level I trauma center. Injury. 2011;42(5):511–4.
Wherrett LJ, et al. Hypotension after blunt abdominal trauma: the role of emergent abdominal sonography in surgical triage. J Trauma. 1996;41(5):815–20.
Hoffmann R, et al. Blunt abdominal trauma in cases of multiple trauma evaluated by ultrasonography: a prospective analysis of 291 patients. J Trauma. 1992;32(4):452–8.
Jehle D, Guarino J, Karamanoukian H. Emergency department ultrasound in the evaluation of blunt abdominal trauma. Am J Emerg Med. 1993;11(4):342–6.
Branney SW, et al. Quantitative sensitivity of ultrasound in detecting free intraperitoneal fluid. J Trauma. 1995;39(2):375–80.
Stawicki SP, et al. Portable ultrasonography in mass casualty incidents: The CAVEAT examination. World J Orthop. 2010;1(1):10–9.
Soyuncu S, et al. Accuracy of physical and ultrasonographic examinations by emergency physicians for the early diagnosis of intraabdominal haemorrhage in blunt abdominal trauma. Injury. 2007;38(5):564–9.
Healey MA, et al. A prospective evaluation of abdominal ultrasound in blunt trauma: is it useful? J Trauma. 1996;40(6):875–83.
McGahan JP, Richards J, Gillen M. The focused abdominal sonography for trauma scan: pearls and pitfalls. J Ultrasound Med. 2002;21(7):789–800.
Carter JW, et al. Do we really rely on fast for decision-making in the management of blunt abdominal trauma? Injury. 2015;46(5):817–21.
Blackstock U, Munson J, Szyld D. Bedside ultrasound curriculum for medical students: report of a blended learning curriculum implementation and validation. J Clin Ultrasound. 2015;43(3):139–44.
Dubois L, Leslie K, Parry N. FACTS survey: focused assessment with sonography in trauma use among Canadian residents training in general surgery. J Trauma. 2010;69(4):765–9.
Ma OJ, et al. Operative versus nonoperative management of blunt abdominal trauma: Role of ultrasound-measured intraperitoneal fluid levels. Am J Emerg Med. 2001;19(4):284–6.
Ollerton JE, et al. Prospective study to evaluate the influence of FAST on trauma patient management. J Trauma. 2006;60(4):785–91.
Wydo SM, et al. Portable ultrasound in disaster triage: a focused review. Eur J Trauma Emerg Surg. 2016;42(2):151–9.
Stengel D, et al. (2015) Emergency ultrasound-based algorithms for diagnosing blunt abdominal trauma. Cochrane Database Syst Rev. 2015;9:CD004446.
Miele V, et al. Contrast-enhanced ultrasound (CEUS) in blunt abdominal trauma. Br J Radiol. 2016;89(1061):20150823.
Zhang Z, et al. Diagnostic accuracy of contrast enhanced ultrasound in patients with blunt abdominal trauma presenting to the emergency department: a systematic review and meta-analysis. Sci Rep. 2017;7(1):4446.
Sessa B, et al. Blunt abdominal trauma: role of contrast-enhanced ultrasound (CEUS) in the detection and staging of abdominal traumatic lesions compared to US and CE-MDCT. Radiol Med. 2015;120(2):180–9.
Valentino M, et al. Contrast-enhanced ultrasound for blunt abdominal trauma. Semin Ultrasound CT MR. 2007;28(2):130–40.
Pinto F, et al. The use of contrast-enhanced ultrasound in blunt abdominal trauma: advantages and limitations. Acta Radiol. 2014;55(7):776–84.
Wongwaisayawan S, et al. Trauma ultrasound. Ultrasound Med Biol. 2015;41(10):2543–61.
Pinto F, et al. The role of CEUS in the assessment of haemodynamically stable patients with blunt abdominal trauma. Radiol Med. 2015;120(1):3–11.
Deunk J, et al. Predictors for the selection of patients for abdominal CT after blunt trauma: a proposal for a diagnostic algorithm. Ann Surg. 2010;251(3):512–20.
Kokabi N, et al. Specific radiological findings of traumatic gastrointestinal tract injuries in patients with blunt chest and abdominal trauma. Can Assoc Radiol J. 2015;66(2):158–63.
Corwin MT, et al. Utilization of a clinical prediction rule for abdominal-pelvic CT scans in patients with blunt abdominal trauma. Emerg Radiol. 2014;21(6):571–6.
Soto JA, Anderson SW. Multidetector CT of blunt abdominal trauma. Radiology. 2012;265(3):678–93.
Marek AP, et al. CT scan-detected pneumoperitoneum: an unreliable predictor of intra-abdominal injury in blunt trauma. Injury. 2014;45(1):116–21.
Hefny AF, et al. Usefulness of free intraperitoneal air detected by CT scan in diagnosing bowel perforation in blunt trauma: experience from a community-based hospital. Injury. 2015;46(1):100–4.
Gonser-Hafertepen LN, et al. Isolated free fluid on abdominal computed tomography in blunt trauma: watch and wait or operate? J Am Coll Surg. 2014;219(4):599–605.
Park MH, Shin BS, Namgung H. Diagnostic performance of 64-MDCT for blunt small bowel perforation. Clin Imaging. 2013;37(5):884–8.
Yu J, et al. Blunt bowel and mesenteric injury: MDCT diagnosis. Abdom Imaging. 2011;36(1):50–61.
Fu CJ, et al. Computed tomography arterial portography for assessment of portal vein injury after blunt hepatic trauma. Diagn Interv Radiol. 2015;21(5):361–7.
Wallace GW, et al. Imaging the pregnant patient with abdominal pain. Abdom Imaging. 2012;37(5):849–60.
Pearce MS, et al. Radiation exposure from CT scans in childhood and subsequent risk of leukaemia and brain tumours: a retrospective cohort study. Lancet. 2012;380(9840):499–505.
Arnold M, Moore SW. Paediatric blunt abdominal trauma - are we doing too many computed tomography scans? S Afr J Surg. 2013;51(1):26–31.
Panda A, et al. Evaluation of diagnostic utility of multidetector computed tomography and magnetic resonance imaging in blunt pancreatic trauma: a prospective study. Acta Radiol. 2015;56(4):387–96.
Tharakan SJ, et al. Laparoscopy in Pediatric Abdominal Trauma: A 13-Year Experience. Eur J Pediatr Surg. 2016;26(5):443–8.
Johnson JJ, et al. The use of laparoscopy in the diagnosis and treatment of blunt and penetrating abdominal injuries: 10-year experience at a level 1 trauma center. Am J Surg. 2013;205(3):317–20.
Sitnikov V, et al. The role of video-assisted laparoscopy in management of patients with small bowel injuries in abdominal trauma. Surg Endosc. 2009;23(1):125–9.
Nicolau AE, et al. Small bowel perforation caused by compound pelvic fracture found in diagnostic laparoscopy. Chirurgia (Bucur). 2006;101(4):423–8.
Uranus S, Dorr K. Laparoscopy in Abdominal Trauma. Eur J Trauma Emerg Surg. 2010;36(1):19–24.
Kindel T, et al. Laparoscopy in trauma: An overview of complications and related topics. Int J Crit Illn Inj Sci. 2015;5(3):196–205.
Becker HP, Willms A, Schwab R. Laparoscopy for abdominal trauma. Chirurg. 2006;77(11):1007–133.
Khubutiya M, et al. Laparoscopy in blunt and penetrating abdominal trauma. Surg Laparosc Endosc Percutan Tech. 2013;23(6):507–12.
Nicolau AE. Is laparoscopy still needed in blunt abdominal trauma? Chirurgia (Bucur). 2011;106(1):59–66.
Lee PC, et al. Laparoscopy decreases the laparotomy rate in hemodynamically stable patients with blunt abdominal trauma. Surg Innov. 2014;21(2):155–65.
Kaban GK, et al. Use of laparoscopy in evaluation and treatment of penetrating and blunt abdominal injuries. Surg Innov. 2008;15(1):26–31.
Gaines BA, Rutkoski JD. The role of laparoscopy in pediatric trauma. Semin Pediatr Surg. 2010;19(4):300–3.
Gregoric PD, et al. Laparoscopy in the evaluation of blunt abdominal trauma. Acta Chir Iugosl. 2010;57(4):33–8.
Addeo P, Calabrese DP. Diagnostic and therapeutic value of laparoscopy for small bowel blunt injuries: A case report. Int J Surg Case Rep. 2011;2(8):316–8.
Fuentes S, et al. Laparoscopy as diagnostic-therapeutic method in abdominal traumatism in the pediatric age. Cir Pediatr. 2011;24(2):115–7.
Van Kerschaver O, et al. An unusual case of blunt abdominal trauma: A bleeding and ruptured gall-bladder managed by laparoscopy. Acta Chir Belg. 2006;106(4):417–9.
Kovachev S, et al. Open laparoscopy–a modified Hasson technique. Akush Ginekol (Sofiia). 2015;54(4):52–6.
Marwan A, et al. Use of laparoscopy in the management of pediatric abdominal trauma. J Trauma. 2010;69(4):761–4.
Lin HF, et al. Value of diagnostic and therapeutic laparoscopy for patients with blunt abdominal trauma: A 10-year medical center experience. PLoS ONE. 2018;13(2):e0193379.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Achatz Gerhard, Schwabe Kerstin, Brill Sebastian, Zischek Christoph, Schmidt Roland, Friemert Benedikt and Beltzer Christian declare that there is no conflict of interest regarding this paper and topic.
Ethical approval
For this study there were no test or experiments to humans or animals.
Additional information
The original version of this article was revised: In the author list, the first and last names were tagged incorrectly. The corrected author list is given above.
Rights and permissions
About this article
Cite this article
Achatz, G., Schwabe, K., Brill, S. et al. Diagnostic options for blunt abdominal trauma. Eur J Trauma Emerg Surg 48, 3575–3589 (2022). https://doi.org/10.1007/s00068-020-01405-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-020-01405-1